Abstract
Purpose
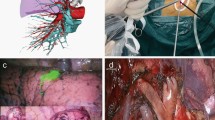
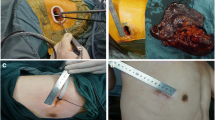
Needlescopic instruments allow us to perform complex laparoscopic procedures, which are almost painless and scarless postoperatively; however, their utilization in thoracoscopic surgery has been limited to minor procedures, including bullectomy and sympathectomy. We present our initial experience of performing thoracoscopic anatomical lung resection via a single utility incision with additional needlescopic working ports and compare the operative results with those of uniportal video-assisted thorascopic surgery (VATS).
Methods
We reviewed data on 75 consecutive patients with lung cancer, who underwent anatomical lung resections, including lobectomy and segmentectomy, between February 2015 and September 2017. Of the 75 patients, 39 underwent uniportal VATS (uniportal group), and 36 underwent needlescopic-assisted VATS (n-VATS group). We compared the peri- and postoperative outcomes of the two groups.
Results
The clinical characteristics did not differ significantly between the groups, except in the ages of the patients. The n-VATS group had a shorter operation time (mean 159.3 min vs. 198.8 min, P = 0.023) and lower intraoperative blood loss (mean 40.9 mL vs. 143.2 mL, P = 0.047). Two major pulmonary arterial bleeding events and one conversion to thoracotomy occurred in the uniportal group.
Conclusion
Uniportal VATS can be performed more efficiently and safely with the assistance of additional needlescopic ports and instruments, without compromising the benefits of less postoperative pain and early recovery.




Similar content being viewed by others
References
Bao F, Ye P, Yang Y, Wang L, Zhang C, Lv X, et al. Segmentectomy or lobectomy for early stage lung cancer: a meta-analysis. Eur J Cardiothorac Surg. 2014;46:1–7.
Zhang L, Li M, Yin R, Zhang Q, Xu L. Comparison of the oncologic outcomes of anatomic segmentectomy and lobectomy for early-stage non-small cell lung cancer. Ann Thorac Surg. 2015;99:728–37.
Tu CC, Hsu PK. Global development and current evidence of uniportal thoracoscopic surgery. J Thorac Dis. 2016;8(Suppl 3):308–18.
Yu PS, Capili F, Ng CS. Single port VATS: recent developments in Asia. J Thorac Dis. 2016;8(Suppl 3):302–7.
Rocco G. One-port (uniportal) video-assisted thoracic surgical resections–a clear advance. J Thorac Cardiovasc Surg. 2012;144:27–31.
Gonzalez-Rivas D, Fieira E, Delgado M, Mendez L, Fernandez R, de la Torre M. Evolving from conventional video-assisted thoracoscopic lobectomy to uniportal: the story behind the evolution. J Thorac Dis. 2014;6(Suppl 6):599–603.
Ismail M, Swierzy M, Nachira D, Rückert JC, Gonzalez-Rivas D. Uniportal video-assisted thoracic surgery for major lung resections: pitfalls, tips and tricks. J Thorac Dis. 2017;9:885–97.
Gonzalez-Rivas D, Yang Y, Ng C. Advances in uniportal video-assisted thoracoscopic surgery: pushing the envelope. Thorac Surg Clin. 2016;26:187–201.
Kim TS, Kim KH, An CH, Kim JS. Single center experiences of needlescopic grasper assisted single incision laparoscopic cholecystectomy for gallbladder benign disease: comparison with conventional 3-port laparoscopic cholecystectomy. Ann Surg Treat Res. 2016;91:233–8.
Inoue S, Kajiwara M, Teishima J, Matsubara A. Needlescopic-assisted laparoendoscopic single-site adrenalectomy. Asian J Surg. 2016;39:6–11.
Krpata DM, Ponsky TA. Needlescopic surgery: what’s in the toolbox? Surg Endosc. 2013;27:1040–4.
Yim AP, Liu HP, Lee TW, Wan S, Arifi AA. ‘Needlescopic’ video-assisted thoracic surgery for palmar hyperhidrosis. Eur J Cardiothorac Surg. 2000;17:697–701.
Chen JS, Hsu HH, Kuo SW, Tsai PR, Chen RJ, Lee JM, et al. Needlescopic versus conventional video-assisted thoracic surgery for primary spontaneous pneumothorax: a comparative study. Ann Thorac Surg. 2003;75:1080–5.
