Abstract
Background
Minimally invasive splenectomy (MIS) is increasingly favored for the treatment of benign and malignant diseases of the spleen over open access approaches. While many studies cite the superiority of MIS in terms of decreased morbidity and length of stay over a traditional open approach, the comparative effectiveness of specific technical and peri-operative approaches to MIS is unclear.
Objective
To develop evidence-based guidelines that support clinicians, patients, and others in decisions on the peri-operative performance of MIS.
Methods
A guidelines committee panel of the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) including methodologists used the Grading of Recommendations Assessment, Development and Evaluation approach to grade the certainty of evidence and formulate recommendations.
Results
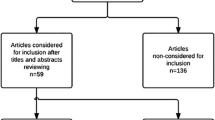
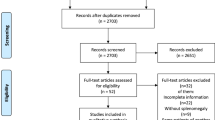
Informed by a systematic review of the evidence, the panel agreed on eight recommendations for the peri-operative performance of MIS for adults and children in elective situations addressing six key questions.
Conclusions
Conditional recommendations were made in favor of lateral positioning for non-hematologic disease, intra-operative platelet administration for patients with idiopathic thrombocytopenic purpura instead of preoperative administration, and the use of mechanical devices to control the splenic hilum. Further, a conditional recommendation was made against routine intra-operative drain placement.
Similar content being viewed by others
References
Feng S, Qiu Y, Li X, Yang H, Wang C, Yang J, Liu W, Wang A, Yao X, Lai XH (2016) Laparoscopic versus open splenectomy in children: a systematic review and meta-analysis. Pediatr Surg Int 32:253–259
Fransvea P, Costa G, Serao A, Cortese F, Balducci G, Sganga G, Marini P (2021) Laparoscopic splenectomy after trauma: who, when and how. A systematic review. J Minim Access Surg 17:141–146
Moris D, Dimitriou N, Griniastsos J (2017) Laparoscopic splenectomy for benign hematological disorders in adults: a systemtatic review. In Vivo 31:291–302
Andrews JC, Schünemann HJ, Oxman AD, Pottie K, Meerpohl JJ, Coello PA, Rind D, Montori VM, Brito JP, Norris S, Elbarbary M, Post P, Nasser M, Shukla V, Jaeschke R, Brozek J, Djulbegovic B, Guyatt G (2013) GRADE guidelines: 15. Going from evidence to recommendation-determinants of a recommendation’s direction and strength. J Clin Epidemiol 66:726–735
Rogers AT, Dirks R, Burt HA, Haggerty S, Kohn GP, Slater BJ, Walsh D, Stefanidis D, Pryor A (2021) Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) guidelines development: standard operating procedure. Surg Endosc 35:2417–2427
Andrews J, Guyatt G, Oxman AD, Alderson P, Dahm P, Falck-Ytter Y, Nasser M, Meerpohl J, Post PN, Kunz R, Brozek J, Vist G, Rind D, Akl EA, Schünemann HJ (2013) GRADE guidelines: 14. Going from evidence to recommendations: the significance and presentation of recommendations. J Clin Epidemiol 66:719–725
Institute of Medicine (U.S.). Committee on Standards for Developing Trustworthy Clinical Practice Guidelines., Graham R (2011) Clinical practice guidelines we can trust. National Academies Press, Washington, DC
Alonso-Coello P, Schünemann HJ, Moberg J, Brignardello-Petersen R, Akl EA, Davoli M, Treweek S, Mustafa RA, Rada G, Rosenbaum S, Morelli A, Guyatt GH, Oxman AD, GRADE Working Group (2016) GRADE Evidence to Decision (EtD) frameworks: a systematic and transparent approach to making well informed healthcare choices. 1: Introduction. BMJ 353:2016
