Abstract
Background
Minimally invasive techniques have been broadly introduced to liver surgery during the last couple of years. In this study, we aimed to report the incidence and potential risk factors for incisional hernia (IH) as well as health-related quality of life (HRQoL) after laparoscopic liver resections (LLR).
Methods
All patients undergoing LLR between January 2014 and June 2017 were contacted for an outpatient hernia examination. In all eligible patients, photo documentation of the scar was performed and IH was evaluated by clinical examination and by ultrasound. Patients also completed a questionnaire to evaluate IH-specific symptoms and HRQoL. Obtained results were retrospectively analyzed with regard to patients’ characteristics, perioperative outcomes and applied minimally invasive techniques, such as multi-incision laparoscopic liver surgery or hand-assisted/single-incision laparoscopic surgery (HALS/SILS).
Results
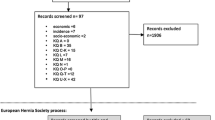
Of 184 patients undergoing surgery, 161 (87.5%) met the inclusion criteria and 49 patients (26.6%) participated in this study. After a median time of 26 months (range 19–50 months) after surgery, we observed an overall incidence of IH of 12%. Five of 6 patients were overweight or obese (BMI ≥ 25) and 5 of 6 hernias were located at the umbilical site. Univariate analysis suggested the performance status at time of operation (ASA score ≥ 3; HR 5.616, 95% CI 1.012–31.157, p = 0.048) and the approach (HALS/SILS, HR 6.571, 95% CI 1.097–39.379, p = 0.039) as potential risk factors for IH. A higher frequency of hernia-related physical restrictions (HRR; p = 0.058) and a decreased physical functioning (p = 0.17) were noted in patients with IH; however, both being short of statistical significance.
Conclusion
Advantages of laparoscopic surgery with regard to low rates of IH can be translated to minimally invasive liver surgery. Even though there are low rates of IH, patients with poor performance status at the time of operation should be monitored closely. While patients’ characteristics are hard to influence, it might be worth focusing on surgical factors such as the approach and the closure of the umbilical site to further minimize the rate of IH.


Similar content being viewed by others
References
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS et al (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261(4):619–629
Benzing C, Krenzien F, Gohlke D, Andreou A, Haber P, Wabitsch S et al (2017) Health-related quality of life after laparoscopic liver resection. J Minim Access Surg. https://doi.org/10.4103/jmas.JMAS_137_17
Beppu T, Wakabayashi G, Hasegawa K, Gotohda N, Mizuguchi T, Takahashi Y et al (2015) Long-term and perioperative outcomes of laparoscopic versus open liver resection for colorectal liver metastases with propensity score matching: a multi-institutional Japanese study. J Hepatobiliary Pancreat Sci 22(10):711–720
Okuno M, Goumard C, Mizuno T, Omichi K, Tzeng CD, Chun YS et al (2018) Operative and short-term oncologic outcomes of laparoscopic versus open liver resection for colorectal liver metastases located in the posterosuperior liver: a propensity score matching analysis. Surg Endosc 32(4):1776–1786
Cipriani F, Rawashdeh M, Stanton L, Armstrong T, Takhar A, Pearce NW et al (2016) Propensity score-based analysis of outcomes of laparoscopic versus open liver resection for colorectal metastases. Br J Surg 103(11):1504–1512
Kim H, Suh KS, Lee KW, Yi NJ, Hong G, Suh SW et al (2014) (2014) Long-term outcome of laparoscopic versus open liver resection for hepatocellular carcinoma: a case-controlled study with propensity score matching. Surg Endosc 28(3):950–960
Fretland AA, Dagenborg VJ, Bjornelv GMW, Kazaryan AM, Kristiansen R, Fagerland MW et al (2018) Laparoscopic versus open resection for colorectal liver metastases: the OSLO-COMET randomized controlled trial. Ann Surg 267(2):199–207
