Abstract
Background
Nonradiation, digital cholangioscope (DCS)-assisted endoscopic intervention for cholelithiasis has not been widely performed. For this study, we aimed to report the feasibility, efficacy, and safety of an established DCS-guided lithotomy procedure.
Methods
Data relating to biliary exploration, stone clearance, adverse events, and follow-up were obtained from 289 patients. The choledocholithiasis-related outcomes via the DCS-guided procedure were subsequently compared to those via conventional endoscopic retrograde cholangiopancreatography (ERCP).
Results
Biliary access was achieved in 285 patients. The technical success rate for the exploration of the common bile duct, the cystic stump, the hilar ducts, and secondary radicals was 100%. Moreover, the success rates were 98.4%, 61.7%, and 20.7%, for the exploration of the cystic duct, complete cystic duct, and gallbladder, respectively. Suspicious or confirmed suppurative cholecystitis, cholesterol polyps, and hyperplastic polyps were detected in 42, 23, and 5 patients, respectively. Stone clearance was achieved in one session in 285 (100%), 11 (100%), 13 (100%), 7 (100%), 6 (100%), and 3 (14.3%) patients with choledocholithiasis and hepatolithiasis, cystic duct stump stones, nondiffuse located intrahepatic lithiasis, a single cystic duct stone, a single gallbladder stone, and diffuse located intrahepatic lithiasis, respectively. Complete stone clearance for diffuse intrahepatic lithiasis was achieved in 19 (90.5%) patients, and fractioned re-lithotomy was performed in 16 (76.2%) patients. One patient developed mild acute cholangitis, and 12 developed mild pancreatitis. Stones recurred in one patient. Compared with conventional ERCP, DCS-guided lithotomy has the advantages of clearing difficult-to-treat choledocholithiasis and revealing concomitant biliary lesions, and this technique has fewer complications and a decreased risk of stone recurrence.
Conclusions
The technical profile, efficacy, and safety of nonradiation-guided and DCS-guided lithotomy are shown in this study. We provide a feasible modality for the endoscopic removal of cholelithiasis.
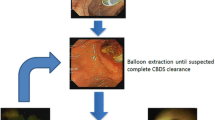
Graphical abstract


Similar content being viewed by others
References
Brewer Gutierrez OI, Bekkali NLH, Raijman I et al (2018) Efficacy and safety of digital single-operator cholangioscopy for difficult biliary stones. Clin Gastroenterol Hepatol 16(6):918–926
Yodice M, Choma J, Tadros M (2020) The expansion of cholangioscopy: established and investigational uses of spyglass in biliary and pancreatic disorders. Diagnostics (Basel) 10:132
Bang JY, Sutton B, Navaneethan U et al (2020) Efficacy of single-operator cholangioscopy-guided lithotripsy compared with large balloon sphincteroplasty in management of difficult bile duct stones in a randomized trial. Clin Gastroenterol Hepatol 18:2349–2356
Netinatsunton N, Sottisuporn J, Attasaranya S et al (2017) Prospective randomized trial of EUS-assisted ERCP without fluoroscopy versus ERCP in common bile duct stones. Gastrointest Endosc 86:1059–1065
Barakat MT, Girotra M, Choudhary A et al (2018) A prospective evaluation of radiation-free direct solitary cholangioscopy for the management of choledocholithiasis. Gastrointest Endosc 87(584–9):e1
Ridtitid W, Luangsukrerk T, Angsuwatcharakon P et al (2018) Uncomplicated common bile duct stone removal guided by cholangioscopy versus conventional endoscopic retrograde cholangiopancreatography. Surg Endosc 32:2704–2712
Feng Y, Liang Y, Liu Y et al (2021) Radiation-free digital cholangioscopy-guided laser lithotripsy for large common bile duct stones: feasibility and technical notes. Surg Endosc 35:6390–6395
Feng Y, Xu W, Liu Y et al (2021) Digital cholangioscopy-assisted nonradiation endoscopic retrograde cholangiopancreatography for retrieval of common bile duct stone. Surg Laparosc Endosc Percutan Tech 32:203–208
