Abstract
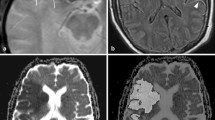
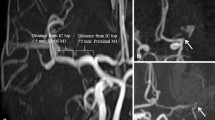
A rapid and complete recanalization of the occluded artery is the ideal goal when intravenous (IV) recombinant tissue plasminogen activator (rt-PA) is administrated to patients with acute ischemic stroke, i.e., limiting the ongoing ischemia to achieve a better outcome. We explored the effect of complete versus partial recanalization of the occluded intracranial artery after IV thrombolysis on the infarct growth and evaluated the functional impact. Using diffusion-weighted (DWI) volumetric measurements before rt-PA administration (DWI1) and 24 h later (DWI2), we calculated the infarct growth in 36 consecutive patients with ischemic stroke treated with IV rt-PA, with the formula DWI2/DWI1. Recanalization of the affected artery was assessed by transcranial Doppler (TCD) and magnetic resonance angiography (MRA) within 24 h of stroke onset. Three patients were eliminated from the analysis; 33 patients were fully analyzed (men: n = 23; mean (SD) age: 72.4 ± 16 years; time from stroke onset to rt-PA: 179 ± 54 min; mean NIHSS score at admission: 17). Patients achieving full recanalization by TCD had a smaller infarct growth, compared to those who had a partial or persistent occlusion after thrombolysis: 1.86 versus 2.91 (P = 0.017). This difference was not significant using MRA criteria: 2.01 versus 2.69 (P = 0.193). In the regression analysis, complete recanalization by TCD was an independent predictor of infarct growth (P = 0.045). Thus, complete recanalization measured by TCD within 24 h of IV thrombolysis was independently associated with smaller infarct growth.


Similar content being viewed by others
References
Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, Marsh EE III (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24:35–41
Albers GW, Thijs VN, Wechsler L, Kemp S, Schlaug G, Skalabrin E, Bammer R, Kakuda W, Lansberg MG, Shuaib A, Coplin W, Hamilton S, Moseley M, Marks MP, DEFUSE investigators (2006) Magnetic resonance imaging profiles predict clinical response to early reperfusion: the diffusion and perfusion imaging evaluation for understanding stroke evolution (DEFUSE) study. Ann Neurol 60:508–517
Alexandrov AV, Grotta JC (2002) Arterial reocclusion in stroke patients treated with intravenous tissue plasminogeno activator. Neurology 59:862–867
Barber PA, Davis SM, Darby DG, Desmond PM, Gerraty RP, Yang Q, Jolley D, Donnan GA, Tres BM (1999) Absent middle cerebral artery flow predicts the presence and evolution of the ischemic penumbra. Neurology 52:1125–1132
Christoforidis GA, Mohammad Y, Kehagias D, Avutu B, Slivka AP (2005) Angiographic assessment of pial collaterals as a prognostic indicator following intra-arterial thrombolysis for acute ischemic stroke. AJNR Am J Neuroradiol 26:1789–1797
Delgado-Mederos R, Rovira A, Alvarez-Sabin J, Ribo M, Munuera J, Rubiera M (2007) Speed of tPA-induced clot lysis predicts DWI lesion evolution in acute stroke. Stroke 38:955–960
Demchuck AM, Burgin WS, Christou I, Felberg RA, Barber PA, Hill MD, Alexandrov AM (2001) Thrombolysis in brain ischemia (TIBI) transcranial Doppler flow grades predict clinical severity, early recovery, and mortality in patients treated with intravenous tissue plasminogen activator. Stroke 32:89–93
Gordon DL, Bendixen BH, Adams HP Jr, Clarke W, Kappelle LJ, Woolson RF, The TOAST Investigators (1993) Interphysician agreement in the diagnosis of subtypes of acute ischemic stroke: implications for clinical trials. Neurology 43:1021–1027
Hacke W, Kaste M, Fieschi C, Toni D, Lesaffre E, von Kummer R, Boysen G, Bluhmki E, Hoxter G, Mahagne MH, The European Cooperative Acute Stroke Study (ECASS) (1995) Intravenous thrombolysis with recombinant tissue plasminogen activator for acute hemispheric stroke. JAMA 274:1017–1025
Hacke W, Kaste M, Bluhmki E, Brozman M, Dávalos A, Guidetti D, Larrue V, Lees KR, Medeghri Z, Machnig T, Schneider D, von Kummer R, Wahlgren N, Toni D, ECASS Investigators (2008) Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med 359:1317–1329
