Abstract
Background
Cystinosis is a rare autosomal recessive lysosomal disorder that mainly affects the kidney and eye. Early treatment with cysteamine significantly improves the prognosis. However, early diagnosis of cystinosis, especially the juvenile nephropathic form, remains challenging because typical symptoms only become apparent in adulthood. We herein describe a 13-year-old girl who presented with proteinuria only but was diagnosed with juvenile nephropathic cystinosis based on multinucleated podocytes in her kidney biopsy specimen. We also studied the nephropathology of another case to determine the features of the multinucleated podocytes.
Case diagnosis
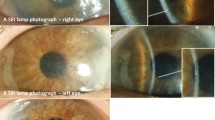
A previously healthy 13-year-old girl presented to our hospital because proteinuria had been detected in her school urine screening. She had been noted to have proteinuria on her school urine screening when she was 11 years of age but there was no consultation with her physician at that time. She was asymptomatic and had no other abnormalities on examination other than a relatively high urinary β-2 microglobulin level. Her kidney biopsy showed 15 multinucleated podocytes in 34 glomeruli, and the mean number of nuclei per multinucleated podocyte was 4.4. Ophthalmological examination showed cystine crystals in her cornea. Her white blood cell cystine level was high, and she was diagnosed with juvenile nephropathic cystinosis. She started oral cysteamine treatment and showed almost no progression of the disease after 2 years. In another patient with juvenile nephropathic cystinosis, there were 25 multinucleated podocytes in 63 glomeruli, and the mean number of nuclei per multinucleated podocyte was 2.9.
Conclusion
Early diagnosis is crucial to improve the prognosis of patients with cystinosis. This report emphasizes the importance of recognizing the unique pathological feature of multinucleated podocytes as an essential clue to the diagnosis of cystinosis.

Similar content being viewed by others
Data availability
Data will be made available upon reasonable request.
References
Gahl WA, Thoene JG, Schneider JA (2002) Cystinosis. N Engl J Med 347:111–121. https://doi.org/10.1056/NEJMra020552
Nesterova G, Gahl WA (2013) Cystinosis: the evolution of a treatable disease. Pediatr Nephrol 28:51–59. https://doi.org/10.1007/s00467-012-2242-5
Elmonem MA, Veys KR, Soliman NA, van Dyck M, van den Heuvel LP, Levtchenko E (2016) Cystinosis: a review. Orphanet J Rare Dis 11:47. https://doi.org/10.1186/s13023-016-0426-y
Nesterova G, Gahl W (2008) Nephropathic cystinosis: late complications of a multisystemic disease. Pediatr Nephrol 23:863–878. https://doi.org/10.1007/s00467-007-0650-8
Lusco MA, Najafian B, Alpers CE, Fogo AB (2017) AJKD Atlas of Renal Pathology: Cystinosis. Am J Kidney Dis 70:e23–e24. https://doi.org/10.1053/j.ajkd.2017.10.002
Brodin-Sartorius A, Tête MJ, Niaudet P, Antignac C, Guest G, Ottolenghi C, Charbit M, Moyse D, Legendre C, Lesavre P, Cochat P, Servais A (2012) Cysteamine therapy delays the progression of nephropathic cystinosis in late adolescents and adults. Kidney Int 81:179–189. https://doi.org/10.1038/ki.2011.277
Higashi S, Matsunoshita N, Otani M, Tokuhiro E, Nozu K, Ito S (2017) Diagnostic challenge in a patient with nephropathic juvenile cystinosis: a case report. BMC Nephrol 18:300. https://doi.org/10.1186/s12882-017-0721-4
Bonsib SM, Horvath F Jr (1999) Multinucleated podocytes in a child with nephrotic syndrome and Fanconi’s syndrome: a unique clue to the diagnosis. Am J Kidney Dis 34:966–971. https://doi.org/10.1016/S0272-6386(99)70060-0
Servais A, Morinière V, Grünfeld JP, Noël LH, Goujon JM, Chadefaux-Vekemans B, Antignac C (2008) Late-onset nephropathic cystinosis: clinical presentation, outcome, and genotyping. Clin J Am Soc Nephrol 3:27–35. https://doi.org/10.2215/CJN.01740407
Sharma A, Gupta R, Sethi SK, Bagga A, Dinda AK (2011) Giant cell transformation of podocytes: a unique histological feature associated with cystinosis. Indian J Nephrol 21:123–125. https://doi.org/10.4103/0971-4065.78067
Chandra M, Stokes MB, Kaskel F (2010) Multinucleated podocytes: a diagnostic clue to cystinosis. Kidney Int 78:1052. https://doi.org/10.1038/ki.2010.341
Mühldorfer J, Pfister E, Büttner-Herold M, Klewer M, Amann K, Daniel C (2018) Bi-nucleation of podocytes is uniformly accompanied by foot processes widening in renal disease. Nephrol Dial Transplant 33:796–803. https://doi.org/10.1093/ndt/gfx201
Nagata M, Yamaguchi Y, Komatsu Y, Ito K (1995) Mitosis and the presence of binucleate cells among glomerular podocytes in diseased human kidneys. Nephron 70:68–71. https://doi.org/10.1159/000188546
Fantone S, Tossetta G, Graciotti L, Galosi AB, Skrami E, Marzioni D, Morroni M (2022) Identification of multinucleated cells in human kidney cortex: A way for tissue repairing? J Anat 240:985–990. https://doi.org/10.1111/joa.13595
Acknowledgements
We thank Angela Morben, DVM, ELS, from Edanz (http://jp.edanz.com/ac) for editing a draft of this manuscript.
Author information
Authors and Affiliations
Contributions
AO and SI wrote the first draft of the manuscript. MO provided the pathology reports and figures. All authors reviewed and edited the manuscript and approved the final version.
Corresponding author
Ethics declarations
Consent for publication
Written informed consent for publication was provided by the patient’s legal guardians.
Competing interests
The authors have no financial or proprietary interests in any material discussed in this article.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ogata, A., Deki, S., Uchimura, T. et al. Multinucleated podocytes as a clue to diagnosis of juvenile nephropathic cystinosis. Pediatr Nephrol 39, 609–612 (2024). https://doi.org/10.1007/s00467-023-06103-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06103-9