Abstract
Purpose
To evaluate whether and how preoperative visual acuity predicts visual acuity outcome after Descemet Membrane Endothelial Keratoplasty (DMEK).
Methods
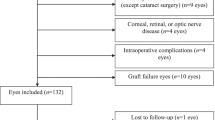
One thousand eighty-four out of 1162 consecutive eyes having undergone DMEK alone or combined with cataract surgery (triple-DMEK) between July 2011 and February 2016 from the prospective Cologne DMEK database were included and analyzed retrospectively for correlations between pre- and postoperative visual acuity values at 1, 3, 6, and 12 months after transplantation.
Results
There is a significant correlation between pre- and postoperative visual acuity (VA) after (triple)-DMEK after 6 and 12 months (p = 0.005 and p = 0.011 respectively; Pearson’s correlation coefficient 0.240 and 0.224). Preoperative VA below 20/100 leads to delayed and reduced final visual acuity results after 12 months (p < 0.001). However, defining an increase in VA > 0.1 logMAR as clinically relevant, we could not show any clinically relevant significant difference in the time needed to recover to final VA and in final VA. There is no significant difference for preoperative VA values above 20/40. The chance to reach postoperative VA above 20/25 is 40% for preoperative VA of 20/200, 50% for preoperative VA of 20/60 and > 60% for preoperative VA of 20/40.
Conclusion
DMEK results in very good final postoperative visual acuity results even in eyes with very poor preoperative vision caused by corneal pathology. However, preoperative visual acuity values below 20/100 result in significantly poorer visual recovery, which suggests that there is benefit in performing surgery early enough before this value is reached. Preoperative visual acuity seems to be an adjuvant tool for the prediction of the final visual outcome after DMEK.






Similar content being viewed by others
References
Melles GR, Ong TS, Ververs B, van der Wees J (2006) Descemet membrane endothelial keratoplasty (DMEK). Cornea 25:987–990. https://doi.org/10.1097/01.ico.0000248385.16896.34
Price MO, Price FW (2007) Descemet’s stripping endothelial keratoplasty. Curr Opin Ophthalmol 18:290–294. https://doi.org/10.1097/ICU.0b013e3281a4775b
Maier P, Reinhard T, Cursiefen C (2013) Descemet stripping endothelial keratoplasty--rapid recovery of visual acuity. Dtsch Arztebl Int 110:365–371. https://doi.org/10.3238/arztebl.2013.0365
Steven P, Hos D, Heindl LM, Bock F, Cursiefen C (2013) Immune reactions after DMEK, DSAEK and DALK. Klin Monatsbl Augenheilkd 230:494–499. https://doi.org/10.1055/s-0032-1328257
Anshu A, Price MO, Price FW Jr (2012) Risk of corneal transplant rejection significantly reduced with Descemet’s membrane endothelial keratoplasty. Ophthalmology 119:536–540. https://doi.org/10.1016/j.ophtha.2011.09.019
Dapena I, Ham L, Netukova M, van der Wees J, Melles GR (2011) Incidence of early allograft rejection after Descemet membrane endothelial keratoplasty. Cornea 30:1341–1345. https://doi.org/10.1097/ICO.0b013e31820d8540
Hamzaoglu EC, Straiko MD, Mayko ZM, Sales CS, Terry MA (2015) The first 100 eyes of standardized Descemet stripping automated endothelial Keratoplasty versus standardized Descemet Membrane Endothelial Keratoplasty. Ophthalmology 122:2193–2199. https://doi.org/10.1016/j.ophtha.2015.07.003
Hos D, Tuac O, Schaub F, Stanzel TP, Schrittenlocher S, Hellmich M, Bachmann BO, Cursiefen C (2017) Incidence and clinical course of immune reactions after Descemet Membrane Endothelial Keratoplasty: retrospective analysis of 1000 consecutive eyes. Ophthalmology 124:512–518. https://doi.org/10.1016/j.ophtha.2016.12.017
Wilson SE, Bourne WM (1988) Fuchs’ dystrophy. Cornea 7:2–18
Amin SR, Baratz KH, McLaren JW, Patel SV (2014) Corneal abnormalities early in the course of Fuchs’ endothelial dystrophy. Ophthalmology 121:2325–2333. https://doi.org/10.1016/j.ophtha.2014.07.001
Baratz KH, McLaren JW, Maguire LJ, Patel SV (2012) Corneal haze determined by confocal microscopy 2 years after Descemet stripping with endothelial keratoplasty for Fuchs corneal dystrophy. Arch Ophthalmol 130:868–874. https://doi.org/10.1001/archophthalmol.2012.73
Stanzel TP, Ersoy L, Sansanayudh W, Felsch M, Dietlein T, Bachmann B, Cursiefen C (2016) Immediate postoperative intraocular pressure changes after anterior chamber air fill in Descemet Membrane Endothelial Keratoplasty. Cornea 35:14–19. https://doi.org/10.1097/ICO.0000000000000669
