Abstract
Introduction
This systematic review aims at reporting the incidence, predictive factors, and the oncological outcomes of incidental prostate cancer (IPCa) in men who underwent endoscopic enucleation of prostate (EEP).
Methods
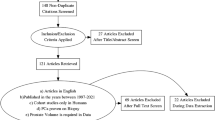
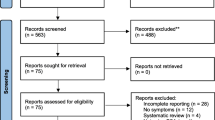
A literature search was performed using the following Medical Subject Heading (MeSH) terms and keywords: “Prostatic Neoplasms”, “Prostate Cancer”, “Transurethral Resection of Prostate”, “Prostate resection”, “Prostate enucleation”. Meta-analysis was performed if there were two or more studies reporting the same outcome under the same definition. In case of insufficient data, results were presented in a narrative manner.
Results
Sixty-one studies were included in qualitative synthesis and 55 were included in meta-analysis. The pooled IPCa rate was 0.08 (95% CI 0.073–0.088). Increasing age, higher preoperative serum prostate-specific antigen (PSA) level, higher preoperative PSA density (PSAD), smaller prostate volume, higher postoperative PSA velocity and lower enucleated prostate weight, were reported to have significant correlation with IPCa. In BPH patients, the mean pre-operative and post-operative PSA levels were 5.58 ± 1.48 ng/dL and 1.06 ± 0.27 ng/dL, respectively. In patients with IPCa, the mean pre-operative and post-operative PSA levels were 7.72 ± 2.90 ng/dL and 2.77 ± 1.66 ng/dL, respectively. The mean percentage PSA reduction was 82.0% ± 1.8% for BPH patients and 68.2% ± 12.1% for IPCa patients. IPCa was most commonly managed by active surveillance (68.7%).
Conclusions
The pooled incidence of IPCa after EEP was 8%. An absolute post-operative PSA level of < 2.0 and a percentage PSA reduction of > 70% should be expected in BPH patients after EEP.



Similar content being viewed by others
References
Rawla P (2019) Epidemiology of prostate cancer. World J Oncol 10(2):63–89
Loeb S, Gonzalez CM, Roehl KA, Han M, Antenor JA, Yap RL et al (2006) Pathological characteristics of prostate cancer detected through prostate specific antigen based screening. J Urol 175(3 Pt 1):902–906
Distler FA, Radtke JP, Bonekamp D, Kesch C, Schlemmer HP, Wieczorek K et al (2017) The value of PSA density in combination with PI-RADS for the accuracy of prostate cancer prediction. J Urol 198(3):575–582
Ahmed HU, El-Shater Bosaily A, Brown LC, Gabe R, Kaplan R, Parmar MK et al (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 389(10071):815–822
Loeb S, Catalona WJ (2014) The Prostate Health Index: a new test for the detection of prostate cancer. Ther Adv Urol 6(2):74–77
Jones JS, Follis HW, Johnson JR (2009) Probability of finding T1a and T1b (incidental) prostate cancer during TURP has decreased in the PSA era. Prostate Cancer Prostatic Dis 12(1):57–60
Adolfsson J (2008) The management of category T1a–T1b (incidental) prostate cancer: can we predict who needs treatment? Eur Urol 54(1):16–18
Cho CL, Teoh JY, Cho SY, Ng AC, Henkel R (2020) Quest for the best-A move to anatomical endoscopic enucleation of the prostate. Andrologia 52(8):e13757
Gratzke C, Bachmann A, Descazeaud A, Drake MJ, Madersbacher S, Mamoulakis C et al (2015) EAU guidelines on the assessment of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol 67(6):1099–1109
Teoh JY, Cho CL, Wei Y, Isotani S, Tiong HY, Ong TA et al (2020) Surgical training for anatomical endoscopic enucleation of the prostate. Andrologia. https://doi.org/10.1111/and.13708
Wroclawski ML, Teles SB, Amaral BS, Kayano PP, Cha JD, Carneiro A et al (2020) A systematic review and meta-analysis of the safety and efficacy of endoscopic enucleation and non-enucleation procedures for benign prostatic enlargement. World J Urol 38(7):1663–1684
Hirayama T, Matsumoto K, Sugita Y, Nishi M, Tabata K, Fujita T et al (2015) 826 Incidence and outcomes of prostate cancer following holmium laser enucleation of the prostate. Eur Urol Suppl 14(2):826
Hutchison D, Peabody H, Kuperus JM, Humphrey JE, Ryan M, Moriarity A, Brede CM, Lane BR (2021) Management of prostate cancer after holmium laser enucleation of the prostate. Urol Oncol 39(5):297.e1–297.e8. https://doi.org/10.1016/j.urolonc.2020.11.003
