Abstract
Background
Optimizing a living kidney donation program is important to guarantee a high grade of acceptance among potential donors. Hand-assisted retroperitoneoscopic donor nephrectomy (HARP) is an alternative to the open anterior approach (AA) technique. Problems associated to the learning curve could hinder a transition. 3D display technique seems to ease minimally invasive surgery. Aim of this study was to evaluate the learning curve during the transition from AA to HARP and the influence of the 3D display system on the established technique.
Methods
Observational study (n = 207) during transition to HARP and introduction of 3D display technique.
Results
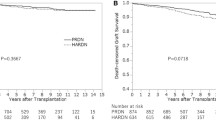
Operation time (OT), warm ischemia time (WIT) and blood loss (BL) of HARP decreased during transition. Pairwise group comparison for OT showed a significant learning effect for the first 30 out of 50 HARPs without influence on graft function. Between AA and HARP no significant difference in OT (133 ± 24 vs. 127 ± 19 min, p = 0.25) but for WIT (23 ± 28 vs. 126 ± 40 s, p < 0.005) and BL (328 ± 207 vs. 54 ± 35 ml, p < 0.005) was seen. There was neither a significant difference in donors’ nor recipients’ eGFR. OT (98 ± 16 vs. 106 ± 19 min, p = 0.036) and WIT (97 ± 37 vs. 120 ± 57 s, p = 0.023) were significantly shorter for the 3D technique compared to 2D.
Conclusion
A transition to HARP is possible without additional risk for the donor or loss of quality for the recipient. The learning curve for HARP is steep and short. The introduction of 3D display technique after transition facilitates the surgical preparation and could further help to optimize HARP.





Similar content being viewed by others
References
Eurotransplant Foundation (2014) Annual report 2014, April 2014
Hart A, Smith JM, Skeans MA et al (2016) OPTN/SRTR annual data report 2014 Kidney. Am J Transplant 16(S2):11–46
Klop KW, Dols LF, Kok NF, Weimar W, Ijzermans JN (2012) Attitudes among surgeons towards live-donor nephrectomy: a European update. Transplantation 94(3):263–268
Dols LF, Kok NF, d’Ancona FC et al (2014) Randomized controlled trial comparing hand-assisted retroperitoneoscopic versus standard laparoscopic donor nephrectomy. Transplantation 97(2):161–167
Klop KW, Kok NF, Dols LF et al (2014) Can right-sided hand-assisted retroperitoneoscopic donor nephrectomy be advocated above standard laparoscopic donor nephrectomy: a randomized pilot study. Transpl Int 27(2):162–169
He B, Bremner A, Han Y, Hamdorf JM (2016) Determining the superior technique for living-donor nephrectomy: the laparoscopic intraperitoneal versus the retroperitoneoscopic approach. Exp Clin Transplant 14(2):129–138
Sorensen SM, Savran MM, Konge L, Bjerrum F (2016) Three-dimensional versus two-dimensional vision in laparoscopy: a systematic review. Surg Endosc 30(1):11–23
Smith R, Schwab K, Day A et al (2014) Effect of passive polarizing three-dimensional displays on surgical performance for experienced laparoscopic surgeons. Br J Surg 101(11):1453–1459
Sakata S, Watson MO, Grove PM, Stevenson AR (2016) The conflicting evidence of three-dimensional displays in laparoscopy: a review of systems old and new. Ann Surg 263(2):234–239
Wadstrom J, Lindstrom P (2002) Hand-assisted retroperitoneoscopic living-donor nephrectomy: initial 10 cases. Transplantation 73(11):1839–1840
Lyon R (1958) An anterior extraperitoneal incision for kidney surgery. J Urol 79(3):383–392
Connor WT, Van Buren CT, Floyd M, Kahan BD (1981) Anterior extraperitoneal donor nephrectomy. J Urol 126(4):443–447
Jones KW, Peters TG, Walker GW (1999) Anterior-retroperitoneal living donor nephrectomy: technique and outcomes. Am Surg 65(3):197–204
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Kocak B, Koffron AJ, Baker TB et al (2006) Proposed classification of complications after live donor nephrectomy. Urology 67(5):927–931
Wadstrom J, Biglarnia A, Gjertsen H, Sugitani A, Fronek J (2011) Introducing hand-assisted retroperitoneoscopic live donor nephrectomy: learning curves and development based on 413 consecutive cases in four centers. Transplantation 91(4):462–469
Chin EH, Hazzan D, Edye M et al (2009) The first decade of a laparoscopic donor nephrectomy program: effect of surgeon and institution experience with 512 cases from 1996 to 2006. J Am Coll Surg 209(1):106–113
Dols LF, Kok NF, Terkivatan T et al (2010) Optimizing left-sided live kidney donation: hand-assisted retroperitoneoscopic as alternative to standard laparoscopic donor nephrectomy. Transpl Int 23(4):358–363
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Roger Wahba, Robert Kleinert, Martin Hellmich, Nadine Heiermann, Georg Dieplinger, Hans A. Schlößer, Denise Buchner, Christine Kurschat and Dirk L. Stippel have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Wahba, R., Kleinert, R., Hellmich, M. et al. Optimizing a living kidney donation program: transition to hand-assisted retroperitoneoscopic living donor nephrectomy and introduction of a passive polarizing three-dimensional display system. Surg Endosc 31, 2577–2585 (2017). https://doi.org/10.1007/s00464-016-5264-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5264-4