Abstract
Purpose
The aim was to compare changes in peripheral and cerebral oxygenation, as well as metabolic and performance responses during conditions of blood flow restriction (BFR, bilateral vascular occlusion at 0% vs. 45% of resting pulse elimination pressure) and systemic hypoxia (~ 400 m, FIO2 20.9% vs. ~ 3800 m normobaric hypoxia, FIO2 13.1 ± 0.1%) during repeated sprint tests to exhaustion (RST) between leg- and arm-cycling exercises.
Methods
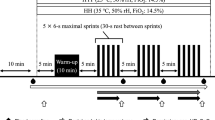
Seven participants (26.6 ± 2.9 years old; 74.0 ± 13.1 kg; 1.76 ± 0.09 m) performed four sessions of RST (10-s maximal sprints with 20-s recovery until exhaustion) during both leg and arm cycling to measure power output and metabolic equivalents as well as oxygenation (near-infrared spectroscopy) of the muscle tissue and prefrontal cortex.
Results
Mean power output was lower in arms than legs (316 ± 118 vs. 543 ± 127 W; p < 0.001) and there were no differences between conditions for a given limb. Arms demonstrated greater changes in concentration of deoxyhemoglobin (∆[HHb], − 9.1 ± 6.1 vs. − 6.5 ± 5.6 μm) and total hemoglobin concentration (∆[tHb], 15.0 ± 10.8 vs. 11.9 ± 7.9 μm), as well as the absolute maximum tissue saturation index (TSI, 62.0 ± 8.3 vs. 59.3 ± 8.1%) than legs, respectively (p < 0.001), demonstrating a greater capacity for oxygen extraction. Further, there were greater changes in tissue blood volume [tHb] during BFR only compared to all other conditions (p < 0.01 for all).
Conclusions
The combination of BFR and/or hypoxia led to increased changes in [HHb] and [tHb] likely due to greater vascular resistance, to which arms were more responsive than legs.


Similar content being viewed by others
Abbreviations
- ACSM:
-
American College of Sports Medicine
- BFR:
-
Blood flow restriction
- ES:
-
Effect size
- HHb:
-
Deoxyhemoglobin
- NIRS:
-
Near-infrared spectroscopy
- O2Hb:
-
Oxyhemoglobin
- RER:
-
Respiratory exchange ratio
- RPE:
-
Rate of perceived exertion
- RST:
-
Repeated sprint ability test to exhaustion
- S dec :
-
Percent decrement in RST
- S best :
-
Highest mean power of either of the first two sprints in RST
- SpO2 :
-
Pulse oxygen saturation
- tHb:
-
Total hemoglobin
- TSI:
-
Tissue saturation index
- V̇E:
-
Minute ventilation
- V̇O2 :
-
Maximal oxygen uptake
- ∆:
-
Delta change over time
References
Amann M, Calbet JA (2008) Convective oxygen transport and fatigue. J Appl Physiol 104:861–870. https://doi.org/10.1152/japplphysiol.01008.2007
Amann M, Kayser B (2009) Nervous system function during exercise in hypoxia. High Alt Med Biol 10:149–164. https://doi.org/10.1089/ham.2008.1105
Amann M, Romer LM, Subudhi AW, Pegelow DF, Dempsey JA (2007) Severity of arterial hypoxaemia affects the relative contributions of peripheral muscle fatigue to exercise performance in healthy humans. J Physiol 581:389–403. https://doi.org/10.1113/jphysiol.2007.129700
American College of Sports Medicine (2014) ACSM's guidelines for exercise testing and prescription. Lippincott Williams & Wilkins, Baltimore
Andersen P, Saltin B (1985) Maximal perfusion of skeletal muscle in man. J Physiol 366:233–249
Billaut F, Smith K (2010) Prolonged repeated-sprint ability is related to arterial O2 desaturation in men. Int J Sports Physiol Perform 5:197–209