Kim HK, Jo WM, Jung JH, Chung WJ, Shim JH, Choi YH, et al. Needlescopic lung biopsy for interstitial lung disease and indeterminate pulmonary nodules: a report on 65 cases. Ann Thorac Surg. 2008;86:1098–103.
McCormack HM, Horne DJ, Sheather S. Clinical applications of visual analogue scales: a critical review. Psychol Med. 1988;18:1007–19.
Migliore M, Halezeroglu S, Molins L, Van Raemdonck D, Mueller MR, Rea F, et al. Uniportal video-assisted thoracic surgery or single-incision video-assisted thoracic surgery for lung resection: clarifying definitions. Fut Oncol. 2016;12:5–7.
Bertolaccini L, Rocco G, Pardolesi A, Solli P. The geometric and ergonomic appeal of uniportal video-assisted thoracic surgery. Thorac Surg Clin. 2017;27:331–8.
Sihoe AD. The evolution of minimally invasive thoracic surgery: implications for the practice of uniportal thoracoscopic surgery. J Thorac Dis. 2014;6(Suppl 6):604-17.
Tagaya N, Kubota K. Reevaluation of needlescopic surgery. Surg Endosc. 2012;26:137–43.
Gould JC, Frydman J. Reverse-alignment surgical skills assessment. Surg Endosc. 2007;21:669–71.
Dunnican WJ, Singh TP, Ata A, Bendana EE, Conlee TD, Dolce CJ, et al. Reverse alignment “mirror image” visualization as a laparoscopic training tool improves task performance. Surg Innov. 2010;17:108–13.
Johnston WK, Low RK, Das S. Image converter eliminates mirror imaging during laparoscopy. J Endourol. 2003;17:327–31.
Gill RS, Al-Adra DP, Mangat H, Wang H, Shi X, Sample C. Image inversion and digital mirror-image technology aid laparoscopic surgery task performance in the paradoxical view: a randomized controlled trial. Surg Endosc. 2011;25:3535–9.
Hirai K, Takeuchi S, Usuda J. Single-incision thoracoscopic surgery and conventional video-assisted thoracoscopic surgery: a retrospective comparative study of perioperative clinical outcomes. Eur J Cardiothorac Surg. 2016;49(Suppl 1):i37–41.
McElnay PJ, Molyneux M, Krishnadas R, Batchelor TJ, West D, Casali G. Pain and recovery are comparable after either uniportal or multiport video-assisted thoracoscopic lobectomy: an observation study. Eur J Cardiothorac Surg. 2015;47:912–5.
Yang HC, Cho S, Jheon S. Single-incision thoracoscopic surgery for primary spontaneous pneumothorax using the SILS port compared with conventional three-port surgery. Surg Endosc. 2013;27:139–45.
Song IH, Lee SY, Lee SJ. Can single-incision thoracoscopic surgery using a wound protector be used as a first-line approach for the surgical treatment of primary spontaneous pneumothorax? A comparison with three-port video-assisted thoracoscopic surgery. Gen Thorac Cardiovasc Surg. 2015;63:284–9.
Sihoe AD, Manlulu AV, Lee TW, Thung KH, Yim AP. Pre-emptive local anesthesia for needlescopic video-assisted thoracic surgery: a randomized controlled trial. Eur J Cardiothorac Surg. 2007;31:103–8.
Sandri A, Sihoe AD, Salati M, Gonzalez-Rivas D, Brunelli A. Training in uniportal video-assisted thoracic surgery. Thorac Surg Clin. 2017;27:417–23.
Acknowledgements
We thank the staff of Biotechnology R&D Center, National Taiwan University Hospital, Hsin-Chu Branch for their assistance with the study design and statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Drs. Huan-Jang Ko, Xu-Heng Chiang, Shun-Mao Yang, and Ming-Chi Yang have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Ko, HJ., Chiang, XH., Yang, SM. et al. Needlescopic-assisted thoracoscopic pulmonary anatomical lobectomy and segmentectomy for lung cancer: a bridge between multiportal and uniportal thoracoscopic surgery. Surg Today 49, 49–55 (2019). https://doi.org/10.1007/s00595-018-1707-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-018-1707-y