Abstract
Background
Small bowel cancer is not a single entity. Population-based studies taking into account histological diversity are scarce. The aim of this study was to report on their trends in incidence by histology in France over the past 20 years.
Methods
All patients with a small bowel cancer diagnosed in 15 French administrative areas covered by a registry from the network of French cancer registries (FRANCIM) were included. Age-standardized incidence rates were estimated using the world standard population. Incidence rates were calculated by gender, age group, histology, and 5-year period.
Results
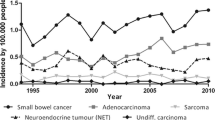
The overall age-standardized incidence rates were 1.46/100,000 inhabitants in men and 0.9/100,000 inhabitants in women. Adenocarcinoma was the most common histological type (38%), followed by neuroendocrine tumors (35%), lymphoma (15%) and sarcoma (12%). Age at diagnosis and tumor location differed between adenocarcinoma and neuroendocrine tumors. The incidence of all four tumor types increased significantly over the 20-year period, with the exception of lymphoma in men. The annual percentage change for neuroendocrine tumors was 3.89% in men and 3.61% in women; for sarcoma, it was 3.38% and 4.08%, respectively. The incidence of adenocarcinoma and lymphoma also increased in women with an annual percentage change of 3.05% and 3.32%, respectively.
Conclusion
Small bowel cancer incidence has increased over time. This increase occurred with different amplitudes and patterns in the four major histological types. The improvement in imaging techniques could partly explain this increase. It is necessary to determine whether predisposing conditions may contribute to this change.

Similar content being viewed by others
References
Surveillance, Epidemiology, and End Results (SEER) Program. SEER*Stat Database: Incidence—SEER 18 Regs Research Data + Hurricane Katrina Impacted Louisiana Cases, Nov 2015 Sub (1973–2013 Varying)—Linked To County Attributes—Total U.S., 1969–2014 Counties, National Cancer Institute, DCCPS, Surveillance Research Program, Surveillance Systems Branch, Released April 2016, Based on the November 2015. https://seer.cancer.gov/statfacts/html/smint.html. Accessed 15 Feb 2019.
Defossez G, Le Guyader-Peyrou S, Uhry Z, et al. Estimations nationales de l’incidence et de la mortalité par cancer en France métropolitaine entre 1990 et 2018. Étude à partir des registres des cancers du réseau Francim. Rapport. Saint-Maurice (Fra): Santé publique France, 2019. 161 p. http://www.santepubliquefrance.fr. Accessed 15 Feb 2019.
Kotz SJN, Read CB. Encyclopedia of statistical sciences. New York: Wiley; 1988.
Bilimoria KY, Bentrem DJ, Wayne JD, et al. Small bowel cancer in the United States: changes in epidemiology, treatment, and survival over the last 20 years. Ann Surg. 2009;249:63–71.
Dasari A, Shen C, Halperin D, et al. Trends in the incidence, prevalence, and survival outcomes in patients with neuroendocrine tumors in the United States. JAMA Oncol. 2017;3:1335–42.
Shack LG, Wood HE, Kang JY, et al. Small intestinal cancer in England & Wales and Scotland: time trends in incidence, mortality and survival. Aliment Pharmacol Ther. 2006;23:1297–306.
Sakae H, Kanzaki H, Nasu J, et al. The characteristics and outcomes of small bowel adenocarcinoma: a multicentre retrospective observational study. Br J Cancer. 2017;117:1607–13.
Lepage C, Bouvier AM, Manfredi S, et al. Incidence and management of primary malignant small bowel cancers: a well-defined French population study. Am J Gastroenterol. 2006;101:2826–32.
Goodman MT, Matsuno RK, Shvetsov YB. Racial and ethnic variation in the incidence of small-bowel cancer subtypes in the United States, 1995–2008. Dis Colon Rectum. 2013;56:441–8.
Bernstein H, Bernstein C, Payne CM, et al. Bile acids as endogenous etiologic agents in gastrointestinal cancer. World J Gastroenterol. 2009;15:3329–40.
Delaunoit T, Neczyporenko F, Limburg PJ, et al. Pathogenesis and risk factors of small bowel adenocarcinoma: a colorectal cancer sibling? Am J Gastroenterol. 2005;100:703–10.
Raghav K, Overman MJ. Small bowel adenocarcinomas—existing evidence and evolving paradigms. Nat Rev Clin Oncol. 2013;10:534–44.
