Abstract
Purpose
Many studies have reported on the segmental motion range of the lumbar spine using various in vitro and in vivo experimental designs. However, the in vivo weightbearing dynamic motion characteristics of the L4–5 and L5–S1 motion segments are still not clearly described in literature. This study investigated in vivo motion of the lumbar spine during a weight-lifting activity.
Methods
Ten asymptomatic subjects (M/F: 5/5; age: 40–60 years) were recruited. The lumbar segment of each subject was MRI-scanned to construct 3D models of the L2–S1 vertebrae. The lumbar spine was then imaged using a dual fluoroscopic imaging system as the subject performed a weight-lifting activity from a lumbar flexion position (45°) to maximal extension position. The 3D vertebral models and the fluoroscopic images were used to reproduce the in vivo vertebral positions along the motion path. The relative translations and rotations of each motion segment were analyzed.
Results
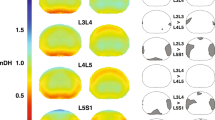
All vertebral motion segments, L2–3, L3–4, L4–5 and L5–S1, rotated similarly during the lifting motion. L4–5 showed the largest anterior-posterior (AP) translation with 2.9 ± 1.5 mm and was significantly larger than L5–S1 (p < 0.05). L5–S1 showed the largest proximal–distal (PD) translation with 2.8 ± 0.9 mm and was significantly larger than all other motion segments (p < 0.05).
Conclusions
The lower lumbar motion segments L4–5 and L5–S1 showed larger AP and PD translations, respectively, than the higher vertebral motion segments during the weight-lifting motion. The data provide insight into the physiological motion characteristics of the lumbar spine and potential mechanical mechanisms of lumbar disease development.




Similar content being viewed by others
References
Gilbert JW, Martin JC, Wheeler GR, Storey BB, Mick GE, Richardson GB, Herder SL, Gyarteng-Dakwa K, Broughton PG (2010) Lumbar disk protrusion rates of symptomatic patients using magnetic resonance imaging. J Manipulative Physiol Ther 33:626–629. doi:10.1016/j.jmpt.2010.08.010
Biluts H, Munie T, Abebe M (2012) Review of lumbar disc diseases at Tikur Anbessa Hospital. Ethiop Med J 50:57–65
Kuisma M, Karppinen J, Niinimaki J, Ojala R, Haapea M, Heliovaara M, Korpelainen R, Taimela S, Natri A, Tervonen O (2007) Modic changes in endplates of lumbar vertebral bodies: prevalence and association with low back and sciatic pain among middle-aged male workers. Spine 32:1116–1122. doi:10.1097/01.brs.0000261561.12944.ff
Evans W, Jobe W, Seibert C (1989) A cross-sectional prevalence study of lumbar disc degeneration in a working population. Spine 14:60–64
Takatalo J, Karppinen J, Niinimaki J, Taimela S, Nayha S, Jarvelin MR, Kyllonen E, Tervonen O (2009) Prevalence of degenerative imaging findings in lumbar magnetic resonance imaging among young adults. Spine 34:1716–1721. doi:10.1097/BRS.0b013e3181ac5fec
Cheung KM, Karppinen J, Chan D, Ho DW, Song YQ, Sham P, Cheah KS, Leong JC, Luk KD (2009) Prevalence and pattern of lumbar magnetic resonance imaging changes in a population study of one thousand forty-three individuals. Spine 34:934–940. doi:10.1097/BRS.0b013e3181a01b3f
Kanayama M, Togawa D, Takahashi C, Terai T, Hashimoto T (2009) Cross-sectional magnetic resonance imaging study of lumbar disc degeneration in 200 healthy individuals. J Neurosurg Spine 11:501–507. doi:10.3171/2009.5.SPINE08675
Rosenberg NJ (1975) Degenerative spondylolisthesis. Predisposing factors. J Bone Joint Surg Am 57:467–474
Herkowitz HN, Garfin SR, Eismont FJ, Bell GR, Balderston RA (2011) Rothman-Simeone the spine, 6th edn. Saunders Elsevier, Philadelphia
Iguchi T, Wakami T, Kurihara A, Kasahara K, Yoshiya S, Nishida K (2002) Lumbar multilevel degenerative spondylolisthesis: radiological evaluation and factors related to anterolisthesis and retrolisthesis. J Spinal Disord Tech 15:93–99
Friberg O (1987) Lumbar instability: a dynamic approach by traction-compression radiography. Spine 12:119–129
Sato H, Kikuchi S (1993) The natural history of radiographic instability of the lumbar spine. Spine 18:2075–2079
