Abstract
Purpose
Submandibular gland (SMG) carcinoma has an unfavorable clinical course and a low survival rate. Specific tumor and nodal findings might help predict posttreatment recurrence and survival in SMG carcinoma patients. This study evaluated factors predictive of posttreatment recurrence and survival in SMG carcinoma patients.
Methods
This study enrolled 99 consecutive patients with previously untreated SMG carcinoma. All patients underwent tumor and metastatic lymph node resection along with or without radiation/chemo-radiation. The predictive clinical and pathological factors for disease-free survival (DFS), distant metastasis–free survival (DMFS), disease-specific survival (DSS), and overall survival (OS) were determined using univariate and multivariate Cox proportional hazards regression analyses.
Results
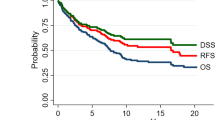
The median tumor size was 2.7 cm and 53 patients (53.5%) had high-grade tumors. The rates of initial nodal and distant metastasis at initial presentation or follow-up were 45.5% and 42.4%, respectively. The actuarial 5-year DFS, DMFS, DSS, and OS rates were 46.4%, 55.9%, 61.5%, and 59.7%, respectively. The independent factors associated with poor DFS, DMFS, DSS, and OS outcomes (all p < 0.05) were T3–T4 classification and lymph node ratio. A histological high-grade tumor was an independent prognostic factor predictive of poor DMFS, DSS, and OS outcomes (all p < 0.05).
Conclusions
A high rate of distant site failure is associated with SMG carcinoma, resulting in a poor survival rate. Lymph node ratio might help predict recurrence, distant metastasis, and death due to SMG carcinoma.

Similar content being viewed by others
References
Ali S, Palmer FL, Yu C, DiLorenzo M, Shah JP, Kattan MW, Patel SG, Ganly I (2014) Postoperative nomograms predictive of survival after surgical management of malignant tumors of the major salivary glands. Ann Surg Oncol 21(2):637–642
Ali S, Bryant R, Palmer FL, DiLorenzo M, Shah JP, Patel SG, Ganly I (2015) Distant metastases in patients with carcinoma of the major salivary glands. Ann Surg Oncol 22(12):4014–4019
Amin MB, Greene ES, Byrd FL, Brookland DR, Washington RK MK (eds) (2017a) AJCC cancer staging manual, 8th edn. Springer, New York, pp 79–94
Amin MB, Greene ES, Byrd FL, Brookland DR, Washington RK MK (eds) (2017b) AJCC cancer staging manual, 8th edn. Springer, New York, pp 55–181
Amini A, Waxweiler TV, Brower JV, Jones BL, McDermott JD, Raben D, Ghosh D, Bowles DW, Karam SD (2016) Association of adjuvant chemoradiotherapy vs radiotherapy alone with survival in patients with resected major salivary gland carcinoma: data from the national cancer data base. JAMA Otolaryngol Head Neck Surg 142(11):1100–1110
Argiris A, Karamouzis MV, Raben D, Ferris RL (2008) Head and neck cancer. Lancet 371(9625):1695–1709
Aro K, Ho AS, Luu M, Kim S, Tighiouart M, Clair JM, Yoshida EJ, Shiao SL, Leivo I, Zumsteg ZS (2018a) Development of a novel salivary gland cancer lymph node staging system. Cancer 124(15):3171–3180
Aro K, Tarkkanen J, Saat R, Saarilahti K, Makitie A, Atula T (2018b) Submandibular gland cancer: Specific features and treatment considerations. Head Neck 40(1):154–162
Barnes L, Reichart EJ, Sidransky P D (2005) Tumours of the salivary glands. In: WHO classification of tumours, vol 9, 3rd ednVolume. IARC Press, Lyon, pp 209–281
Bhattacharyya N (2004) Survival and prognosis for cancer of the submandibular gland. J Oral Maxillofac Surg 62(4):427–430
Cohen AN, Damrose EJ, Huang RY, Nelson SD, Blackwell KE, Calcaterra TC (2004) Adenoid cystic carcinoma of the submandibular gland: a 35-year review. Otolaryngol Head Neck Surg 131(6):994–1000
