Abstract
Purpose
Postpartum depression is a common complication of childbirth. In the last decade, it has been suggested that subdissociative-dose ketamine is a fast-acting antidepressant. We aimed to investigate the efficacy of low-dose ketamine administered during caesarean section in preventing postpartum depression.
Methods
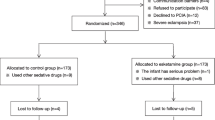
Using a randomized, double-blind, placebo-controlled design, 330 parturients who were scheduled to undergo caesarean section were enrolled in this trial. The parturients were randomly assigned to receive intravenous ketamine (0.25 mg/kg diluted to 10 mL with 0.9% saline) or placebo (10 mL of 0.9% saline) within 5 min following clamping of the neonatal umbilical cord. The primary outcome was the degree of depression, which was evaluated using the Edinburgh Postnatal Depression Scale (EPDS) (a threshold of 9/10 was used) at 3 days and 6 weeks after delivery. The secondary outcome was the numeric rating scale score of pain at 3 day and 6 week postpartum.
Results
No significant differences were found in the prevalence of postpartum depression between the two groups at 3 days and 6 weeks after delivery. The pain scores measured at 3 days postoperatively were not significantly different between the groups, whereas the scores measured at 6 week postpartum were significantly reduced in the treatment group compared with the saline group (P = 0.014).
Conclusions
Intra-operative low-dose ketamine (0.25 mg/kg) does not have a preventive effect on postpartum depression.

Similar content being viewed by others
References
Gaynes BN, Gavin N, Meltzer-Brody S, Lohr KN, Swinson T, Gartlehner G, Brody S, Miller WC (2005) Perinatal Depression: Prevalence, Screening Accuracy, and Screening Outcomes. Evid Rep Technol Assess (summ) (119):1–8.
Qian YR, Yan XY (2013) Prevalence of postpartum depression in China: a systematic analysis. Chin J Prac Nurs 29:1–3.
Lindahl V, Pearson JL, Colpe L (2005) Prevalence of suicidality during pregnancy and the postpartum. Arch Womens Ment Health 8:77–87
Beck CT (1995) The effects of postpartum depression on maternal-infant interaction: A meta-analysis. Nurs Res 44:298–304
Stein A, Pearson RM, Goodman SH, Rapa E, Rahman A, McCallum M, Howard LM, Pariante CM (2014) Effects of perinatal mental disorders on the fetus and child. The Lancet 84:1800–1819. doi:10.1016/S0140-6736(14)61277-0
Letourneau NL, Dennis CL, Benzies K, Duffett-Leger L, Stewart M, Tryphonopoulos PD, Este D, Watson W (2012) Postpartum depression is a family affair: addressing the impact on mothers, fathers, and children. Issues Ment Health Nurs 33:445–457. doi:10.3109/01612840.2012.673054
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders, 5th edn. American Psychiatric Association, Arlington, VA
Kishimoto T, Chawla JM, Hagi K, Zarate CA, Kane JM, Bauer M, Correll CU (2016) Single-dose infusion ketamine and non-ketamine N-methyl-D-aspartate receptor antagonists for unipolar and bipolar depression: a meta-analysis of efficacy, safety and time trajectories. Psychol Med 46:1459–1472. doi:10.1017/S0033291716000064
Clements JA, Nimmo WS, Grant IS (1982) Bioavailability, pharmacokinetics, and analgesic activity of ketamine in humans. J Pharm Sci 71:539–542
Monteggia LM, Zarate C Jr (2015) Antidepressant actions of ketamine: from molecular mechanisms to clinical practice. Curr Opin Neurobiol 30:139–143. doi:10.1016/j.conb.2014.12.004
Ding T, Wang DX, Qu Y, Chen Q, Zhu SN (2014) Epidural Labor Analgesia Is Associated with a Decreased Risk of Postpartum Depression. Anesth Analg 119:383–392. doi:10.1213/ANE.0000000000000107
Eisenach JC, Pan PH, Smiley R, Lavand’homme P, Landau R, Houle TT (2008) Severity of acute pain after childbirth, but not type of delivery, predicts persistent pain and postpartum depression. Pain 140:87–94. doi:10.1016/j.pain.2008.07.011
Gaudet C, Wen SW, Walker MC (2013) Chronic perinatal pain as a risk factor for postpartum depression symptoms in Canadian women. Can J Public Health 104:e375–e387
Bell RF, Dahl JB, Moore RA, Kalso E (2006) Perioperative ketamine for acute postoperative pain. Cochrane Database Syst Rev 25:CD004603
Chaparro LE, Smith SA, Moore RA, Wiffen PJ, Gilron I (2013) Pharmacotherapy for the prevention of chronic pain after surgery in adults. Cochrane Database Syst Rev 24:CD008307. doi:10.1002/14651858
Hirota K, Lambert DG (2011) Ketamine: new uses for an old drug? Br J Anaesth 107:123–126. doi:10.1093/bja/aer221
