Abstract
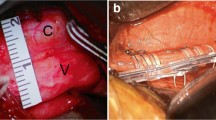
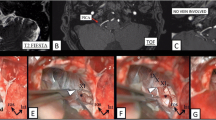
Vagal neuropathy causing vocal fold palsy is an uncommon complication of vagal nerve stimulator (VNS) placement. It may be associated with intraoperative nerve injury or with device stimulation. Here we present the first case of delayed, compressive vagal neuropathy associated with VNS coil placement which presented with progressive hoarseness and vocal cord paralysis. Coil removal and vagal neurolysis was performed to relieve the compression. Larger 3 mm VNS coils were placed for continuation of therapy. Coils with a larger inner diameter should be employed where possible to prevent this complication. The frequency of VNS-associated vagal nerve compression may warrant further investigation.



Similar content being viewed by others
Abbreviations
- VNS:
-
Vagal nerve stimulator
- VHI-10:
-
Voice handicap index-10
- EMG:
-
Electromyography
- CMAPs:
-
Compound motor action potentials
References
Alantie S, Makkonen T, Hietala S, Peltola J (2021) Clinical management of voice and breathing problems in two patients with vagus nerve stimulation therapy. Epileptic Disord 23:173–179. https://doi.org/10.1684/epd.2021.1250
Arffa RE, Krishna P, Gartner-Schmidt J, Rosen CA (2012) Normative values for the voice handicap index-10. J Voice 26:462–465. https://doi.org/10.1016/j.jvoice.2011.04.006
Ben-Menachem E (2001) Vagus nerve stimulation, side effects, and long-term safety. J Clin Neurophysiol 18:415–418. https://doi.org/10.1097/00004691-200109000-00005
Clark AJ, Kuperman RA, Auguste KI, Sun PP (2012) Intractable episodic bradycardia resulting from progressive lead traction in an epileptic child with a vagus nerve stimulator: a delayed complication. J Neurosurg Pediatr 9:389–393. https://doi.org/10.3171/2011.12.PEDS11124
Englot DJ, Chang EF, Auguste KI (2011) Vagus nerve stimulation for epilepsy: a meta-analysis of efficacy and predictors of response. J Neurosurg 115:1248–1255. https://doi.org/10.3171/2011.7.JNS11977
Felisati G, Gardella E, Schiavo P, Saibene AM, Pipolo C, Bertazzoli M, Chiesa V, Maccari A, Franzini A, Canevini MP (2014) Endoscopic laryngeal patterns in vagus nerve stimulation therapy for drug-resistant epilepsy. Eur Arch Otorhinolaryngol 271:117–123. https://doi.org/10.1007/s00405-013-2568-z
Giordano F, Zicca A, Barba C, Guerrini R, Genitori L (2017) Vagus nerve stimulation: surgical technique of implantation and revision and related morbidity. Epilepsia 58(Suppl 1):85–90. https://doi.org/10.1111/epi.13678
Kahlow H, Olivecrona M (2013) Complications of vagal nerve stimulation for drug-resistant epilepsy: a single center longitudinal study of 143 patients. Seizure 22:827–833. https://doi.org/10.1016/j.seizure.2013.06.011
Kalkanis JG, Krishna P, Espinosa JA, Naritoku DK (2002) Self-inflicted vocal cord paralysis in patients with vagus nerve stimulators. Report of two cases. J Neurosurg 96:949–951. https://doi.org/10.3171/jns.2002.96.5.0949
Kersing W, Dejonckere PH, van der Aa HE, Buschman HP (2002) Laryngeal and vocal changes during vagus nerve stimulation in epileptic patients. J Voice 16:251–257. https://doi.org/10.1016/s0892-1997(02)00094-2
Misono S, Yueh B, Stockness AN, House ME, Marmor S (2017) Minimal important difference in voice handicap index-10. JAMA Otolaryngol Head Neck Surg 143:1098–1103. https://doi.org/10.1001/jamaoto.2017.1621
Panebianco M, Rigby A, Marson AG (2022) Vagus nerve stimulation for focal seizures. Cochrane Database Syst Rev 7:CD002896. https://doi.org/10.1002/14651858.CD002896.pub3
Penry JK, Dean JC (1990) Prevention of intractable partial seizures by intermittent vagal stimulation in humans: preliminary results. Epilepsia 31(Suppl 2):S40-43. https://doi.org/10.1111/j.1528-1157.1990.tb05848.x
Robinson LC, Winston KR (2015) Relationship of vocal cord paralysis to the coil diameter of vagus nerve stimulator leads. J Neurosurg 122:532–535. https://doi.org/10.3171/2014.10.JNS14640
Rychlicki F, Zamponi N, Cesaroni E, Corpaci L, Trignani R, Ducati A, Scerrati M (2006) Complications of vagal nerve stimulation for epilepsy in children. Neurosurg Rev 29:103–107. https://doi.org/10.1007/s10143-005-0005-5
Wheless JW, Gienapp AJ, Ryvlin P (2018) Vagus nerve stimulation (VNS) therapy update. Epilepsy Behav 88S:2–10. https://doi.org/10.1016/j.yebeh.2018.06.032
Acknowledgements
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent
Written informed consent was obtained from the patient for the publication of this work.
Competing interests
None relevant to this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This abstract and operative video demonstration are original and have not been submitted or presented elsewhere in part or in whole.
Comments
The authors of this case report present an interesting case of intraoperatively documented constriction of the vagus nerve by a long-ago implanted electrode in a patient who experienced symptomatic improvement after the electrode was replaced with a larger version of the same device. Although very unusual, the finding is not completely unexpected as the nerve malfunctions and excessive fibrosis in the vicinity of implanted electrodes have been a known issue during the last several decades, ever since the peripheral nerve stimulation became an established therapeutic modality. As a matter of fact, I would venture to suspect this to be one of the main sources of voice alteration in VNS patients—just as the authors suggest here.
With all this, I want to congratulate the authors with their ability to preserve the vagus nerve functionality following their corrective surgery. One of the reasons such approach (electrode revision or replacement) is rarely considered is the remarkable fragility of the vagus nerve and serious risk of development of complete—and irreversible—vocal cord paralysis with any attempt to mobilize or remove the electrodes that are strongly attached to the nerve after being in place for a prolonged period of time.
As with everything else in medicine, it is better to prevent the problem than deal with it post-factum; perhaps development of softer and more pliable electrodes—or replacing them with non-invasive alternative options—would be an optimal solution for the future.
Konstantin Slavin
Chicago, USA
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
McGrath, H., Pennington, Z., Cross, M.R. et al. Delayed vagal nerve compressive neuropathy following placement of vagal nerve stimulator: case report. Acta Neurochir 166, 193 (2024). https://doi.org/10.1007/s00701-024-06087-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00701-024-06087-x