Abstract
Purpose
To identify the most effective dressing for application to surgical wounds with primary closure to prevent surgical site infection (SSI) in adult patients with cancer undergoing elective surgeries.
Methods
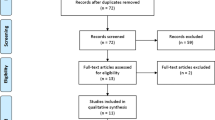
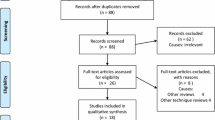
This systematic review was based on the Preferred Reporting Items for Systematic Reviews and Meta-Analysis, with online searches conducted in the CINHAL, Cochrane Central, LILACS, PubMed, Scopus, Embase, Livivo, and Web of Science databases. An additional search was conducted in gray literature using Google Scholar. The risk of bias was assessed using RoB 2.0. The certainty of evidence was evaluated using the Grading of Recommendations Assessment and Development and Evaluation, and the results were synthesized in a descriptive manner and using meta-analysis.
Results
Eleven randomized clinical trials were conducted to compare different types of dressing—silver dressing with absorbent dressing (n = 3), mupirocin dressing with paraffin/no dressing (n = 1), honey-based dressing with absorbent dressing (n = 1), vitamin E and silicone-containing dressing with absorbent dressing (n = 1), and negative pressure wound therapy with absorbent dressing (n = 4)—and compare the usage duration of absorbent dressing (n = 1). Nine trials presented a low risk of bias, and two were classified as having uncertain bias. Compared with absorbent dressing, silver dressing did not reduce the risk of developing any type of SSI in 894 clinical trial participants (risk relative RR: 0.72; 95% confidence interval [CI] [0.44, 1.17] p = 0.18). Compared with absorbent dressing, negative pressure wound therapy did not reduce the risk of developing any type of SSI in the 1041 participants of two clinical trials (RR 0.68; 95% CI [0.31, 1.26] p = 0.22). The certainty of evidence of the three meta-analyses was considered low or very low for the prevention of SSI. We believe that this low certainty of evidence can be improved by conducting new studies in the future.
Conclusion
There is no evidence regarding which dressing is the most effective in preventing SSI in adult patients with cancer.
Similar content being viewed by others
Data Availability
Data supporting this review are available within the study and its supplementary material.
References
Ferlay J, Colombet M, Soerjomataram I, Parkin DM, Piñeros M, Znaor A et al (2021) Cancer statistics for the year 2020: an overview. Int J Cancer 148:2863–3122. https://doi.org/10.1002/ijc.33588
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: Cancer J Clin 71:1–41. https://doi.org/10.3322/caac.21660
Instituto Nacional de Câncer (2019) Estimativa 2020: incidência de câncer no Brasil. INCA. https://www.inca.gov.br/publicacoes/livros/estimativa-2020-incidencia-de-cancer-no-brasil. Accessed 20 April 2021
Brierley R, Collingridge D (2015) Cancer surgery: a vital specialty to prevent premature death. Lancet Oncol 16:1187. https://doi.org/10.1016/s1470-2045(15)00306-x
Sullivan R, Alatise OI, Anderson BO, Audisio R, Autier P, Aggarwal A et al (2015) Global cancer surgery: delivering safe, affordable, and timely cancer surgery. Lancet Oncol 16:1193–1224. https://doi.org/10.1016/S1470-2045(15)00223-5
Vieira SC, Lustosa AML, Barbosa CNB, Teixeira JMR, Brito LXE, Soares LFM, et al. (2012) Oncologia básica. Fundação Quixote. http://doutorsabas.com.br/wp-content/uploads/2018/04/Livro-Oncologia-Ba%CC%81sica.pdf. Accessed 12 May 2021
Berríos-Torres SI, Umscheid CA, Bratzler DW, Leas B, Stone EC, Kelz RR et al (2017) Centers for Disease Control and Prevention guideline for the prevention of surgical site infection, 2017. JAMA Surg 152:784–791. https://doi.org/10.1001/jamasurg.2017.0904
