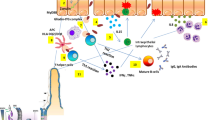
Abstract
Exclusive enteral nutrition (EEN) has been recommended as the first-line therapy in children with active Crohn disease (CD). The primary aim of our study was to determine whether it is possible to use the difference between basal fecal calprotectin (F-CPT) and the value at week 2 of EEN to predict clinical response at week 6. We prospectively collected stool samples for F-CPT analysis and clinical and laboratory parameters during EEN from 38 pediatric patients (28 boys, median age 12.8 years) with newly diagnosed active luminal CD. The difference between F-CPT concentrations before EEN and at week 2 did not predict clinical non-response at week 6 (OR 0.9996 95% CI 0.9989–1.0002, p = 0.18); however, it predicted patients who did not achieve clinical remission at week 6 (OR 0.9993, 95% CI 00.9985–0.9998, p = 0.006) with sensitivity of 58%, and specificity of 92% for cut-off of F-CPT increase by 486 μg/g.
Conclusions: An early decrease in F-CPT levels in children with newly diagnosed active luminal CD did not predict clinical response at week 6 of EEN induction therapy, and clinical remission was predicted with low accuracy. Therefore, F-CPT cannot be used as a predictor to select the patients in whom EEN should be terminated.
What is Known: | |
• The fecal calprotectin (F-CPT) is an important marker of intestinal inflammation. | |
• Approximately 25% of pediatric patients with Crohn disease (CD) do not achieve clinical remission, and there is still no sufficient predictor of response to exclusive enteral nutrition (EEN) treatment. | |
What is New: | |
• The difference between the F-CPT concentrations before EEN treatment and at week 2 did not predict clinical response to treatment at week 6, even if it predicted clinical remission, however, with low accuracy. F-CPT is not a suitable predictor to select the patients for discontinuing of EEN induction therapy. |


Similar content being viewed by others
Change history
02 October 2018
This article was originally published with all author names incorrectly listed. All author names have now been transposed and appear correctly above. The original article was corrected.
Abbreviations
- AUC :
-
Area under the curve
- AZA :
-
Azathioprine
- CD :
-
Crohn disease
- CI :
-
Confidence interval
- CRP :
-
C-reactive protein
- ECCO :
-
European Crohn and Colitis Organization
- EEN :
-
Exclusive enteral nutrition
- ELIA :
-
Fluorescence immunoassay
- ESR :
-
Erythrocyte sedimentation rate
- F-CPT :
-
Fecal calprotectin
- IQR :
-
Interquartile ranges
- OR :
-
Odds ratio
- ROC :
-
Receiver operating characteristic
- wPCDAI :
-
Weighted Pediatric Crohn Disease Activity Index
References
Bannerjee K, Camacho-hu C, Babinska K, Dryhurst KM, Edwards R, Savage MO, et al. (2004) Anti-inflammatory and growth-stimulating effects precede nutritional restitution during enteral feeding in Crohn disease, (March), 270–275
Berni Canani R, Terrin G, Borrelli O, Romano MT, Manguso F, Coruzzo A et al (2006) Short- and long-term therapeutic efficacy of nutritional therapy and corticosteroids in paediatric Crohn’s disease. Digest Liver Dis 38(6):381–387. https://doi.org/10.1016/j.dld.2005.10.005
Borrelli O, Cordischi L, Cirulli M, Paganelli M, Labalestra V, Uccini S, Russo PM, Cucchiara S (2006) Polymeric diet alone versus corticosteroids in the treatment of active pediatric Crohn’s disease: a randomized controlled open-label trial. Clin Gastroenterol Hepatol 4(6):744–753. https://doi.org/10.1016/j.cgh.2006.03.010
Buchanan E, Gaunt WW, Cardigan T, Garrick V, McGrogan P, Russell RK (2009) The use of exclusive enteral nutrition for induction of remission in children with Crohn’s disease demonstrates that disease phenotype does not influence clinical remission. Aliment Pharmacol Ther 30(5):501–507. https://doi.org/10.1111/j.1365-2036.2009.04067.x
