Abstract
Introduction
The treatment landscape of postmenopausal osteoporosis (OP) in an Asian population is yet to be explored.
Materials and methods
We conducted a retrospective cohort study to explore treatment patterns and characteristics associated with treatment interruption in postmenopausal women diagnosed with OP between 2008 and 2014. Treatment pattern assessment included the initial distribution of OP medications and treatment interruption rate according to the treatment groups during a 3-year follow-up period. We used multivariate logistic regression to estimate odds ratio (OR) and 95% confidence interval (CI) to identify factors associated with treatment interruption.
Results
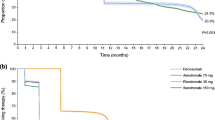
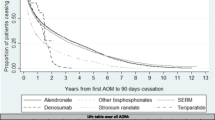
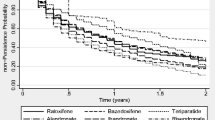
Of 21,813 patients, 87.9% initiated oral bisphosphonates (BP), followed by ibandronate intravenous (IV; 5.4%), selective estrogen receptor modulators (SERMs; 5.2%), pamidronate IV (1.4%) and zoledronic acid (0.06%). Treatment interruption was most notable in the first year of treatment, with cumulative treatment interruption rates highest for oral BP (76.3%) and lowest for pamidronate IV (50.5%). Compared to oral BP users, users of ibandronate IV (OR 0.34, 95% CI 0.30–0.39), pamidronate IV (0.49, 0.39–0.63), zoledronic acid (0.26, 0.09–0.77), and SERMs (0.50, 0.44–0.57) were less likely to interrupt treatment. Of characteristics assessed, presence of rheumatoid arthritis increased the odds of treatment interruption in ibandronate IV group (3.94, 2.12–7.33), and concomitant use of glucocorticoids for oral BP (1.11, 1.03–1.19) and pamidronate IV (2.04, 1.06–3.93) groups, respectively.
Conclusion
Given the frequent treatment interruptions across all OP medications, our findings on the factors associated with treatment interruption will serve to implement targeted interventions in reinforcing persistence to OP treatment.



Similar content being viewed by others
Availability of data and material
We used the customized DB extracted and provided National Health Insurance Sharing System (NHISS) (Further details are available on the website: https://nhiss.nhis.or.kr/bd/ab/bdaba032eng.do).
Code availability
Available upon request.
References
Singer A, Exuzides A, Spangler L, O’Malley C, Colby C, Johnston K, Agodoa I, Baker J, Kagan R (2015) Burden of illness for osteoporotic fractures compared with other serious diseases among postmenopausal women in the United States. Mayo Clin Proc 90:53–62. https://doi.org/10.1016/j.mayocp.2014.09.011
Jackson RD, Mysiw WJ (2014) Insights into the epidemiology of postmenopausal osteoporosis: the Women’s Health Initiative. Semin Reprod Med 32:454–462. https://doi.org/10.1055/s-0034-1384629
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R, National Osteoporosis F (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25:2359–2381. https://doi.org/10.1007/s00198-014-2794-2
Choi YJ, Oh HJ, Kim DJ, Lee Y, Chung YS (2012) The prevalence of osteoporosis in Korean adults aged 50 years or older and the higher diagnosis rates in women who were beneficiaries of a national screening program: the Korea National Health and Nutrition Examination Survey 2008–2009. J Bone Miner Res 27:1879–1886. https://doi.org/10.1002/jbmr.1635
Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S, Dawson-Hughes B (2014) The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. J Bone Miner Res 29:2520–2526. https://doi.org/10.1002/jbmr.2269
Siris ES, Harris ST, Rosen CJ, Barr CE, Arvesen JN, Abbott TA, Silverman S (2006) Adherence to bisphosphonate therapy and fracture rates in osteoporotic women: relationship to vertebral and nonvertebral fractures from 2 US claims databases. Mayo Clin Proc 81:1013–1022. https://doi.org/10.4065/81.8.1013
Fujiwara S, Miyauchi A, Hamaya E, Nicholls RJ, Weston A, Baidya S, Pinto L, Barron R, Takada J (2018) Treatment patterns in patients with osteoporosis at high risk of fracture in Japan: retrospective chart review. Arch Osteoporos 13:34. https://doi.org/10.1007/s11657-018-0443-7
Melo M, Qiu F, Sykora K, Juurlink D, Laupacis A, Mamdani M (2006) Persistence with bisphosphonate therapy in older people. J Am Geriatr Soc 54:1015–1016. https://doi.org/10.1111/j.1532-5415.2006.00758.x
Cramer JA, Gold DT, Silverman SL, Lewiecki EM (2007) A systematic review of persistence and compliance with bisphosphonates for osteoporosis. Osteoporos Int 18:1023–1031. https://doi.org/10.1007/s00198-006-0322-8