Kahl ERPY, Brião RC, Costa LM, Silveira LR, Moraes MAP (2019) Cenário ambulatorial de pacientes com sítio cirúrgico infectado após intervenção cardíaca. Rev Gaúcha Enferm 40:e20180200. https://doi.org/10.1590/1983-1447.2019.20180200
Dumville JC, Gray TA, Walter CJ, Sharp CA, Page T, Macefield R et al (2016) Dressings for the prevention of surgical site infection. Cochrane Database Syst Rev 12:CD003091. https://doi.org/10.1002/14651858.CD003091.pub4
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:1–9. https://doi.org/10.1136/bmj.n71
National Healthcare Safety Network (2022) Surgical Site Infection Event (SSI). Centers for Disease Control and Prevention. https://www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf. Accessed 14 April 2022
Rayyan Systems Inc. (2022). https://rayyan.qcri.org/welcome. Accessed 14 April 2022
RoB 2 and ROBINS-I (2022). www.riskofbias.info. Accessed 14 April 2022
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, et al. (ed) (2021) Cochrane handbook for systematic reviews of interventions. Version 6.2. London, The Cochrane Collaboration
Balshem H, Helfand M, Schünemann HJ, Oxman AD, Kunz R, Brozek J et al (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64:401–406. https://doi.org/10.1016/j.jclinepi.2010.07.015
Schünemann H, Brożek J, Guyatt G, Oxman A (eds) (2013) GRADE Handbook. The GRADE Working Group
Biffi R, Fattori L, Bertani E, Radice D, Rotmensz N, Misitano P et al (2012) Surgical site infections following colorectal cancer surgery: a randomized prospective trial comparing common and advanced antimicrobial dressing containing ionic silver. World J Surg Onc 10:1–9. https://doi.org/10.1186/1477-7819-10-94
Dixon AJ, Dixon MP, Dixon JB (2006) Randomized clinical trial of the effect of applying ointment to surgical wounds before occlusive dressing. BJS 93:937–943. https://doi.org/10.1002/bjs.5400
Robson V, Yorke J, Sen RA, Lowe D, Rogers SN (2012) Randomised controlled feasibility trial on the use of medical grade honey following microvascular free tissue transfer to reduce the incidence of wound infection. Br J Oral Maxillofac Surg 50:321–327. https://doi.org/10.1016/j.bjoms.2011.07.014
Ruiz-Tovar J, Llavero C, Morales V, Gamallo C (2015) Total occlusive ionic silver-containing dressing vs mupirocin ointment application vs conventional dressing in elective colorectal surgery: effect on incisional surgical site infection. J Am Coll Surg 221:424–429. https://doi.org/10.1016/j.jamcollsurg.2015.04.019
Shen P, Blackham AU, Lewis S, Dodson RM, Russell GB, Levine EA et al (2017) Phase II randomized trial of negative-pressure wound therapy to decrease surgical site infection in patients undergoing laparotomy for gastrointestinal, pancreatic, and peritoneal surface malignancies. J Am Coll Surg 224:726–737. https://doi.org/10.1016/j.jamcollsurg.2016.12.028
Struik GM, Vrijland WW, Birnie E, Klem TMAL (2018) A randomized controlled trial on the effect of a silver carboxymethylcellulose dressing on surgical site infections after breast cancer surgery. PLoS ONE 13:e0195715. https://doi.org/10.1371/journal.pone.0195715
Veiga DF, Damasceno CAV, Veiga-Filho J, Paiva LF, Fonseca FEM, Cabralet IV, al. (2016) Dressing wear time after breast reconstruction: a randomized clinical trial. PLoS ONE 11:e0166356. https://doi.org/10.1371/journal.pone.0166356
Ker H, Al-Murrani A, Rolfe G, Martin R (2019) WOUND study: a cost-utility analysis of negative pressure wound therapy after split-skin grafting for lower limb skin cancer. J Surg Res 235:308–314. https://doi.org/10.1016/j.jss.2018.10.016
Ruiz-Tovar J, Llavero C, Perez-Lopez M, Garcia-Marin A (2019) Effects of the application of vitamin E and silicone dressings vs conventional dressings on incisional surgical site infection in elective laparoscopic colorectal surgery: a prospective randomized clinical trial. J Hosp Infect 102:262–266. https://doi.org/10.1016/j.jhin.2018.10.021
