Abstract
Purpose
To assess and compare 5-year outcomes following uninstrumented spinal decompression and decompression with interlaminar device (ILD). To determine whether improvement in clinical outcomes correlated with changes in the radiological indices studied. This is because comparative literature between the above two procedures is limited past the 2-year timeframe.
Methods
We conducted a retrospective review of prospectively collected data from a single surgeon across 116-patients who underwent spinal decompression with or without ILD insertion between 2007 and 2015. Patients with symptomatic LSS who met the study criteria were offered spinal decompression with ILD insertion. Patients who accepted ILD were placed in the D + ILD group (n = 61); while those opting for decompression alone were placed in the DA group (n = 55). Clinical outcomes were assessed preoperatively and up to 5-years postoperatively using the ODI, Eq. 5d, VAS back and leg pain, and SF-36. Radiological indices were assessed preoperatively and up to 5-years postoperatively.
Results
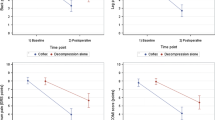
Both groups showed statistically significant (p < 0.001) improvement in all clinical outcome indicators at all timepoints as compared to their preoperative status. The D + ILD group achieved significant improvement in radiological parameters namely foraminal height and posterior disc height in the immediate postoperative period that was maintained while the DA group did not.
Conclusion
Our study found that in the management of LSS, clinical outcomes between those patients undergoing decompression alone compared to decompression with ILD showed statistically significant improvement in VAS back pain and radiological parameters namely foraminal height and posterior disc height at the 5-year mark. ILD does not predispose to increased reoperation rates.

Similar content being viewed by others
References
Fritz JM, Lurie JD, Zhao W, Whitman JM, Delitto A, Brennan GP, Weinstein JN (2014) Associations between physical therapy and long-term outcomes for individuals with lumbar spinal stenosis in the SPORT study. Spine J 14:1611–1621. https://doi.org/10.1016/j.spinee.2013.09.044
Weinstein JN, Lurie JD, Tosteson TD, Zhao W, Blood EA, Tosteson AN, Birkmeyer N, Herkowitz H, Longley M, Lenke L, Emery S, Hu SS (2009) Surgical compared with nonoperative treatment for lumbar degenerative spondylolisthesis. four-year results in the Spine Patient Outcomes Research Trial (SPORT) randomized and observational cohorts. J Bone Jt Surg Am 91:1295–1304. https://doi.org/10.2106/jbjs.H.00913
Ahmad S, Hamad A, Bhalla A, Turner S, Balain B, Jaffray D (2017) The outcome of decompression alone for lumbar spinal stenosis with degenerative spondylolisthesis. Eur Spine J 26:414–419. https://doi.org/10.1007/s00586-016-4637-7
Thomas K, Faris P, McIntosh G, Manners S, Abraham E, Bailey CS, Paquet J, Cadotte D, Jacobs WB, Rampersaud YR, Manson NA, Hall H, Fisher CG (2019) Decompression alone vs. decompression plus fusion for claudication secondary to lumbar spinal stenosis. Spine J 19:1633–1639. https://doi.org/10.1016/j.spinee.2019.06.003
Masuda S, Kanba Y, Kawai J, Ikeda N (2020) Outcomes after decompression surgery without fusion for patients with lumbar spinal stenosis and substantial low back pain. Eur Spine J 29:147–152. https://doi.org/10.1007/s00586-019-06130-x
Anjarwalla NK, Brown LC, McGregor AH (2007) The outcome of spinal decompression surgery 5 years on. Eur Spine J 16:1842–1847. https://doi.org/10.1007/s00586-007-0393-z
Kumar N, Shah SM, Ng YH, Pannierselvam VK, Dasde S, Shen L (2014) Role of coflex as an adjunct to decompression for symptomatic lumbar spinal stenosis. Asian Spine J 8:161–169. https://doi.org/10.4184/asj.2014.8.2.161
Lu T, Lu Y (2020) Interlaminar stabilization offers greater biomechanical advantage compared to interspinous stabilization after lumbar decompression: a finite element analysis. J Orthop Surg Res 15:291. https://doi.org/10.1186/s13018-020-01812-5
Lønne G, Johnsen LG, Rossvoll I, Andresen H, Storheim K, Zwart JA, Nygaard ØP (2015) Minimally invasive decompression versus x-stop in lumbar spinal stenosis: a randomized controlled multicenter study. Spine (Phila Pa 1976) 40:77–85. https://doi.org/10.1097/brs.0000000000000691
Moojen WA, Arts MP, Jacobs WC, van Zwet EW, van den Akker-van Marle ME, Koes BW, Vleggeert-Lankamp CL, Peul WC (2015) IPD without bony decompression versus conventional surgical decompression for lumbar spinal stenosis: 2-year results of a double-blind randomized controlled trial. Eur Spine J 24:2295–2305. https://doi.org/10.1007/s00586-014-3748-2
Yuan W, Su QJ, Liu T, Yang JC, Kang N, Guan L, Hai Y (2017) Evaluation of Coflex interspinous stabilization following decompression compared with decompression and posterior lumbar interbody fusion for the treatment of lumbar degenerative disease: a minimum 5-year follow-up study. J Clin Neurosci 35:24–29. https://doi.org/10.1016/j.jocn.2016.09.030
