Abstract
Purpose
Different mutations in coding and non-coding sequences of the SERPINA1 gene have been implicated in the pathogenesis of COPD. However, − 10T/C mutation in the hepatocyte-directed promoter region has not been associated with COPD pathogenesis so far. Here, we report an increased frequency of − 10C genotype that is associated with decreased levels of serum alpha1-antitrypsin (α1AT) in COPD patients.
Methods
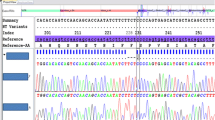
The quantification of serum α1AT was done by ELISA, the phenol–chloroform method was used for DNA extraction, PCR products were directly sequenced. The IBM SPSS Statistics v21 software was used for statistical analyses of the data.
Results
The mean serum α1AT level was found to be 1.203+0.239 and 3.162+0.160 g/L in COPD cases and in control, respectively. The − 10C allele is associated with an increased risk of COPD [OR, 3.50 (95%CI, 1.86-6.58); p < 0.001]. The combined variant genotype (TT+CC) was significantly found associated with an increased risk of COPD [OR, 3.20 (95% CI, 1.47-6.96); p = 0.003]. A significant association of the family history with COPD (overall p value= 0.0331) suggests that genetics may play an important role in the pathogenesis of COPD.
Conclusion
The polymorphism associated with hepatocyte-specific promoter region (− 10T/C) is likely to be associated with the pathogenesis of COPD. It is quite possible that the change of the base in the hepatocyte-specific promoter of the SERPINA1 gene can modulate its strength, thereby driving the reduced expression of α1AT.





Similar content being viewed by others

References
Celli BR, MacNee W (2004) Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS/ERS position paper. Eur Respir J 23(6):932–946
Thornton Snider J, Romley JA, Wong KS, Zhang J, Eber M, Goldman DP (2012) The disability burden of COPD. Copd 9(5):513–521. https://doi.org/10.3109/15412555.2012.696159
Minino AM, Xu J, Kochanek KD (2010) Deaths: preliminary data for 2008. Natl Vital Stat Rep 59(2):1–52
Burney P, Jithoo A, Kato B, Janson C, Mannino D, Nizankowska-Mogilnicka E et al. (2014) Chronic obstructive pulmonary disease mortality and prevalence: the associations with smoking and poverty–a BOLD analysis. Thorax 69(5):465–473. https://doi.org/10.1136/thoraxjnl-2013-204460
Lomas DA, Mahadeva R (2002) Alpha1-antitrypsin polymerization and the serpinopathies: pathobiology and prospects for therapy. J Clin Invest 110(11):1585–1590
Kelly E, Greene CM, Carroll TP, McElvaney NG, O’Neill SJ (2010) Alpha-1 antitrypsin deficiency. Respir Med 104(6):763–772. https://doi.org/10.1016/j.rmed.2010.01.016
Bashir A, Shah NN, Hazari YM, Habib M, Bashir S, Hilal N et al. (2016) Novel variants of SERPIN1A gene: interplay between alpha1-antitrypsin deficiency and chronic obstructive pulmonary disease. Respir Med 117:139–149. https://doi.org/10.1016/j.rmed.2016.06.005
Crystal RG (1990) Alpha 1-antitrypsin deficiency, emphysema, and liver disease. Genetic basis and strategies for therapy. J Clin Invest 85(5):1343–1352
Hazari YM, Bashir A, Habib M, Bashir S, Habib H, Qasim MA et al. (2017) Alpha-1-antitrypsin deficiency: Genetic variations, clinical manifestations and therapeutic interventions. Mutat Res2017 Jul;773:14–25. https://doi.org/10.1016/j.mrrev.2017.03.001
Stoller JK, Aboussouan LS (2005) Alpha1-antitrypsin deficiency. Lancet 365(9478):2225–2236
Hazari Y, Habib M, Bashir S, Bashir A, Hilal N, Irfan S et al. (2016) Natural osmolytes alleviate GRP78 and ATF-4 levels: corroboration for potential modulators of unfolded protein response. Life Sci 146:148–53
Gupta J, Bhadoria DP, Lal MK, Kukreti R, Chattopadhaya D, Gupta VK et al (2005) Association of the PIM3 allele of the alpha-1-antitrypsin gene with chronic obstructive pulmonary disease. Clin Biochem 38(5):489–491
Acknowledgements
The financial support provided by grants from the Department of Biotechnology (DBT), New Delhi to Khalid Majid Fazili and Arif Bashir (No. BT/PR7240/MED/30/915/2012) is acknowledged. We would also like to acknowledge the financial support provided bygrants from the Department of Science and Technology (No. SB/SO/ AS-126/2012), FIST (No. SR/FST/LSI-384/2008), SAP and UGC (No. F.3–26/2011(SAP-II)) and the facilities extended by University of Kashmir, Srinagar-190006, India. The authors would also like to thank all the COPD patients and control subjects who took part in this study and cooperated during the interview and sample collection. We also acknowledge the support and cooperation from the technical staff of the Government Chest Disease Hospital, Srinagar, Jammu and Kashmir-India.
Author information
Authors and Affiliations
Contributions
All authors have made substantial contributions: (1) The concept and design of the study was done by AB, YMH, KMF, and NNS (2) the article was drafted critically for important intellectual content by Dr. KMF, Dr. NNS and AB (3) Dr. MKI, NH, MB, SB and MB prepared reagents for DNA extraction, (4) Statistical analysis was done by Dr. TRJ, and (5) Pulmonary function assistance by SSF and (6) final approval of the version by KMF, NNS, and AB.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declared that they have no competing interests.
Ethical Approval
This study is approved by the Ethics Committee of the Government Medical College Srinagar-India.
Rights and permissions
About this article
Cite this article
Bashir, A., Hazari, Y.M., Bashir, S. et al. SERPINA1 Hepatocyte-Specific Promoter Polymorphism Associate with Chronic Obstructive Pulmonary Disease in a Study of Kashmiri Ancestry Individuals. Lung 196, 447–454 (2018). https://doi.org/10.1007/s00408-018-0124-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-018-0124-8