de Morais EF, Mafra RP, Gonzaga AKG, de Souza DLB, Pinto LP, da Silveira EJ (2017) Prognostic factors of oral squamous cell carcinoma in young patients: a systematic review. J Oral Maxillofac Surg 75(7):1555–1566
Denaro N, Merlano MC (2018) Immunotherapy in head and neck squamous cell cancer. Clin Exp Otorhinolaryngol 11(4):217–223
Denaro N, Merlano MC, Russi EG (2016) Follow-up in head and neck cancer: do more does it mean do better? A systematic review and our proposal based on our experience. Clin Exp Otorhinolaryngol 9(4):287–297
Ebrahimi A, Gil Z, Amit M, Yen TC, Liao CT, Chaturvedi P, Agarwal JP, Kowalski LP, Kohler HF, Kreppel M, Cernea CR, Brandao J, Bachar G, Bolzoni Villaret A, Fliss D, Fridman E, Robbins KT, Shah JP, Patel SG, Clark JR (2014) The prognosis of N2b and N2c lymph node disease in oral squamous cell carcinoma is determined by the number of metastatic lymph nodes rather than laterality: evidence to support a revision of the American Joint Committee on Cancer staging system. Cancer 120(13):1968–1974
Edge SB, Compton BD, Fritz CC, Greene AG, Trotti FL A, (eds) (2010) AJCC cancer staging manual, 7th edn. Springer, New York, pp 29–40.’ in
El-Naggar AK, Grandis CJ, Takata JR, Slootweg T PJ (2017) Tumours of salivary glands. In: WHO classification of tumours, vol 9, 4th edn. IARC Press, Lyon, pp 159–201
Heagerty PJ, Lumley T, Pepe MS (2000) Time-dependent ROC curves for censored survival data and a diagnostic marker. Biometrics 56(2):337–344
Ho AS, Kim S, Tighiouart M, Gudino C, Mita A, Scher KS, Laury A, Prasad R, Shiao SL, Van Eyk JE, Zumsteg ZS (2017) Metastatic lymph node burden and survival in oral cavity cancer. J Clin Oncol 35(31):3601–3609
Hong HR, Roh JL, Cho KJ, Choi SH, Nam SY, Kim SY (2015) Prognostic value of lymph node density in high-grade salivary gland cancers. J Surg Oncol 111(6):784–789
Hosni A, Huang SH, Goldstein D, Xu W, Chan B, Hansen A, Weinreb I, Bratman SV, Cho J, Giuliani M, Hope A, Kim J, O’Sullivan B, Waldron J, Ringash J (2016) Outcomes and prognostic factors for major salivary gland carcinoma following postoperative radiotherapy. Oral Oncol 54:75–80
Hsieh CE, Lee LY, Chou YC, Fan KH, Tsang NM, Chang JT, Wang HM, Ng SH, Liao CT, Yen TC, Fang KH, Lin CY (2018) Nodal failure patterns and utility of elective nodal irradiation in submandibular gland carcinoma treated with postoperative radiotherapy—a multicenter experience. Radiat Oncol 13(1):184
Jegadeesh N, Liu Y, Prabhu RS, Magliocca KR, Marcus DM, Higgins KA, Vainshtein JM, Wadsworth TJ, Beitler JJ (2015) Outcomes and prognostic factors in modern era management of major salivary gland cancer. Oral Oncol 51(8):770–777
Kim BH, Park SJ, Jeong WJ, Ahn SH (2018) Comparison of treatment outcomes for T3 glottic squamous cell carcinoma: a meta-analysis. Clin Exp Otorhinolaryngol 11(1):1–8
Laurie SA, Ho AL, Fury MG, Sherman E, Pfister DG (2011) Systemic therapy in the management of metastatic or locally recurrent adenoid cystic carcinoma of the salivary glands: a systematic review. Lancet Oncol 12(8):815–824
Liu Y, Qin L, Zhuang R, Huang X, Su M, Han Z (2018) Nodal stage: Is it a prognostic factor for submandibular gland cancer?. J Oral Maxillofac Surg 76(8):1794–1799
Lydiatt WM, O’Sullivan MS, Paten B, Shah SG (2017) Major salivary glands. In: Edge SB, Byrd DR, Brookland RK, Washington MK, Gershenwald JE, Compton CC, Hess KR, Sulivan DC, Jessup JM, Brierley JD, Gaspar LE, Schilsky RL, Balch CM, Winchester DP, Asare EA, Madera M (edn) AJCC cancer staging manual, 8th edn. Springer, Chicago, pp 95–102