Boushel R et al (2011) Muscle mitochondrial capacity exceeds maximal oxygen delivery in humans. Mitochondrion 11:303–307. https://doi.org/10.1016/j.mito.2010.12.006
Boushel R et al (2014) Low-intensity training increases peak arm VO2 by enhancing both convective and diffusive O2 delivery. Acta Physiol (Oxf) 211:122–134. https://doi.org/10.1111/apha.12258
Calbet JA (2000) Oxygen tension and content in the regulation of limb blood flow. Acta Physiol Scand 168:465–472. https://doi.org/10.1046/j.1365-201x.2000.00698.x
Calbet JA, Joyner MJ (2010) Disparity in regional and systemic circulatory capacities: do they affect the regulation of the circulation? Acta Physiol (Oxf) 199:393–406. https://doi.org/10.1111/j.1748-1716.2010.02125.x
Calbet JA, Holmberg HC, Rosdahl H, van Hall G, Jensen-Urstad M, Saltin B (2005) Why do arms extract less oxygen than legs during exercise? Am J Physiol Regul Integr Comp Physiol 289:R1448–1458. https://doi.org/10.1152/ajpregu.00824.2004
Calbet JA, Radegran G, Boushel R, Saltin B (2009) On the mechanisms that limit oxygen uptake during exercise in acute and chronic hypoxia: role of muscle mass. J Physiol 587:477–490. https://doi.org/10.1113/jphysiol.2008.162271
Calbet JA, Gonzalez-Alonso J, Helge JW, Sondergaard H, Munch-Andersen T, Saltin B, Boushel R (2015) Central and peripheral hemodynamics in exercising humans: leg vs. arm exercise. Scand J Med Sci Sports 25(Suppl 4):144–157. https://doi.org/10.1111/sms.12604
Clausen JP, Klausen K, Rasmussen B, Trap-Jensen J (1973) Central and peripheral circulatory changes after training of the arms or legs. Am J Physiol 225:675–682. https://doi.org/10.1152/ajplegacy.1973.225.3.675
Curtelin D et al. (2017) Cerebral blood flow, frontal lobe oxygenation and intra-arterial blood pressure during sprint exercise in normoxia and severe acute hypoxia in humans. J Cereb Blood Flow Metab https://doi.org/10.1177/0271678X17691986
Delp MD, Laughlin MH (1998) Regulation of skeletal muscle perfusion during exercise. Acta Physiol Scand 162:411–419. https://doi.org/10.1046/j.1365-201X.1998.0324e.x
Faiss R, Leger B, Vesin JM, Fournier PE, Eggel Y, Deriaz O, Millet GP (2013) Significant molecular and systemic adaptations after repeated sprint training in hypoxia. PLoS ONE 8:e56522. https://doi.org/10.1371/journal.pone.0056522
Glaister M, Howatson G, Pattison JR, McInnes G (2008) The reliability and validity of fatigue measures during multiple-sprint work: an issue revisited. J Strength Cond 22:1597–1601. https://doi.org/10.1519/JSC.0b013e318181ab80
Gualano B et al. (2010) Vascular occlusion training for inclusion body myositis: a novel therapeutic approach. J Vis Exp https://doi.org/10.3791/1894
Holmberg HC (2015) The elite cross-country skier provides unique insights into human exercise physiology. Scand J Med Sci Sports 25(Suppl 4):100–109. https://doi.org/10.1111/sms.12601
Kaijser L, Sundberg CJ, Eiken O, Nygren A, Esbjornsson M, Sylven C, Jansson E (1990) Muscle oxidative capacity and work performance after training under local leg ischemia. J Appl Physiol 69:785–787. https://doi.org/10.1152/jappl.1990.69.2.785
Kishi K, Kawaguchi M, Yoshitani K, Nagahata T, Furuya H (2003) Influence of patient variables and sensor location on regional cerebral oxygen saturation measured by INVOS 4100 near-infrared spectrophotometers. J Neurosurg Anesthesiol 15:302–306
