Abstract
Background
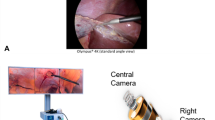
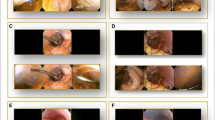
The limited 70° field of view (FoV) used in standard laparoscopy necessitates maneuvering the laparoscope to view the ports, follow the surgical tools, and search for a target region. Complications related to events that take place outside the FoV are underreported. Recently, a novel laparoscopic system (SurroundScope, 270Surgical) was reported to dramatically expand the FoV from 70 to 270°. This study focuses on differences in performing laparoscopic cholecystectomy using the SurroundScope compared to the standard laparoscope.
Methods
Forty-four laparoscopic surgeries were performed and video recorded. A subanalysis of 21 Cholecystectomies was performed and compared to 21 Cholecystectomies, performed with the standard laparoscope during the study period by the same surgeon.
Results
No accidental or intraoperative adverse events occurred when using the SurroundScope. Subanalysis of 21 Cholecystectomies revealed shorter fog/smoke cleaning times using the SurroundScope compared to the standard scope (1.45 ± 5.08 sec vs. 54.95 ± 137.77 sec, p = 0.0454). Furthermore, operations performed with the SurroundScope had a shorter trocar placement duration (85.0 ± 40.9 sec vs. 111.3 ± 70.5 sec; p = 0.077), shorter time to achieve critical view of safety (9.5 ± 4.14 min vs. 15.8 ± 11.87 min; p = 0.015), and shorter procedure duration (31.9 ± 10.4 min vs. 42.9 ± 22 min; p = 0.025). In post-operative evaluations, the surgeon noted that tools could be continuously followed and ports were visible without camera manipulation. Also, the surgeon agreed that the procedure could be better planned due to the wide FoV and that surgical workflow was improved. Furthermore, the surgeon agreed that the procedure was safer using the SurroundScope.
Conclusions
Initial results demonstrate the advantages of the SurroundScope over standard laparoscopy. By expanding the FoV, visualization is improved, the procedure is more efficient, significantly shorter and most important, patient safety, per surgeons’ testimonials is improved. Further investigation to quantify these benefits in a larger group of patients and among various surgical procedures should be considered.








Similar content being viewed by others
References
Abbitt D, Khallouq BB, Redan J (2017) Quantifying intraoperative laparoscopic visual field opacity. JSLS. https://doi.org/10.4293/JSLS.2017.00004
Song T, Lee DH (2020) A randomized Comparison of laparoscopic LEns defogging using Anti-fog solution, waRm saline, and chlorhexidine solution (CLEAR). Surg Endosc 34(2):940–945
Roviaro GC, Varoli F, Saguatti L, Vergani C, Maciocco M, Scarduelli A (2002) Major vascular injuries in laparoscopic surgery. Surg Endosc 16(8):1192–1196
Way LW, Stewart L, Gantert W, Liu K, Lee CM, Whang K et al (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective. Ann Surg 237(4):460–469
Lawrentschuk N, Fleshner NE, Bolton DM (2010) Laparoscopic lens fogging: a review of etiology and methods to maintain a clear visual field. J Endourol 24(6):905–913
Martin KE, Moore CM, Tucker R, Fuchshuber P, Robinson T (2016) Quantifying inadvertent thermal bowel injury from the monopolar instrument. Surg Endosc 30(11):4776–4784
Thompson KJ, Sroka G, Loveitt AP, Matter I, McCollister HM, Laniado M et al (2022) The introduction of wide-angle 270° laparoscopy through a novel laparoscopic camera system. Surg Endosc 36(3):2151–2158
Rolinger J, Model N, Jansen K, Knöll M, Beyersdorffer P, Kunert W et al (2022) Quantification of electrosurgery-related critical events during laparoscopic cholecystectomy—a prospective experimental study among surgical novices. 4open. 25(5):4
Strasberg SM, Helton WS (2011) An analytical review of vasculobiliary injury in laparoscopic and open cholecystectomy. HPB (Oxford) 13(1):1–14
Binenbaum SJ, Goldfarb MA (2006) Inadvertent enterotomy in minimally invasive abdominal surgery. JSLS 10(3):336–340
Cassaro S (2015) Delayed manifestations of laparoscopic bowel injury. Am Surg 81(5):478–482
Platz J, Hyman N (2012) Tracking intraoperative complications. J Am Coll Surg 215(4):519–523
Conde Monroy D, Torres Gómez P, Rey Chaves CE, Recamán A, Pardo M, Sabogal JC (2022) Early vs. delayed reconstruction for bile duct injury a multicenter retrospective analysis of a hepatopancreaticobiliary group. Sci Rep 12(1):11609
Nordestgaard AG, Bodily KC, Osborne RW, Buttorff JD (1995) Major vascular injuries during laparoscopic procedures. Am J Surg 169(5):543–545
Bhoyrul S, Vierra MA, Nezhat CR, Krummel TM, Way LW (2001) Trocar injuries in laparoscopic surgery. J Am Coll Surg 192(6):677–683
Jones MW, Guay E, Deppen JG (2023) Open cholecystectomy. StatPearls. Treasure Island (FL): StatPearls Publishing.
Majumder A, Altieri MS, Brunt LM (2020) How do I do it: laparoscopic cholecystectomy. Ann Laparosc Endosc Surg 5:15–15
Hershkovitz Y, Kais H, Halevy A, Lavy R (2016) Interval laparoscopic cholecystectomy: what is the best timing for surgery? Isr Med Assoc J 18(1):10–12
Lucocq J, Scollay J, Patil P (2022) Defining Prolonged Length of Stay (PLOS) following elective laparoscopic cholecystectomy and derivation of a pre-operative risk score to inform resource utilization, risk stratification, and patient consent. Ann Surg. https://doi.org/10.1097/SLA.0000000000005469
Watras AJ, Kim JJ, Ke J, Liu H, Greenberg JA, Heise CP et al (2020) Large-field-of-view visualization with small blind spots utilizing tilted micro-camera array for laparoscopic surgery. Micromachines (Basel) 11(5):488
Koong JK, Ng GH, Ramayah K, Koh PS, Yoong BK (2021) Early identification of the critical view of safety in laparoscopic cholecystectomy using indocyanine green fluorescence cholangiography: a randomised controlled study. Asian J Surg 44(3):537–543
Procter LD, Davenport DL, Bernard AC, Zwischenberger JB (2010) General surgical operative duration is associated with increased risk-adjusted infectious complication rates and length of hospital stay. J Am Coll Surg 210(1):60–65
Vettoretto N, Saronni C, Harbi A, Balestra L, Taglietti L, Giovanetti M (2011) Critical view of safety during laparoscopic cholecystectomy. JSLS 15(3):322–325
Lau H, Brooks DC (2002) Contemporary outcomes of ambulatory laparoscopic cholecystectomy in a major teaching hospital. World J Surg 26(9):1117–1121
Funding
This work is supported by 270Surgical.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Shirley Shapira is an employee and owns employee stock options in 270Surgical Ltd. Gideon Sroka, Zvi Ehrlich, and Pazit Koren have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shapira, S.S., Ehrlich, Z., Koren, P. et al. Comparing a novel wide field of view laparoscope with conventional laparoscope while performing laparoscopic cholecystectomy. Surg Endosc 37, 8910–8918 (2023). https://doi.org/10.1007/s00464-023-10393-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10393-3