Abstract
Purpose
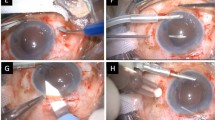
To report the short-term outcomes of a modified small-incision technique for implantation of scleral-fixated intraocular lenses (IOLs) using Gore-Tex sutures.
Methods
A retrospective, interventional, consecutive case series was conducted. From June 2019 to February 2020, 10 patients underwent small-incision scleral-fixated IOL implantation using Gore-Tex sutures at a tertiary referral center. Visual and anatomical outcomes and complications were recorded with a minimum follow-up period of 3 months. Surgically induced astigmatism (SIA) and IOL-induced astigmatism were measured.
Results
The mean follow-up duration (range) was 396 (240–573) days. Best-corrected visual acuity improved significantly from logarithm of the minimal angle of resolution (logMAR) 0.88 ± 0.65 (Snellen equivalent: 20/153) preoperation to logMAR = 0.30 ± 0.51 (Snellen equivalent: 20/40) at final follow-up (P = .008). The estimated SIA and IOL-induced astigmatism were 0.61 diopters (D) ± 0.49D and 0.40D ± 0.36D, respectively. No intraoperative complications occurred. The postoperative complications, which included ocular hypertension (20%), cystoid macular edema (30%), and vitreous hemorrhage (20%), were transient and resolved with topical medication.
Conclusions
The modified small-incision technique for implantation of scleral-fixated IOLs using Gore-Tex sutures was well tolerated in all patients, with favorable postoperative visual outcomes and minimal SIA and IOL-induced astigmatism.

Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Wagoner MD, Cox TA, Ariyasu RG, Jacobs DS, Karp CL, American Academy of O (2003) Intraocular lens implantation in the absence of capsular support: a report by the American Academy of Ophthalmology. Ophthalmology 110:840–859. https://doi.org/10.1016/s0161-6420(02)02000-6
Stem MS, Todorich B, Woodward MA, Hsu J, Wolfe JD (2017) Scleral-fixated intraocular lenses: past and present. J Vitreoretin Dis 1:144–152. https://doi.org/10.1177/2474126417690650
Vote BJ, Tranos P, Bunce C, Charteris DG, Da Cruz L (2006) Long-term outcome of combined pars plana vitrectomy and scleral fixated sutured posterior chamber intraocular lens implantation. Am J Ophthalmol 141:308–312. https://doi.org/10.1016/j.ajo.2005.09.012
Price MO, Price FW Jr, Werner L, Berlie C, Mamalis N (2005) Late dislocation of scleral-sutured posterior chamber intraocular lenses. J Cataract Refract Surg 31:1320–1326. https://doi.org/10.1016/j.jcrs.2004.12.060
Ma IH, Tsai CY, Yang CM, Lai TT (2019) Modified cow-hitch suture for repositioning of subluxated scleral-fixated rigid intraocular lens. Ophthalmic Surg Lasers Imaging Retina 50:179–182. https://doi.org/10.3928/23258160-20190301-08
Scharioth GB, Prasad S, Georgalas I, Tataru C, Pavlidis M (2010) Intermediate results of sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg 36:254–259. https://doi.org/10.1016/j.jcrs.2009.09.024
Czajka MP, Frajdenberg A, Stopa M, Pabin T, Johansson B, Jakobsson G (2020) Sutureless intrascleral fixation using different three-piece posterior chamber intraocular lenses: a literature review of surgical techniques in cases of insufficient capsular support and a retrospective multicentre study. Acta Ophthalmol 98:224–236. https://doi.org/10.1111/aos.14307
Stem MS, Wa CA, Todorich B, Woodward MA, Walsh MK, Wolfe JD (2019) 27-gauge sutureless intrascleral fixation of intraocular lenses with haptic flanging: short-term clinical outcomes and a disinsertion force study. Retina 39:2149–2154. https://doi.org/10.1097/IAE.0000000000002268
