Abstract
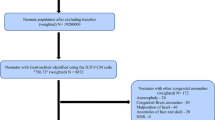
The objective of this study was to determine temporal trends of dysphagia diagnoses in hospitalized children. This is a retrospective observational study from the 1997–2012 Kids’ Inpatient Database (KID) conducted in the setting of weighted hospitalizations in a KID participating center. More than 6 million pediatric admissions were captured in each triennial KID report. Main outcomes included triennial rates of dysphagia diagnosis in hospitalized pediatric patients, and secondary outcomes included rates of dysphagia in premature and low-birthweight infants. Dysphagia diagnoses were coded in 5107/6607653 (0.08%) of these admissions in 1997, rising to 27,464/6,675,222 (0.41%) in 2012 (p < 0.001). The portion of these diagnoses in premature neonates has been increasing over time from 162/9551 (1.7%) in 2003 to 1027/27,464 (3.7%) by 2012 (p < 0.001). Similarly, low-birthweight children constituted 40/5107 (0.8%) of dysphagia diagnoses in 1997, a number that increased to 762/27,464 (2.8%) in 2012. Rates of dysphagia are increasing nationally, particularly in premature and low-birthweight infants, which may represent an increase alongside other neuroanatomic abnormalities. This growing problem illustrates the need for better data on the comparative efficacy of diagnostic and treatment modalities.



Similar content being viewed by others
Abbreviations
- LBW:
-
Low birthweight
- VLBW:
-
Very low birthweight
- MFM:
-
Maternal–Fetal medicine
- NNIC:
-
Neonatal intensive care
- KID:
-
Kids’ inpatient database
- HCUP:
-
Healthcare utilization project
- ICD-9:
-
International classification of disease, ninth revision
- SPSS:
-
Statistical package for the social sciences
- IQR:
-
Interquartile range
References
Venkata SPB, Durvasula MD, O’Neill AC. Oropharyngeal dysphagia in children. Otolaryngol Clin North Am. 2014;47(5):691–720.
Lefton-Greif MA, Arvedson JC. Pediatric feeding/swallowing: yesterday, today, and tomorrow. Semin Speech Lang. 2016;37(4):298–309.
Johnson JT, Rosen CA, Bailey BJ (2014) Bailey’s head and neck surgery–otolaryngology. Fifth edition. ed. Philadelphia, PA.: Wolters Kluwer Health/Lippincott Williams & Wilkins
Martin JA, Hamilton BE, Ventura SJ, et al. Births: final data for 2009. Nat Vital Stat Rep. 2011;60(1):1–70.
Stoll BJ, Hansen NI, Bell EF, et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993–2012. JAMA. 2015;314(10):1039–51.
Varga P, Berecz B, Gasparics A, et al. Morbidity and mortality trends in very-very low birth weight premature infants in light of recent changes in obstetric care. Eur J Obstet Gynecol Reprod Biol. 2017;211:134–9.
Zeballos-Sarrato S, Villar-Castro S, Zeballos-Sarrato G, Ramos-Navarro C, Gonzalez-Pacheco N, Sanchez Luna M. Survival estimations at the limit of viability. The J Mat-Fet Neonatal Med. 2016;29(22):3660–4.
Bhattacharyya N. The prevalence of pediatric voice and swallowing problems in the United States. The Laryngoscope. 2015;125(3):746–50.
Riordan MM, Iwata BA, Wohl MK, Finney JW. Behavioral treatment of food refusal and selectivity in developmentally disabled children. Appl Res in Mental Retardat. 1980;1(1–2):95–112.
Babbitt RL, Hoch TA, Coe DA, et al. Behavioral assessment and treatment of pediatric feeding disorders. J develop behav pediatr. 1994;15(4):278–91.
Rommel N, De Meyer AM, Feenstra L, Veereman-Wauters G. The complexity of feeding problems in 700 infants and young children presenting to a tertiary care institution. J Pediatr Gastroenterol Nutr. 2003;37(1):75–84.
Seddon PC, Khan Y. Respiratory problems in children with neurological impairment. Arch Dis Child. 2003;88(1):75–8.
Kramer SS. Special swallowing problems in children. Gastrointestinal Radiol. 1985;10(3):241–50.
Lau C, Smith EO, Schanler RJ. Coordination of suck-swallow and swallow respiration in preterm infants. Acta Paediatrica. 2003;92(6):721–7.
Rempel G, Moussavi Z. The effect of viscosity on the breath-swallow pattern of young people with cerebral palsy. Dysphagia. 2005;20(2):108–12.
Rommel N, van Wijk M, Boets B, et al. Development of pharyngo-esophageal physiology during swallowing in the preterm infant. Neurogastroenterol motil. 2011;23(10):e401–8.
Uhm KE, Yi SH, Chang HJ, Cheon HJ, Kwon JY. Videofluoroscopic swallowing study findings in full-term and preterm infants with Dysphagia. Annal Rehabilit Med. 2013;37(2):175–82.
Ancel PY, Livinec F, Larroque B, et al. Cerebral palsy among very preterm children in relation to gestational age and neonatal ultrasound abnormalities: the EPIPAGE cohort study. Pediatrics. 2006;117(3):828–35.
Uccella S, De Carli A, Sirgiovanni I, et al. Survival rate and neurodevelopmental outcome of extremely premature babies: an 8-year experience of an Italian single neonatal tertiary care center. La Pediatria medica e chirurgica. 2015. https://doi.org/10.4081/pmc.2015.106.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Disclosure
The authors have nothing to disclose.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Horton, J., Atwood, C., Gnagi, S. et al. Temporal Trends of Pediatric Dysphagia in Hospitalized Patients. Dysphagia 33, 655–661 (2018). https://doi.org/10.1007/s00455-018-9884-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-018-9884-9