Abstract
Purpose
To examine the predictability of exophthalmos reduction using preoperative computed tomography (CT) in deep lateral orbital wall decompression for Graves’ orbitopathy.
Methods
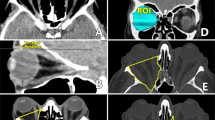
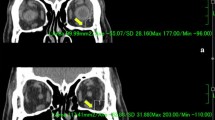
This was a retrospective, observational, case-control study conducted at a single institution. Forty-three patients (43 orbits) who were treated with deep lateral decompression with (27 patients) and without (16 patients) fat removal. Multivariate linear regression analyses were used to identify factors influencing exophthalmos reduction 3 months postoperatively. Variables investigated included age; smoking history; history of corticosteroid therapy and/or radiotherapy; preoperative diplopia; width, depth, and height of the greater wing of the sphenoid bone (trigone); and volume of fat removed. The influence of these parameters on the area of the orbital opening was also analyzed.
Results
Trigone width and amount of fat removed were positively correlated with exophthalmos reduction (both, P < .050); none of the other variables exhibited significant correlations. The predictive equation for postoperative reduction in Hertel exophthalmometric values was 0.57 + 0.15 × trigone width (mm) + 1.1 × fat removed (cm3). Depth and height were positively correlated (both, P < .050) and width was negatively correlated (P = .0045) with orbital opening area.
Conclusions
Trigone width and amount of fat removed were positive predictors of exophthalmos reduction after deep lateral decompression. Trigone width was inversely associated with orbital width, and results showed that larger exophthalmos reductions could be achieved in narrower orbits. This CT-based prediction method will assist preoperative decision-making regarding additional fat removal and/or removal of another orbital wall.




Similar content being viewed by others
References
Goldberg RA (1998) The evolving paradigm of orbital decompression surgery. Arch Ophthalmol 116:95–96
Goldberg RA, Perry JD, Hortaleza V, Tong JT (2000) Strabismus after balanced medial plus lateral wall versus lateral wall only orbital decompression for dysthyroid orbitopathy. Ophthal Plast Reconstr Surg 16:271–277
Ben Simon GJ, Syed HM, Lee S, Wang DY, Schwarcz RM, McCann JD, Goldberg RA (2006) Strabismus after deep lateral wall orbital decompression in thyroid-related orbitopathy patients using automated Hess screen. Ophthalmology 113:1050–1055
Shepard KG, Levin PS, Terris DJ (1998) Balanced orbital decompression for Graves’ ophthalmopathy. Laryngoscope 108:1648–1653
Mourits MP, Koornneef L, Wiersinga WM, Prummel MF, Berghout A, van der Gaag R (1990) Orbital decompression for Graves’ ophthalmopathy by inferomedial, by inferomedial plus lateral, and by coronal approach. Ophthalmology 97:636–641
Kikkawa DO, Pornpanich K, Cruz RC Jr, Levi L, Granet DB (2002) Graded orbital decompression based on severity of proptosis. Ophthalmology 109:1219–1224
Goldberg RA, Kim AJ, Kerivan KM (1998) The lacrimal keyhole, orbital door jamb, and basin of the inferior orbital fissure. Three areas of deep bone in the lateral orbit. Arch Ophthalmol 116:1618–1624
Lefebvre DR, Yoon MK (2015) CT-based measurements of the sphenoid trigone in different sex and race. Ophthal Plast Reconstr Surg 31:155–158
Wilson WB, Manke WF (1991) Orbital decompression in Graves’ disease. The predictability of reduction of proptosis. Arch Ophthalmol 109:343–345
Kamer L, Noser H, Schramm A, Hammer B, Kirsch E (2010) Anatomy-based surgical concepts for individualized orbital decompression surgery in Graves orbitopathy. I. Orbital size and geometry. Ophthal Plast Reconstr Surg 26:348–352
Nishimura K, Takahashi Y, Katahira N, Uchida Y, Ueda H, Ogawa T (2019) Visual changes after transnasal endoscopic versus transcaruncular medial orbital wall decompression for dysthyroid optic neuropathy. Auris Nasus Larynx 46:876-881
Berke RN (1953) A modified Krönlein operation. Trans Am Ophthalmol Soc 51:193–231
Sivak-Callcott JA, Linberg JV, Patel S (2005) Ultrasonic bone removal with the Sonopet Omni: a new instrument for orbital and lacrimal surgery. Arch Ophthalmol 123:1595–1597
Takahashi Y, Kakizaki H (2014) Horizontal eye position in thyroid eye disease: a retrospective comparison with normal individuals and changes after orbital decompression surgery. PLoS One 9:e114220
Takahashi Y, Miyazaki H, Ichinose A, Nakano T, Asamoto K, Kakizaki H (2013) Anatomy of deep lateral and medial orbital walls: implications in orbital decompression surgery. Orbit 32:409–412
Takahashi Y, Kitaguchi Y, Sabundayo MS, Kakizaki H (2018) Orbital fat volume in the inferolateral quadrant in Japanese: a guide for orbital fat decompression without injury to the oculomotor nerve. Int Ophthalmol 38:2471–2475
Kim KW, Byun JS, Lee JK (2014) Surgical effects of various orbital decompression methods in thyroid-associated orbitopathy: computed tomography-based comparative analysis. J Craniomaxillofac Surg 42:1286–1291
Wu CH, Chang TC, Liao SL (2008) Results and predictability of fat-removal orbital decompression for disfiguring graves exophthalmos in an Asian patient population. Am J Ophthalmol 145:755–759
Leone CR Jr, Piest KL, Newman RJ (1989) Medial and lateral wall decompression for thyroid ophthalmopathy. Am J Ophthalmol 108:160–166