Khan MA, Gerstenblith AT, Dollin ML, Gupta OP, Spirn MJ (2014) Scleral fixation of posterior chamber intraocular lenses using gore-tex suture with concurrent 23-gauge pars plana vitrectomy. Retina 34:1477–1480. https://doi.org/10.1097/IAE.0000000000000233
Khan MA, Gupta OP, Smith RG, Ayres BD, Raber IM, Bailey RS, Hsu J, Spirn MJ (2016) Scleral fixation of intraocular lenses using Gore-Tex suture: clinical outcomes and safety profile. Br J Ophthalmol 100:638–643. https://doi.org/10.1136/bjophthalmol-2015-306839
Das S, Nicholson M, Deshpande K, Kummelil MK, Nagappa S, Shetty BK (2016) Scleral fixation of a foldable intraocular lens with polytetrafluoroethylene sutures through a Hoffman pocket. J Cataract Refract Surg 42:955–960. https://doi.org/10.1016/j.jcrs.2016.06.018
Khan MA, Samara WA, Gerstenblith AT, Chiang A, Mehta S, Garg SJ, Hsu J, Gupta OP (2018) combined pars plana vitrectomy and scleral fixation of an intraocular lens using gore-tex suture: one-year outcomes. Retina 38:1377–1384. https://doi.org/10.1097/IAE.0000000000001692
Patel NA, Shah P, Yannuzzi NA, Ansari Z, Zaveri JS, Relhan N, Williams BK Jr, Kuriyan AE, Henry CR, Sridhar J, Haddock L, Fortun JA, Albini TA, Davis JL, Flynn HW Jr (2018) Clinical outcomes of 4-point scleral fixated 1-piece hydrophobic acrylic equiconvex intraocular lens using polytetrafluoroethylene suture. Clin Ophthalmol 12:2145–2148. https://doi.org/10.2147/OPTH.S174211
Bonnell AC, Mantopoulos D, Fine HF, Shah SP, Wheatley HM, Prenner JL (2020) One-year outcomes of a novel surgical approach for fixation of a posterior chamber intraocular lens using Gore-Tex suture. Retina 40:833–837. https://doi.org/10.1097/IAE.0000000000002456
Cutler NE, Sridhar J, Khan MA, Gupta OP, Fineman MS (2017) Transconjunctival approach to scleral fixation of posterior chamber intraocular lenses using Gore-Tex suture. Retina 37:1003–1005. https://doi.org/10.1097/IAE.0000000000001333
Botsford BW, Williams AM, Conner IP, Martel JN, Eller AW (2019) Scleral fixation of intraocular lenses with Gore-Tex suture: refractive outcomes and comparison of lens power formulas. Ophthalmol Retina 3:468–472. https://doi.org/10.1016/j.oret.2019.02.005
Su D, Stephens JD, Obeid A, Borkar D, Storey PP, Khan MA, Hsu J, Garg SJ, Gupta O (2019) Refractive outcomes after pars plana vitrectomy and scleral fixated intraocular lens with Gore-Tex suture. Ophthalmol Retina 3:548–552. https://doi.org/10.1016/j.oret.2019.02.012
Sanchez-Tabernero S (2018) SIA-formula: an easy way to calculate surgically induced astigmatism. Eye (Lond) 32:659–660. https://doi.org/10.1038/eye.2017.232
Masket S, Wang L, Belani S (2009) Induced astigmatism with 2.2- and 3.0-mm coaxial phacoemulsification incisions. J Refract Surg 25:21–24. https://doi.org/10.3928/1081597X-20090101-04
Wang J, Zhang EK, Fan WY, Ma JX, Zhao PF (2009) The effect of micro-incision and small-incision coaxial phaco-emulsification on corneal astigmatism. Clin Exp Ophthalmol 37:664–669. https://doi.org/10.1111/j.1442-9071.2009.02117.x
Bergren RL (1994) Four-point fixation technique for sutured posterior chamber intraocular lenses. Arch Ophthalmol 112:1485–1487. https://doi.org/10.1001/archopht.1994.01090230099029
Pollmann AS, Lewis DR, Gupta RR (2020) Structural integrity of intraocular lenses with eyelets in a model of transscleral fixation with the Gore-Tex suture. J Cataract Refract Surg 46:617–621. https://doi.org/10.1097/j.jcrs.0000000000000129
Zhao H, Wang W, Hu Z, Chen B (2019) Long-term outcome of scleral-fixated intraocular lens implantation without conjunctival peritomies and sclerotomy in ocular trauma patients. BMC Ophthalmol 19:164. https://doi.org/10.1186/s12886-019-1172-4