Gillion J-F, Sanders D, Miserez M, Muysoms F (2016) The economic burden of incisional ventral hernia repair: a multicentric cost analysis. Hernia 20(6):819–830
Haueter R, Schutz T, Raptis DA, Clavien PA, Zuber M (2017) Meta-analysis of single-port versus conventional laparoscopic cholecystectomy comparing body image and cosmesis. Br J Surg 104(9):1141–1159
Milas M, Devedija S, Trkulja V (2014) Single incision versus standard multiport laparoscopic cholecystectomy: up-dated systematic review and meta-analysis of randomized trials. Surgeon 12(5):271–289
Sangster W, Kulaylat AN, Stewart DB, Schubart JR, Koltun WA, Messaris E (2015) Hernia incidence following single-site vs standard laparoscopic colorectal surgery. Colorectal Dis 17(3):250–256
Tamini N, Rota M, Bolzonaro E, Nespoli L, Nespoli A, Valsecchi MG et al (2014) Single-incision versus standard multiple-incision laparoscopic cholecystectomy: a meta-analysis of experimental and observational studies. Surg Innov 21(5):528–545
Marks JM, Phillips MS, Tacchino R, Roberts K, Onders R, DeNoto G et al (2013) Single-incision laparoscopic cholecystectomy is associated with improved cosmesis scoring at the cost of significantly higher hernia rates: 1-year results of a prospective randomized, multicenter, single-blinded trial of traditional multiport laparoscopic cholecystectomy vs single-incision laparoscopic cholecystectomy. J Am Coll Surg 216(6):1037–1047
Ware JE Jr, Kosinski M, Gandek B, Aaronson NK, Apolone G, Bech P et al (1998) The factor structure of the SF-36 health survey in 10 countries: results from the IQOLA project. international quality of life assessment. J Clin Epidemiol 51:1159–1165
Heniford BT, Walters AL, Lincourt AE, Novitsky YW, Hope WW, Kercher KW (2008) Comparison of generic versus specific quality-of-life scales for mesh hernia repairs. J Am Coll Surg 206:638–644
Walming S, Angenete E, Block M, Bock D, Gessler B, Haglind E (2017) Retrospective review of risk factors for surgical wound dehiscence and incisional hernia. BMC Surg 17(1):19
Guitarte C, Grant J, Zhao H, Wang S, Ferriss JS, Hernandez E (2016) Incisional hernia formation and associated risk factors on a gynecologic oncology service: an exploratory analysis. Arch Gynecol Obstet 294(4):805–811
Yamada T, Okabayashi K, Hasegawa H, Tsuruta M, Abe Y, Ishida T et al (2016) Age, preoperative subcutaneous fat area, and open laparotomy are risk factors for incisional hernia following colorectal cancer surgery. Ann Surg Oncol 23(Suppl 2):S236–S241
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Strasberg SM (2005) Nomenclature of hepatic anatomy and resections: a review of the Brisbane 2000 system. J Hepatobiliary Pancreat Surg 12(5):351–355
Schmelzle M, Wabitsch S, Haber PK, Krenzien F, Kastner A, Biebl M et al (2018) Laparoscopic liver surgery—a single centre series of 250 consecutive cases. Zentralbl Chir 144(2):145–152
Deerenberg EB, Harlaar JJ, Steyerberg EW, Lont HE, van Doorn HC, Heisterkamp J et al (2015) Small bites versus large bites for closure of abdominal midline incisions (STITCH): a double-blind, multicentre, randomised controlled trial. Lancet 386(10000):1240–1260
Schiffman SC, Kim KH, Tsung A, Marsh JW, Geller DA (2015) Laparoscopic versus open liver resection for metastatic colorectal cancer: a metaanalysis of 610 patients. Surgery 157(2):211–222
Wabitsch S, Haber PK, Ekwelle N, Kästner A, Krenzien F, Benzing C et al (2019) Minimally invasive liver surgery in elderly patients-a single-center experience. J Surg Res 239:92–97
Sotiropoulos GC, Prodromidou A, Kostakis ID, Machairas N (2017) Meta-analysis of laparoscopic vs open liver resection for hepatocellular carcinoma. Updat Surg 69(3):291–311
Jensen KK, Krarup P-M, Scheike T, Jorgensen LN, Mynster T (2016) Incisional hernias after open versus laparoscopic surgery for colonic cancer: a nationwide cohort study. Surg Endosc 30(10):4469–4479