Alonso-Coello P, Oxman AD, Moberg J, Brignardello-Petersen R, Akl EA, Davoli M, Treweek S, Mustafa RA, Vandvik PO, Meerpohl J, Guyatt GH, Schünemann HJ, GRADE Working Group (2016) GRADE Evidence to Decision (EtD) frameworks: a systematic and transparent approach to making well informed healthcare choices. 2: clinical practice guidelines. BMJ 353:i2089
Chen Y, Yang K, Marusic A, Qaseem A, Meerpohl JJ, Flottorp S, Akl EA, Schunemann HJ, Chan ES, Falck-Ytter Y, Ahmed F, Barber S, Chen C, Zhang M, Xu B, Tian J, Song F, Shang H, Tang K, Wang Q, Norris SL, RW Group (2017) A reporting tool for practice guidelines in health care: the RIGHT statement. Ann Intern Med 166:128–132
McMaster University (2013) GRADEpro GDT: GRADEpro Guideline Development Tool. [Software]. (developed by Evidence Prime, Inc.). http://gradepro.org
Covidence systematic review software. Veritas Health Innovation, Melbourne, Australia. http://www.covidence.org
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Wells GA Shea B, O'Connell D, Peterson J, Welch V, Losos M, Tugwell P (2019) The Newcastle-Ottawa Scale (NOS) for assessing the quality if nonrandomized studies in meta-analyses. Ottawa Hospital, Ottawa, Canada. http://www.ohrica/programs/clinical_epidemiology/oxford.asp
Manager (RevMan) R (2014) The Nordic Cochrane Centre. The Cochrane Collaboration, Copenhagen
McMaster University (2015) GRADEpro GDT: GRADEpro guideline development tool. [Software]. (developed by Evidence Prime, Inc.). http://gradepro.org
Schünemann H, Brożek J, Guyatt G, Oxman A, (eds) (2013) GRADE handbook for grading quality of evidence and strength of recommendations. Updated October 2013. The GRADE Working Group. http://guidelinedevelopment.org/handbook.
Koshenkov VP, Pahuja AK, Németh ZH, Abkin A, Carter MS (2012) Identification of accessory spleens during laparoscopic splenectomy is superior to preoperative computed tomography for detection of accessory spleens. JSLS 16:387–391
Quah C, Ayiomamitis GD, Shah A, Ammori BJ (2011) Computed tomography to detect accessory spleens before laparoscopic splenectomy: is it necessary? Surg Endosc 25:261–265
Stanek A, Stefaniak T, Makarewicz W, Kaska L, Podgórczyk H, Hellman A, Lachinski A (2005) Accessory spleens: preoperative diagnostics limitations and operational strategy in laparoscopic approach to splenectomy in idiopathic thrombocytopenic purpura patients. Langenbecks Arch Surg 390:47–51
Napoli A, Catalano C, Silecchia G, Fabiano P, Fraioli F, Pediconi F, Venditti F, Basso N, Passariello R (2004) Laparoscopic splenectomy: multi-detector row CT for preoperative evaluation. Radiology 232:361–367
Vikse J, Sanna B, Henry BM, Taterra D, Sanna S, Pękala PA, Walocha JA, Tomaszewski KA (2017) The prevalence and morphometry of an accessory spleen: a meta-analysis and systematic review of 22,487 patients. Int J Surg 45:18–28
Altaf AM, Sawatzky M, Ellsmere J, Bonjer HJ, Burrell S, Abraham R, Couban S, Klassen D (2009) Laparoscopic accessory splenectomy: the value of perioperative localization studies. Surg Endosc 23:2675–2679
Furlow B (2011) Radiation protection in pediatric imaging. Radiol Technol 82:421–439
Naoum JJ, Silberfein EJ, Zhou W, Sweeney JF, Albo D, Brunicardi FC, Kougias P, El Sayed HF, Lin PH (2007) Concomitant intraoperative splenic artery embolization and laparoscopic splenectomy versus laparoscopic splenectomy: comparison of treatment outcome. Am J Surg 193:713–718
Wu Z, Zhou J, Pankaj P, Peng B (2012) Comparative treatment and literature review for laparoscopic splenectomy alone versus preoperative splenic artery embolization splenectomy. Surg Endosc 26:2758–2766
Li J, You N, Deng C, Wu K, Wang L, Huang X, Wang W, Fan J, Zheng L (2018) Use of iodized oil and gelatin sponge embolization in splenic artery coiling reduces bleeding from laparoscopic splenectomy for cirrhotic portal hypertension patients with complicating hypersplenic splenomegaly: a comparative study. J Laparoendosc Adv Surg Tech A 28:713–720