Kolb JC, Ainslie PN, Ide K, Poulin MJ (2004) Protocol to measure acute cerebrovascular and ventilatory responses to isocapnic hypoxia in humans. Respir Physiol Neurobiol 141:191–199. https://doi.org/10.1016/j.resp.2004.04.014
Lenth RV (2016) Least-Squares Means: the R package lsmeans. J Stat Softw 69:33. https://doi.org/10.18637/jss.v069.i01
Nielsen HB, Madsen P, Svendsen LB, Roach RC, Secher NH (1998) The influence of PaO2, pH and SaO2 on maximal oxygen uptake. Acta Physiol Scand 164:87–89. https://doi.org/10.1046/j.1365-201X.1998.00405.x
Nielsen HB, Bredmose PP, Stromstad M, Volianitis S, Quistorff B, Secher NH (2002) Bicarbonate attenuates arterial desaturation during maximal exercise in humans. J Appl Physiol 93:724–731. https://doi.org/10.1152/japplphysiol.00398.2000
Pernow B, Saltin B, Wahren J, Cronestrand R, Ekestroom S (1975) Leg blood flow and muscle metabolism in occlusive arterial disease of the leg before and after reconstructive surgery. Clin Sci Mol Med 49:265–275
Physiology CSfE (2002) PAR-Q & YOU
Pinheiro J. BD, DebRoy S., Sarkar D., and R Core Team (2017) nlme: Linear and Nonlinear Mixed Effects Models. https://CRAN.R-project.org/package=nlme. Accessed Aug 2017
Rodriguez RF, Townsend NE, Aughey RJ, Billaut F (2018) Influence of averaging method on muscle deoxygenation interpretation during repeated-sprint exercise. Scand J Med Sci Sports https://doi.org/10.1111/sms.13238
Saltin B (1985) Hemodynamic adaptations to exercise. Am J Cardiol 55:42D–47D
Smith KJ, Billaut F (2010) Influence of cerebral and muscle oxygenation on repeated-sprint ability. Eur J Appl Physiol 109:989–999. https://doi.org/10.1007/s00421-010-1444-4
van der Zee P et al (1992) Experimentally measured optical pathlengths for the adult head, calf and forearm and the head of the newborn infant as a function of inter optode spacing. Adv Exp Med Biol 316:143–153
Wagner PD (1993) Algebraic analysis of the determinants of VO2, max. Respir Physiol 93:221–237
Willis SJ, Alvarez L, Borrani F, Millet GP (2018) Oxygenation time course and neuromuscular fatigue during repeated cycling sprints with bilateral blood flow restriction. Physiol Rep 6:e13872. https://doi.org/10.14814/phy2.13872
Wray DW, Uberoi A, Lawrenson L, Richardson RS (2005) Heterogeneous limb vascular responsiveness to shear stimuli during dynamic exercise in humans. J Appl Physiol 99:81–86. https://doi.org/10.1152/japplphysiol.01285.2004
Zinner C et al (2016) The physiological mechanisms of performance enhancement with sprint interval training differ between the upper and lower extremities in humans. Front Physiol 7:426. https://doi.org/10.3389/fphys.2016.00426
Acknowledgements
The authors would like to thank all participants for their efforts, patience, and cooperation with this study.
Author information
Authors and Affiliations
Contributions
SJW, FB, and GPM conceived and designed research. SJW conducted experiments. SJW and FB analyzed data. SJW, FB, and GPM wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Communicated by I. Mark Olfert.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Willis, S.J., Borrani, F. & Millet, G.P. Leg- vs arm-cycling repeated sprints with blood flow restriction and systemic hypoxia. Eur J Appl Physiol 119, 1819–1828 (2019). https://doi.org/10.1007/s00421-019-04171-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-019-04171-0