Abstract
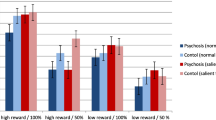
Negative symptoms in the motivational domain are strongly correlated with deficits in social and occupational functioning in schizophrenia. However, the neural substrates underlying these symptoms remain largely unknown. Twenty-eight adults with schizophrenia and twenty healthy volunteers underwent functional magnetic resonance while completing a lottery game designed to capture reward-related cognitive processes. Each trial demanded an initial investment of effort in form of key presses to increase the odds of winning. Brain activity in response to different reward cues (1 euro versus 1 cent) was compared between groups. Whereas controls invested more effort in improving their chances to win 1 euro compared to 1 cent in the lottery game, patients invested similarly high amounts of effort in both reward conditions. The neuroimaging analysis revealed lower neural activity in the bilateral caudate and cingulo-opercular circuits and decreased effective connectivity between reward-associated areas and neural nodes in the frontoparietal and salience network in response to high- versus low-reward conditions in schizophrenia patients compared to controls. Effective connectivity differences across conditions were associated with amotivation symptoms in patients. Overall, our data provide the evidence of alterations in neural activity in the caudate and cingulo-opercular “task maintenance” circuits and frontoparietal effective connectivity with reward-associated nodes as possible underlying mechanisms of reward value discrimination deficits affecting effort computation in schizophrenia.




Similar content being viewed by others
References
Blanchard JJ, Cohen AS (2006) The structure of negative symptoms within schizophrenia: Implications for assessment. Schizophr Bull 32(2):238–245
Kirkpatrick B, Fenton WS, Carpenter WT, Marder SR (2006) The NIMH-MATRICS consensus statement on negative symptoms. Schizophr Bull 32:214–219. https://doi.org/10.1093/schbul/sbj053
Fervaha G, Graff-Guerrero A, Zakzanis KK et al (2013) Incentive motivation deficits in schizophrenia reflect effort computation impairments during cost–benefit decision-making. J Psychiatr Res 47:1590–1596. https://doi.org/10.1016/j.jpsychires.2013.08.003
Foussias G, Remington G (2010) Negative symptoms in schizophrenia: avolition and Occam’s razor. Schizophr Bull 36:359–369. https://doi.org/10.1093/schbul/sbn094
Marwaha S, Johnson S (2004) Schizophrenia and employment. Soc Psychiatry Psychiatr Epidemiol 39:337–349. https://doi.org/10.1007/s00127-004-0762-4
Saha S, Chant D, Welham J, McGrath J (2005) A systematic review of the prevalence of schizophrenia. PLoS Med 2:e141. https://doi.org/10.1371/journal.pmed.0020141
Strauss GP, Waltz JA, Gold JM (2014) A review of reward processing and motivational impairment in schizophrenia. Schizophr Bull 40:S107–S116. https://doi.org/10.1093/schbul/sbt197
Gold JM, Strauss GP, Waltz JA et al (2013) Negative symptoms of schizophrenia are associated with abnormal effort–cost computations. Biol Psychiatry 74:130–136. https://doi.org/10.1016/j.biopsych.2012.12.022
Gold JM, Waltz JA, Prentice KJ et al (2008) Reward processing in schizophrenia: a deficit in the representation of value. Schizophr Bull 34:835–847. https://doi.org/10.1093/schbul/sbn068
Jones C, Hacker D, Cormac I et al (2012) Cognitive behavioural therapy versus other psychosocial treatments for schizophrenia. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD008712.pub2
Kring AM, Barch DM (2014) The motivation and pleasure dimension of negative symptoms: Neural substrates and behavioral outputs. Eur Neuropsychopharmacol 24:725–736. https://doi.org/10.1016/j.euroneuro.2013.06.007
Gold JM, Waltz JA, Matveeva TM et al (2012) Negative symptoms and the failure to represent the expected reward value of actions: behavioral and computational modeling evidence. Arch Gen Psychiatry 69:129–138. https://doi.org/10.1001/archgenpsychiatry.2011.1269
Heerey EA, Bell-Warren KR, Gold JM (2008) Decision-making impairments in the context of intact reward sensitivity in schizophrenia. Biol Psychiatry 64:62–69. https://doi.org/10.1016/j.biopsych.2008.02.015
Barch DM, Treadway MT, Schoen N (2014) Effort, anhedonia, and function in schizophrenia: Reduced effort allocation predicts amotivation and functional impairment. J Abnorm Psychol 123:387–397. https://doi.org/10.1037/a0036299