Fink C, Baumann P, Wente MN, Knebel P, Bruckner T, Ulrich A et al (2014) Incisional hernia rate 3 years after midline laparotomy. Br J Surg 101(2):51–54
Julliard O, Hauters P, Possoz J, Malvaux P, Landenne J, Gherardi D (2016) Incisional hernia after single-incision laparoscopic cholecystectomy: incidence and predictive factors. Surg Endosc 30(10):4539–4543
Barutcu AG, Klein D, Kilian M, Biebl M, Raakow R, Pratschke J et al (2019) Long-term follow-up after single-incision laparoscopic surgery. Surg Endosc. https://doi.org/10.1007/s00464-019-06739-5
Coelho FF, Bernardo WM, Kruger JAP, Jeismann VB, Fonseca GM, Macacari RL et al (2018) Laparoscopy-assisted versus open and pure laparoscopic approach for liver resection and living donor hepatectomy: a systematic review and meta-analysis. HPB 20(8):687–694
Petersson J, Koedam T, Bonjer H, Andersson J, Angenete E, Bock D et al (2018) Bowel obstruction and ventral hernia after laparoscopic versus open surgery for rectal cancer in a randomized trial (COLOR II). Ann Surg 269:53–57
Laurent C, Leblanc F, Gineste C, Saric J, Rullier E (2007) Laparoscopic approach in surgical treatment of rectal cancer. Br J Surg 94:1555–1561
Kazaryan A, Marangos I, Rosok B, Rosseland A, Villanger O, Fosse E et al (2010) Laparoscopic resection of colorectal liver metastases. Surgical and long-term oncologic outcome. Ann Surg 252:1005–1012
Chen-Xu J, Bessa-Melo R, Graça L, Costa-Maia J (2019) Incisional hernia in hepatobiliary and pancreatic surgery: incidence and risk factors. Hernia 23(1):67–79
Kayashima H, Maeda T, Harada N, Masuda T, Guntani A, Ito S et al (2015) Risk factors for incisional hernia after hepatic resection for hepatocellular carcinoma in patients with liver cirrhosis. Surgery 158(6):1669–1675
Hasson HM (1971) A modified instrument and method for laparoscopy. Am J Obstet Gynecol 110(6):886–887
Palmer R (1974) Safety in laparoscopy. J Reprod Med 13(1):1–5
Giuliani A, Migliaccio C, Ceriello A, Aragiusto G, La Manna G, Calise F (2014) Laparoscopic vs. open surgery for treating benign liver lesions: assessing quality of life in the first year after surgery. Updat Surg 66(2):127–133
Author information
Authors and Affiliations
Contributions
WS: conception and design, analysis and interpretation, writing of the manuscript, SP: data collection, critical revision of the manuscript, FF: data collection, critical revision of the manuscript, KA: data collection, statistical analysis, critical revision of the manuscript, FU: ultrasound, critical revision of the article, BC: analysis and interpretation, critical revision of the manuscript, HPK: analysis and interpretation, critical revision of the manuscript, DT: supervision of ultrasound, critical analysis of the article, PJ: conception and interpretation, critical revision of the article, FP: conception and design, clinical examination, critical revision of the article, hernia repair, SM: conception and design, analysis and interpretation, critical revision of the article.
Corresponding author
Ethics declarations
Disclosures
Schmelzle M reports personal fees from Merck, personal fees from Bayer, personal fees and other from ERBE, other from Ethicon, other from Takeda, other from Olympus, other from Medtronic, other from Intuitive, outside the submitted work. Pratschke J reports personal fees from Verb Surgical, other from Medtronic, other from Intuitive, from Merck, outside the submitted work. The authors Wabitsch S, Schulz P, Fröschle F, Kästner A, Fehrenbach U, Benzing C, Haber PK, Denecke T Fikatas P have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wabitsch, S., Schulz, P., Fröschle, F. et al. Incidence of incisional hernia after laparoscopic liver resection. Surg Endosc 35, 1108–1115 (2021). https://doi.org/10.1007/s00464-020-07475-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07475-x