Zheng X, Chen Z, Yu H, Zhuang J, Yu H, Chang Y (2021) A minimum 8-year follow-up comparative study of decompression and coflex stabilization with decompression and fusion. Exp Ther Med 21:595. https://doi.org/10.3892/etm.2021.10027
Du MR, Wei FL, Zhu KL, Song RM, Huan Y, Jia B, Gu JT, Pan LX, Zhou HY, Qian JX, Zhou CP (2020) Coflex interspinous process dynamic stabilization for lumbar spinal stenosis: long-term follow-up. J Clin Neurosci 81:462–468. https://doi.org/10.1016/j.jocn.2020.09.040
Machado GC, Ferreira PH, Yoo RI, Harris IA, Pinheiro MB, Koes BW, van Tulder MW, Rzewuska M, Maher CG, Ferreira ML (2016) Surgical options for lumbar spinal stenosis. Cochrane Database Syst Rev 11:CD012421. doi: https://doi.org/10.1002/14651858.CD012421
Röder C, Baumgärtner B, Berlemann U, Aghayev E (2015) Superior outcomes of decompression with an interlaminar dynamic device versus decompression alone in patients with lumbar spinal stenosis and back pain: a cross registry study. Eur Spine J 24:2228–2235. https://doi.org/10.1007/s00586-015-4124-6
Galarza M, Gazzeri R, De la Rosa P, Martínez-Lage JF (2014) Microdiscectomy with and without insertion of interspinous device for herniated disc at the L5–S1 level. J Clin Neurosci 21:1934–1939. https://doi.org/10.1016/j.jocn.2014.02.029
Zhang Y, Lu D, Ji W, He F, Chen AC, Yang H, Zhu X (2021) Which is the most effective treatment for lumbar spinal stenosis: decompression, fusion, or interspinous process device? A Bayesian network meta-analysis. J Orthop Transl 26:45–53. https://doi.org/10.1016/j.jot.2020.07.003
Schmidt S, Franke J, Rauschmann M, Adelt D, Bonsanto MM, Sola S (2018) Prospective, randomized, multicenter study with 2-year follow-up to compare the performance of decompression with and without interlaminar stabilization. J Neurosurg Spine 28:406–415. https://doi.org/10.3171/2017.11.Spine17643
Krakowiak M, Rulewska N, Rudaś M, Broda M, Sabramowicz M, Jaremko A, Leki K, Sokal P (2022) Interspinous process devices do not reduce intervertebral foramina and discs heights on adjacent segments. J Pain Res 15:1971–1982. https://doi.org/10.2147/jpr.S356898
Celik H, Derincek A, Koksal I (2012) Surgical treatment of the spinal stenosis with an interspinous distraction device: do we really restore the foraminal height? Turk Neurosurg 22:50–54. https://doi.org/10.5137/1019-5149.Jtn.4681-11.2
Zhou L, Schneck CD, Shao ZH (2012) The anatomy of dorsal ramus nerves and its implications in lower back pain. Neurosci Med 3:192–201
Guo Z, Liu G, Wang L, Zhao Y, Zhao Y, Lu S, Cheng C (2022) Biomechanical effect of Coflex and X-STOP spacers on the lumbar spine: a finite element analysis. Am J Transl Res 14:5155–5163
Bae HW, Davis RJ, Lauryssen C, Leary S, Maislin G, Musacchio MJ Jr (2016) Three-year follow-up of the prospective, randomized, controlled trial of coflex interlaminar stabilization vs instrumented fusion in patients with lumbar stenosis. Neurosurgery 79:169–181. https://doi.org/10.1227/NEU.0000000000001237
Cho YJ, Park J-B, Chang D-G, Kim HJ (2021) 15-year survivorship analysis of an interspinous device in surgery for single-level lumbar disc herniation. BMC Musculoskelet Disord 22:1030. https://doi.org/10.1186/s12891-021-04929-8
Zhong J, O’Connell B, Balouch E, Stickley C, Leon C, O’Malley N, Protopsaltis TS, Kim YH, Maglaras C, Buckland AJ (2021) Patient outcomes after single-level coflex interspinous implants versus single-level laminectomy. Spine (Phila Pa 1976) 46:893–900. https://doi.org/10.1097/brs.0000000000003924
Deyo RA, Martin BI, Ching A, Tosteson AN, Jarvik JG, Kreuter W, Mirza SK (2013) Interspinous spacers compared with decompression or fusion for lumbar stenosis: complications and repeat operations in the medicare population. Spine (Phila Pa 1976) 38:865–872. https://doi.org/10.1097/BRS.0b013e31828631b8
Barbagallo GM, Olindo G, Corbino L, Albanese V (2009) Analysis of complications in patients treated with the X-stop interspinous process decompression system: proposal for a novel anatomic scoring system for patient selection and review of the literature. Neurosurgery 65:111–119. https://doi.org/10.1227/01.NEU.0000346254.07116.31
Lo HJ, Chen HM, Kuo YJ, Yang SW (2020) Effect of different designs of interspinous process devices on the instrumented and adjacent levels after double-level lumbar decompression surgery: a finite element analysis. PLoS ONE 15:e0244571. https://doi.org/10.1371/journal.pone.0244571
Richter A, Schütz C, Hauck M, Halm H (2010) Does an interspinous device (Coflex) improve the outcome of decompressive surgery in lumbar spinal stenosis? One-year follow up of a prospective case control study of 60 patients. Eur Spine J 19:283–289. https://doi.org/10.1007/s00586-009-1229-9
Acknowledgements
We would like to acknowledge Dr. Karthigesh Palanichami and Ms Nandika Naresh for their help in data collection and manuscript editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kumar, N., Thomas, A.C., Rajoo, M.S. et al. Evaluating 5-year outcomes of interlaminar devices as an adjunct to decompression for symptomatic lumbar spinal stenosis. Eur Spine J 32, 1367–1374 (2023). https://doi.org/10.1007/s00586-023-07610-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07610-x