Abstract
Purpose
Tenosynovial giant cell tumor of the diffuse type (TGCT-D) involving the spine is rare. Its differential diagnosis includes metastatic disease; however, there have been few reports of spinal TGCT-D mimicking spinal metastasis in patients with a history of malignancy.
Methods
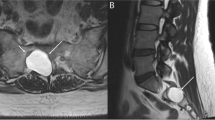
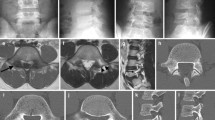
We report on a 35-year-old woman with a history of papillary thyroid cancer who was diagnosed with TGCT-D of the thoracic spine mimicking spinal metastasis. Preoperative computed tomography (CT) revealed a 1.0 × 1.0-cm lytic bone lesion involving the left T7 vertebral lamina, pedicle, and the T6–7 facet joint; the thoracic spine lesion was markedly fluorodeoxyglucose-avid on positron-emission tomography/computed tomography (PET/CT).
Results
Spinal metastasis was initially suspected given the patient’s history of papillary thyroid cancer. Total excision was performed with recapping laminoplasty. The resected lamina was frozen in liquid nitrogen and used as a frozen autograft (frozen recapping laminoplasty) for spinal reconstruction with posterior instrumentation. Histological findings supported a diagnosis of TGCT-D. The patient had no evidence of local recurrence 2 years post-surgery. Bone union was achieved 3 years post-surgery.
Conclusions
TGCT-D can mimic metastasis in PET/CT and should be included in the differential diagnosis if a lytic lesion affecting the posterior elements of the vertebrae involves the facet joints. CT-guided biopsy is recommended for accurate diagnosis when an occult tumor, such as TGCT, is incidentally detected on PET-CT, even in patients with a history of malignant neoplasm. Frozen recapping laminoplasty is useful for complete resection of a spinal tumor, preventing local recurrence, and preservation of the posterior spinal elements.







Similar content being viewed by others
References
Jaffe H, Lichtenstein L, Sutro C (1941) Pigmented villonodular synovitis, bursitis and tenosynovitis. Arch Pathol 31:731–765
Somerhausen N, Rijn M (2013) Tenosynovial giant cell tumour, diffuse type. In: Fletcher CD, Bridge JA, Hogendoorn PC, Mertens F (eds) WHO classification of tumours of soft tissue and bone, 4th edn. IARC, Lyon, pp 102–103
Byers PD, Cotton RE, Deacon OW, Lowy M, Newman PH, Sissons HA, Thomson AD (1968) The diagnosis and treatment of pigmented villonodular synovitis. J Bone Joint Surg Br 50:290–305
Mahmood S, de Llano SR (2007) Localized nodular synovitis mimicking metastatic melanoma in a patient with metastatic melanoma on whole-body F-18 FDG PET/CT with MRI and pathological correlation. Clin Nucl Med 32:532–534
Kitapci MT, Coleman RE (2003) Incidental detection of pigmented villonodular synovitis on FDG PET. Clin Nucl Med 28:668–669
Takeuchi A, Yamamoto N, Hayashi K, Miwa S, Takahira M, Fukui K, Oikawa T, Tsuchiya H (2016) Tenosynovial giant cell tumors in unusual locations detected by positron emission tomography imaging confused with malignant tumors: report of two cases. BMC Musculoskelet Disord 17:180
Selby L, Kukar M, Wang J, Beg M, Sullivan J (2014) Pigmented villous nodular synovitis mimicking metastatic melanoma on PET-CT. Int J Surg Case Rep 5:231–233
Chang KJ, Byun BH, Moon HS, Park J, Koh JS, Kim BI, Lim SM (2014) Tenosynovial giant cell tumor of diffuse type mimicking bony metastasis detected on F-18 FDG PET/CT. Nucl Med Mol Imaging 48:230–232
Pallas A, Hagge R, Borys D, Hunter J (2009) Intense FDG uptake in an intra-articular localized giant-cell tumor of the tendon sheath (pigmented villonodular synovitis) mimics metastatic melanoma. Radiol Case Rep 4:343
Elumogo CO, Kochenderfer JN, Civelek AC, Bluemke DA (2016) Pigmented villonodular synovitis mimics metastases on fluorine 18 fluorodeoxyglucose position emission tomography-computed tomography. Quant Imaging Med Surg 6:218–223
Lavrador JP, Oliveira E, Gil N, Francisco AF, Livraghi S (2015) C1–C2 pigmented villonodular synovitis and clear cell carcinoma: unexpected presentation of a rare disease and a review of the literature. Eur Spine J 24(Suppl 4):S465–S471
Tomita K, Kawahara N (1996) The threadwire saw: a new device for cutting bone. J Bone Joint Surg Am 78:1915–1917
Kawahara N, Tomita K, Shinya Y, Matsumoto T, Baba H, Fujita T, Murakami H, Kobayashi T (1999) Recapping T-saw laminoplasty for spinal cord tumors. Spine (Phila Pa 1976) 24(13):1363–1370
Kawahara N, Tomita K, Abdel-Wanis ME, Fujita T, Murakami H, Demura S (2009) Recapping T-saw laminocostotransversoplasty for ventral meningiomas in the thoracic region. J Orthop Sci. 14(5):548–555
Myers BW, Masi AT (1980) Pigmented villonodular synovitis and tenosynovitis: a clinical epidemiologic study of 166 cases and literature review. Medicine (Baltimore) 59:223–238
