Abstract
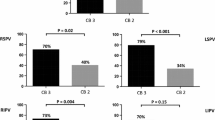
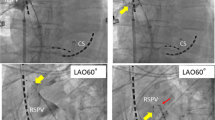
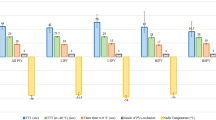
The association between circulatory dynamics changes during cryoballoon applications and a successful pulmonary vein isolation (PVI) is unknown. Seventy atrial fibrillation patients who underwent PVI with 28-mm second-generation cryoballoons and single 3-min freezes were included. Intra-procedural parameters including circulatory dynamics changes during cryoapplications, were compared between 113 successful applications (30 left superior PVs[LSPVs], 30 left inferior PVs[LIPVs], 25 right superior PVs[RSPVs], and 28 right inferior PVs[RIPVs]) and 47 failed applications (10 LSPVs, 9 LIPVs, 8 RSPVs, and 20 RIPVs). In all individual PVs, lower nadir balloon temperatures (MinTemps) and longer thawing times (ThawTimes) significantly predicted a successful PVI. In addition, greater systolic blood pressure drops following releasing the PV occlusion (SBP-drops) significantly predicted a successful right PV PVI, and longer elapse times during SBP-drops significantly predicted a successful RIPV PVI. Composite parameters incorporating MinTemps and ThawTimes, SBP-drops, and ThawTimes showed the highest area under the curve to predict a successful left PV (0.876 for LSPVs, 0.851 for LIPVs) and right PV (0.927 for RSPVs, 0.980 for RIPVs) PVI, respectively. If the ThawTime (≥ 30 s) and SBP-drop (≤ − 21 mmHg) cutoff values were achieved for the RIPVs, the positive predictive value was 100%. In contrast, if both criteria were not achieved for the RIPVs, the negative predictive value was 100%. In the second-generation cryoballoon PVI, the MinTemp and ThawTime were significantly associated with acute success for all four PVs. In addition, SBP-drops further improved the accuracy of predicting a successful right PV PVI, especially of the RIPV.



Similar content being viewed by others
References
Haissaguerre M, Jais P, Shah DC, Takahashi A, Hocini M, Quiniou G, Garrigue S, Le Mouroux A, Le Métayer P, Clémenty J (1998) Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med 339:659–666
Calkins H, Kuck KH, Cappato R, Brugada J, Camm AJ, Chen SA, Crijns HJ, Damiano RJ, Davies DW, DiMarco J, Edgerton J, Ellenbogen K, Ezekowitz MD, Haines DE, Haissaguerre M, Hindricks G, Iesaka Y, Jackman W, Jalife J, Jais P, Kalman J, Keane D, Kim YH, Kirchhof P, Klein G, Kottkamp H, Kumagai K, Lindsay BD, Mansour M, Marchlinski FE, McCarthy PM, Mont JL, Morady F, Nademanee K, Nakagawa H, Natale A, Nattel S, Packer DL, Pappone C, Prystowsky E, Raviele A, Reddy V, Ruskin JN, Shemin RJ, Tsao HM, Wilber D, Heart Rhythm Society Task Force on Catheter, and Surgical Ablation of Atrial Fibrillation (2012) 2012 HRS/EHRA/ECAS expert consensus statement on catheter and surgical ablation of atrial fibrillation: recommendations for patient selection, procedural techniques, patient management and follow-up, definitions, endpoints, and research trial design: a report of the Heart Rhythm Society (HRS) task force on catheter and surgical ablation of atrial fibrillation. Heart Rhythm 9(632–696):e21
Kojodjojo P, O'Neill MD, Lim PB, Malcolm-Lawes L, Whinnett ZI, Salukhe TV, Linton NW, Lefroy D, Mason A, Wright I, Peters NS, Kanagaratnam P, Davies DW (2010) Pulmonary venous isolation by antral ablation with a large cryoballoon for treatment of paroxysmal and persistent atrial fibrillation: medium-term outcomes and non-randomised comparison with pulmonary venous isolation by radiofrequency ablation. Heart 96:1379–1384
Packer DL, Kowal RC, Wheelan KR, Irwin JM, Champagne J, Guerra PG, Dubuc M, Reddy V, Nelson L, Holcomb RG, Lehmann JW, Ruskin JN, Cryoablation Investigators STOPAF (2013) Cryoballoon ablation of pulmonary veins for paroxysmal atrial fibrillation: first results of the North American Arctic Front (STOP AF) pivotal trial. J Am Coll Cardiol 61:1713–1723
Kuck KH, Brugada J, Furnkranz A, Metzner A, Ouyang F, Chun KR, Elvan A, Arentz T, Bestehorn K, Pocock SJ, Albenque JP, Tondo C, FIRE AND ICE investigators (2016) Cryoballoon or radiofrequency ablation for paroxysmal atrial fibrillation. N Engl J Med 374:2235–2245
Coulombe N, Paulin J, Su W (2013) Improved in vivo performance of second-generation cryoballoon for pulmonary vein isolation. J Cardiovasc Electrophysiol 24:919–925
Kajiyama T, Miyazaki S, Matsuda J, Watanabe T, Niida T, Takagi T, Nakamura H, Taniguchi H, Hachiya H, Iesaka Y (2017) Anatomic parameters predicting procedural difficulty and balloon temperature predicting successful applications in individual pulmonary veins during 28-mm second-generation cryoballoon ablation. JACC Clin Electrophysiol 3:580–588
Deubner N, Greiss H, Akkaya E, Zaltsberg S, Hain A, Berkowitsch A, Guttler N, Kuniss M, Neumann T (2017) The slope of the initial temperature drop predicts acute pulmonary vein isolation using the second-generation cryoballoon. Europace 19:1470–1477
Kajiyama T, Miyazaki S, Watanabe T, Yamao K, Kusa S, Igarashi M, Nakamura H, Hachiya H, Iesaka Y (2017) Circulatory dynamics during pulmonary vein isolation using the second-generation cryoballoon. J Am Heart Assoc 6:e006559
Miyazaki S, Hachiya H, Taniguchi H, Nakamura H, Ichihara N, Usui E, Kuroi A, Takagi T, Iwasawa J, Hirao K, Iesaka Y (2015) Prospective evaluation of bilateral diaphragmatic electromyograms during cryoballoon ablation of atrial fibrillation. J Cardiovasc Electrophysiol 26:622–628
Su W, Kowal R, Kowalski M, Metzner A, Svinarich JT, Wheelan K, Wang P (2015) Best practice guide for cryoballoon ablation in atrial fibrillation: the compilation experience of more than 3000 procedures. Heart Rhythm 12:1658–1666
R Core Team (2017) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. https://www.R-project.org/
Furnkranz A, Koster I, Chun KR, Metzner A, Mathew S, Konstantinidou M, Ouyang F, Kuck KH (2011) Cryoballoon temperature predicts acute pulmonary vein isolation. Heart Rhythm 8:821–825
Acknowledgements
We would like to thank Mr. John Martin for his help in the preparation of the manuscript.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kajiyama, T., Miyazaki, S., Hamaya, R. et al. Circulatory dynamics changes are an additional predictor of successful pulmonary vein isolation during cryoballoon ablation. Heart Vessels 35, 125–131 (2020). https://doi.org/10.1007/s00380-019-01467-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-019-01467-1