Wolf DH, Satterthwaite TD, Kantrowitz JJ et al (2014) Amotivation in schizophrenia: integrated assessment with behavioral, clinical, and imaging measures. Schizophr Bull 40:1328–1337. https://doi.org/10.1093/schbul/sbu026
Bergé D, Pretus C, Guell X et al (2018) Reduced willingness to invest effort in schizophrenia with high negative symptoms regardless of reward stimulus presentation and reward value. Compr Psychiatry 87:153–160. https://doi.org/10.1016/j.comppsych.2018.10.010
Brown RG, Pluck G (2000) Negative symptoms: the “pathology” of motivation and goal-directed behaviour. Trends Neurosci 23:412–417
Rudebeck PH, Murray EA (2011) Dissociable effects of subtotal lesions within the macaque orbital prefrontal cortex on reward-guided behavior. J Neurosci 31:10569–10578. https://doi.org/10.1523/JNEUROSCI.0091-11.2011
Botvinick MM, Huffstetler S, McGuire JT (2009) Effort discounting in human nucleus accumbens. Cogn Affect Behav Neurosci 9:16–27. https://doi.org/10.3758/CABN.9.1.16
Kurniawan IT, Seymour B, Talmi D et al (2010) Choosing to make an effort: the role of striatum in signaling physical effort of a chosen action. J Neurophysiol 104:313–321. https://doi.org/10.1152/jn.00027.2010
Croxson PL, Walton ME, Reilly JXO et al (2009) Effort-based cost–benefit valuation and the human brain. J Neurosci 29:4531–4541. https://doi.org/10.1523/JNEUROSCI.4515-08.2009
Klein-Flugge MC, Kennerley SW, Friston K, Bestmann S (2016) Neural signatures of value comparison in human cingulate cortex during decisions requiring an effort-reward trade-off. J Neurosci 36:10002–10015. https://doi.org/10.1523/JNEUROSCI.0292-16.2016
Morris RW, Vercammen A, Lenroot R et al (2012) Disambiguating ventral striatum fMRI-related bold signal during reward prediction in schizophrenia. Mol Psychiatry 17:280–289. https://doi.org/10.1038/mp.2011.75
Nielsen MØ, Rostrup E, Wulff S et al (2012) Alterations of the brain reward system in antipsychotic naïve schizophrenia patients. Biol Psychiatry 71:898–905. https://doi.org/10.1016/J.BIOPSYCH.2012.02.007
Juckel G, Schlagenhauf F, Koslowski M et al (2006) Dysfunction of ventral striatal reward prediction in schizophrenia. Neuroimage 29:409–416. https://doi.org/10.1016/j.neuroimage.2005.07.051
Burrer A, Caravaggio F, Manoliu A et al (2020) Apathy is not associated with reduced ventral striatal volume in patients with schizophrenia. medRxiv. https://doi.org/10.1101/2020.02.07.20019943
Chung YS, Barch DM (2016) Frontal-Striatum dysfunction during reward processing: relationships to amotivation in schizophrenia. J Abnorm Psychol 125:1–17. https://doi.org/10.1037/abn0000137
Park IH, Chun JW, Park HJ et al (2015) Altered cingulo-striatal function underlies reward drive deficits in schizophrenia. Schizophr Res 161:229–236. https://doi.org/10.1016/j.schres.2014.11.005
Guessoum SB, Le Strat Y, Dubertret C, Mallet J (2020) A transnosographic approach of negative symptoms pathophysiology in schizophrenia and depressive disorders. Prog Neuro-Psychopharmacol Biol Psychiatry 99:109862
Segarra N, Metastasio A, Ziauddeen H et al (2016) Abnormal frontostriatal activity during unexpected reward receipt in depression and schizophrenia: relationship to anhedonia. Neuropsychopharmacology 41:2001–2010. https://doi.org/10.1038/npp.2015.370
Reckless GE, Andreassen OA, Server A et al (2015) Negative symptoms in schizophrenia are associated with aberrant striato-cortical connectivity in a rewarded perceptual decision-making task. Neuroimage Clin 8:290–297. https://doi.org/10.1016/j.nicl.2015.04.025
Xu P, Klaasen NG, Opmeer EM et al (2019) Intrinsic mesocorticolimbic connectivity is negatively associated with social amotivation in people with schizophrenia. Schizophr Res 208:353–359. https://doi.org/10.1016/j.schres.2019.01.023
Bergé D, Mané A, Salgado P et al (2016) Predictors of relapse and functioning in first-episode psychosis: a two-year follow-up study. Psychiatr Serv 67:227–233. https://doi.org/10.1176/appi.ps.201400316
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders (DSM-5), 5th edn. American Psychiatric Association, Washington, DC
Kirkpatrick B, Strauss GP, Nguyen L et al (2011) The brief negative symptom scale: psychometric properties. Schizophr Bull 37:300–305. https://doi.org/10.1093/schbul/sbq059
Jones SH, Thornicroft G, Coffey M, Dunn G (1995) A brief mental health outcome scale: reliability and validity of the global assessment of functioning (GAF). Br J Psychiatry 166:654–659. https://doi.org/10.1192/bjp.166.5.654
