Abstract
Purpose
Pediatric primary high-grade spinal glioma (p-HGSG) is an extremely rare disease process, with little data within the current literature. Akin to primary high-grade gliomas, this cancer has been exemplified by dismal prognosis and poor response to modern treatment paradigms. This study seeks to investigate the current trends affecting overall survival using the National Cancer Database (NCDB).
Methods
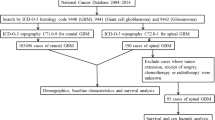
The NCDB was queried for p-HGSG between 2004 and 2016, by utilizing the designated diagnosis codes. Kaplan-Meier curves were generated, and log-rank testing was performed to analyze factors affecting overall survival. In addition, a Cox proportional-hazards model was used to perform multivariate regression analysis of survival outcomes.
Results
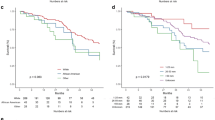
A cohort of 97 patients was identified with a histologically confirmed p-HGSG. The overall incidence of p-HGSG in all pediatric spinal cord tumors is 7.5%, with a mean survival time of 25.3 months (SD, 21.0) and 5-year overall survival of 17.0%. The majority of patients underwent surgery (n = 87, 89.7%), radiotherapy (n = 73, 75.3%), and chemotherapy (n = 60, 61.9%). Univariate, multivariate, and Kaplan-Meier log-rank testing failed to demonstrate an association between performing surgery, extent of resection, radiotherapy, or chemotherapy with improved survival outcomes.
Conclusions
The current study constitutes the largest retrospective analysis of p-HGSGs to date, finding that current treatment options of surgery, radiotherapy, and chemotherapy have unclear benefit. This disease process has a poor prognosis without a current modality of treatment that conclusively alters survival. The risks and side effects of these treatment modalities must be carefully considered in such a highly aggressive disease process, especially given potentially limited survival benefits.



Similar content being viewed by others
References
Ostrom QT, Cioffi G, Gittleman H, Patil N, Waite K, Kruchko C, Barnholtz-Sloan JS (2019) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2012-2016. Neuro-Oncol 21:v1–v100. https://doi.org/10.1093/neuonc/noz150
DeSousa AL, Kalsbeck JE, Mealey J et al (1979) Intraspinal tumors in children. A review of 81 cases. J Neurosurg 51:437–445. https://doi.org/10.3171/jns.1979.51.4.0437
Constantini S, Houten J, Miller DC, Freed D, Ozek MM, Rorke LB, Allen JC, Epstein FJ (1996) Intramedullary spinal cord tumors in children under the age of 3 years. J Neurosurg 85:1036–1043. https://doi.org/10.3171/jns.1996.85.6.1036
Reimer R, Onofrio BM (1985) Astrocytomas of the spinal cord in children and adolescents. J Neurosurg 63:669–675. https://doi.org/10.3171/jns.1985.63.5.0669
Lam S, Lin Y, Melkonian S (2012) Analysis of risk factors and survival in pediatric high-grade spinal cord astrocytoma: a population-based study. Pediatr Neurosurg 48:299–305. https://doi.org/10.1159/000353135
Benesch M, Frappaz D, Massimino M (2012) Spinal cord ependymomas in children and adolescents. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 28:2017–2028. https://doi.org/10.1007/s00381-012-1908-4
Kutluk T, Varan A, Kafalı C, Hayran M, Söylemezoğlu F, Zorlu F, Aydın B, Yalçın B, Akyüz C, Büyükpamukçu M (2015) Pediatric intramedullary spinal cord tumors: a single center experience. Eur J Paediatr Neurol EJPN Off J Eur Paediatr Neurol Soc 19:41–47. https://doi.org/10.1016/j.ejpn.2014.09.007
Rossitch E, Zeidman SM, Burger PC et al (1990) Clinical and pathological analysis of spinal cord astrocytomas in children. Neurosurgery 27:193–196. https://doi.org/10.1097/00006123-199008000-00003