Park EC, Jang SI, Jeon SY, Lee SA, Lee JE, Choi DW (2017) Report of the evaluation for validity of discharged diagnoses in Korean Health Insurance database. Health Insurance Review & Assessment Service,
Kim HS, Shin DW, Lee WC, Kim YT, Cho B (2012) National screening program for transitional ages in Korea: a new screening for strengthening primary prevention and follow-up care. J Korean Med Sci 27(Suppl):S70–S75. https://doi.org/10.3346/jkms.2012.27.S.S70
Seong SC, Kim YY, Park SK, Khang YH, Kim HC, Park JH, Kang HJ, Do CH, Song JS, Lee EJ, Ha S, Shin SA, Jeong SL (2017) Cohort profile: the National Health Insurance Service-National Health Screening Cohort (NHIS-HEALS) in Korea. BMJ Open 7:e016640. https://doi.org/10.1136/bmjopen-2017-016640
Solomon DH, Avorn J, Katz JN, Finkelstein JS, Arnold M, Polinski JM, Brookhart MA (2005) Compliance with osteoporosis medications. Arch Intern Med 165:2414–2419. https://doi.org/10.1001/archinte.165.20.2414
Balasubramanian A, Brookhart MA, Goli V, Critchlow CW (2013) Discontinuation and reinitiation patterns of osteoporosis treatment among commercially insured postmenopausal women. Int J Gen Med 6:839–848. https://doi.org/10.2147/IJGM.S36944
Burden AM, Paterson JM, Solomon DH, Mamdani M, Juurlink DN, Cadarette SM (2012) Bisphosphonate prescribing, persistence and cumulative exposure in Ontario, Canada. Osteoporos Int 23:1075–1082. https://doi.org/10.1007/s00198-011-1645-7
Wysowski DK, Greene P (2013) Trends in osteoporosis treatment with oral and intravenous bisphosphonates in the United States, 2002–2012. Bone 57:423–428. https://doi.org/10.1016/j.bone.2013.09.008
Yun H, Curtis JR, Guo L, Kilgore M, Muntner P, Saag K, Matthews R, Morrisey M, Wright NC, Becker DJ, Delzell E (2014) Patterns and predictors of osteoporosis medication discontinuation and switching among Medicare beneficiaries. BMC Musculoskelet Disord 15:112. https://doi.org/10.1186/1471-2474-15-112
Tremollieres FA, Pouilles JM, Drewniak N, Laparra J, Ribot CA, Dargent-Molina P (2010) Fracture risk prediction using BMD and clinical risk factors in early postmenopausal women: sensitivity of the WHO FRAX tool (in eng). J Bone Mineral Res: Off J Am Soc Bone Mineral Res 25:1002–1009. https://doi.org/10.1002/jbmr.12
National Osteoporosis Foundation: 2013 Clinician's Guide to Prevention and Treatment of Osteoporosis. (2013) National Osteoporosis Foundation.
Jiao H, Xiao E, Graves DT (2015) Diabetes and its effect on bone and fracture healing (in eng). Curr Osteoporos Rep 13:327–335. https://doi.org/10.1007/s11914-015-0286-8
Hippisley-Cox J, Coupland C (2012) Derivation and validation of updated QFracture algorithm to predict risk of osteoporotic fracture in primary care in the United Kingdom: prospective open cohort study (in eng). BMJ (Clinical research ed) 344:e3427. https://doi.org/10.1136/bmj.e3427
Kim HA, Shin JY, Kim MH, Park BJ (2014) Prevalence and predictors of polypharmacy among Korean elderly (in eng). PLoS ONE 9:e98043. https://doi.org/10.1371/journal.pone.0098043
Szklo M, Nieto J (2007) Epidemiology: Beyond the Basics. Jones & Bartlett Learning
Gleason LJ, Menzies IB, Mendelson DA, Kates SL, Friedman SM (2012) Diagnosis and treatment of osteoporosis in high-risk patients prior to hip fracture. Geriatr Orthop Surg Rehabil 3:79–83. https://doi.org/10.1177/2151458512454878
Siris ES, Modi A, Tang J, Gandhi S, Sen S (2014) Substantial under-treatment among women diagnosed with osteoporosis in a US managed-care population: a retrospective analysis. Curr Med Res Opin 30:123–130. https://doi.org/10.1185/03007995.2013.851074
Reyes C, Tebe C, Martinez-Laguna D, Ali MS, Soria-Castro A, Carbonell C, Prieto-Alhambra D (2017) One and two-year persistence with different anti-osteoporosis medications: a retrospective cohort study. Osteoporos Int 28:2997–3004. https://doi.org/10.1007/s00198-017-4144-7
Kothawala P, Badamgarav E, Ryu S, Miller RM, Halbert RJ (2007) Systematic review and meta-analysis of real-world adherence to drug therapy for osteoporosis. Mayo Clin Proc 82:1493–1501. https://doi.org/10.1016/s0025-6196(11)61093-8
Epstein S, Jeglitsch M, McCloskey E (2009) Update on monthly oral bisphosphonate therapy for the treatment of osteoporosis: focus on ibandronate 150 mg and risedronate 150 mg. Curr Med Res Opin 25:2951–2960. https://doi.org/10.1185/03007990903361307
