Abstract
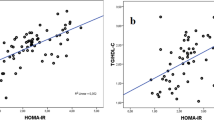
The study aims to assess the utility of the triglyceride-glucose index (TyG) as a marker of insulin resistance (IR) in neonates. TyG and the homeostatic model assessment (HOMA-IR) values were compared in 196 singleton, term normoweight and without distress newborns. A Decision Tree procedure (CHAID) was used to classify cases into groups or predict values of a dependent (Ln HOMA-IR) variable. Three nodes were drawn for TyG: ≤ 6.7, > 6.7–7.8 and > 7.8 (p < 0.0001; F = 20.52). The predictability of those TyG values vs HOMA-IR was statistically significant (p < 0.0001). It was neither affected by gender (p = 0.084), glucose challenge test (p = 0.138) classifications nor by the TyG node* glucose challenge test and TyG node*gender interactions (p = 0.456 and p = 0.209, respectively). Glucose, HOMA-IR, and the triglyceride/HDL cholesterol ratio increased progressively from node 1 to 3 for TyG while QUICKI decreased.
Conclusion: In conclusion, TyG appears to be a suitable tool for identifying IR at birth, justifying the further insulin determination in those neonates. TyG ≥ 7.8 is recommended as cut-off point in neonates. The need for a follow-up study to confirm the TyG as early IR marker is desirable.
What is Known
• HOMA-IR and the triglyceride-glucose index (TyG) show a high correlation.
• The TyG has been used as an insulin resistance marker in adults.
What is New
• This is the first study where TyG has been assessed in neonates.
• TyG appears to be a suitable and cheap tool for identifying insulin resistance at birth.

Similar content being viewed by others
Abbreviations
- CHAID:
-
Chi-squared automatic interaction detection
- GDM:
-
Gestational diabetes mellitus
- GH:
-
Growth hormone
- HDLc:
-
High density lipoprotein cholesterol
- HOMA-IR:
-
Homeostatic model assessment-insulin resistance
- IGF-1:
-
Insulin-like growth factor 1
- IGT:
-
Impaired glucose tolerance
- IR:
-
Insulin resistance
- MS:
-
Metabolic syndrome
- QUICKI:
-
Quantitative insulin sensitivity check index
- T2DM:
-
Type 2 diabetes mellitus
- TG:
-
Triglycerides
- TyG:
-
Triglyceride-glucose index
References
Abbasi F, Reaven GM (2011) Comparison of two methods using plasma triglyceride concentration as a surrogate estimate of insulin action in nondiabetic subjects: triglycerides × glucose versus triglyceride/high-density lipoprotein cholesterol. Metabolism 60(12):1673–1676. https://doi.org/10.1016/j.metabol.2011.04.006
Al-Hamad D, Raman V (2017) Metabolic syndrome in children and adolescents. Transl Pediatr 6(4):397–407. https://doi.org/10.21037/tp.2017.10.02
Bastida S, Sánchez-Muniz FJ, Cuesta C, Perea S, Aragonés A (1997) Male and female cord blood lipoprotein profile differences throughout the term-period. J Perinat Med 25(2):184–191. https://doi.org/10.1515/jpme.1997.25.2.184
Gesteiro E, Bastida S, Sánchez-Muniz FJ (2009) Insulin resistance markers in term, normoweight neonates. The Mérida cohort. Eur J Pediatr 168:281–288
Gesteiro E, Bastida S, Sánchez-Muniz FJ (2011) Effects of maternal glucose tolerance, pregnancy diet quality and neonatal insulinemia upon insulin resistance/sensitivity biomarkers in normoweight neonates. Nutr Hosp 26:1447–1455
Gesteiro E, Bastida S, Sánchez-Muniz FJ (2013) Cord-blood lipoproteins, homocysteine, insulin sensitivity/resistance marker profile, and concurrence of dysglycaemia and dyslipaemia in full-term neonates of the Merida study. Eur J Ped 172:883–894
Gesteiro E, Rodríguez Bernal B, Bastida S, Sánchez-Muniz FJ (2012) Maternal diets with low healthy eating index or Mediterranean diet adherence scores are associated with high cord-blood insulin levels and insulin resistance markers at birth. Eur J Clin Nutr 66(9):1008–1015. https://doi.org/10.1038/ejcn.2012.92
Gesteiro E, Sánchez-Muniz FJ, Bastida S (2017) Hypercortisolaemia and hyperinsulinaemia interaction and their impact upon insulin resistance/sensitivity markers at birth. In: Mauricio AC (ed) Blood banking for clinical application and regenerative medicine. InTech. Rijeka, Croatia, pp 69–98
Gesteiro E, Sánchez-Muniz FJ, Ortega-Azorín C, Guillén M, Corella D, Bastida S (2016) Maternal and neonatal FTO rs9939609 polymorphism affect insulin sensitivity markers and lipoprotein profile at birth in appropriate-for-gestational-age term neonates. J Physiol Biochem 72(2):169–181. https://doi.org/10.1007/s13105-016-0467-7
Guerrero Romero F, Simental Mendia LE, Gonzalez Ortiz M, Martinez Abundis E, Ramos Zavala MG, Hernandez Gonzalez SO et al (2010) The product of triglycerides and glucose, a simple measure of insulin sensitivity. Comparison with the euglycemic-hyperinsulinemic clamp. J Clin Endocrinol Metab 95(7):3347–3351. https://doi.org/10.1210/jc.2010-0288
Higgins V, Adeli K (2017) Pediatric metabolic syndrome: pathophysiology and laboratory assessment. EJIFCC 28(1):25–42
Irace C, Carallo C, Scavelli FB, De Franceschi MS, Esposito T, Tripolino C, Gnasso A (2013) Markers of insulin resistance and carotid atherosclerosis. A comparison of the homeostasis model assessment and triglyceride glucose index. Int J Clin Pract 67(Suppl. 7):665–672. https://doi.org/10.1111/ijcp.12124
