Abstract
Objective
The aim of this study was to predict the risk of lingual plate fracture during mandibular third molar (M3) extraction.
Materials and methods
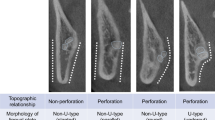
Cone beam computed tomography (CBCT) data from 264 mandibular M3s (erupted and impacted) from 264 patients (104 males and 160 females; age range, 17–75 years) were retrospectively analyzed. Lingual plate thicknesses at the levels of the mid-root and root apex of the M3s were measured and defined as “thicker” (bone thicker than 1 mm), “thinner” (bone thinner than 1 mm), or “perforated” (bone perforated by the M3 root). These measurements were correlated with potential risk factors for thinner and perforated lingual plates: tooth position of the mandibular M3, morphology of the lingual plate, and patient characteristics (age and sex).
Results
The mean thickness of the lingual plate was 1.49 ± 1.38 mm at the mid-root of the M3s, and 2.35 ± 2.03 mm at the root apex. Multivariate regression analyses revealed that mesioangularly and horizontally impacted M3s were significantly associated with thinner and perforated lingual plates at the mid-root (P < 0.001), whereas the M3s in infra-occlusion positions (in infra-occlusion when compared with the adjacent second molar) had thinner lingual bone at the root apex (P = 0.022 and P = 0.027, depending on the level of impaction). Female patients were less likely to have lingual plate perforation (P = 0.036).
Conclusions
Mesioangulation, infra-occlusion, and male sex were risk factors for lingual plate fracture.
Clinical relevance
When the risk of lingual plate fracture is high, a sufficiently large flap, osteotomy, and tooth section by bur or piezosurgery are recommended to create a good operative field and avoid excessive pressure on the lingual plate.







Similar content being viewed by others
References
Boffano P, Ferretti F, Giunta G, Gallesio C (2012) Surgical removal of a third molar at risk for mandibular pathologic fracture: case report and clinical considerations. Oral Surg Oral Med Oral Pathol Oral Radiol 114(6):e1–e4. https://doi.org/10.1016/j.oooo.2011.09.025
Aznar-Arasa L, Figueiredo R, Gay-Escoda C (2012) Iatrogenic displacement of lower third molar roots into the sublingual space: report of 6 cases. J Oral Maxillofac Surg 70(2):e107–e115. https://doi.org/10.1016/j.joms.2011.09.039
Figueiredo R, Valmaseda-Castellon E, Formoso-Senande MF, Berini-Aytés L, Gay-Escoda C (2012) Delayed-onset infections after impacted lower third molar extraction: involved bacteria and sensitivity profiles to commonly used antibiotics. Oral Surg Oral Med Oral Pathol Oral Radiol 114(1):43–48. https://doi.org/10.1016/j.tripleo.2011.06.022
Kose I, Koparal M, Günes N, Atalay Y, Yaman F, Atilgan S, Kaya G (2014) Displaced lower third molar tooth into the submandibular space: two case reports. J Nat Sci Biol Med 5(2):482–484. https://doi.org/10.4103/0976-9668.136274
Zhao S, Huang Z, Geng T, Huang L (2015) Intraoral management of iatrogenically displaced lower third molar roots in the sublingual space: a report of 2 cases. Int J Clin Exp Med 8(10):19591–19595
Figueiredo R, Valmaseda-Castellon E, Laskin DM, Berini-Aytes L, Gay-Escoda C (2008) Treatment of delayed-onset infections after impacted lower third molar extraction. J Oral Maxillofac Surg 66(5):943–947. https://doi.org/10.1016/j.joms.2008.01.045
Charan Babu HS, Reddy PB, Pattathan RK, Desai R, Shubha AB (2013) Factors influencing lingual nerve paraesthesia following third molar surgery: a prospective clinical study. J Maxillofac Oral Surg 12(2):168–172. https://doi.org/10.1007/s12663-012-0391-5
Jerjes W, Upile T, Shah P, Nhembe F, Gudka D, Kafas P, McCarthy E, Abbas S, Patel S, Hamdoon Z, Abiola J, Vourvachis M, Kalkani M, Al-Khawalde M, Leeson R, Banu B, Rob J, El-Maaytah M, Hopper C (2010) Risk factors associated with injury to the inferior alveolar and lingual nerves following third molarsurgery-revisited. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109(3):335–345. https://doi.org/10.1016/j.tripleo.2009.10.010
Bataineh AB (2001) Sensory nerve impairment following mandibular third molar surgery. J Oral Maxillofac Surg 59(9):1012–1017. https://doi.org/10.1053/joms.2001.25827
Ge J, Zheng JW, Yang C, Qian WT (2016) Variations in the buccal-lingual alveolar bone thickness of impacted mandibular third molar: our classification and treatment perspectives. Sci Rep 6:16375. https://doi.org/10.1038/srep16375
Wang D, He X, Wang Y, Zhou G, Sun C, Yang L, Bai J, Gao J, Wu Y, Cheng J (2016) Topographic relationship between root apex of mesially and horizontally impacted mandibular third molar and lingual plate cross-sectional analysis using CBCT. Sci Rep 6:39268. https://doi.org/10.1038/srep39268
Emes Y, Oncu B, Aybar B, Al-Badri N, Işsever H, Atalay B, Yalçın S (2015) Measurement of the lingual position of the lower third molar roots using cone-beam computed tomography. J Oral Maxillofac Surg 73(1):13–17. https://doi.org/10.1016/j.joms.2014.06.460
Pell GJ, Gregory GT (1933) Impacted mandibular third molars: classification and modified technique for removal. Dent Dig 39(9):e330–e338