Javed AA, Teinor J, Wright M, Ding D, Burkhart RA, Hundt J et al (2019) Negative pressure wound therapy for surgical-site infections: a randomized trial. Ann Surg 269:1034–1040. https://doi.org/10.1097/SLA.0000000000003056
Leitao MM Jr, Zhou QC, Schiavone MB, Cowan RA, Smith ES, Iasonos A et al (2021) Prophylactic negative pressure wound therapy after laparotomy for gynecologic surgery: a randomized controlled trial. Obstet Gynecol 137:334–341. https://doi.org/10.1097/AOG.0000000000004243
Tang Y, Zhang R, Yang W, Li W, Tao K (2020) Prognostic value of surgical site infection in patients after radical colorectal cancer resection. Med Sci Monit 26:e928054. https://doi.org/10.12659/MSM.928054
Xu Z, Qu H, Kanani G, Guo Z, Ren Y, Chen X (2020) Update on risk factors of surgical site infection in colorectal cancer: a systematic review and meta-analysis. Int J Colorectal Dis 35:2147–2156. https://doi.org/10.1007/s00384-020-03706-8
Anatone AJ, Danford NC, Jang ES, Smartt A, Konigsberg M, Tyler WK (2020) Risk factors for surgical site infection in orthopaedic oncology. J Am Acad Orthop Surg 28:e923–e928. https://doi.org/10.5435/JAAOS-D-19-00582
Poruk KE, Lin JA, Cooper MA, He J, Makary MA, Hirose K et al (2016) A novel, validated risk score to predict surgical site infection after pancreaticoduodenectomy. HPB (Oxford) 18:893–899. https://doi.org/10.1016/j.hpb.2016.07.011
O’Donnell RL, Angelopoulos G, Beirne JP, Biliatis I, Bolton H, Bradbury M et al (2019) Impact of surgical site infection (SSI) following gynaecological cancer surgery in the UK: a trainee-led multicentre audit and service evaluation. BMJ Open 9:e024853. https://doi.org/10.1136/bmjopen-2018-024853
Zheng Y, Chen Y, Yu K, Yang Y, Wang X, Yang X et al (2021) Fatal infections among cancer patients: a population-based study in the United States. Infect Dis Ther 10:871–895. https://doi.org/10.1007/s40121-021-00433-7
Rolston KVI (2017) Infections in cancer patients with solid tumors: a review. Infect Dis Ther 6:69–83. https://doi.org/10.1007/s40121-017-0146-1
Guinan JL, McGuckin M, Nowell PC (2003) Management of health-care–associated infections in the oncology patient. Oncology 17:415–420
Camargo IM (2012) Potencial cicatrizante do mel de abelha (Apis mellifera L.) em lesões do tecido cutâneo de ratos Wistar, Completion of Course Work. Faculdade Assis Gurgacz
National Institute for Health and Care Excellence (2019) PICO negative pressure wound dressings for closed surgical incisions. NICE, London
Webster J, Liu Z, Norman G, Dumville JC, Chiverton L, Scuffham P et al (2019) Negative pressure wound therapy for surgical wounds healing by primary closure. Cochrane Database Syst Rev 3:CD009261. https://doi.org/10.1002/14651858.CD009261.pub4
Author information
Authors and Affiliations
Contributions
T.A.D. and D.R.F. performed literature searches. T.A.D. and D.R.F. performed data collection. T.A.D., D.R.F., B.N.S., and R.C.C.P.S. performed data analysis. T.A.D., B.N.S., P.E.D.R., A.S.M., and R.C.C.P.S. wrote the first draft and critically revised the manuscript. All the authors contributed to the study design and have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This is a systematic review; no ethical approval is required.
Consent to participate
This was a systematic review, and informed consent was not required.
Consent for publication
This was a systematic review with no human research participants.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dias, T.A., Fernandes, D.R., dos Santos, B.N. et al. Dressing to prevent surgical site infection in adult patients with cancer: a systematic review with meta-analysis. Support Care Cancer 31, 11 (2023). https://doi.org/10.1007/s00520-022-07467-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-022-07467-8