Abstract
Objective
To analyze the prognosis of cutaneous adnexal malignancies, survival relative to surgical management, and utility of lymph-node biopsy.
Design
Population-based study of the SEER-18 database from 1975 to 2016.
Participants
7591 patients with sweat gland carcinoma, hidradenocarcinoma, spiradenocarcinoma, sclerosing sweat duct tumor/microcystic adnexal tumor (SSDT/MAC), porocarcinoma, eccrine adenocarcinoma, and sebaceous carcinoma
Results
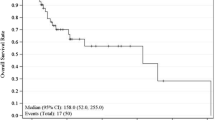
Five-year OS ranged from 68.0 to 82.6%, while 5-year DSS ranged from 94.6 to 99.0%. The majority of patients were treated with narrow (42.4%) or wide local excision (16.9%). DSS at 5 years showed that patients with stage IV had significantly poorer survival (50.3%) than I, II, or III (99.3%, 97.8%, and 89.0% respectively). 5-year OS was significantly higher for narrow excision (excision with < 1 cm margin, 78.5%) than observation (65.0%), excisional biopsy (66.8%), or wide local excision (WLE, 73.2%). Lymph-node biopsy was performed in a minority of cases (8.1%) and patients showed no significant difference in survival based on nodal status. The sensitivity and specificity of lymph-node biopsy for all malignancies were 46% and 80%, respectively. The PPV and NPV for that group were 0.46 and 0.80, respectively. Invasion of deep extradermal structures was a poor predictor of nodal positivity.
Conclusions
These malignancies have excellent DSS. Narrow excisions demonstrate better 5-year DSS and OS compared with WLE. Lymph-node biopsy is a poor predictor of survival in advanced stage disease and utility is limited.
Similar content being viewed by others
References
Obaidat NA, Alsaad KO, Ghazarian D (2007) Skin adnexal neoplasms–part 2: an approach to tumours of cutaneous sweat glands. J Clin Pathol 60(2):145–159. https://doi.org/10.1136/jcp.2006.041608
Worley B, Owen JL, Barker CA et al (2019) Evidence-based clinical practice guidelines for microcystic adnexal carcinoma. JAMA Dermatol 155(9):1059. https://doi.org/10.1001/jamadermatol.2019.1251
Bogner PN, Fullen DR, Lowe L et al (2003) Lymphatic mapping and sentinel lymph node biopsy in the detection of early metastasis from sweat gland carcinoma. Cancer 97(9):2285–2289. https://doi.org/10.1002/cncr.11328
Delgado R, Kraus D, Coit DG, Busam KJ (2003) Sentinel lymph node analysis in patients with sweat gland carcinoma. Cancer 97(9):2279–2284. https://doi.org/10.1002/cncr.11327
Crowson AN, Magro CM, Mihm MC (2006) Malignant adnexal neoplasms. Mod Pathol 19(Suppl 2):S93–S126. https://doi.org/10.1038/modpathol.3800511
Martinez SR (2011) Rare tumors through the looking glass. Arch Dermatol 147(9):1058. https://doi.org/10.1001/archdermatol.2011.229
Cancer AJC (2001) On AJCC cancer staging manual, vol 6; 2001
Oyasiji T, Tan W, Kane J et al (2018) Malignant adnexal tumors of the skin: a single institution experience. World J Surg Oncol 16(1):99. https://doi.org/10.1186/s12957-018-1401-y
De Iuliis F, Amoroso L, Taglieri L et al (2014) Chemotherapy of rare skin adnexal tumors: a review of literature. Anticancer Res 34(10):5263–5268. https://www.ncbi.nlm.nih.gov/pubmed/25275018
Staiger RD, Helmchen B, Papet C, Mattiello D, Zingg U (2017) Spiradenocarcinoma: a comprehensive data review. Am J Dermatopathol 39(10):715–725. https://doi.org/10.1097/DAD.0000000000000910
Owen JL, Kibbi N, Worley B et al (2019) Sebaceous carcinoma: evidence-based clinical practice guidelines. Lancet Oncol 20(12):e699–e714. https://doi.org/10.1016/S1470-2045(19)30673-4
Leibovitch I, Huilgol SC, Selva D, Lun K, Richards S, Paver R (2005) Microcystic adnexal carcinoma: treatment with Mohs micrographic surgery. J Am Acad Dermatol 52(2):295–300. https://doi.org/10.1016/j.jaad.2004.10.868
Brady KL, Hurst EA (2017) Sebaceous carcinoma treated with Mohs micrographic surgery. Dermatol Surg 43(2):281–286. https://doi.org/10.1097/DSS.0000000000000943
Tolkachjov SN, Hocker TL, Hochwalt PC et al (2015) Mohs micrographic surgery for the treatment of hidradenocarcinoma: the Mayo Clinic experience from 1993 to 2013. Dermatol Surg 41(2):226–231. https://doi.org/10.1097/DSS.0000000000000242
Beaulieu D, Fathi R, Mir A, Nijhawan RI (2019) Spiradenocarcinoma treated with Mohs micrographic surgery. Dermatol Surg 45(1):152–154. https://doi.org/10.1097/DSS.0000000000001534
Funding
Research reported in this publication was supported by NIH Grant P30 CA77598 utilizing the Biostatistics and Bioinformatics Core shared resource of the Masonic Cancer Center, University of Minnesota, and by the National Center for Advancing Translational Sciences of the National Institutes of Health Award Number UL1-TR002494. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
Drs. AG and IM had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: AG; acquisition, analysis, and interpretation of data: AG; drafting of the manuscript: AG; critical revision of the manuscript for important intellectual content: AG, TM, NG, NR, KP, KG, DO, KB, and IM. Statistical analysis: AG and NR; obtained funding: NR. Administrative, technical, or material support: AG; study supervision and research mentorship: IM.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest relevant to this manuscript and have no other financial relationships to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Goyal, A., Marghitu, T., Goyal, N. et al. Surgical management and lymph-node biopsy of rare malignant cutaneous adnexal carcinomas: a population-based analysis of 7591 patients. Arch Dermatol Res 313, 623–632 (2021). https://doi.org/10.1007/s00403-020-02143-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-020-02143-5