Abstract
Purpose
Prostaglandin-mediated inflammatory reactions play a major role in different cancers. Recently, it has been observed that prostaglandin E2-receptor 3 (EP3) might be an independent prognostic factor for overall survival in cervical and endometrial cancer. The role of EP3 expression in ovarian cancer is currently unknown.
Methods
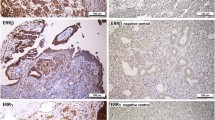
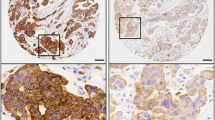
EP3 expression was analyzed by immunohistochemistry in 156 patient samples using the IR-scoring system. Expression levels were correlated with clinical and pathological parameters and with overall survival (OS) to assess for prognostic relevance. Data analysis was performed using Spearman’s correlations, Kruskal–Wallis test and Kaplan–Meier estimates.
Results
EP3 expression was significantly higher in clear-cell carcinoma (p < 0.001) compared to the other histological subtypes. No further correlations with clinical parameters could be found. EP3 expression correlated significantly with FSH-receptor expression (p < 0.001), galectin-1 expression in the tumor (p = 0.012) and with cytoplasmatic TA-MUC1 expression (p = 0.001). None of these parameters showed significant correlation with OS. In the TA-MUC1 negative subgroup, EP3 negative patients showed significantly longer OS (median OS: 102 months vs. 34 months in EP3 positive patients, p = 0.035), while EP3 did not appear to have prognostic relevance in the TA-MUC1-positive subgroup.
Conclusion
The potential prognostic relevance of EP3 expression for OS in TA-MUC1 negative patients might reflect an interplay between the COX and the MUC1 pathway, as it has been shown that MUC1 could induce COX2 expression. Our findings support the importance of the prostanoid signaling in TA-MUC1 negative ovarian cancer; however, future studies are necessary to characterize specific pathways and possible interactions.



Similar content being viewed by others
Data availability
The data sets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Aletti GD, Gostout BS, Podratz KC, Cliby WA (2006) Ovarian cancer surgical resectability: relative impact of disease, patient status, and surgeon. Gynecol Oncol 100(1):33–37
Ali-Fehmi R, Morris RT, Bandyopadhyay S, Che M, Schimp V, Malone JM Jr et al (2005) Expression of cyclooxygenase-2 in advanced stage ovarian serous carcinoma: correlation with tumor cell proliferation, apoptosis, angiogenesis, and survival. Am J Obstet Gynecol 192(3):819–825
Baldwin LA, Huang B, Miller RW, Tucker T, Goodrich ST, Podzielinski I et al (2012) Ten-year relative survival for epithelial ovarian cancer. Obstet Gynecol 120(3):612–618
Bertagnolli MM, Eagle CJ, Zauber AG, Redston M, Solomon SD, Kim K et al (2006) Celecoxib for the prevention of sporadic colorectal adenomas. N Engl J Med 355(9):873–884
Chetry M, Thapa S, Hu X, Song Y, Zhang J, Zhu H et al (2018) The Role of galectins in tumor progression, treatment and prognosis of gynecological cancers. J Cancer 9(24):4742–4755
Dembo AJ, Davy M, Stenwig AE, Berle EJ, Bush RS, Kjorstad K (1990) Prognostic factors in patients with stage I epithelial ovarian cancer. Obstet Gynecol 75(2):263–273
Dian D, Lenhard M, Mayr D, Heublein S, Karsten U, Goletz S et al (2013) Staining of MUC1 in ovarian cancer tissues with PankoMab-GEX detecting the tumour-associated epitope, TA-MUC1, as compared to antibodies HMFG-1 and 115D8. Histol Histopathol 28(2):239–244
du Bois A, Reuss A, Pujade-Lauraine E, Harter P, Ray-Coquard I, Pfisterer J (2009) Role of surgical outcome as prognostic factor in advanced epithelial ovarian cancer: a combined exploratory analysis of 3 prospectively randomized phase 3 multicenter trials: by the Arbeitsgemeinschaft Gynaekologische Onkologie Studiengruppe Ovarialkarzinom (AGO-OVAR) and the Groupe d’Investigateurs Nationaux Pour les Etudes des Cancers de l’Ovaire (GINECO). Cancer 115(6):1234–1244
Emons G, Pahwa GS, Ortmann O, Knuppen R, Oberheuser F, Schulz KD (1990) LHRH-receptors and LHRH-agonist treatment in ovarian cancer: an overview. J Steroid Biochem Mol Biol 37(6):1003–1006