D’Incà R, Pont E, Leo V, Ferronato A, Fries W, Vettorato MG et al (2007) Calprotectin and lactoferrin in the assessment of intestinal inflammation and organic disease. Int J Color Dis 22(4):429–437. https://doi.org/10.1007/s00384-006-0159-9
Day AS, Whitten KE, Lemberg DA, Clarkson C, Vitug-Sales M, Jackson R, Bohane TD (2006) Exclusive enteral feeding as primary therapy for Crohn’s disease in Australian children and adolescents: a feasible and effective approach. J Gastroenterol Hepatol 21(10):1609–1614. https://doi.org/10.1111/j.1440-1746.2006.04294.x
Day AS, Whitten KE, Sidler M, Lemberg DA (2007) Systematic review: nutritional therapy in paediatric Crohn’s disease. Aliment Pharmacol Ther 27(4):293–307. https://doi.org/10.1111/j.1365-2036.2007.03578.x
Day AS, Whitten KE, Sidler M, Lemberg DA (2008) Systematic review: nutritional therapy in paediatric Crohn’s disease. Aliment Pharmacol Ther 27(4):293–307. https://doi.org/10.1111/j.1365-2036.2007.03578.x
Denis MA, Reenaers C, Fontaine F, Belaïche J, Louis E (2007) Assessment of endoscopic activity index and biological inflammatory markers in clinically active Crohn’s disease with normal C-reactiveprotein serum level. Inflamm Bowel Dis 13(9):1100–1105. https://doi.org/10.1002/ibd.20178
Dziechciarz P, Horvath A, Shamir R, Szajewska H (2007) Meta-analysis: enteral nutrition in active Crohn’s disease in children. Aliment Pharmacol Ther 26(6):795–806. https://doi.org/10.1111/j.1365-2036.2007.03431.x
Frivolt K, Schwerd T, Werkstetter KJ, Schwarzer A, Schatz SB, Bufler P, Koletzko S (2014) Repeated exclusive enteral nutrition in the treatment of paediatric Crohn’s disease: predictors of efficacy and outcome. Aliment Pharmacol Ther 39(12):1398–1407. https://doi.org/10.1111/apt.12770
Gerasimidis K, Nikolaou CK, Edwards CA, McGrogan P (2011) Serial fecal calprotectin changes in children with Crohn’s disease on treatment with exclusive enteral nutrition: associations with disease activity, treatment response, and prediction of a clinical relapse. J Clin Gastroenterol 45(3):234–239. https://doi.org/10.1097/MCG.0b013e3181f39af5
Gerasimidis K, Talwar D, Duncan A, Moyes P, Buchanan E, Hassan K, OʼReilly D, McGrogan P, Ann Edwards C (2012) Impact of exclusive enteral nutrition on body composition and circulating micronutrients in plasma and erythrocytes of children with active Crohn’s disease. Inflamm Bowel Dis 18(9):1672–1681. https://doi.org/10.1002/ibd.21916
Grover Z, Muir R, Lewindon P (2014) Exclusive enteral nutrition induces early clinical, mucosal and transmural remission in paediatric Crohn’s disease. J Gastroenterol 49(4):638–645. https://doi.org/10.1007/s00535-013-0815-0
Hämäläinen A, Sipponen T, Kolho K-L (2011) Infliximab in pediatric inflammatory bowel disease rapidly decreases fecal calprotectin levels. World J Gastroenterol 17(47):5166–5171. https://doi.org/10.3748/wjg.v17.i47.5166
Hill RJ (2014) Update on nutritional status, body composition and growth in paediatric inflammatory bowel disease. World J Gastroenterol: WJG 20(12):3191–3197. https://doi.org/10.3748/wjg.v20.i12.3191
Hradsky O (2016) Time to relapse in children with Crohn ’ s disease treated with azathioprine and nutritional therapy or corticosteroids. Dig Dis Sci 61:2041–2050. https://doi.org/10.1007/s10620-016-4103-8
Hradsky O, Ohem J, Mitrova K, Durilova M, Kotalova RA, Nevoral J et al (2014) Fecal calprotectin levels in children is more tightly associated with histological than with macroscopic endoscopy findings. Clin Lab 60(12):1993–2000. https://doi.org/10.7754/Clin.Lab.2014.140203
Jones J, Loftus EV Jr, Panaccione R, Chen LIS, Peterson S, Mcconnell J et al (2008) Relationships between disease activity and serum and fecal biomarkers in patients with Crohn’ s disease. YJCGH 6(11):1218–1224. https://doi.org/10.1016/j.cgh.2008.06.010