Durden E, Pinto L, Lopez-Gonzalez L, Juneau P, Barron R (2017) Two-year persistence and compliance with osteoporosis therapies among postmenopausal women in a commercially insured population in the United States. Arch Osteoporos 12:22. https://doi.org/10.1007/s11657-017-0316-5
Ettinger B, Black DM, Mitlak BH, Knickerbocker RK, Nickelsen T, Genant HK, Christiansen C, Delmas PD, Zanchetta JR, Stakkestad J, Gluer CC, Krueger K, Cohen FJ, Eckert S, Ensrud KE, Avioli LV, Lips P, Cummings SR (1999) Reduction of vertebral fracture risk in postmenopausal women with osteoporosis treated with raloxifene: results from a 3-year randomized clinical trial. Multiple Outcomes of Raloxifene Evaluation (MORE) Investigators. JAMA 282:637–645. https://doi.org/10.1001/jama.282.7.637
Foster SA, Shi N, Curkendall S, Stock J, Chu BC, Burge R, Diakun DR, Krege JH (2013) Fractures in women treated with raloxifene or alendronate: a retrospective database analysis. BMC Womens Health 13:15. https://doi.org/10.1186/1472-6874-13-15
Ferrari S, Nakamura T, Hagino H, Fujiwara S, Lange JL, Watts NB (2011) Longitudinal change in hip fracture incidence after starting risedronate or raloxifene: an observational study. J Bone Miner Metab 29:561–570. https://doi.org/10.1007/s00774-010-0249-1
Bachmann G, Kriegman A, Goncalves J, Kianifard F, Warren M, Simon JA (2011) Effect of zoledronic acid compared with raloxifene on bone turnover markers in postmenopausal women with low bone density. Menopause 18:851–856. https://doi.org/10.1097/gme.0b013e31820b80f1
Foster SA, Foley KA, Meadows ES, Johnston JA, Wang S, Pohl GM, Long SR (2008) Characteristics of patients initiating raloxifene compared to those initiating bisphosphonates. BMC Womens Health 8:24. https://doi.org/10.1186/1472-6874-8-24
Berry SD, Dufour AB, Travison TG, Zhu H, Yehoshua A, Barron R, Recknor C, Samelson EJ (2018) Changes in bone mineral density (BMD): a longitudinal study of osteoporosis patients in the real-world setting. Arch Osteoporos 13:124. https://doi.org/10.1007/s11657-018-0528-3
Perazella MA, Markowitz GS (2008) Bisphosphonate nephrotoxicity. Kidney Int 74:1385–1393. https://doi.org/10.1038/ki.2008.356
Conte P, Guarneri V (2004) Safety of intravenous and oral bisphosphonates and compliance with dosing regimens. Oncologist 9(Suppl 4):28–37. https://doi.org/10.1634/theoncologist.9-90004-28
Raterman HG, Lems WF (2019) Pharmacological management of osteoporosis in rheumatoid arthritis patients: a review of the literature and practical guide (in eng). Drugs Aging 36:1061–1072. https://doi.org/10.1007/s40266-019-00714-4
Richards JS, Cannon GW, Hayden CL, Amdur RL, Lazaro D, Mikuls TR, Reimold AM, Caplan L, Johnson DS, Schwab P, Cherascu BN, Kerr GS (2012) Adherence with bisphosphonate therapy in US veterans with rheumatoid arthritis. Arthritis Care Res 64:1864–1870. https://doi.org/10.1002/acr.21777
Ladova K, Vlcek J, Vytrisalova M, Maly J (2014) Healthy adherer effect – the pitfall in the interpretation of the effect of medication adherence on health outcomes. J Eval Clin Pract 20:111–116. https://doi.org/10.1111/jep.12095
Stein JD, Lum F, Lee PP, Rich WL 3rd, Coleman AL (2014) Use of health care claims data to study patients with ophthalmologic conditions. Ophthalmology 121:1134–1141. https://doi.org/10.1016/j.ophtha.2013.11.038
Funding
This study received funding from Amgen Korea, Ltd.
Author information
Authors and Affiliations
Contributions
JK: conceptualization and writing—original draft. HJ: methodology, software, and writing—original draft. YB: conceptualization and methodology. SC and HL: methodology and writing—review and editing. JS: funding acquisition, conceptualization, and supervision. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflict of interest.
Ethics approval
This study was approved by the Sungkyunkwan University’s Institutional Review Board (SKKU-IRB- 2018–11-004), which waived the requirement for informed consent.
Consent for publication
This manuscript has been approved by all co-authors and has not been published before.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Kim, J.H., Jeong, H.E., Baek, YH. et al. Treatment pattern in postmenopausal women with osteoporosis: a population-based cohort study in South Korea. J Bone Miner Metab 40, 109–119 (2022). https://doi.org/10.1007/s00774-021-01259-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-021-01259-6