Chow WH, Linet MS, McLaughlin JK, et al. Risk factors for small intestine cancer. Cancer Causes Control. 1993;4:163–9.
Negri E, Bosetti C, La Vecchia C, et al. Risk factors for adenocarcinoma of the small intestine. Int J Cancer. 1999;82:171–4.
Bennett CM, Coleman HG, Veal PG, et al. Lifestyle factors and small intestine adenocarcinoma risk: a systematic review and meta-analysis. Cancer Epidemiol. 2015;39:265–73.
Aparicio T, Zaanan A, Svrcek M, et al. Small bowel adenocarcinoma: epidemiology, risk factors, diagnosis and treatment. Dig Liver Dis. 2014;46:97–104.
Watson P, Vasen HFA, Mecklin JP, et al. The risk of extra-colonic, extra-endometrial cancer in the Lynch syndrome. Int J Cancer. 2008;123:444–9.
Bonadona V, Bonaiti B, Olschwang S, et al. Cancer risks associated with germline mutations in MLH1, MSH2, and MSH6 genes in Lynch syndrome. JAMA. 2011;305:2304–10.
ten Kate GL, Kleibeuker JH, Nagengast FM, et al. Is surveillance of the small bowel indicated for Lynch syndrome families? Gut. 2007;56:1198–201.
Offerhaus GJ, Giardiello FM, Krush AJ, et al. The risk of upper gastrointestinal cancer in familial adenomatous polyposis. Gastroenterology. 1992;102:1980–2.
Warth A, Kloor M, Schirmacher P, et al. Genetics and epigenetics of small bowel adenocarcinoma: the interactions of CIN, MSI, and CIMP. Mod Pathol. 2011;24:564–70.
Bernstein CN, Blanchard JF, Kliewer E, et al. Cancer risk in patients with inflammatory bowel disease: a population-based study. Cancer. 2001;91:854–62.
Jess T, Loftus EV Jr, Velayos FS, et al. Risk of intestinal cancer in inflammatory bowel disease: a population-based study from Olmsted county, Minnesota. Gastroenterology. 2006;130:1039–46.
Palascak-Juif V, Bouvier AM, Cosnes J, et al. Small bowel adenocarcinoma in patients with Crohn’s disease compared with small bowel adenocarcinoma de novo. Inflamm Bowel Dis. 2005;11:828–32.
Bojesen RD, Riis LB, Hogdall E, et al. Inflammatory bowel disease and small bowel cancer risk, clinical characteristics, and histopathology: a population-based study. Clin Gastroenterol Hepatol. 2017;15(1900–7):e2.
Askling J, Linet M, Gridley G, et al. Cancer incidence in a population-based cohort of individuals hospitalized with celiac disease or dermatitis herpetiformis. Gastroenterology. 2002;123:1428–35.
Howdle PD, Jalal PK, Holmes GK, et al. Primary small-bowel malignancy in the UK and its association with coeliac disease. QJM. 2003;96:345–53.
Solcia E, Vanoli A. Histogenesis and natural history of gut neuroendocrine tumors: present status. Endocr Pathol. 2014;25:165–70.
Ghimire P, Wu GY, Zhu L. Primary gastrointestinal lymphoma. World J Gastroenterol. 2011;17:697–707.
Malamut G, Chandesris O, Verkarre V, et al. Enteropathy associated T cell lymphoma in celiac disease: a large retrospective study. Dig Liver Dis. 2013;45:377–84.
Schottenfeld D, Beebe-Dimmer JL, Vigneau FD. The epidemiology and pathogenesis of neoplasia in the small intestine. Ann Epidemiol. 2009;19:58–69.
Shenoy S. Small bowel sarcoma: tumor biology and advances in therapeutics. Surg Oncol. 2015;24:136–44.
Acknowledgements
Zoe Uhry (Biostatistique-Bioinformatique, Hospices Civils de Lyon, F-69003, Département des Maladies, Non Transmissible et des Traumatismes, Santé Publique France, France) for maintaining and extracting data from the common FRANCIM database.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any conflicts of interest to declare regarding this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bouvier, AM., Robaszkiewicz, M., Jooste, V. et al. Trends in incidence of small bowel cancer according to histology: a population-based study. J Gastroenterol 55, 181–188 (2020). https://doi.org/10.1007/s00535-019-01636-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-019-01636-z