Kolho K-L, Sipponen T (2014) The long-term outcome of anti-tumor necrosis factor-α therapy related to fecal calprotectin values during induction therapy in pediatric inflammatory bowel disease. Scand J Gastroenterol 49(4):434–441. https://doi.org/10.3109/00365521.2014.886719
Konikoff MR, Denson LA (2006) Role of fecal calprotectin as a biomarker of intestinal inflammation in inflammatory bowel disease. Inflamm Bowel Dis 12(6):524–534. https://www.ncbi.nlm.nih.gov/pubmed/16775498
Lasson A, Stotzer P-O, Öhman L, Isaksson S, Sapnara M, Strid H (2015) The intra-individual variability of faecal calprotectin: a prospective study in patients with active ulcerative colitis. J Crohn’s Colitis 9(1):26–32. https://doi.org/10.1016/j.crohns.2014.06.002
Levine A, Koletzko S, Turner D, Escher JC, Cucchiara S, de Ridder L, Kolho KL, Veres G, Russell RK, Paerregaard A, Buderus S, Greer ML, Dias JA, Veereman-Wauters G, Lionetti P, Sladek M, Martin de Carpi J, Staiano A, Ruemmele FM, Wilson DC, European Society of Pediatric Gastroenterology, Hepatology, and Nutrition (2014) ESPGHAN revised Porto criteria for the diagnosis of inflammatory bowel disease in children and adolescents. J Pediatr Gastroenterol Nutr 58(6):795–806. https://doi.org/10.1097/MPG.0000000000000239
Ruemmele FM, Veres G, Kolho KL, Griffiths A, Levine A, Escher JC et al (2014) Consensus guidelines of ECCO/ESPGHAN on the medical management of pediatric Crohn’s disease. J Crohn’s Colitis 8:1179–1207. https://doi.org/10.1016/j.crohns.2014.04.005
Ruemmele FM, Hyams JS, Otley A, Griffiths A, Kolho K-L, Amil Dias J et al (2014) Outcome measures for clinical trials in paediatric IBD: an evidence-based, expert-driven practical statement paper of the paediatric ECCO committee. Gut 64:438–446. https://doi.org/10.1136/gutjnl-2014-307008
Sipponen T, Kärkkäinen P, Savilahti E, Kolho K-L, Nuutinen H, Turunen U et al (2008) Correlation of faecal calprotectin and lactoferrin with an endoscopic score for Crohn’s disease and histological findings. Aliment Pharmacol Ther 28(10):1221–1229. https://doi.org/10.1111/j.1365-2036.2008.03835.x
Stewart M, Day AS, Otley A (2011) Physician attitudes and practices of enteral nutrition as primary treatment of paediatric Crohn disease in North America. J Pediatr Gastroenterol Nutr 52(1):38–42. https://doi.org/10.1097/MPG.0b013e3181e2c724
Talbotec C, Schmitz J, Canioni D, Goulet O, Ruemmele FM (2011) Alimentary pharmacology and therapeutics the efficacy of exclusive nutritional therapy in paediatric Crohn’ s disease, comparing fractionated oral vs. continuous enteral feeding. 1332–1339.https://doi.org/10.1111/j.1365-2036.2011.04662.x
Tibble J, Teahon K, Thjodleifsson B, Roseth A, Sigthorsson G, Bridger S et al (2000) A simple method for assessing intestinal inflammation in Crohn’s disease. Gut 47(4):506–513. https://doi.org/10.1136/gut.47.4.506
Turner D, Griffiths AM, Walters TD, Seah T, Markowitz J, Pfefferkorn M et al (2012) Mathematical weighting of the Pediatric Crohn’ s Disease Activity Index ( PCDAI ) and comparison with its other short versions. 18(1):55–62. https://doi.org/10.1002/ibd.21649
Van Assche G, Dignass A, Panes J, Beaugerie L, Karagiannis J, Allez M et al (2010) The second European evidence-based consensus on the diagnosis and management of Crohn’s disease: definitions and diagnosis. J Crohn's Colitis 4(1):7–27. https://doi.org/10.1016/j.crohns.2009.12.003
Acknowledgments
The project was supported by the Grant Agency of Charles University in Prague, Project No. 136215, No. 364617, and No. 246216, and by the Czech Ministry of Health for the conceptual development of research organizations 00064203 (University Hospital Motol, Prague, Czech Republic).