Patel KH, Gikas PD, Pollock RC, Carrington RW, Cannon SR, Skinner JA, Briggs TW, Aston WJS (2017) Pigmented villonodular synovitis of the knee: a retrospective analysis of 214 cases at a UK tertiary referral centre. Knee 24:808–815
Koontz NA, Quigley EP, Witt BL, Sanders RK, Shah LM (2016) Pigmented villonodular synovitis of the cervical spine: case report and review of the literature. BJR Case Rep 2:20150264
Roguski M, Safain MG, Zerris VA, Kryzanski JT, Thomas CB, Magge SN, Riesenburger RI (2014) Pigmented villonodular synovitis of the thoracic spine. J Clin Neurosci 21:1679–1685
Watanabe H, Shinozaki T, Yanagawa T, Aoki J, Tokunaga M, Inoue T, Endo K, Mohara S, Sano K, Takagishi K (2000) Glucose metabolic analysis of musculoskeletal tumours using 18fluorine-FDG PET as an aid to preoperative planning. J Bone Joint Surg Br 82:760–767
Flipo RM, Chastanet P, Duquesnoy B (1993) Imaging of pigmented villonodular synovitis. Presse Med 22:591–594
An C, Lee YH, Kim S, Cho HW, Suh JS, Song HT (2013) Characteristic MRI findings of spinal metastases from various primary cancers: retrospective study of pathologically-confirmed cases. J Korean Soc Magn Reson Med 17:8–18
Parmar HA, Sitoh YY, Tan KK, Teo J, Ibet SM, Hui F (2004) MR imaging features of pigmented villonodular synovitis of the cervical spine. AJNR Am J Neuroradiol 25:146–149
Motamedi K, Murphey MD, Fetsch JF, Furlong MA, Vinh TN, Laskin WB, Sweet DE (2005) Villonodular synovitis (PVNS) of the spine. Skelet Radiol 34:185–195
Wu K, Hou SM, Huang TS, Yang RS (2008) Thyroid carcinoma with bone metastases: a prognostic factor study. Clin Med Oncol 2:129–134
Pittas AG, Adler M, Fazzari M, Tickoo S, Rosai J, Larson SM, Robbins RJ (2000) Bone metastases from thyroid carcinoma: clinical characteristics and prognostic variables in one hundred forty-six patients. Thyroid 10:261–268
Farooki A, Leung V, Tala H, Tuttle RM (2012) Skeletal-related events due to bone metastases from differentiated thyroid cancer. J Clin Endocrinol Metab 97:2433–2439
Kushchayeva YS, Kushchayev SV, Carroll NM, Felger EA, Links TP, Teytelboym OM, Bonichon F, Preul MC, Sonntag VK, Van Nostrand D, Burman KD, Boyle LM (2014) Spinal metastases due to thyroid carcinoma: an analysis of 202 patients. Thyroid 24:1488–1500
Tsuchiya H, Wan SL, Sakayama K, Yamamoto N, Nishida H, Tomita K (2005) Reconstruction using an autograft containing tumor treated by liquid nitrogen. J Bone Joint Surg Br 87:218–225
Yamamoto N, Tsuchiya H, Tomita K (2003) Effects of liquid nitrogen treatment on the proliferation of osteosarcomas and biomechanical properties of normal bone. J Orthop Sci 8:374–380
Takata M, Sugimoto N, Yamamoto N, Shirai T, Hayashi K, Nishida H, Tanzawa Y, Kimura H, Miwa S, Takeuchi A, Tsuchiya H (2011) Activity of bone morphogenetic protein-7 after treatment at various temperatures: freezing vs. pasteurization vs. allograft. Cryobiology 63:235–239
Igarashi K, Yamamoto N, Shirai T, Hayashi K, Nishida H, Kimura H, Takeuchi A, Tsuchiya H (2014) The long-term outcome following the use of frozen autograft treated with liquid nitrogen in the management of bone and soft-tissue sarcomas. Bone Joint J 96(4):555–561
Giannini C, Scheithauer BW, Wenger DE, Unni KK (1996) Pigmented villonodular synovitis of the spine: a clinical, radiological, and morphological study of 12 cases. J Neurosurg 84:592–597
Zettinig G, Fueger BJ, Passler C, Kaserer K, Pirich C, Dudczak R, Niederle B (2002) Long-term follow-up of patients with bone metastases from differentiated thyroid carcinoma—surgery or conventional therapy? Clin Endocrinol (Oxf) 56:377–382
Demura S, Kawahara N, Murakami H, Abdel-Wanis ME, Kato S, Yoshioka K, Tomita K, Tsuchiya H (2011) Total en bloc spondylectomy for spinal metastases in thyroid carcinoma. J Neurosurg Spine 14:172–176
Kato S, Murakami H, Demura S, Fujimaki Y, Yoshioka K, Yokogawa N, Tsuchiya H (2016) The impact of complete surgical resection of spinal metastases on the survival of patients with thyroid cancer. Cancer Med 5:2343–2349
Acknowledgements
We would like to thank Editage (http://www.editage.jp) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
N. Yonezawa, H. Murakami, S. Kato, H. Hayashi, and H. Tsuchiya declare that they have no conflict of interest. This study was not funded by any external source.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from the patient described in the study.
Rights and permissions
About this article
Cite this article
Yonezawa, N., Murakami, H., Kato, S. et al. Successful treatment of a diffuse type tenosynovial giant cell tumor in the thoracic spine mimicking spinal metastasis by frozen recapping laminoplasty in a patient with thyroid cancer. Eur Spine J 27 (Suppl 3), 526–532 (2018). https://doi.org/10.1007/s00586-018-5603-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-018-5603-3