Abstract
Background
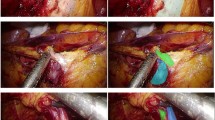
The precise recognition of liver vessels during liver parenchymal dissection is the crucial technique for laparoscopic liver resection (LLR). This retrospective feasibility study aimed to develop artificial intelligence (AI) models to recognize liver vessels in LLR, and to evaluate their accuracy and real-time performance.
Methods
Images from LLR videos were extracted, and the hepatic veins and Glissonean pedicles were labeled separately. Two AI models were developed to recognize liver vessels: the “2-class model” which recognized both hepatic veins and Glissonean pedicles as equivalent vessels and distinguished them from the background class, and the “3-class model” which recognized them all separately. The Feature Pyramid Network was used as a neural network architecture for both models in their semantic segmentation tasks. The models were evaluated using fivefold cross-validation tests, and the Dice coefficient (DC) was used as an evaluation metric. Ten gastroenterological surgeons also evaluated the models qualitatively through rubric.
Results
In total, 2421 frames from 48 video clips were extracted. The mean DC value of the 2-class model was 0.789, with a processing speed of 0.094 s. The mean DC values for the hepatic vein and the Glissonean pedicle in the 3-class model were 0.631 and 0.482, respectively. The average processing time for the 3-class model was 0.097 s. Qualitative evaluation by surgeons revealed that false-negative and false-positive ratings in the 2-class model averaged 4.40 and 3.46, respectively, on a five-point scale, while the false-negative, false-positive, and vessel differentiation ratings in the 3-class model averaged 4.36, 3.44, and 3.28, respectively, on a five-point scale.
Conclusion
We successfully developed deep-learning models that recognize liver vessels in LLR with high accuracy and sufficient processing speed. These findings suggest the potential of a new real-time automated navigation system for LLR.


Similar content being viewed by others
References
Abu Hilal M, Aldrighetti L, Dagher I, Edwin B, Troisi RI, Alikhanov R, Aroori S, Belli G, Besselink M, Briceno J, Gayet B, D’Hondt M, Lesurtel M, Menon K, Lodge P, Rotellar F, Santoyo J, Scatton O, Soubrane O, Sutcliffe R, Van Dam R, White S, Halls MC, Cipriani F, Van der Poel M, Ciria R, Barkhatov L, Gomez-Luque Y, Ocana-Garcia S, Cook A, Buell J, Clavien P-A, Dervenis C, Fusai G, Geller D, Lang H, Primrose J, Taylor M, Van Gulik T, Wakabayashi G, Asbun H, Cherqui D (2018) The Southampton Consensus Guidelines for laparoscopic liver surgery: from indication to implementation. Ann Surg 268:11–18
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2,804 patients. Ann Surg 250:831–841
Ciria R, Cherqui D, Geller DA, Briceno J, Wakabayashi G (2016) Comparative short-term benefits of laparoscopic liver resection: 9000 cases and climbing. Ann Surg 263:761–777
Mirnezami R, Mirnezami AH, Chandrakumaran K, Abu Hilal M, Pearce NW, Primrose JN, Sutcliffe RP (2011) Short- and long-term outcomes after laparoscopic and open hepatic resection: systematic review and meta-analysis. HPB (Oxford) 13:295–308
Honda G, Ome Y, Yoshida N, Kawamoto Y (2020) How to dissect the liver parenchyma: excavation with cavitron ultrasonic surgical aspirator. J Hepatobiliary Pancreat Sci 27:907–912
Jin S, Fu Q, Wuyun G, Wuyun T (2013) Management of post-hepatectomy complications. World J Gastroenterol 19:7983–7991
McKay A, You I, Bigam D, Lafreniere R, Sutherland F, Ghali W, Dixon E (2008) Impact of surgeon training on outcomes after resective hepatic surgery. Ann Surg Oncol 15:1348–1355
Yu KH, Beam AL, Kohane IS (2018) Artificial intelligence in healthcare. Nat Biomed Eng 2:719–731
Amann J, Blasimme A, Vayena E, Frey D, Madai VI, Precise4Q Consortium (2020) Explainability for artificial intelligence in healthcare: a multidisciplinary perspective. BMC Med Inform 20:310
Kelly CJ, Karthikesalingam A, Suleyman M, Corrado G, King D (2019) Key challenges for delivering clinical impact with artificial intelligence. BMC Med 17:195
Johnson KB, Wei W-Q, Weeraratne D, Frisse ME, Misulis K, Rhee K, Zhao J, Snowdon JL (2021) Precision medicine, AI, and the future of personalized health care. Clin Transl Sci 14:86–93
Vellido A (2020) The importance of interpretability and visualization in machine learning for applications in medicine and health care. Neural Comput Appl 32:18069–18083
Shelhamer E, Long J, Darrell T (2017) Fully convolutional networks for semantic segmentation. IEEE Trans Pattern Anal Mach Intell 39:640–651
Kitaguchi D, Lee Y, Hayashi K, Nakajima K, Kojima S, Hasegawa H, Takeshita N, Mori K, Ito M (2022) Development and validation of a model for laparoscopic colorectal surgical instrument recognition using convolutional neural network-based instance segmentation and videos of laparoscopic procedures. JAMA Netw Open 5:e2226265