Kimura K, Iguchi Y, Shibazaki K, Aoki J, Uemura J (2009) Early recanalization rate of major occluded brain arteries after intravenous tissue plasminogen activator therapy using serial magnetic resonance angiography studies. Eur Neurol 62:287–292
Kimura K, Iguchi Y, Yamashita S, Shibazaki K, Kobayashi K, Inoue T (2008) Atrial fibrillation as an independent predictor for no early recanalization after IV t-PA in acute ischemic stroke. J Neurol Sci 267:57–61
Lee KY, Latour LL, Luby M, Hsia AW, Merino JG, Phil M, Warach S (2009) Distal hyperintense vessels on FLAIR. An MRI marker for collateral circulation in acute stroke? Neurology 72:1134–1139
Martinez-Sanchez P, Serena J, Alexandrov AV, Fuentes B, Fernandez-Dominguez J, Diez-Tejedor E (2009) Update on ultrasound techniques for the diagnosis of cerebral ischemia. Cerebrovasc Dis 27(Suppl 1):9–18
Navarro JC, Lao AY, Sharma VK, Tsivgoulis G, Alexandrov AV (2007) The accuracy of transcranial Doppler in the diagnosis of middle cerebral artery stenosis. Cerebrovasc Dis 23:325–330
Neumann-Haefelin T, du mesnil de Rochemont R, Fiebach JB, Gass A, Nolte C, Kucinski T, Rother J, Siebler M, Singer OC, Szabo K, Villringer A, Schellinger PD, Kompetenznetz Schlaganfall Study Group (2004) Effect of incomplete (spontaneous and postthrombolytic) recanalization after middle cerebral artery occlusion: a magnetic resonance imaging study. Stroke 35:109–114
Pantano P, Toni D, Caramia F, Falcou A, Fiorelli M, Argentino C, Fantozzi LM, Bozzao L (2001) Relationship between vascular enhancement, cerebral hemodynamics, and MR angiography in cases of acute stroke. AJNR Am J Neuroradiol 22:255–260
Ribo M, Molina CA, Delgado P, Rubiera M, Delgado-Mederos R, Rovira A, Munuera J, Alvarez Sabin J (2007) Hyperglycemia during ischemia rapidly accelerates brain damage in stroke patients treated with tPA. J Cereb Blood Flow Metab 27:1616–1622
Rosso C, Hevia-Montiel N, Deltour S, Bardinet E, Dormont D, Crozier S, Baillet S, Samson Y (2009) Prediction of infarct growth based on apparent diffusion coefficients: penumbral assessment without intravenous contrast material. Radiology 250:184–192
Rubiera M, Ribo M, Delgado-Mederos R, Santamarina E, Delgado P, Montaner J, Alvarez Sabin J, Molina C (2006) Tandem internal carotid artery/middle cerebral artery occlusion: an independent predictor of poor outcome after systemic thrombolysis. Stroke 37:2301–2305
Saqqur M, Uchino K, Demchuck AM, Molina CA, Garami Z, Calleja S, Akhtar N, Orouk FO, Salam A, Shuaib A, Alexandrov AV, for CLOTBUST Investigators (2007) Site of arterial occlusion identified by transcranial Doppler predicts the response to intravenous thrombolysis for stroke. Stroke 38:948–954
Shrier DA, Tanaka H, Numaguchi Y, Konno S, Patel U, Shibata D (1997) CT angiography in the evaluation of acute ischemic stroke. AJNR Am J Neuroradiol 18:1011–1020
Stolz E, Cioli F, Allendoerfer J, Gerriets T, Del Sette M, Kaps M (2008) Can early neurosonology predict outcome in acute stroke? A meta-analysis of prognostic clinical effect sizes related to the vascular status. Stroke 39:3255–3261
Tsivgoulis G, Sharma VK, Lao AY, Malkoff MD, Alexandrov AV (2007) Validation of transcranial Doppler with computed tomography angiography in acute cerebral ischemia. Stroke 38:1245–1249
von Kummer R, Holle R, Rosin L, Forsting M, Hacke W (1995) Does arterial recanalization improve outcome in carotid territory stroke? Stroke 26:581–587
Zangerle A, Kiechl S, Spiegel M, Furtner M, Knoflach M, Werner P, Mair A, Wille G, Schmidauer C, Gautsch K, Gotwald T, Felber S, Powe W, Willeit J (2007) Recanalization after thrombolysis in stroke patients: predictors and prognostic implications. Neurology 68:39–44
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baizabal-Carvallo, J.F., Rosso, C., Alonso-Juarez, M. et al. The hemodynamic status within 24 h after intravenous thrombolysis predicts infarct growth in acute ischemic stroke. J Neurol 259, 1045–1050 (2012). https://doi.org/10.1007/s00415-011-6295-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-011-6295-3