Iguchi T, Kanemura A, Kasahara K, Sato K, Kurihara A, Yoshiya S, Nishida K, Miyamoto H, Doita M (2004) Lumbar instability and clinical symptoms: which is the more critical factor for symptoms: sagittal translation or segment angulation? J Spinal Disord Tech 17:284–290
Kanemura A, Doita M, Kasahara K, Sumi M, Kurosaka M, Iguchi T (2009) The influence of sagittal instability factors on clinical lumbar spinal symptoms. J Spinal Disord Tech 22:479–485. doi:10.1097/BSD.0b013e31818d1b18
Auerbach JD, Wills BP, McIntosh TC, Balderston RA (2007) Evaluation of spinal kinematics following lumbar total disc replacement and circumferential fusion using in vivo fluoroscopy. Spine 32:527–536. doi:10.1097/01.brs.0000256915.90236.17
Kettler A, Marin F, Sattelmayer G, Mohr M, Mannel H, Durselen L, Claes L, Wilke HJ (2004) Finite helical axes of motion are a useful tool to describe the three-dimensional in vitro kinematics of the intact, injured and stabilised spine. Eur Spine J 13:553–559. doi:10.1007/s00586-004-0710-8
Lindsey DP, Swanson KE, Fuchs P, Hsu KY, Zucherman JF, Yerby SA (2003) The effects of an interspinous implant on the kinematics of the instrumented and adjacent levels in the lumbar spine. Spine 28:2192–2197. doi:10.1097/01.BRS.0000084877.88192.8E
el SariAli H, Lemaire JP, Pascal-Mousselard H, Carrier H, Skalli W (2006) In vivo study of the kinematics in axial rotation of the lumbar spine after total intervertebral disc replacement: long-term results: a 10–14 years follow up evaluation. Eur Spine J 15:1501–1510. doi:10.1007/s00586-005-0016-5
Siddiqui M, Karadimas E, Nicol M, Smith FW, Wardlaw D (2006) Effects of X-STOP device on sagittal lumbar spine kinematics in spinal stenosis. J Spinal Disord Tech 19:328–333. doi:10.1097/01.bsd.0000211297.52260.d5
Wong KW, Luk KD, Leong JC, Wong SF, Wong KK (2006) Continuous dynamic spinal motion analysis. Spine 31:414–419. doi:10.1097/01.brs.0000199955.87517.82
Zhu Q, Larson CR, Sjovold SG, Rosler DM, Keynan O, Wilson DR, Cripton PA, Oxland TR (2007) Biomechanical evaluation of the Total Facet Arthroplasty System: 3-dimensional kinematics. Spine 32:55–62. doi:10.1097/01.brs.0000250983.91339.9f
Bible JE, Biswas D, Miller CP, Whang PG, Grauer JN (2010) Normal functional range of motion of the lumbar spine during 15 activities of daily living. J Spinal Disord Tech 23:106–112. doi:10.1097/BSD.0b013e3181981823
Chleboun GS, Amway MJ, Hill JG, Root KJ, Murray HC, Sergeev AV (2012) Measurement of segmental lumbar spine flexion and extension using ultrasound imaging. J Orthop Sports Phys Ther 42:880–885. doi:10.2519/jospt.2012.3915
Hashemirad F, Hatef B, Jaberzadeh S, Ale Agha N (2013) Validity and reliability of skin markers for measurement of intersegmental mobility at L2-3 and L3-4 during lateral bending in healthy individuals: a fluoroscopy study. J Bodyw Mov Ther 17:46–52. doi:10.1016/j.jbmt.2012.04.010
Takayanagi K, Takahashi K, Yamagata M, Moriya H, Kitahara H, Tamaki T (2001) Using cineradiography for continuous dynamic-motion analysis of the lumbar spine. Spine 26:1858–1865
Yamamoto I, Panjabi MM, Crisco T, Oxland T (1989) Three-dimensional movements of the whole lumbar spine and lumbosacral joint. Spine 14:1256–1260
Panjabi M, Yamamoto I, Oxland T, Crisco J (1989) How does posture affect coupling in the lumbar spine? Spine 14:1002–1011
Mimura M, Panjabi MM, Oxland TR, Crisco JJ, Yamamoto I, Vasavada A (1994) Disc degeneration affects the multidirectional flexibility of the lumbar spine. Spine 19:1371–1380
Fujiwara A, An HS, Lim TH, Haughton VM (2001) Morphologic changes in the lumbar intervertebral foramen due to flexion-extension, lateral bending, and axial rotation: an in vitro anatomic and biomechanical study. Spine 26:876–882
Abumi K, Panjabi MM, Kramer KM, Duranceau J, Oxland T, Crisco JJ (1990) Biomechanical evaluation of lumbar spinal stability after graded facetectomies. Spine 15:1142–1147
Hayes MA, Howard TC, Gruel CR, Kopta JA (1989) Roentgenographic evaluation of lumbar spine flexion–extension in asymptomatic individuals. Spine 14:327–331