Carstens M, Rinner FM, Bodenstedt S, Jenke AC, Weitz J, Distler M, Speidel S, Kolbinger FR (2023) The Dresden Surgical Anatomy Dataset for abdominal organ segmentation in surgical data science. Sci Data 10:3
Kitaguchi D, Takeshita N, Matsuzaki H, Igaki T, Hasegawa H, Kojima S, Mori K, Ito M (2022) Real-time vascular anatomical image navigation for laparoscopic surgery: experimental study. Surg Endosc 36:6105–6112
Madani A, Namazi B, Altieri MS, Hashimoto DA, Rivera AM, Pucher PH, Navarrete-Welton A, Sankaranarayanan G, Brunt LM, Okrainec A, Alseidi A (2022) Artificial intelligence for intraoperative guidance: using semantic segmentation to identify surgical anatomy during laparoscopic cholecystectomy. Ann Surg 276:363–369
Mascagni P, Vardazaryan A, Alapatt D, Urade T, Emre T, Fiorillo C, Pessaux P, Mutter D, Marescaux J, Costamagna G, Dallemagne B, Padoy N (2022) Artificial intelligence for surgical safety: automatic assessment of the critical view of safety in laparoscopic cholecystectomy using deep learning. Ann Surg 275:955–961
Takamoto T, Hashimoto T, Ogata S, Inoue K, Maruyama Y, Miyazaki A, Makuuchi M (2013) Planning of anatomical liver segmentectomy and sub-segmentectomy with 3-dimensional simulation software. Am J Surg 206:530–538
Mise Y, Tani K, Aoki T, Sakamoto Y, Hasegawa K, Sugawara Y, Kokudo N (2013) Virtual liver resection: computer-assisted operation planning using a three-dimensional liver representation. J Hepatobiliary Pancreat Sci 20:157–164
Lamadé W, Glombitza G, Fischer L, Chiu P, Cárdenas CE Sr, Thorn M, Meinzer HP, Grenacher L, Bauer H, Lehnert T, Herfarth C (2000) The impact of 3-dimensional reconstructions on operation planning in liver surgery. Arch Surg 135:1256–1261
Marescaux J, Clément JM, Tassetti V, Koehl C, Cotin S, Russier Y, Mutter D, Delingette H, Ayache N (1998) Virtual reality applied to hepatic surgery simulation: the next revolution. Ann Surg 228:627–634
Nicolau S, Soler L, Mutter D, Marescaux J (2011) Augmented reality in laparoscopic surgical oncology. Surg Oncol 20:189–201
Tang R, Ma L-F, Rong Z-X, Li M-D, Zeng J-P, Wang X-D, Liao H-E, Dong J-H (2018) Augmented reality technology for preoperative planning and intraoperative navigation during hepatobiliary surgery: a review of current methods. Hepatobiliary Pancreat Dis Int 17:101–112
Kenngott HG, Wagner M, Gondan M, Nickel F, Nolden M, Fetzer A, Weitz J, Fischer L, Speidel S, Meinzer H-P, Böckler D, Büchler MW, Müller-Stich BP (2014) Real-time image guidance in laparoscopic liver surgery: first clinical experience with a guidance system based on intraoperative CT imaging. Surg Endosc 28:933–940
Ishizawa T, Fukushima N, Shibahara J, Masuda K, Tamura S, Aoki T, Hasegawa K, Beck Y, Fukayama M, Kokudo N (2009) Real-time identification of liver cancers by using indocyanine green fluorescent imaging. Cancer 115:2491–2504
Inoue Y, Arita J, Sakamoto T, Ono Y, Takahashi M, Takahashi Y, Kokudo N, Saiura A (2015) Anatomical liver resections guided by 3-dimensional parenchymal staining using fusion indocyanine green fluorescence imaging. Ann Surg 262:105–111
Boni L, David G, Mangano A, Dionigi G, Rausei S, Spampatti S, Cassinotti E, Fingerhut A (2015) Clinical applications of indocyanine green (ICG) enhanced fluorescence in laparoscopic surgery. Surg Endosc 29:2046–2055
Sasaki K, Ito M, Kobayashi S, Kitaguchi D, Matsuzaki H, Kudo M, Hasegawa H, Takeshita N, Sugimoto M, Mitsunaga S, Gotohda N (2022) Automated surgical workflow identification by artificial intelligence in laparoscopic hepatectomy: experimental research. Int J Surg 105:106856
Ayabe RI, Azimuddin A, Cao HST (2022) Robot-assisted liver resection: the real benefit so far. Langenbecks Arch Surg 407:1779–1787
Bozkurt E, Sijberden JP, Abu Hilal M (2022) What is the current role, and what are the prospects of the robotic approach in liver surgery? Cancers (Basel) 14:4268
Bholat OS, Haluck RS, Murray WB, Gorman PJ, Krummel TM (1999) Tactile feedback is present during minimally invasive surgery. J Am Coll Surg 189:349–355
Acknowledgements
We thank Kensaku Mori, Department of Intelligent Science, Graduate School of Informatics, Nagoya University, for developing and contributing to Nu-VAT as an annotation tool.
Funding
No funding sources were available for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Norikazu Une, Shin Kobayashi, Daichi Kitaguchi, Taiki Sunakawa, Kimimasa Sasaki, Tateo Ogane, Kazuyuki Hayashi, Norihito Kosugi, Masashi Kudo, Motokazu Sugimoto, Hiro Hasegawa, Nobuyoshi Takeshita, Naoto Gotohda, and Masaaki Ito have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Electronic supplementary material 3 (MP4 15383 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Une, N., Kobayashi, S., Kitaguchi, D. et al. Intraoperative artificial intelligence system identifying liver vessels in laparoscopic liver resection: a retrospective experimental study. Surg Endosc 38, 1088–1095 (2024). https://doi.org/10.1007/s00464-023-10637-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10637-2