First MB, Spitzer RL, Gibbon M, Williams JBW (1997) Structured clinical interview for DSM-IV axis I disorders (SCID I). Biometric Research Department, New York
Sheehan DV, Lecrubier Y, Sheehan KH et al (1998) The mini-international neuropsychiatric interview (MINI): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 59(20):22–33 (quiz 34-57)
Kay SR, Fiszbein A, Opler LA (1987) The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr Bull 13:261–276
Kleiner M, Brainard D, Pelli D et al (2007) What’s new in psychtoolbox-3. Perception 36:1–16
Kapur S, Seeman P (2001) Does fast dissociation from the dopamine D2 receptor explain the action of atypical antipsychotics? A new hypothesis. Am J Psychiatry 158:360–369
Yarkoni T, Poldrack RA, Nichols TE et al (2011) NeuroSynth: a new platform for large-scale automated synthesis of human functional neuroimaging data. Front Neuroinform. https://doi.org/10.3389/conf.fninf.2011.08.00058
McLaren DG, Ries ML, Xu G, Johnson SC (2012) A generalized form of context-dependent psychophysiological interactions (gPPI): a comparison to standard approaches. Neuroimage 61:1277–1286. https://doi.org/10.1016/j.neuroimage.2012.03.068
Guitart-Masip M, Fuentemilla L, Bach DR et al (2011) Action dominates valence in anticipatory representations in the human striatum and dopaminergic midbrain. J Neurosci 31:7867–7875. https://doi.org/10.1523/JNEUROSCI.6376-10.2011
Grahn JA, Parkinson JA, Owen AM (2008) The cognitive functions of the caudate nucleus. Prog Neurobiol 86:141–155. https://doi.org/10.1016/j.pneurobio.2008.09.004
Delgado MR, Stenger VA, Fiez JA (2004) Motivation-dependent responses in the human caudate nucleus. Cereb Cortex 14:1022–1030. https://doi.org/10.1093/cercor/bhh062
Dosenbach NUF, Visscher KM, Palmer ED et al (2006) A core system for the implementation of task sets. Neuron 50:799–812. https://doi.org/10.1016/j.neuron.2006.04.031
Sadaghiani S, D’Esposito M (2015) Functional characterization of the cingulo-opercular network in the maintenance of tonic alertness. Cereb Cortex 25:2763–2773. https://doi.org/10.1093/cercor/bhu072
Shukla DK, Chiappelli JJ, Sampath H et al (2019) Aberrant frontostriatal connectivity in negative symptoms of schizophrenia. Schizophr Bull 45:1051–1059. https://doi.org/10.1093/schbul/sby165
Van Den Heuvel MP, Sporns O, Collin G et al (2013) Abnormal rich club organization and functional brain dynamics in schizophrenia. JAMA Psychiatry 70:783–792. https://doi.org/10.1001/jamapsychiatry.2013.1328
Zhou Y, Zeidman P, Wu S et al (2018) Altered intrinsic and extrinsic connectivity in schizophrenia. NeuroImage Clin 17:704–716. https://doi.org/10.1016/j.nicl.2017.12.006
Van Den Heuvel MP, Fornito A (2014) Brain networks in schizophrenia. Neuropsychol Rev 24:32–48
Fornito A, Zalesky A, Pantelis C, Bullmore ET (2012) Schizophrenia, neuroimaging and connectomics. Neuroimage 62:2296–2314
Carpenter WT, Heinrichs DW, Alphs LD (1985) Treatment of negative symptoms. Schizophr Bull 11:440–452
Kirschner M, Aleman A, Kaiser S (2017) Secondary negative symptoms—a review of mechanisms, assessment and treatment. Schizophr Res 186:29–38
Fervaha G, Takeuchi H, Lee J et al (2015) Antipsychotics and amotivation. Neuropsychopharmacology 40:1539–1548. https://doi.org/10.1038/npp.2015.3
Acknowledgements
We would like to thank all the volunteers who kindly agreed to participate in this study. This work was supported by the Instituto de Salud Carlos III (ISCiii), Proyectos de Investigación y Salud, Grant reference PI18/00053.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
The study was approved by the Hospital del Mar Medical Research Institute Ethical Committee and was carried out in accordance with the Declaration of Helsinki. After a full explanation of the study, written informed consent was obtained from all participants before taking part in the study.
Additional information
Communicated by Sebastian Walther.
Rights and permissions
About this article
Cite this article
Pretus, C., Bergé, D., Guell, X. et al. Brain activity and connectivity differences in reward value discrimination during effort computation in schizophrenia. Eur Arch Psychiatry Clin Neurosci 271, 647–659 (2021). https://doi.org/10.1007/s00406-020-01145-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-020-01145-8