Ekeh AP, Khalaf S, Ilyas S, Kauffman S, Walusimbi M, McCarthy MC (2013) Complications arising from splenic artery embolization: a review of an 11-year experience. Am J Surg 205:250–254
Gaba RC, Katz JR, Parvinian A, Reich S, Omene BO, Yap FY, Owens CA, Knuttinen MG, Bui JT (2013) Splenic artery embolization: a single center experience on the safety, efficacy, and clinical outcomes. Diagn Interv Radiol 19:49–55
Major P, Matlok M, Pedziwiatr M, Budzynski A (2012) Do we really need routine drainage after laparoscopic adrenalectomy and splenectomy? Wideochir Inne Tech Maloinwazyjne 8:33–39
Mujagic E, Zeindler J, Coslovsky M, Hoffmann H, Soysal SD, Mechera R, von Strauss M, Delko T, Saxer F, Glaab R, Kraus R, Mueller A, Curti G, Gurke L, Jakob M, Marti WR, Weber WP (2019) The association of surgical drains with surgical site infections—A prospective observational study. Am J Surg 217:17–23
Degrate L, Zanframundo C, Bernasconi DP, Real G, Garancini M, Uggeri F, Romano F, Braga M (2020) Futility of abdominal drain in elective laparoscopic splenectomy. Langenbecks Arch 405:665–672
Fathi A, Eldamshety O, Bahy O, Denewer A, Fady T, Shehatto F, Khater A, Elnahas W, Roshdy S, Farouk O, Senbel A, Hamed EE, Setit A (2016) Lateral versus anterior approach laparoscopic splenectomy: a randomized-controlled study. Surg Laparosc Endosc Percutan Tech 26:465–469
Wu Z, Zhou J, Li J, Zhu Y, Peng B (2012) The feasibility of laparoscopic splenectomy for ITP patients without preoperative platelet transfusion. Hepatogastroenterology 59:81–85
Fathi A, Elmoatasembellah M, Senbel A, Shahatto F, Eldamshety O, Shetiwy M, Abdel Wahab K, Abouzid A, Setit A (2020) Safety and efficacy of using staplers and vessel sealing devices for laparoscopic splenectomy: A randomized controlled trial. Surg Innov 28:303–308. https://doi.org/10.1177/1553350620953023
Shabahang H, Maddah G, Tavassoli A, Jangjoo A, Alvandipour M, Abdollahi A, Noorshafiee S (2012) Laparoscopic splenectomy: ligasure or clip ligation? Surg Laparosc Endosc Percutan Tech 22:136–138
Acknowledgements
The authors thank Sarah Colon (SAGES) for administrative support and Shauna Bostian and Holly Burt for librarian support.
Author information
Authors and Affiliations
Contributions
TK was the panel Chair, wrote the first draft of the manuscript, and revised the manuscript based on author’s suggestions; RD and AC were the panel co-chairs and non-voting members, contributed to drafting and critical revisions of the manuscript and contributed to further drafts, moderated the panel sessions, and checked the manuscript accuracy; AMAS and MTA provided methodological support; DW, SH, and DS provided supervision and guidance throughout the development process and critically revised this guideline. Guideline panel members (see Supplementary Material Appendix A), participated in the creation of the EtD tables (Supplementary Material Appendix C), critically reviewed the manuscript and provided suggestions for improvement. All authors approved the content.
Corresponding author
Ethics declarations
Disclosures
A full list of disclosures and conflicts of interest can be found in Supplementary Material Appendix B. All conflicts of interest and disclosures were assessed as not having influenced the construction of the Guidelines.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kindel, T.L., Dirks, R.C., Collings, A.T. et al. Guidelines for the performance of minimally invasive splenectomy. Surg Endosc 35, 5877–5888 (2021). https://doi.org/10.1007/s00464-021-08741-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08741-2