Funding
Author Ivana Copova has received research grants from the Grant Agency of Charles University in Prague, Project No. 136215 and No. 246216. Author Tereza Lerchova has received a grant from the Grant Agency of Charles University in Prague, Project No. 364617. The project was supported by the Czech Ministry of Health for the conceptual development of research organizations 00064203 (University Hospital Motol, Prague, Czech Republic).
Author information
Authors and Affiliations
Contributions
Ivana Copova M.D. worked on the conception and design of the study as well as on background research, data collection, and its control and completion of the missing data, statistical analysis of data, and writing of this original article. She was responsible for financial planning and work efficiency within the budget of the study.
Ondrej Hradsky M.D., Assoc. Prof., Ph.D. worked on the conception and design of the study as well as on data collection and its control, statistical analysis of data, and revision of the original article. He critically revised the work for important intellectual content.
Kristyna Zarubova M.D. actively participated in data collection and its control in the context of the research, and revision of the original article.
Lucie Gonsorcikova M.D., Ph.D. participated in data collection and its control.
Kristyna Potuznikova M.D. participated in data collection and its control. She obtained the necessary documents from patients and their guardians, and revised the work.
Tereza Lerchova M.D. participated in data collection and its control. She obtained the necessary documents from patients and their guardians, and revised the work.
Jiri Nevoral M.D., Prof., Ph.D. worked on the conception and design of the study as well as on revision of the original article.
Jiri Bronsky M.D., Assoc. Prof., Ph.D. was responsible for leading the project team, he was involved in study scheduling, obtaining the necessary documents, highlighting potential problems, and proposing solutions. He critically revised the work critically for important intellectual content.
Corresponding author
Ethics declarations
The study was approved by the Ethics Committee of the authors’ institution (the Ethics Committee Reference number is 1491/16).
Conflict of interest
The authors alone are responsible for the content and writing of the paper. There is no direct conflict of interest in relation to the topic of this study in any of the authors. Jiri Bronsky received honoraria/speaker’s fees/coverage of travel expenses from AbbVie, MSD, Nutricia, Nestle, Biocodex, Walmark, and Ferring. Ondrej Hradsky received honoraria/speaker’s fees/coverage of travel expenses from AbbVie, MSD, Nutricia, Nestle, Biocodex, Falk, and Ferring.
Informed consent
The patients’ guardians received written information on the study and signed a consent form.
Additional information
Communicated by Peter de Winter
The original version of this article was revised: This article was originally published with all author names incorrectly listed. All author names have now been transposed and appear correctly above.
Electronic supplementary material
Fig. 3aFig. 3b
(PNG 86 kb)
(PNG 85 kb)
Prediction of the accuracy of the non-remission (a, b) based on the differences in the F-CPT levels between weeks 0 and 2. The non-remission was best predicted using an increase of fecal calprotectin (F-CPT) by 486 μg/g till week 2 and had a specificity of 92% and sensitivity of 58% (area under the curve (AUC) 0.753). Using cut-off of 1.47%, a specificity was 79% and sensitivity was 80% (AUC 0.788) to predict patient who did not achieve clinical remission at week 6 of exclusive enteral nutrition (EEN) treatment.
Rights and permissions
About this article
Cite this article
Copova, I., Hradsky, O., Zarubova, K. et al. Fecal calprotectin is not a clinically useful marker for the prediction of the early nonresponse to exclusive enteral nutrition in pediatric patients with Crohn disease. Eur J Pediatr 177, 1685–1693 (2018). https://doi.org/10.1007/s00431-018-3228-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-018-3228-5