Harris RE (2009) Cyclooxygenase-2 (cox-2) blockade in the chemoprevention of cancers of the colon, breast, prostate, and lung. Inflammopharmacology 17(2):55–67
Heidegger H, Dietlmeier S, Ye Y, Kuhn C, Vattai A, Aberl C et al (2017) The prostaglandin EP3 receptor is an independent negative prognostic factor for cervical cancer patients. Int J Mol Sci 18(7):1571. https://doi.org/10.3390/ijms18071571
Heublein S, Page S, Mayr D, Schmoeckel E, Trillsch F, Marme F et al (2019) Potential interplay of the gatipotuzumab epitope TA-MUC1 and estrogen receptors in ovarian cancer. Int J Mol Sci 20(2):295. https://doi.org/10.3390/ijms20020295
Hou R, Jiang L, Liu D, Lin B, Hu Z, Gao J et al (2017) Lewis(y) antigen promotes the progression of epithelial ovarian cancer by stimulating MUC1 expression. Int J Mol Med 40(2):293–302
Howe LR (2007) Inflammation and breast cancer. Cyclooxygenase/prostaglandin signaling and breast cancer. Breast Cancer Res 9(4):210
Kossai M, Leary A, Scoazec JY, Genestie C (2018) Ovarian cancer: a heterogeneous disease. Pathobiology 85(1–2):41–49
Ledermann J, Sehouli J, Zurawski B, Raspagliesi F, De Giorgi U, Banerjee S et al (2017) LBA41A double-blind, placebo-controlled, randomized, phase 2 study to evaluate the efficacy and safety of switch maintenance therapy with the anti-TA-MUC1 antibody PankoMab-GEX after chemotherapy in patients with recurrent epithelial ovarian carcinoma. Ann Oncol 28(suppl_8):viii46–viii50
Matsumura N, Yamamoto M, Aruga A, Takasaki K, Nakano M (2002) Correlation between expression of MUC1 core protein and outcome after surgery in mass-forming intrahepatic cholangiocarcinoma. Cancer 94(6):1770–1776
Mukherjee P, Basu GD, Tinder TL, Subramani DB, Bradley JM, Arefayene M et al (2009) Progression of pancreatic adenocarcinoma is significantly impeded with a combination of vaccine and COX-2 inhibition. J Immunol 182(1):216–224
Nath S, Roy LD, Grover P, Rao S, Mukherjee P (2015) Mucin 1 regulates Cox-2 gene in pancreatic cancer. Pancreas 44(6):909–917
Niringiyumukiza JD, Cai H, Xiang W (2018) Prostaglandin E2 involvement in mammalian female fertility: ovulation, fertilization, embryo development and early implantation. Reprod Biol Endocrinol 16(1):43
Obermajer N, Muthuswamy R, Odunsi K, Edwards RP, Kalinski P (2011) PGE(2)-induced CXCL12 production and CXCR38 expression controls the accumulation of human MDSCs in ovarian cancer environment. Can Res 71(24):7463–7470
Perales-Puchalt A, Svoronos N, Rutkowski MR, Allegrezza MJ, Tesone AJ, Payne KK et al (2017) Follicle-stimulating hormone receptor is expressed by most ovarian cancer subtypes and is a safe and effective immunotherapeutic target. Clin Cancer Res 23(2):441–453
Rask K, Zhu Y, Wang W, Hedin L, Sundfeldt K (2006) Ovarian epithelial cancer: a role for PGE2-synthesis and signalling in malignant transformation and progression. Mol Cancer 5:62
Reader J, Holt D, Fulton A (2011) Prostaglandin E2 EP receptors as therapeutic targets in breast cancer. Cancer Metastasis Rev 30(3–4):449–463
Rodriguez-Burford C, Barnes MN, Oelschlager DK, Myers RB, Talley LI, Partridge EE et al (2002) Effects of nonsteroidal anti-inflammatory agents (NSAIDs) on ovarian carcinoma cell lines: preclinical evaluation of NSAIDs as chemopreventive agents. Clin Cancer Res 8(1):202–209
Schulz H, Schmoeckel E, Kuhn C, Hofmann S, Mayr D, Mahner S et al (2017) Galectins-1, -3, and -7 are prognostic markers for survival of ovarian cancer patients. Int J Mol Sci 18(6):1230. https://doi.org/10.3390/ijms18061230
Schulz H, Kuhn C, Hofmann S, Mayr D, Mahner S, Jeschke U et al (2018) Overall survival of ovarian cancer patients is determined by expression of galectins-8 and -9. Int J Mol Sci 19(1):323. https://doi.org/10.3390/ijms19010323
Semmlinger A, von Schoenfeldt V, Wolf V, Meuter A, Kolben TM, Kolben T et al (2018) EP3 (prostaglandin E2 receptor 3) expression is a prognostic factor for progression-free and overall survival in sporadic breast cancer. BMC Cancer 18(1):431
Siegel RL, Miller KD, Jemal A (2019) Cancer statistics. CA Cancer J Clin 69(1):7–34
Sugimoto Y, Narumiya S (2007) Prostaglandin E receptors. J Biol Chem 282(16):11613–11617