Kruse FE, Laaser K, Cursiefen C, Heindl LM, Schlotzer-Schrehardt U, Riss S, Bachmann BO (2011) A stepwise approach to donor preparation and insertion increases safety and outcome of Descemet membrane endothelial keratoplasty. Cornea 30:580–587
Hoerster R, Stanzel TP, Bachmann BO, Siebelmann S, Felsch M, Cursiefen C (2016) Intensified topical steroids as prophylaxis for macular edema after posterior lamellar keratoplasty combined with cataract surgery. Am J Ophthalmol 163:174–179 e172. https://doi.org/10.1016/j.ajo.2015.12.008
Siebelmann S, Gehlsen U, Le Blanc C, Stanzel TP, Cursiefen C, Steven P (2016) Detection of graft detachments immediately following Descemet membrane endothelial keratoplasty (DMEK) comparing time domain and spectral domain OCT. Graefes Arch Clin Exp Ophthalmol. https://doi.org/10.1007/s00417-016-3484-x
Jonah Gabry BG (2016) rstanarm: Bayesian applied regression modeling via Stan. R package version 2.13.1. Stan Development Team. http://mc-stan.org/. Accessed 27 Aug 2018
Juho Piironen AV (2017) Comparison of Bayesian predictive methods for model selection. Stat Comput. https://doi.org/10.1007/s11222-016-9649-y
Markus Paasiniemi JP, Vehtari A, Gabry J (2018) Projection Predictive Feature Selection https://CRAN.R-project.org/package=projpred Accessed 27 Aug 2018
John Fox SW (2011) An {R} companion to applied regression. Sage, Thousand oaks CA
Fox JaM G (1992) Generalized collinearity diagnostics. JASA 87:178–183
McLaren JW, Wacker K, Kane KM, Patel SV (2016) Measuring corneal haze by using Scheimpflug photography and confocal microscopy. Invest Ophthalmol Vis Sci 57:227–235. https://doi.org/10.1167/iovs.15-17657
Wacker K, McLaren JW, Amin SR, Baratz KH, Patel SV (2015) Corneal high-order aberrations and backscatter in Fuchs’ endothelial corneal dystrophy. Ophthalmology 122:1645–1652. https://doi.org/10.1016/j.ophtha.2015.05.005
Ripandelli G, Scarinci F, Piaggi P, Guidi G, Pileri M, Cupo G, Sartini MS, Parisi V, Baldanzellu S, Giusti C, Nardi M, Stirpe M, Lazzeri S (2015) Macular pucker: to peel or not to peel the internal limiting membrane? A microperimetric response. Retina 35:498–507. https://doi.org/10.1097/IAE.0000000000000330
Grewing R, Mester U (1996) Results of surgery for epiretinal membranes and their recurrences. Br J Ophthalmol 80:323–326
Asaria R, Garnham L, Gregor ZJ, Sloper JJ (2008) A prospective study of binocular visual function before and after successful surgery to remove a unilateral epiretinal membrane. Ophthalmology 115:1930–1937. https://doi.org/10.1016/j.ophtha.2008.05.020
Falkner-Radler CI, Glittenberg C, Hagen S, Benesch T, Binder S (2010) Spectral-domain optical coherence tomography for monitoring epiretinal membrane surgery. Ophthalmology 117:798–805. https://doi.org/10.1016/j.ophtha.2009.08.034
Scheerlinck LM, van der Valk R, van Leeuwen R (2015) Predictive factors for postoperative visual acuity in idiopathic epiretinal membrane: a systematic review. Acta Ophthalmol 93:203–212. https://doi.org/10.1111/aos.12537
Kunikata H, Abe T, Kinukawa J, Nishida K (2011) Preoperative factors predictive of postoperative decimal visual acuity >/= 1.0 following surgical treatment for idiopathic epiretinal membrane. Clin Ophthalmol 5:147–154. https://doi.org/10.2147/OPTH.S15848
Inoue M, Morita S, Watanabe Y, Kaneko T, Yamane S, Kobayashi S, Arakawa A, Kadonosono K (2011) Preoperative inner segment/outer segment junction in spectral-domain optical coherence tomography as a prognostic factor in epiretinal membrane surgery. Retina 31:1366–1372. https://doi.org/10.1097/IAE.0b013e318203c156
Rice TA, De Bustros S, Michels RG, Thompson JT, Debanne SM, Rowland DY (1986) Prognostic factors in vitrectomy for epiretinal membranes of the macula. Ophthalmology 93:602–610
McDonald HR, Verre WP, Aaberg TM (1986) Surgical management of idiopathic epiretinal membranes. Ophthalmology 93:978–983
Marco Günther KV (2014) Mathematische Modellbildung und simulation. Wiley-VCH, Berlin
Acknowledgments
We would like to thank Ms. Jennifer Austin for the language correction of the manuscript.
Funding
This study is funded by DFG FOR 2240 (www.for2240.de) and EU ARREST BLINDNESS (www.arrestblindness.eu).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
ESM 1
(PDF 3947 kb)
Rights and permissions
About this article
Cite this article
Schrittenlocher, S., Bachmann, B., Tiurbe, A.M. et al. Impact of preoperative visual acuity on Descemet Membrane Endothelial Keratoplasty (DMEK) outcome. Graefes Arch Clin Exp Ophthalmol 257, 321–329 (2019). https://doi.org/10.1007/s00417-018-4193-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-018-4193-4