Dvorak J, Panjabi MM, Chang DG, Theiler R, Grob D (1991) Functional radiographic diagnosis of the lumbar spine. Flexion–extension and lateral bending. Spine 16:562–571
Boden SD, Wiesel SW (1990) Lumbosacral segmental motion in normal individuals. Have we been measuring instability properly? Spine 15:571–576
Miyasaka K, Ohmori K, Suzuki K, Inoue H (2000) Radiographic analysis of lumbar motion in relation to lumbosacral stability. Investigation of moderate and maximum motion. Spine 25:732–737
Li G, Wang S, Passias P, Xia Q, Wood K (2009) Segmental in vivo vertebral motion during functional human lumbar spine activities. Eur Spine J 18:1013–1021. doi:10.1007/s00586-009-0936-6
Pearcy MJ (1985) Stereo radiography of lumbar spine motion. Acta Orthop Scand Suppl 212:1–45
Ahmadi A, Maroufi N, Behtash H, Zekavat H, Parnianpour M (2009) Kinematic analysis of dynamic lumbar motion in patients with lumbar segmental instability using digital videofluoroscopy. Eur Spine J 18:1677–1685. doi:10.1007/s00586-009-1147-x
Passias PG, Wang S, Kozanek M, Xia Q, Li W, Grottkau B, Wood KB, Li G (2011) Segmental lumbar rotation in patients with discogenic low back pain during functional weight-bearing activities. J Bone Joint Surg Am 93:29–37. doi:10.2106/JBJS.I.01348
Li W, Wang S, Xia Q, Passias P, Kozanek M, Wood K, Li G (2011) Lumbar facet joint motion in patients with degenerative disc disease at affected and adjacent levels: an in vivo biomechanical study. Spine 36:E629–E637. doi:10.1097/BRS.0b013e3181faaef7
Shin JH, Wang S, Yao Q, Wood KB, Li G (2013) Investigation of coupled bending of the lumbar spine during dynamic axial rotation of the body. Eur Spine J 22:2671–2677. doi:10.1007/s00586-013-2777-6
Mundt DJ, Kelsey JL, Golden AL, Pastides H, Berg AT, Sklar J, Hosea T, Panjabi MM (1993) An epidemiologic study of non-occupational lifting as a risk factor for herniated lumbar intervertebral disc. The northeast collaborative group on low back pain. Spine 18:595–602
Kelsey JL, Golden AL, Mundt DJ (1990) Low back pain/prolapsed lumbar intervertebral disc. Rheum Dis Clin North Am 16:699–716
Li G, DeFrate LE, Park SE, Gill TJ, Rubash HE (2005) In vivo articular cartilage contact kinematics of the knee: an investigation using dual-orthogonal fluoroscopy and magnetic resonance image-based computer models. Am J Sports Med 33:102–107
Wang S, Passias P, Li G, Li G, Wood K (2008) Measurement of vertebral kinematics using noninvasive image matching method-validation and application. Spine 33:E355–E361. doi:10.1097/BRS.0b013e3181715295
Hanson GR, Suggs JF, Freiberg AA, Durbhakula S, Li G (2006) Investigation of in vivo 6DOF total knee arthoplasty kinematics using a dual orthogonal fluoroscopic system. J Orthop Res 24:974–981. doi:10.1002/jor.20141
Bingham J, Li G (2006) An optimized image matching method for determining in vivo TKA kinematics with a dual-orthogonal fluoroscopic imaging system. J Biomech Eng 128:588–595. doi:10.1115/1.2205865
Li G, Van de Velde SK, Bingham J (2008) Validation of a non-invasive fluoroscopic imaging technique for the measurement of dynamic knee joint motion. J Biomech 41(7):1616–1622
Rozumalski A, Schwartz MH, Wervey R, Swanson A, Dykes DC, Novacheck T (2008) The in vivo three-dimensional motion of the human lumbar spine during gait. Gait Posture 28:378–384. doi:10.1016/j.gaitpost.2008.05.005
Pearcy M, Portek I, Shepherd J (1984) Three-dimensional x-ray analysis of normal movement in the lumbar spine. Spine 9:294–297
Bogduk N, Twomey LT (1987) Clinical anatomy of the lumbar spine. Churchill Livingstone, Melbourne, Edinburgh, London, New York
Masharawi Y, Rothschild B, Dar G, Peleg S, Robinson D, Been E, Hershkovitz I (2004) Facet orientation in the thoracolumbar spine: three-dimensional anatomic and biomechanical analysis. Spine 29:1755–1763
Kozanek M, Wang S, Passias PG, Xia Q, Li G, Bono CM, Wood KB, Li G (2009) Range of motion and orientation of the lumbar facet joints in vivo. Spine 34:E689–E696. doi:10.1097/BRS.0b013e3181ab4456
Spangfort EV (1972) The lumbar disc herniation. A computer-aided analysis of 2,504 operations. Acta Orthop Scand Suppl 142:1–95