Mallik S, Agarwal J, Gupta T, Kane S, Laskar SG, Budrukkar A, Murthy V, Goel V, Jain S (2010) Prognostic factors and outcome analysis of submandibular gland cancer: a clinical audit. J Oral Maxillofac Surg 68(9):2104–2110
National Comprehensive Cancer Network (NCCN) (2018) NCCN clinical practice guidelines in oncology: head and neck cancers. Version I. Fort Washington, PA
Noh JM, Ahn YC, Nam H, Park W, Baek CH, Son YI, Jeong HS (2010) Treatment results of major salivary gland cancer by surgery with or without postoperative radiation therapy. Clin Exp Otorhinolaryngol 3(2):96–101
Pinkston JA, Cole P (1999) Incidence rates of salivary gland tumors: results from a population-based study. Otolaryngol Head Neck Surg 120(6):834–840
Qian K, Di L, Guo K, Zheng X, Ji Q, Wang Z (2018) Cervical lymph node metastatic status and adjuvant therapy predict the prognosis of salivary duct carcinoma. J Oral Maxillofac Surg 76(7):1578–1586
Renehan A, Gleave EN, Hancock BD, Smith P, McGurk M (1996) Long-term follow-up of over 1000 patients with salivary gland tumours treated in a single centre. Br J Surg 83(12):1750–1754
Roh JL, Choi SH, Lee SW, Cho KJ, Nam SY, Kim SY (2008) ‘Carcinomas arising in the submandibular gland: high propensity for systemic failure’. J Surg Oncol 97(6):533–537
Speight PM, Barrett AW (2002) ‘Salivary gland tumours’. Oral Dis 8(5):229–240
Storey MR, Garden AS, Morrison WH, Eicher SA, Schechter NR, Ang KK (2001) ‘Postoperative radiotherapy for malignant tumors of the submandibular gland’. Int J Radiat Oncol Biol Phys 51(4):952–958
Suh JD, Cho JH (2016) Trends in head and neck cancer in South Korea between 1999 and 2012. Clin Exp Otorhinolaryngol 9(3):263–269
Suzuki H, Hanai N, Hirakawa H, Nishikawa D, Hasegawa Y (2015) Lymph node density is a prognostic factor in patients with major salivary gland carcinoma. Oncol Lett 10(6):3523–3528
Sykes AJ, Slevin NJ, Birzgalis AR, Gupta NK (1999) Submandibular gland carcinoma; an audit of local control and survival following adjuvant radiotherapy. Oral Oncol 35(2):187–190
Thompson L (2006) ‘World Health Organization classification of tumours: pathology and genetics of head and neck tumours. Ear Nose Throat J 85(2):74
Vander Poorten VL, Balm AJ, Hilgers FJ, Tan IB, Loftus-Coll BM, Keus RB, Hart AA (1999) Prognostic factors for long term results of the treatment of patients with malignant submandibular gland tumors. Cancer 85(10):2255–2264
Yamada K, Honda K, Tamaki H, Tanaka S, Shinohara S, Takebayashi S, Tateya I, Kitamura M, Mizuta M, Maetani T, Kojima T, Kitani Y, Asato R, Ichimaru K, Kumabe Y, Ushiro K, Omori K (2018) Survival in patients with submandibular gland carcinoma—results of a multi-institutional retrospective study. Auris Nasus Larynx 45(5):1066–1072
Zheng CM, Ji YB, Song CM, Ge MH, Tae K (2018) Number of metastatic lymph nodes and ratio of metastatic lymph nodes to total number of retrieved lymph nodes are risk factors for recurrence in patients with clinically node negative papillary thyroid carcinoma. Clin Exp Otorhinolaryngol 11(1):58–64
Funding
None reported.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research board and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors. Informed consent from all individual participants was waved because of the retrospective nature of this study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cho, W.K., Roh, JL., Cho, KJ. et al. Lymph node ratio predictive of recurrence, distant metastasis, and survival in submandibular gland carcinoma patients. J Cancer Res Clin Oncol 145, 1055–1062 (2019). https://doi.org/10.1007/s00432-019-02876-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-019-02876-5