Ediriwickrema LS, Korn BS, Kikkawa DO (2018) Orbital decompression for thyroid-related orbitopathy during the quiescent phase. Ophthal Plast Reconstr Surg 34:S90–S97
Choi SU, Kim KW, Lee JK (2016) Surgical outcomes of balanced deep lateral and medial orbital wall decompression in Korean population: clinical and computed tomography-based analysis. Korean J Ophthalmol 30:85–91
Kakizaki H, Nakano T, Asamoto K, Iwaki M (2008) Posterior border of the deep lateral orbital wall—appearance, width, and distance from the orbital rim. Ophthal Plast Reconstr Surg 24:262–265
Beden U, Edizer M, Elmali M, Icten N, Gungor I, Sullu Y, Erkan D (2007) Surgical anatomy of the deep lateral orbital wall. Eur J Ophthalmol 17:281–286
Lee H, Lee Y, Ha S, Park M, Baek S (2011) Measurement of width and distance of the posterior border of the deep lateral orbital wall using computed tomography. J Craniomaxillofac Surg 39:606–609
Stabile JR, Trokel SM (1983) Increase in orbital volume obtained by decompression in dried skulls. Am J Ophthalmol 95:327–331
Chang EL, Piva AP (2008) Temporal fossa orbital decompression for treatment of disfiguring thyroid-related orbitopathy. Ophthalmology 115:1613–1619
Ben Simon GJ, Wang L, McCann JD, Goldberg RA (2004) Primary-gaze diplopia in patients with thyroid-related orbitopathy undergoing deep lateral orbital decompression with intraconal fat debulking: a retrospective analysis of treatment outcome. Thyroid 14:379–383
Liao SL, Shih MJ, Chang TC, Lin LL (2006) Transforniceal lateral deep bone decompression—a modified technique to prevent postoperative diplopia in patients with disfiguring exophthalmos due to dysthyroid orbitopathy. J Formos Med Assoc 105:611–616
Baldeschi L, Wakelkamp IM, Lindeboom R, Prummel MF, Wiersinga WM (2006) Early versus late orbital decompression in Graves’ orbitopathy: a retrospective study in 125 patients. Ophthalmology 113:874–878
Goldberg RA, Weinberg DA, Shorr N, Wirta D (1997) Maximal, three-wall, orbital decompression through a coronal approach. Ophthalmic Surg Lasers 28:832–843
Paridaens DA, Verhoeff K, Bouwens D, van Den Bosch (2000) Transconjunctival orbital decompression in Graves’ ophthalmopathy: lateral wall approach ab interno. Br J Ophthalmol 84:775–781
Mehta P, Durrani OM (2011) Outcome of deep lateral wall rim-sparing orbital decompression in thyroid-associated orbitopathy: a new technique and results of a case series. Orbit 30:265–268
Ramesh S, Nobori A, Wang Y, Rootman D, Goldberg RA (2019) Orbital expansion in cranial vault after minimally invasive extradural transorbital decompression for thyroid orbitopathy. Ophthal Plast Reconstr Surg 35:17–21
Lam AK, Lam CF, Leung WK, Hung PK (2009) Intra-observer and inter-observer variation of Hertel exophthalmometry. Ophthalmic Physiol Opt 29:472–476
Cole HP 3rd, Couvillion JT, Fink AJ, Haik BG, Kastl PR (1997) Exophthalmometry: a comparative study of the Naugle and Hertel instruments. Ophthal Plast Reconstr Surg 13:189–194
Acknowledgments
The authors wish to acknowledge Dr. Makoto Ito at Department of Radiology, Aichi Medical University, for assisting us in the interpretation of imaging studies. We also thank Editage (www.editage.jp) for English language editing.
Author information
Authors and Affiliations
Contributions
All authors qualify for authorship based on contributions to the conception and design (YK, YT), acquisition of data (YK), literature search (YK, YT), and analyses and interpretation of data (all authors). All authors contributed to drafting the article and revising it critically for important intellectual content and final approval of the version to be published.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Patient consent information and ethical approvals
This retrospective observational study was approved by the Institutional Review Board (IRB) of Aichi Medical University Hospital (application number 2016-H238) and adhered to the tenets of the Declaration of Helsinki and its amendments. The IRB granted a waiver of informed consent for this study on the basis of the ethical guidelines for medical and health research involving human subjects established by the Japanese Ministry of Education, Culture, Sports, Science, and Technology and the Ministry of Health, Labour, and Welfare. The waiver was granted because the study was a retrospective chart review, not an interventional study, and because it was difficult to obtain consent from patients who had been treated several years prior to the study. Nevertheless, at the request of the IRB, we published an outline of the study, which is available for public viewing on the Aichi Medical University Hospital website. This public posting also gave patients the opportunity to decline participation, although none of the patients did so. Personal identifiers were removed from all records prior to data analysis.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kitaguchi, Y., Takahashi, Y. & Kakizaki, H. Computed Tomography–Based Prediction of Exophthalmos Reduction After Deep Lateral Orbital Wall Decompression for Graves’ Orbitopathy. Graefes Arch Clin Exp Ophthalmol 257, 2759–2767 (2019). https://doi.org/10.1007/s00417-019-04500-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-019-04500-1