Siepe CJ, Mayer HM, Heinz-Leisenheimer M, Korge A (2007) Total lumbar disc replacement: different results for different levels. Spine 32:782–790. doi:10.1097/01.brs.0000259071.64027.04
Dewing CB, Provencher MT, Riffenburgh RH, Kerr S, Manos RE (2008) The outcomes of lumbar microdiscectomy in a young, active population: correlation by herniation type and level. Spine 33:33–38. doi:10.1097/BRS.0b013e31815e3a42
Sinigaglia R, Bundy A, Costantini S, Nena U, Finocchiaro F, Monterumici DA (2009) Comparison of single-level L4-L5 versus L5-S1 lumbar disc replacement: results and prognostic factors. Eur Spine J 18(Suppl 1):52–63. doi:10.1007/s00586-009-0992-y
Okoro T, Sell P (2010) A short report comparing outcomes between L4/L5 and L5/S1 single-level discectomy surgery. J Spinal Disord Tech 23:40–42. doi:10.1097/BSD.0b013e3181b38537
Roussouly P, Gollogly S, Berthonnaud E, Dimnet J (2005) Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine 30:346–353
Acknowledgments
The authors would like to gratefully acknowledge the financial support from the National Institute of Health (R21AR057989), Synthes, Inc., and the Department of Orthopaedic Surgery at Massachusetts General Hospital.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
M. Wu and S. Wang contributed equally to this study.
Appendix: Validation of the DFIS technique in measurement of dynamic human lumbar motion
Appendix: Validation of the DFIS technique in measurement of dynamic human lumbar motion
Experiment setup
A validation study was performed to evaluate the accuracy of the DFIS technique when used to determine human lumbar spine kinematics during dynamic motion. In this validation, a cadaveric human body segment from feet to chest was acquired. The body segment included the entire lumbar spine and had all the surrounding soft tissues intact. Titanium beads (MRI compatible) of 4 mm in diameter were implanted into the L3, L4 and L5 vertebrae by a spine surgeon (Fig. 5). The lumbar spine was then MRI-scanned using the protocol described in the Sect. “Materials and methods”. The contours of L3, L4, L5 vertebrae and the beads were digitized from the MR images to reconstruct their 3D mesh models. A local coordinate system was created for each spine vertebral segment model as described in our previous study [35]. The specimen was then placed in a sitting position and the lumbar spine was manually flexed to simulate a dynamic physiologic flexion–extension motion at a rotation speed of ~50°/second. The test was guided using a timer. Dynamic orthogonal images of the lumbar spine were taken simultaneously from the anteromedial and anterolateral directions using two fluoroscopes (Fig. 2a).
The spatial positions of the vertebral bodies during the flexion–extension motion were reproduced in Rhinoceros® software through 3D to 2D imaging matching (Fig. 6), as described in the Sect. “Materials and Method”. To evaluate the accuracy of the image matching technique of DFIS in reproducing vertebral motion, five positions were chosen along the dynamic motion path of the spine: maximum flexion, middle flexion, upright, middle extension and maximum extension. Each position was independently reproduced using both the vertebral body matching technique (DFIS method) and the beads position matching technique (RSA method––gold standard) [35]. The positions and orientations of each vertebra determined using the DFIS and RSA methods were compared to evaluate the accuracy of the DFIS method in determination of dynamic lumbar kinematics.
Results
The model matching process showed a high accuracy in determination of the positions of the spinal segments (see Table 2). The average translational and rotational accuracy of L3, L4 and L5 vertebrae were within 0.3 mm and 0.7° from the five tested positions along the flexion–extension path.
Rights and permissions
About this article
Cite this article
Wu, M., Wang, S., Driscoll, S.J. et al. Dynamic motion characteristics of the lower lumbar spine: implication to lumbar pathology and surgical treatment. Eur Spine J 23, 2350–2358 (2014). https://doi.org/10.1007/s00586-014-3316-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3316-9