Ridtitid W, Rerknimitr R, Ramchandani M et al (2023) Endoscopic clearance of non-complex biliary stones using fluoroscopy-free direct solitary cholangioscopy: Initial multicenter experience. DEN Open 4:e241
Kiriyama S, Kozaka K, Takada T et al (2018) Tokyo Guidelines 2018: diagnostic criteria and severity grading of acute cholangitis (with videos). J Hepatobiliary Pancreat Sci 25:17–30
Cotton PB, Eisen GM, Aabakken L et al (2010) A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc 71:446–454
Mansilla-Vivar R, Alonso-Lázaro N, Argüello-Viudez L et al (2020) New management of hepatolithiasis: can surgery be avoided? (with video). Gastroenterol Hepatol 43:188–192
Lorio E, Patel P, Rosenkranz L et al (2020) Management of hepatolithiasis: review of the literature. Curr Gastroenterol Rep 22:30
Sakamoto Y, Takeda Y, Seki Y et al (2022) The usefulness of peroral cholangioscopy for intrahepatic stones. J Clin Med 1:6425
Okugawa T, Tsuyuguchi T, K C S, et al (2002) Peroral cholangioscopic treatment of hepatolithiasis: long-term results. Gastrointest Endosc 56:366–371
Averbukh LD, Miller D, Birk JW et al (2019) The utility of single operator cholangioscope (Spyglass) to diagnose and treat radiographically negative biliary stones: a case series and review. J Dig Dis 20:262–266
Robles-Medranda C, Soria-Alcívar M, Oleas R et al (2020) Digital per-oral cholangioscopy to diagnose and manage biliary duct disorders: a single-center retrospective study. Endosc Int Open 8:E796–E804
Yamauchi H, Iwai T, Okuwaki K et al (2022) Risk factors for perforation during endoscopic papillary large balloon dilation and bile duct stone removal. Dig Dis Sci 67:1890–1900
Hollenbach M, Hoffmeister A (2022) Adverse events in endoscopic retrograde cholangiopancreaticography (ERCP): focus on post-ERCP-pancreatitis. United European Gastroenterol J 10:10–11
Cahyadi O, Tehami N, de Madaria E et al (2022) Post-ERCP pancreatitis: prevention, diagnosis and management. Medicina (Kaunas) 58:1261
Kochar B, Akshintala VS, Afghani E et al (2015) Incidence, severity, and mortality of post-ERCP pancreatitis: a systematic review by using randomized, controlled trials. Gastrointest Endosc 81:143-149.e9
Tryliskyy Y, Bryce GJ (2018) Post-ERCP pancreatitis: pathophysiology, early identification and risk stratification. Adv Clin Exp Med 27:149–154
Maydeo AP, Rerknimitr R, Lau JY et al (2019) Cholangioscopy-guided lithotripsy for difficult bile duct stone clearance in a single session of ERCP: results from a large multinational registry demonstrate high success rates. Endoscopy 51:922–929
Lin Y, Yang M, Cao J et al (2023) Saline irrigation for reducing the recurrence of common bile duct stones after lithotripsy: a randomized controlled trial. EClinicalMedicine 59:101978
Yan X, Zheng W, Zhang Y et al (2021) Endoclip papillaplasty restores sphincter of oddi function: pilot study. Dig Endosc 33:962–969
Cheon YK, Lee TY, Kim SN et al (2017) Impact of endoscopic papillary large-balloon dilation on sphincter of Oddi function: a prospective randomized study. Gastrointest Endosc 85:782–790
Acknowledgements
We thank Dr. Xilong Ou, Dazhong Cao and Juan Liu for performing conventional ERCP for the treatment of choledocholithiasis.
Funding
This work was funded by the Program of Nanjing Healthy Commission (YKK22276).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Xiaojun Ma is an employee of Nanjing Microtech Medical Technology Co. Ltd. However, he is one of the key members who designed and modified the slim basket. He has no financial interest in this research and did not prepare the manuscript. Yadong Feng, Yan Liang, Yang Liu, Yinqiu Zhang, Shuaijing Huang, Lihua Ren, Xiaojun Ma, Aijun Zhou, and Ruihua Shi have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Feng, Y., Liang, Y., Liu, Y. et al. Digital cholangioscopy-assisted, direct visualization-guided, radiation-free, endoscopic retrograde intervention for cholelithiasis: technical feasibility, efficacy, and safety. Surg Endosc 38, 1637–1646 (2024). https://doi.org/10.1007/s00464-024-10684-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-024-10684-3