Tinder TL, Subramani DB, Basu GD, Bradley JM, Schettini J, Million A et al (2008) MUC1 enhances tumor progression and contributes toward immunosuppression in a mouse model of spontaneous pancreatic adenocarcinoma. J Immunol 181(5):3116–3125
Tsujii M, Kawano S, DuBois RN (1997) Cyclooxygenase-2 expression in human colon cancer cells increases metastatic potential. Proc Natl Acad Sci USA 94(7):3336–3340
Vergote I, De Brabanter J, Fyles A, Bertelsen K, Einhorn N, Sevelda P et al (2001) Prognostic importance of degree of differentiation and cyst rupture in stage I invasive epithelial ovarian carcinoma. Lancet 357(9251):176–182
Wang D, Dubois RN (2010) Eicosanoids and cancer. Nat Rev Cancer 10(3):181–193
Williams CS, Mann M, DuBois RN (1999) The role of cyclooxygenases in inflammation, cancer, and development. Oncogene 18(55):7908–7916
Ye Y, Vattai A, Ditsch N, Kuhn C, Rahmeh M, Mahner S et al (2018) Prostaglandin E2 receptor 3 signaling is induced in placentas with unexplained recurrent pregnancy losses. Endocr Connect 7(5):749–761
Zhu J, Trillsch F, Mayr D, Kuhn C, Rahmeh M, Hofmann S et al (2018) Prostaglandin receptor EP3 regulates cell proliferation and migration with impact on survival of endometrial cancer patients. Oncotarget 9(1):982–994
Zhuandi G, Tuanjie C, Luju L, Abdiryim A, Yingying D, Haoqin L et al (2018) FSH receptor binding inhibitor restrains follicular development and possibly attenuates carcinogenesis of ovarian cancer through down-regulating expression levels of FSHR and ERbeta in normal ovarian tissues. Gene 668:174–181
Funding
This study was funded by laboratory resources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A.H. has received research grants from the “Walter Schulz Stiftung” and honoraria from Roche and Pfizer. S.M. received research support, advisory board, honoraria and travel expenses from AstraZeneca, Clovis, Medac, MSD, PharmaMar, Roche, Sensor Kinesis, Tesaro and Teva. F.T. declares research support, advisory board, honoraria and travel expenses from AstraZeneca, Medac, PharmaMar, Roche, and Tesaro. S.H. reports grants from Baden-Württemberg Ministry of Science, Research and the Arts, from StuRa Ruprecht-Karls-University of Heidelberg, FöFoLe LMU Munich Medical Faculty, grants from FERRING, personal fees from Roche, other from Astra Zeneca, grants from Novartis Oncology, grants and non-financial support from Apceth GmbH, non-financial support from Addex and grants from Heuer Stiftung. She further reports grants from Deutsche Forschungsgemeinschaft within the funding program Open Access Publishing, by the Baden-Württemberg Ministry of Science, Research and the Arts and by Ruprecht-Karls-University Heidelberg, outside the submitted work. All other authors declare no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The current study was approved by the Ethics Committee of the Ludwig-Maximilians-University, Munich, Germany (approval number 227-09 and 18-392).
Informed consent
This study used tumor tissue that had initially been collected for histo-pathological diagnostics. At the time, the tissue was examined for the current study, all diagnostic procedures had already been fully completed, and the tissue used was thus classified as left-over material. All patient data were fully anonymized, the Ethics Committee of the Ludwig-Maximilians-University (Munich, Germany) approved the study (227-09 and 18-392), and the study was performed according to the standards set in the Declaration of Helsinki 1975. As per declaration of our ethics committee, no written informed consent of the participants or permission to publish is needed given the circumstances described above. Researchers were blinded from patient data during experimental and statistical analyses.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Czogalla, B., Kuhn, C., Heublein, S. et al. EP3 receptor is a prognostic factor in TA-MUC1-negative ovarian cancer. J Cancer Res Clin Oncol 145, 2519–2527 (2019). https://doi.org/10.1007/s00432-019-03017-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-019-03017-8