Winter GB (1926) Principles of exodontia as applied to the impacted third molar. American Medical Books, St Louis
Yilmaz S, Adisen MZ, Misirlioglu M, Yorubulut S (2016) Assessment of third molar impaction pattern and associated clinical symptoms in a central Anatolian Turkish population. Med Princ Pract 25(2):169–175. https://doi.org/10.1159/000442416
Tolstunov L, Brickeen M, Kamanin V, Susarla SM, Selvi F (2016) Is the angulation of mandibular third molars associated with the thickness of lingual bone? Br J Oral Maxillofac Surg 54(8):914–919. https://doi.org/10.1016/j.bjoms.2016.06.005
Chan HL, Brooks SL, Fu JH, Yeh CY, Rudek I, Wang HL (2011) Cross-sectional analysis of the mandibular lingual concavity using cone beam computed tomography. Clin Oral Implants Res 22(2):201–206. https://doi.org/10.1111/j.1600-0501.2010.02018.x
Momin MA, Matsumoto K, Ejima K, Asaumi R, Kawai T, Arai Y, Honda K, Yosue T (2013) Correlation of mandibular impacted tooth and bone morphology determined by cone beam computed topography on a premise of third molar operation. Surg Radiol Anat 35(4):311–318. https://doi.org/10.1007/s00276-012-1031-y
Xavier CB, Gonçalves FR, Batista SH, Veras Filho Rde O, Vogt BF (2011) Spontaneous migration of third molar following displacement to pterygomandibular fossa. J Oral Maxillofac Surg 69(4):1004–1007. https://doi.org/10.1016/j.joms.2010.05.052
Huang IY, Wu CW, Worthington P (2007) The displaced lower third molar: a literature review and suggestions for management. J Oral Maxillofac Surg 65(6):1186–1190. https://doi.org/10.1016/j.joms.2006.11.031
Araki K, Maki K, Seki K, Sakamaki K, Harata Y, Sakaino R, Okano T, Seo K (2004) Characteristics of a newly developed dentomaxillofacial X-ray cone beam CT scanner (CB MercuRay): system configuration and physical properties. Dentomaxillofac Radiol 33(1):51–99. https://doi.org/10.1259/dmfr/54013049
Hashimoto K, Kawashima S, Kameoka S, Akiyama Y, Honjoya T, Ejima K, Sawada K (2007) Comparison of image validity between cone beam computed tomography for dental use and multidetector row helical computed tomography. Dentomaxillofac Radiol 36(8):465–471. https://doi.org/10.1259/dmfr/22818643
Loubele M, Guerrero ME, Jacobs R, Suetens P, van Steenberghe D (2007) A comparison of jaw dimensional and quality assessments of bone characteristics with cone-beam CT, spiral tomography, and multi-slice spiral CT. Int J Oral Maxillofac Implants 22(3):446–454
Pauwels R, Araki K, Siewerdsen JH, Thongvigitmanee SS (2015) Technical aspects of dental CBCT: state of the art. Dentomaxillofac Radiol 44(1):20140224. https://doi.org/10.1259/dmfr.20140224
Aksoy U, Orhan K (2018) Risk factor in endodontic treatment: topographic evaluation of mandibular posterior teeth and lingual cortical plate using cone beam computed tomography (CT). Med Sci Monit 21(24):7508–7516. https://doi.org/10.12659/MSM.908970
Menziletoglu D, Tassoker M, Kubilay-Isik B, Esen A (2019) The assessment of relationship between the angulation of impacted mandibular third molar teeth and the thickness of lingual bone: a prospective clinical study. Med Oral Patol Oral Cir Bucal 24(1):e130–e135. https://doi.org/10.4317/medoral.22596
Mallick A, Vidya KC, Waran A, Rout SK (2017) Measurement of lingual cortical plate thickness and lingual position of lower third molar roots using cone beam computed tomography. J Int Soc Prev Community Dent 7(Suppl 1):S8–S12. https://doi.org/10.4103/jispcd.JISPCD_106_17
Aoki C, Nara T, Kageyama I (2011) Relative position of the mylohyoid line on dentulous and edentulous mandibles. Okajimas Folia Anat Jpn 87(4):171–176. https://doi.org/10.2535/ofaj.87.171
Huang RY, Cochran DL, Cheng WC, Lin MH, Fan WH, Sung CE, Mau LP, Huang PH, Shieh YS (2015) Risk of lingual plate perforation for virtual immediate implant placement in the posterior mandible: a computer simulation study. J Am Dent Assoc 146(10):735–742. https://doi.org/10.1016/j.adaj.2015.04.027
Wolsan M, Suzuki S, Asahara M, Motokawa M (2015) Tooth size variation in pinniped dentitions. PLoS One 10(8):e0137100. https://doi.org/10.1371/journal.pone.0137100
Watanabe H, Mohammad Abdul M, Kurabayashi T, Aoki H (2010) Mandible size and morphology determined with CT on a premise of dental implant operation. Surg Radiol Anat 32(4):343–349. https://doi.org/10.1007/s00276-009-0570-3
Funding
This work was supported by the Medical Scientific Research Foundation of Shanghai Hongkou District Health Commission of China (No. 1803-02) and the Shanghai Hongkou Excellent Youth Physician Training Programme (HKYG 2018-10).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Cheng Huang. The first draft of the manuscript was written by Cheng Huang and Derong Zou, and the revision for important intellectual content was performed by Chun Zhou and Minhua Xu.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of our institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study (retrospective study), formal consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Huang, C., Zhou, C., Xu, M. et al. Risk factors for lingual plate fracture during mandibular third molar extraction. Clin Oral Invest 24, 4133–4142 (2020). https://doi.org/10.1007/s00784-020-03286-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03286-5