Abstract
Background
Perforations are major complications of endoscopic gastric resection, including endoscopic submucosal dissection (ESD), and are generally detected on chest radiography following ESD. We hypothesized that a small amount of free air, defined as “intraperitoneal air,” would not be noted on chest radiography. In this study we aimed to determine how often intraperitoneal air is seen on a computed tomography (CT) scan after ESD and to evaluate the association between clinical factors and intraperitoneal air.
Methods
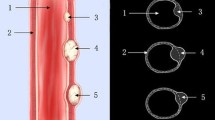
A total of 147 patients who underwent ESD for gastric neoplasms were analyzed between September 2009 and September 2010. Patients underwent both chest radiography and noncontrast CT scans. Intraperitoneal air on the CT scan was stratified by the amount of gas as follows: grade I, free air localized along the outside of the gastric wall; grade II, free air in the lesser sac; and grade III, free air in front of the liver.
Results
Intraperitoneal air was detected in 56 patients (38.1 %) by an abdominal CT scan, whereas free air was noted in 2 patients (1.4 %) by chest radiography. Most patients with intraperitoneal air (96.4 %, 54/56) were grade I or II and 3.6 % (2/56) were grade III. Abdominal pain was more frequent in the intraperitoneal air group (32.1 %, 18/56) than in the no intraperitoneal air group (17.6 %, 16/91; P = 0.042). Tumor location at the lesser curvature was more frequent in the intraperitoneal air group (66.1 %, 37/56) than in the no intraperitoneal air group (38.5 %, 35/91; P < 0.001). Fever, use of antibiotics, duration of hospital stay, C-reactive protein level, white blood cell count, complete resection, and local recurrence did not differ between the two groups. All patients who had intraperitoneal air recovered completely with medical treatment.
Conclusion
Intraperitoneal air after gastric ESD occurred unexpectedly frequently. However, a small amount of intraperitoneal air on a CT scan does not cause clinically significant complications.

Similar content being viewed by others
Abbreviations
- CRP:
-
C-reactive protein
- CT:
-
Computed tomography
- EGC:
-
Early gastric cancer
- EGD:
-
Esophagogastroduodenoscopy
- ESD:
-
Endoscopic submucosal dissection
References
Gotoda T, Yamamoto H, Soetikno RM (2006) Endoscopic submucosal dissection of early gastric cancer. J Gastroenterol 41:929–942
Gotoda T (2007) Endoscopic resection of early gastric cancer. Gastric Cancer 10:1–11
Onozato Y, Ishihara H, Iizuka H et al (2006) Endoscopic submucosal dissection for early gastric cancers and large flat adenomas. Endoscopy 38:980–986
Imagawa A, Okada H, Kawahara Y et al (2006) Endoscopic submucosal dissection for early gastric cancer: results and degrees of technical difficulty as well as success. Endoscopy 38:987–990
Cao Y, Liao C, Tan A, Gao Y, Mo Z, Gao F (2009) Meta-analysis of endoscopic submucosal dissection versus endoscopic mucosal resection for tumors of the gastrointestinal tract. Endoscopy 41:751–757
Choi IJ, Kim CG, Chang HJ, Kim SG, Kook MC, Bae JM (2005) The learning curve for EMR with circumferential mucosal incision in treating intramucosal gastric neoplasm. Gastrointest Endosc 62:860–865
Japanese Gastric Cancer Association (1998) Japanese classification of gastric carcinoma, 2nd English edition. Gastric Cancer 1:10–24
Gotoda T (2005) A large endoscopic resection by endoscopic submucosal dissection procedure for early gastric cancer. Clin Gastroenterol Hepatol 3:S71–S73
Fujishiro M, Yahagi N, Kakushima N et al (2006) Successful nonsurgical management of perforation complicating endoscopic submucosal dissection of gastrointestinal epithelial neoplasms. Endoscopy 38:1001–1006
Watari J, Tomita T, Toyoshima F et al (2012) The incidence of “silent” free air and aspiration pneumonia detected by CT after gastric endoscopic submucosal dissection. Gastrointest Endosc 76:1116–1123
Yoo JH, Shin SJ, Lee KM et al (2012) Risk factors for perforations associated with endoscopic submucosal dissection in gastric lesions: emphasis on perforation type. Surg Endosc 26:2456–2464
Watanabe K, Ogata S, Kawazoe S et al (2006) Clinical outcomes of EMR for gastric tumors: historical pilot evaluation between endoscopic submucosal dissection and conventional mucosal resection. Gastrointest Endosc 63:776–782
Oka S, Tanaka S, Kaneko I et al (2006) Advantage of endoscopic submucosal dissection compared with EMR for early gastric cancer. Gastrointest Endosc 64:877–883
Chung IK, Lee JH, Lee SH et al (2009) Therapeutic outcomes in 1000 cases of endoscopic submucosal dissection for early gastric neoplasms: Korean ESD Study Group multicenter study. Gastrointest Endosc 69:1228–1235
Kakushima N, Fujishiro M, Kodashima S et al (2006) Histopathologic characteristics of gastric ulcers created by endoscopic submucosal dissection. Endoscopy 38:412–415
Minami S, Gotoda T, Ono H, Oda I, Hamanaka H (2006) Complete endoscopic closure of gastric perforation induced by endoscopic resection of early gastric cancer using endoclips can prevent surgery (with video). Gastrointest Endosc 63:596–601
Tamiya Y, Nakahara K, Kominato K et al (2010) Pneumomediastinum is a frequent but minor complication during esophageal endoscopic submucosal dissection. Endoscopy 42:8–14
Onogi F, Araki H, Ibuka T et al (2010) “Transmural air leak”: a computed tomographic finding following endoscopic submucosal dissection of gastric tumors. Endoscopy 42:441–447
Classen M, Tytgat GNJ, Lightdale C (2010) Gastroenterological endoscopy, 2nd edn. Thieme, New York
Parra-Blanco A, Kaminaga N, Kojima T, Endo Y, Tajiri A, Fujita R (2000) Colonoscopic polypectomy with cutting current: is it safe? Gastrointest Endosc 51:676–681
Van Gossum A, Cozzoli A, Adler M, Taton G, Cremer M (1992) Colonoscopic snare polypectomy: analysis of 1485 resections comparing two types of current. Gastrointest Endosc 38:472–475
Lee H, Cheoi KS, Chung H et al (2012) Clinical features and predictive factors of coagulation syndrome after endoscopic submucosal dissection for early gastric neoplasm. Gastric Cancer 15:83–90
Acknowledgments
This study was funded by Grant 1310280 from the National Cancer Center, Korea.
Disclosures
Drs. Soo-Jeong Cho, Il Ju Choi, Soo Jin Kim, Min Ju Kim, Chan Gyoo Kim, Jong Yeul Lee, Keun Won Ryu, and Young-Woo Kim have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cho, SJ., Choi, I.J., Kim, S.J. et al. Clinical significance of intraperitoneal air on computed tomography scan after endoscopic submucosal dissection in patients with gastric neoplasms. Surg Endosc 28, 307–313 (2014). https://doi.org/10.1007/s00464-013-3188-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3188-9