Alvi MA, Ida CM, Paolini MA, Kerezoudis P, Meyer J, Barr Fritcher EG, Goncalves S, Meyer FB, Bydon M, Raghunathan A (2019) Spinal cord high-grade infiltrating gliomas in adults: clinico-pathological and molecular evaluation. Mod Pathol Off J U S Can Acad Pathol Inc 32:1236–1243. https://doi.org/10.1038/s41379-019-0271-3
Wolff B, Ng A, Roth D, Parthey K, Warmuth-Metz M, Eyrich M, Kordes U, Kortmann R, Pietsch T, Kramm C, Wolff JEA (2012) Pediatric high grade glioma of the spinal cord: results of the HIT-GBM database. J Neuro-Oncol 107:139–146. https://doi.org/10.1007/s11060-011-0718-y
Konar SK, Bir SC, Maiti TK, Nanda A (2017) A systematic review of overall survival in pediatric primary glioblastoma multiforme of the spinal cord. J Neurosurg Pediatr 19:239–248. https://doi.org/10.3171/2016.8.PEDS1631
Allen JC, Aviner S, Yates AJ, Boyett JM, Cherlow JM, Turski PA, Epstein F, Finlay JL, _ _ (1998) Treatment of high-grade spinal cord astrocytoma of childhood with “8-in-1” chemotherapy and radiotherapy: a pilot study of CCG-945. Children’s Cancer Group. J Neurosurg 88:215–220. https://doi.org/10.3171/jns.1998.88.2.0215
Tendulkar RD, Pai Panandiker AS, Wu S, Kun LE, Broniscer A, Sanford RA, Merchant TE (2010) Irradiation of pediatric high-grade spinal cord tumors. Int J Radiat Oncol Biol Phys 78:1451–1456. https://doi.org/10.1016/j.ijrobp.2009.09.071
Guss ZD, Moningi S, Jallo GI, Cohen KJ, Wharam MD, Terezakis SA (2013) Management of pediatric spinal cord astrocytomas: outcomes with adjuvant radiation. Int J Radiat Oncol Biol Phys 85:1307–1311. https://doi.org/10.1016/j.ijrobp.2012.11.022
Indelicato DJ, Rotondo RL, Uezono H, Sandler ES, Aldana PR, Ranalli NJ, Beier AD, Morris CG, Bradley JA (2019) Outcomes following proton therapy for pediatric low-grade Glioma. Int J Radiat Oncol Biol Phys 104:149–156. https://doi.org/10.1016/j.ijrobp.2019.01.078
Constantini S, Miller DC, Allen JC, Rorke LB, Freed D, Epstein FJ (2000) Radical excision of intramedullary spinal cord tumors: surgical morbidity and long-term follow-up evaluation in 164 children and young adults. J Neurosurg 93:183–193. https://doi.org/10.3171/spi.2000.93.2.0183
Kheirkhah P, Denyer S, Bhimani AD, Arnone GD, Esfahani DR, Aguilar T, Zakrzewski J, Venugopal I, Habib N, Gallia GL, Linninger A, Charbel FT, Mehta AI (2018) Magnetic drug targeting: a novel treatment for intramedullary spinal cord tumors. Sci Rep 8:11417. https://doi.org/10.1038/s41598-018-29736-5
Wang SS, Bandopadhayay P, Jenkins MR (2019) Towards immunotherapy for pediatric brain tumors. Trends Immunol 40:748–761. https://doi.org/10.1016/j.it.2019.05.009
Rajesh Y, Pal I, Banik P, Chakraborty S, Borkar SA, Dey G, Mukherjee A, Mandal M (2017) Insights into molecular therapy of glioma: current challenges and next generation blueprint. Acta Pharmacol Sin 38:591–613. https://doi.org/10.1038/aps.2016.167
Alinezhad A, Jafari F (2019) Novel management of glioma by molecular therapies, a review article. Eur J Transl Myol 29. https://doi.org/10.4081/ejtm.2019.8209
Funding
The grant support from the AOSPine Innovation Grant (awarded to senior author) was utilized for funding this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nunna, R.S., Khalid, S., Behbahani, M. et al. Pediatric primary high-grade spinal glioma: a National Cancer Database analysis of current patterns in treatment and outcomes. Childs Nerv Syst 37, 185–193 (2021). https://doi.org/10.1007/s00381-020-04722-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-020-04722-3