Abstract
Aim
We aimed to develop a score and validate it in a prospective cohort to identify the patients with ESUS at high risk for stroke recurrence.
Methods
We assessed the stroke recurrence in ESUS patients of the Third China National Stroke Registry. We performed multivariable logistic regression analysis to identify predictors of stroke recurrence in the derivation cohort. Based on the coefficient of each covariate of the fitted multivariable model, we generated an integer-based point scoring system. We validated the score in the validation cohort assessing its discrimination and calibration.
Results
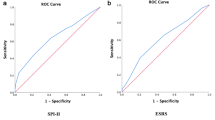
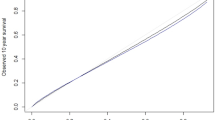
2415 patients were included: 1611 in the derivation and 804 in the validation sample. We developed a scoring system (0–15 points) by assigning 2 points for hypertension, 3 points for diabetes mellitus, 4 points for multiple stage infarction, 2 points for watershed involved infarction, 1 points for left atrial diameter index (per increasing 2.5 mm/m2) and 3 points for without statin at discharge. The rate of stroke recurrence was 5.9% per year (95% CI 4.2–7.6%) in patients with low risk(a score of 0–5), 9.4% (7.3–11.5%) in patients with intermediate risk (6–10), and 26.8% (16.5–37.1%) in patients with high risk (11–15). The AUC (area under curve of receiver operator characteristic curve) of the score in the derivation cohort and validation cohort was, respectively, 0.60 (0.55–0.65) and 0.63 (0.56–0.70). The score was well calibrated both in the derivation cohort (p = 0.36) and validation cohort (p = 0.26) with the Hosmer–Lemeshow test.
Conclusion
The developed score can improve risk stratification after ESUS in secondary care settings.


Similar content being viewed by others
Data availability statement
The datasets during and/or analyzed during the current study available from the corresponding author on reasonable request.
References
Hart RG, Catanese L, Perera KS, Ntaios G, Connolly SJ (2017) Embolic stroke of undetermined source: a systematic review and clinical update. Stroke 48(4):867–872
Perera KS, Vanassche T, Bosch J et al (2016) Embolic strokes of undetermined source: prevalence and patient features in the ESUS Global Registry. Int J Stroke 11:526–533
Yang X, Jing J, Meng X et al (2021) Characteristics and prognosis of patients with embolic stroke of undetermined source in China. Int J Stroke 17(5):526–535. https://doi.org/10.1177/17474930211028040
Diener HC, Sacco RL, Easton JD et al (2019) Dabigatran for prevention of stroke after embolic stroke of undetermined source. N Engl J Med 380:1906–1917
Hart RG, Sharma M, Mundl H et al (2018) Rivaroxaban for stroke prevention after embolic stroke of undetermined source. N Engl J Med 378:2191–2201
Ntaios G, Georgiopoulos G, Perlepe K et al (2019) A tool to identify patients with embolic stroke of undetermined source at high recurrence risk. Neurology 93:e2094–e2104
Hart RG, Veltkamp RC, Sheridan P et al (2019) Predictors of recurrent ischemic stroke in patients with embolic strokes of undetermined source and effects of rivaroxaban versus aspirin according to risk status: the NAVIGATE ESUS trial. J Stroke Cerebrovasc Dis 28:2273–2279
Kashima S, Shimizu T, Akiyama H, Hasegawa Y (2018) Magnetic resonance imaging white matter hyperintensity as a predictor of stroke recurrence in patients with embolic stroke of undetermined source. J Stroke Cerebrovasc Dis 27:3613–3620
de la Riva P, Zubikarai M, Sarasqueta C et al (2017) Nontraditional lipid variables predict recurrent brain ischemia in embolic stroke of undetermined source. J Stroke Cerebrovasc Dis 26:1670–1677
Choi KH, Kim JH, Kim JM et al (2021) d-dimer level as a predictor of recurrent stroke in patients with embolic stroke of undetermined source. Stroke. https://doi.org/10.1161/STROKEAHA120033217
Merkler AE, Pearce LA, Kasner SE et al (2021) Left ventricular dysfunction among patients with embolic stroke of undetermined source and the effect of rivaroxaban vs aspirin: a subgroup analysis of the NAVIGATE ESUS randomized clinical trial. JAMA Neurol 78:1454–1460
Gwak DS, Choi W, Kim YW, Kim YS, Hwang YH (2021) Impact of left atrial appendage morphology on recurrence in embolic stroke of undetermined source and atrial cardiopathy. Front Neurol 12:679320