Janghorbani M, Almasi SZ, Amini M (2015) The product of triglycerides and glucose in comparison with fasting plasma glucose did not improve diabetes prediction. Acta Diabetol 52(4):781–788. https://doi.org/10.1007/s00592-014-0709-5
de Jong M, Cranendonk A, van Weissenbruch MM (2015) Components of the metabolic syndrome in early childhood in very-low-birth-weight infants and term small and appropriate for gestational age infants. Pediatr Res 78:457–461
Kim JW, Park SH, Kim Y, Im M, Han HS (2016) The cutoff values of indirect indices for measuring insulin resistance for metabolic syndrome in Korean children and adolescents. Ann Pediatr Endocrinol Metab 21(3):143–148. https://doi.org/10.6065/apem.2016.21.3.143
Lissau I, Overpeck MD, Ruan WJ, Due P, Holstein BE, Hediger ML, Health behaviour in school-aged children obesity Working Group (2004) Body mass index and overweight in adolescents in 13 European countries, Israel, and the United States. Arch Pediatr Adolesc Med 158(1):27–33. https://doi.org/10.1001/archpedi.158.1.27
Mohd Nor NS, Lee S, Bacha F, Tfayli H, Arslanian S (2016) Triglyceride glucose index as a surrogate measure of insulin sensitivity in obese adolescents with normoglycemia, prediabetes, and type 2 diabetes mellitus: comparison with the hyperinsulinemic-euglycemic clamp. Pediatr Diabetes 17(6):458–465. https://doi.org/10.1111/pedi.12303
Muniyappa R, Lee S, Chen H, Quon MJ (2008) Current approaches for assessing insulin sensitivity and resistance in vivo: advantages, limitations, and appropriate usage. Am J Physiol Endocrinol Metab 294(1):E15–E26. https://doi.org/10.1152/ajpendo.00645.2007
Navarro-González D, Sánchez-Íñigo L, Pastrana-Delgado J, Fernández-Montero A, Martinez JA (2016) Triglyceride-glucose index (TyG index) in comparison with fasting plasma glucose improved diabetes prediction in patients with normal fasting glucose: the vascular-metabolic CUN cohort. Prev Med 86:99–105
Nielsen JH, Haase TN, Jaksch C, Nalla A, Søstrup B, Nalla AA, Larsen L, Rasmussen M, Dalgaard LT, Gaarn LW, Thams P, Kofod H, Billestrup N (2014) Impact of fetal and neonatal environment on beta cell function and development of diabetes. Acta Obstet Gynecol Scand 93(11):1109–1122. https://doi.org/10.1111/aogs.12504
O’Sullivan BA, Henderson ST, Davis JM (1998) Gestational diabetes. JAm Pharm Assoc (Wash) 38(3):364–371; quiz 372-373. https://doi.org/10.1016/S1086-5802(16)30332-1
Plagemann A (2005) Perinatal programming and functional teratogenesis: impact on body weight regulation and obesity. Physiol Behav 86(5):661–668. https://doi.org/10.1016/j.physbeh.2005.08.065
Rodríguez-Morán M, Simental-Mendía LE, Guerrero-Romero F (2017) The triglyceride and glucose index is useful for recognising insulin resistance in children. Acta Paediatr 106(6):979–983. https://doi.org/10.1111/apa.13789
Sánchez-Íñigo L, Navarro-González D, Fernández-Montero A, Pastrana-Delgado J, Martínez JA (2016) The TyG index may predict the development of cardiovascular events. Eur J Clin Investig 46(2):189–197. https://doi.org/10.1111/eci.12583
Sánchez-Muniz FJ, Gesteiro E, Espárrago Rodilla M, Rodríguez Bernal B, Bastida S (2013) Maternal nutrition during pregnancy conditions the fetal pancreas development, hormonal status and diabetes mellitus and metabolic syndrome biomarkers at birth. Nutr Hosp 28:250–274
Singh B, Saxena A (2010) Surrogate markers of insulin resistance: a review. World J Diabetes 1(2):36–47. https://doi.org/10.4239/wjd.v1.i2.36
Unger G, Benozzi SF, Perruzza F, Pennacchiotti GL (2014) Triglycerides and glucose index: a useful indicator of insulin resistance. Endocrinol Nutr 61(10):533–540. https://doi.org/10.1016/j.endonu.2014.06.009
Acknowledgements
We thank the Gynaecology and Obstetrics Department and Laboratory Services of Mérida Hospital (Extremadura, Spain) and participant mothers and neonates.
Funding
Partially supported by the Spanish Project AGL 2014-53207-C2-2-R.
Author information
Authors and Affiliations
Contributions
E Gesteiro contributed to the data acquisition, analysis, discussion and writing of the paper; FJ Sánchez-Muniz contributed to the study design, data discussion, writing of the paper and is the corresponding author and guarantor of the paper; S Bastida contributed to the study design and data discussion; L Barrios has contributed to the design and discussion of the statistical study.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
The study performed in accordance with the Helsinki Declaration of 1975 as revised in year 2000, following approval by the Management and Ethical Committee of the Hospital. Data were obtained from an anonymous hospital screening record.
Nonetheless, informed consent is available from 35 mothers whose pregnancy diet was studied and wished to be engaged in a follow-up study.
Additional information
Communicated by Mario Bianchetti
Rights and permissions
About this article
Cite this article
Gesteiro, E., Bastida, S., Barrios, L. et al. The triglyceride-glucose index, an insulin resistance marker in newborns?. Eur J Pediatr 177, 513–520 (2018). https://doi.org/10.1007/s00431-018-3088-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-018-3088-z