Matsumura T, Takamura Y, Makita J, Kobori A, Inatani M (2019) Influence of sclerotomy size on intraocular lens tilt after intrascleral intraocular lens fixation. J Cataract Refract Surg 45:1446–1451. https://doi.org/10.1016/j.jcrs.2019.06.006
Gupta RR, Seamone ME, Pollmann AS, O’Brien DM, Lewis DR (2019) Dislocation of a scleral-fixated, hydrophobic, single-piece acrylic intraocular lens secondary to eyelet fracture from Gore-Tex suture. J VitreoRetinal Dis 3:395–398. https://doi.org/10.1177/2474126419857207
Chen KJ, Sun CC, Sun MH (2019) Unilateral triangular eyelet disruption of scleral-fixed enVista lens. Ophthalmol Retina 3:680. https://doi.org/10.1016/j.oret.2019.04.020
Lippincott JTB (2019) Three cases of scleral sutured enVista intraocular lens dislocation and determination of the enVista eyelet tensile strength under two different suturing methods. Invest Ophthalmol Vis Sci 60:485
Gregori NZ, Echegaray JJ, Flynn HW Jr (2019) Opacification of Akreos hydrophilic acrylic lens after retinal detachment repair with silicone oil tamponade: a case report. Ophthalmol Ther 8:341–345. https://doi.org/10.1007/s40123-019-0183-9
Shakibai N, Chavala SH (2020) Delayed capsular bag akreos IOL opacification after vitrectomy and gas tamponade. Am J Ophthalmol Case Rep 18:100676. https://doi.org/10.1016/j.ajoc.2020.100676
Chu CJ, Johnston RL, Buscombe C, Sallam AB, Mohamed Q, Yang YC, United Kingdom Pseudophakic Macular Edema Study G (2016) Risk factors and incidence of macular edema after cataract surgery: a database study of 81984 eyes. Ophthalmology 123:316–323. https://doi.org/10.1016/j.ophtha.2015.10.001
Baino F (2010) Scleral buckling biomaterials and implants for retinal detachment surgery. Med Eng Phys 32:945–956. https://doi.org/10.1016/j.medengphy.2010.07.007
Ni S, Wang W, Chen X, Wu X, He S, Ma Y, Xu W (2019) Clinical observation of a novel technique: transscleral suture fixation of a foldable 3-looped haptics one-piece posterior chamber intraocular lens implantation through scleral pockets with intact conjunctiva. BMC Ophthalmol 19:105. https://doi.org/10.1186/s12886-019-1113-2
Hirnschall N, Buehren T, Bajramovic F, Trost M, Teuber T, Findl O (2017) Prediction of postoperative intraocular lens tilt using swept-source optical coherence tomography. J Cataract Refract Surg 43:732–736. https://doi.org/10.1016/j.jcrs.2017.01.026
Weikert MP, Golla A, Wang L (2018) Astigmatism induced by intraocular lens tilt evaluated via ray tracing. J Cataract Refract Surg 44:745–749. https://doi.org/10.1016/j.jcrs.2018.04.035
Marcos S (2011) Special circumstances: effect of IOL tilt on astigmatism. In: Hoffer KJ (ed) IOL power. Thorofare, Slack, pp 223–230
Author information
Authors and Affiliations
Contributions
Study conception and design: C-YT, T-TL. Data acquisition: C-WH, C-YT, T-TL. Analysis and interpretation of data: C-WH, C-YT, T-TL. Drafting or revising the article: C-WH, C-YT, T-TL. Final approval: C-WH, C-YT, T-TL. Overall responsibility: T-TL.
Corresponding author
Ethics declarations
Ethics approval
The study adhered to the tenets of the Declaration of Helsinki and was approved by the National Taiwan University Hospital Research Ethics Committee.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 88903 KB)
Rights and permissions
About this article
Cite this article
Huang, CW., Tsai, CY. & Lai, TT. Short-term outcomes of a modified technique for small-incision scleral-fixated intraocular lens implantation using Gore-Tex sutures. Graefes Arch Clin Exp Ophthalmol 259, 1889–1896 (2021). https://doi.org/10.1007/s00417-021-05201-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-021-05201-4