Bhat A, Mahajan V, Chen HHL, Gan GCH, Pontes-Neto OM, Tan TC (2021) Embolic stroke of undetermined source: approaches in risk stratification for cardioembolism. Stroke 52:e820–e836
Wang Y, Jing J, Meng X et al (2019) The Third China National Stroke Registry (CNSR-III) for patients with acute ischaemic stroke or transient ischaemic attack: design, rationale and baseline patient characteristics. Stroke Vasc Neurol 4:158–164
Hart RG, Diener HC, Coutts SB et al (2014) Embolic strokes of undetermined source: the case for a new clinical construct. Lancet Neurol 13:429–438
Samuels OB, Joseph GJ, Lynn MJ, Smith HA, Chimowitz MI (2000) A standardized method for measuring intracranial arterial stenosis. AJNR Am J Neuroradiol 21:643–646
Fox AJ (1993) How to measure carotid stenosis. Radiology 186:316–318
Ay H, Gungor L, Arsava EM et al (2010) A score to predict early risk of recurrence after ischemic stroke. Neurology 74:128–135
Larsen BS, Kumarathurai P, Falkenberg J, Nielsen OW, Sajadieh A (2015) Excessive atrial ectopy and short atrial runs increase the risk of stroke beyond incident atrial fibrillation. J Am Coll Cardiol 66:232–241
Hu YM, Wu XL, Hu ZH et al (1999) Study of formula for calculating body surface areas of the Chinese adults. Sheng Li Xue Bao 51:45–48
Ntaios G, Lip GYH, Vemmos K et al (2017) Age- and sex-specific analysis of patients with embolic stroke of undetermined source. Neurology 89:532–539
Ntaios G, Vemmos K, Lip GY et al (2016) Risk stratification for recurrence and mortality in embolic stroke of undetermined source. Stroke 47:2278–2285
Sylaja PN, Coutts SB, Subramaniam S et al (2007) Acute ischemic lesions of varying ages predict risk of ischemic events in stroke/TIA patients. Neurology 68:415–419
Kauw F, Takx RAP, de Jong H, Velthuis BK, Kappelle LJ, Dankbaar JW (2018) Clinical and imaging predictors of recurrent ischemic stroke: a systematic review and meta-analysis. Cerebrovasc Dis 45:279–287
Weill C, Suissa L, Darcourt J, Mahagne MH (2017) The pathophysiology of watershed infarction: a three-dimensional time-of-flight magnetic resonance angiography study. J Stroke Cerebrovasc Dis 26:1966–1973
El-Gammal TM, Bahnasy WS, Ragab OAA, Al-Malt AM (2018) Cerebral border zone infarction: an etiological study. Egypt J Neurol Psychiatr Neurosurg 54:6
Jordan K, Yaghi S, Poppas A et al (2019) Left Atrial volume index is associated with cardioembolic stroke and atrial fibrillation detection after embolic stroke of undetermined source. Stroke 50:1997–2001
Wolf PA, Abbott RD, Kannel WB (1991) Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 22:983–988
Jalini S, Rajalingam R, Nisenbaum R, Javier AD, Woo A, Pikula A (2019) Atrial cardiopathy in patients with embolic strokes of unknown source and other stroke etiologies. Neurology 92:e288–e294
Kamel H, Longstreth WT Jr, Tirschwell DL et al (2018) The AtRial cardiopathy and antithrombotic drugs in prevention after cryptogenic stroke randomized trial: rationale and methods. Int J Stroke. https://doi.org/10.1177/1747493018799981
Stone NJ, Robinson JG, Lichtenstein AH et al (2014) 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 129:S1-45
Funding
This work was supported by grants from the Capital’s Funds for Health Improvement and Research (2020-1-2041), Chinese Academy of Medical Sciences Innovation Fund for Medical Sciences (2019-I2M-5-029), National Natural Science Foundation of China (81870905, U20A20358), and grants from National Natural Science Foundation of China (No. 82001237).
Author information
Authors and Affiliations
Contributions
Study concept and design: YJW; Drafting of the manuscript: JJ and XMY; Acquisition of data: XM, ZXL and YYW; Analysis and interpretation of data: YSP, YJ and AMJ; Study supervision: LPL, XQZ, YLW and HL. All authors approved the final version of this work.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the by the Ethics Committee at Beijing Tiantan Hospital (IRB approval number: KY2015-001-01) and all participating centers.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Informed consent included agreement to the publication of study findings.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jing, J., Yang, X., Wu, Y. et al. A score to predict the stroke recurrence of patients with embolic stroke of undetermined source. J Neurol 269, 6428–6435 (2022). https://doi.org/10.1007/s00415-022-11277-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11277-7