Stubhaug A, Breivik H, Eide PK, Kreunen M, Foss A (1997) Mapping of punctuate hyperalgesia around a surgical incision demonstrates that ketamine is a powerful suppressor of central sensitization to pain following surgery. Acta Anaesthesiol Scand 41:1124–1132
Cox JL, Holden JM, Sagovsky R (1987) Detection of Postnatal Depression. Development of the 10-item Edinburgh Postnatal Depression Scale. Br J Psychiatry 150:782–786
Lee DT, Yip SK, Chiu HF, Leung TY, Chan KP, Chan IO, Leung HC, Chung TK (1998) Detecting postnatal depression in Chinese women: validation of the Chinese version of the Edinburgh Postnatal Depression Scale. Br J Psychiatry 172:433–437
Murrough JW, Iosifescu DV, Chang LC, Al Jurdi RK, Green CE, Perez AM, Iqbal S, Pillemer S, Foulkes A, Shah A, Charney DS, Mathew SJ (2013) Antidepressant efficacy of ketamine in treat-resistant major depression: a two site randomized controlled trial. Am J Psychiatry 170:1134–1142. doi:10.1176/appi.ajp.2013.13030392
Wisner KL, Parry BL, Piontek CM (2002) Clinical practice. Postpartum depression. N Engl J Med 347:194–199
O’Hara MW, Swain AM (1996) Rates and risk of postpartum depression: a meta analysis. Int Rev Psychiatry 8:37–54
Norhayati MN, Hazlina NH, Asrenee AR, Emilin WM (2015) Magnitude and risk factors for postpartum symptoms: a literature review. J Affect Disord 175:34–52. doi:10.1016/j.jad.2014.12.041
Levine JA, Bukowinski AT, Sevick CJ, Mehlhaff KM, Conlin AMS (2015) Postpartum depression and timing of spousal military deployment relative to pregnancy and delivery. Arch Gynecol Obstet 292:549–558. doi:10.1007/s00404-015-3672-7
Dias CC, Figueiredo B (2015) Breastfeeding and depression: a systematic review of the literature. J Affect Disord 171:142–154. doi:10.1016/j.jad.2014.09.022
Rogers R, Wise RG, Painter DJ, Longe SE, Tracey I (2004) An investigation to dissociate the analgesic and anesthetic properties of ketamine using functional magnetic resonance imaging. Anesthesiology 100:292–301
Bauchat JR, Higgins N, Wojciechowski KG, McCarthy RJ, Toledo P, Wong CA (2011) Low-dose ketamine with multimodal postcesarean delivery analgesia: a randomized controlled trial. Int J Obstet Anesth 20:3–9. doi:10.1016/j.ijoa.2010.10.002
Han SY, Jin HC, Yang WD, Lee JH, Cho SH, Chae WS, Lee JS, Kim YI (2013) The effect of low-dose ketamine on post-caesarean delivery analgesia after spinal anesthesia. Korean J pain 26:270–276. doi:10.3344/kjp.2013.26.3.270
Kwok S, Wang H, Leong Sng B (2014) Post-caesarean analgesia. Trends in Anaesthesia Critical Care 4:189–194. doi:10.1016/j.tacc.2014.10.001
Gao JX, Xu JM (2015) Efficacy of ketamine in preventing postpartum depression in patients undergoing cesarean section. Chin J Anesthesiol 35:674–676.
Paule MG, Li M, Allen RR, Liu F, Zou X, Hotchkiss C, Hanig JP, Patterson TA, Slikker W Jr, Wang C (2011) Ketamine anesthesia during the first week of life can cause long-lasting cognitive deficits in rhesus monkeys. Neurotoxicol Teratol 33:220–230. doi:10.1016/j.ntt.2011.01.001
Zarate CA Jr, Singh JB, Carlson PJ, Brutsche NE, Ameli R, Luckenbaugh DA, Charney DS, Manji HK (2006) A randomized trial of an Nmethyl-D-aspartate antagonist in treatment resistant major depression. Arch Gen Psychiatry 63:856–864
VanDenKerkhof EG, Peters ML, Bruce J (2013) Chronic pain after surgery.time for standardization? A framework to establish core risk factor and outcome domains for epidemiological studies. Clin J Pain 29:2–8. doi:10.1097/AJP.0b013e31824730c2
Eisenach JC, Pan P, Smiley RM, Lavand’homme P, Landau R, Houle TT (2013) Resolution of pain after childbirth. Anesthesiology 118:143–151. doi:10.1097/ALN.0b013e318278ccfd
Acknowledgements
We extend our appreciation to Yun Yang for statistical support.
Authors' contribution
YX: Project development, Data collection, Manuscript writing. YTL: Project development. XL Huang: Project development. DLC: Random allocation sequence generation BZS: Data collection. DQM: Manuscript writing
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was obtained by any of the authors for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Xu, Y., Li, Y., Huang, X. et al. Single bolus low-dose of ketamine does not prevent postpartum depression: a randomized, double-blind, placebo-controlled, prospective clinical trial. Arch Gynecol Obstet 295, 1167–1174 (2017). https://doi.org/10.1007/s00404-017-4334-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-017-4334-8