Abstract
Purpose
To prospectively evaluate the rate and associated risk factors of early infectious complications after ureterorenoscopy for urolithiasis.
Methods
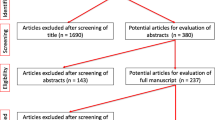
After ethical committee approval, 400 therapeutic retrograde ureterorenoscopy procedures between August 3, 2020 and November 24, 2021 were included for analysis in a single-center study. Postoperative infection was defined as an afebrile urinary tract infection, fever (≥ 38 °C) with pyuria (≥ 300 WBC/μL) or proven urinary pathogen, and urosepsis. The primary outcome was the rate of infectious complications after ureterorenoscopy. Secondary outcomes were the perioperative factors that increased the risk of infectious complications within 30 days of surgery using univariate and multivariate logistic regression analysis.
Results
Twenty-nine of four hundred (7.3%) patients developed an infectious complication within 30 days after ureterorenoscopy. Ten (2.5%) patients developed an afebrile urinary tract infection, eight (2.0%) developed fever with pyuria, five (1.3%) febrile urinary tract infection, and six (1.5%) urosepsis. On univariate analysis, preoperative stent-type JFil® pigtail suture stent was significantly associated with the dependent variable (p < 0.001). On multivariate logistic regression analysis, older age (OR 1.035; 95% CI 1.006–1.070; p = 0.02) was found to be significantly associated with developing a postoperative infectious complication.
Conclusions
A 7.3% rate of postoperative infectious complications and 1.5% urosepsis rate were observed after therapeutic ureterorenoscopy, without the need of intensive care admission. The only significant risk factors were preoperative stent type (JFil® pigtail suture stent) on univariate analysis, and older age on multivariate logistic regression analysis. Further multicentric prospective observational data are needed in this field.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author.
References
De Coninck V, Keller EX, Somani B et al (2020) Complications of ureteroscopy: a complete overview. World J Urol 38:2147–2166. https://doi.org/10.1007/s00345-019-03012-1
Fernbach SK, Maizels M, Conway JJ (1993) Ultrasound grading of hydronephrosis: introduction to the system used by the Society for Fetal. Urology 23:478–480. https://doi.org/10.1007/BF02012459
Ito H, Kawahara T, Terao H et al (2013) Evaluation of preoperative measurement of stone surface area as a predictor of stone-free status after combined ureteroscopy with holmium laser lithotripsy: a single-center experience. J Endourol 27:715–721. https://doi.org/10.1089/end.2012.0548
De Coninck V, Traxer O (2018) The time has come to report stone burden in terms of volume instead of largest diameter. J Endourol 32:265–266. https://doi.org/10.1089/end.2017.0886
Panthier F, Kutchukian S, Ducousso H et al (2023) How to estimate stone volume and its use in stone surgery: a comprehensive review. Actas Urol Esp (Engl Ed). https://doi.org/10.1016/j.acuroe.2023.08.009. (English, Spanish)
Uchida Y, Takazawa R, Kitayama S, Tsujii T (2018) Predictive risk factors for systemic inflammatory response syndrome following ureteroscopic laser lithotripsy. Urolithiasis 46:375–381. https://doi.org/10.1007/s00240-017-1000-3
De Coninck V, Defraigne C, Traxer O (2022) Watt determines the temperature during laser lithotripsy. World J Urol 40:1257–1258. https://doi.org/10.1007/s00345-021-03848-6
Singer M, Deutschman CS, Seymour CW et al (2016) The third international consensus definitions for sepsis and septic shock (sepsis-3). JAMA 315:801–810. https://doi.org/10.1001/jama.2016.0287
Bernasconi V, Tozzi M, Pietropaolo A et al (2023) Comprehensive overview of ureteral stents based on clinical aspects, material and design. Cent Eur J Urol 76:49–56. https://doi.org/10.5173/ceju.2023.218
Boeykens M, Keller EX, Bosio A et al (2022) Impact of ureteral stent material on stent-related symptoms: a systematic review of the literature. Eur Urol Open Sci 45:108–117. https://doi.org/10.1016/j.euros.2022.09.005
Veeratterapillay R, Gravestock P, Harding C et al (2023) Infection after ureteroscopy for ureteric stones: analysis of 71,305 cases in the hospital episode statistics database. BJU Int 131:109–115. https://doi.org/10.1111/bju.15850
Mathias S, Wiseman O (2022) Silicone vs. polyurethane stent: the final countdown. J Clin Med. 11:2746. https://doi.org/10.3390/jcm11102746
Dybowski B, Bres-Niewada E, Rzeszutko M et al (2021) Risk factors for infectious complications after retrograde intrarenal surgery—a systematic review and narrative synthesis. Cent Eur J Urol 74:437–445. https://doi.org/10.5173/ceju.2021.250
Chugh S, Pietropaolo A, Montanari E et al (2020) Predictors of urinary infections and urosepsis after ureteroscopy for stone disease: a systematic review from EAU section of urolithiasis (EULIS). Curr Urol Rep 21:16. https://doi.org/10.1007/s11934-020-0969-2
De Coninck V, Somani B, Sener ET et al (2022) Ureteral access sheaths and its use in the future: a comprehensive update based on a literature review. J Clin Med 11:5128. https://doi.org/10.3390/jcm11175128
De Coninck V, Keller EX, Rodríguez-Monsalve M et al (2018) Systematic review of ureteral access sheaths: facts and myths. BJU Int 122:959–969. https://doi.org/10.1111/bju.14389
Muslumanoglu AY, Fuglsig S, Frattini A et al (2017) Risks and benefits of postoperative double-J stent placement after ureteroscopy: results from the clinical research office of endourological society ureteroscopy global study. J Endourol 31:446–451. https://doi.org/10.1089/end.2016.0827
Borboroglu PG, Amling CL, Schenkman NS et al (2001) Ureteral stenting after ureteroscopy for distal ureteral calculi: a multi-institutional prospective randomized controlled study assessing pain, outcomes and complications. J Urol 166:1651–1657. https://doi.org/10.1016/s0022-5347(05)65646-7
Acknowledgements
We owe a significant debt of gratitude to Martial Luyts, an esteemed biostatistics expert from the University of Leuven, for his invaluable statistical assistance in crafting this paper.
Disclosures
Vincent De Coninck is a speaker and/or consultant for BD, Coloplast, and Karl Storz, and has no specific conflicts relevant to this study. Etienne Xavier Keller is a speaker and/or consultant for Coloplast, Olympus, Boston Scientific, Recordati, Debiopharm and Alnylam, and has no specific conflicts of interest relevant to this work. All other authors have no relevant financial or non-financial interests to disclose.
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
B Devos: project development, data collection or management, data analysis, manuscript writing. M Claessens: project development, data collection or management. A Duchateau: project development, data collection or management. R Hente: project development, data collection or management. W Vanderbruggen: project development, data collection or management. E.X. Keller: manuscript editing. A. Pietropaolo: manuscript editing. B Van Cleynenbreugel: project development, data analysis, manuscript editing. V De Coninck: research concept, protocol/project development, data collection or management, data analysis, manuscript writing/editing.
Corresponding author
Ethics declarations
Conflicts of interests
The other authors declare that they have no conflict of interest.
Informed consent
This is a prospective study. Patients were consented for their participation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Devos, B., Vanderbruggen, W., Claessens, M. et al. Risk factors of early infectious complications after ureterorenoscopy for stone disease: a prospective study. World J Urol 42, 277 (2024). https://doi.org/10.1007/s00345-024-04983-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00345-024-04983-6