Otsubo S, Yokomizo A, Mochida O, Shiota M, Tatsugami K, Inokuchi J et al (2015) Significance of prostate-specific antigen-related factors in incidental prostate cancer treated by holmium laser enucleation of the prostate. World J Urol 33(3):329–333
Gudaru K, Gonzalez Padilla DA, Castellani D, Tortolero Blanco L, Tanidir Y, Ka Lun L et al (2020) A global knowledge, attitudes and practices survey on anatomical endoscopic enucleation of prostate for benign prostatic hyperplasia among urologists. Andrologia 52(8):e13717
Li M, Qiu J, Hou Q, Wang D, Huang W, Hu C et al (2015) Endoscopic enucleation versus open prostatectomy for treating large benign prostatic hyperplasia: a meta-analysis of randomized controlled trials. PLoS ONE 10(3):e0121265
Lin Y, Wu X, Xu A, Ren R, Zhou X, Wen Y et al (2016) Transurethral enucleation of the prostate versus transvesical open prostatectomy for large benign prostatic hyperplasia: a systematic review and meta-analysis of randomized controlled trials. World J Urol 34(9):1207–1219
Rosenhammer B, Lausenmeyer EM, Mayr R, Burger M, Eichelberg C (2018) HoLEP provides a higher prostate cancer detection rate compared to bipolar TURP: a matched-pair analysis. World J Urol 36(12):2035–2041
Herlemann A, Wegner K, Roosen A, Buchner A, Weinhold P, Bachmann A et al (2017) “Finding the needle in a haystack”: oncologic evaluation of patients treated for LUTS with holmium laser enucleation of the prostate (HoLEP) versus transurethral resection of the prostate (TURP). World J Urol 35(11):1777–1782
Naspro R, Freschi M, Salonia A, Guazzoni G, Girolamo V, Colombo R et al (2004) Holmium laser enucleation versus transurethral resection of the prostate. Are histological findings comparable? J Urol 171(3):1203–1206
Bell KJ, Del Mar C, Wright G, Dickinson J, Glasziou P (2015) Prevalence of incidental prostate cancer: a systematic review of autopsy studies. Int J Cancer 137(7):1749–1757
McNeal JE, Redwine EA, Freiha FS, Stamey TA (1988) Zonal distribution of prostatic adenocarcinoma. Correlation with histologic pattern and direction of spread. Am J Surg Pathol 12(12):897–906
Dickinson JA (2018) Guideline: USPSTF recommends against PSA screening except in men 55 to 69 years who express a preference for it. Ann Intern Med 169(6):JC28
Jue JS, Barboza MP, Prakash NS, Venkatramani V, Sinha VR, Pavan N et al (2017) Re-examining prostate-specific antigen (PSA) density: defining the optimal psa range and patients for using psa density to predict prostate cancer using extended template biopsy. Urology 105:123–128
Elkoushy MA, Elshal AM, Elhilali MM (2015) Incidental prostate cancer diagnosis during holmium laser enucleation: assessment of predictors, survival, and disease progression. Urology 86(3):552–557
Capogrosso P, Capitanio U, Vertosick EA, Ventimiglia E, Chierigo F, Oreggia D et al (2018) Temporal trend in incidental prostate cancer detection at surgery for benign prostatic hyperplasia. Urology 122:152–157
Kim M, Song SH, Ku JH, Oh SJ, Paick JS (2014) Prostate cancer detected after Holmium laser enucleation of prostate (HoLEP): significance of transrectal ultrasonography. Int Urol Nephrol 46(11):2079–2085
Ohwaki K, Endo F, Shimbo M, Fujisaki A, Hattori K (2017) Comorbidities as predictors of incidental prostate cancer after Holmium laser enucleation of the prostate: diabetes and high-risk cancer. Aging Male 20(4):257–260
Thompson IM Jr, Goodman PJ, Tangen CM, Parnes HL, Minasian LM, Godley PA et al (2013) Long-term survival of participants in the prostate cancer prevention trial. N Engl J Med 369(7):603–610
Andriole GL, Bostwick DG, Brawley OW, Gomella LG, Marberger M, Montorsi F et al (2010) Effect of dutasteride on the risk of prostate cancer. N Engl J Med 362(13):1192–1202
Feng X, Song M, Preston MA, Ma W, Hu Y, Pernar CH et al (2020) The association of diabetes with risk of prostate cancer defined by clinical and molecular features. Br J Cancer 123(4):657–665
Kasper JS, Liu Y, Giovannucci E (2009) Diabetes mellitus and risk of prostate cancer in the health professionals follow-up study. Int J Cancer 124(6):1398–1403
Leitzmann MF, Ahn J, Albanes D, Hsing AW, Schatzkin A, Chang SC et al (2008) Diabetes mellitus and prostate cancer risk in the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial. Cancer Causes Control 19(10):1267–1276
Bandini M, Gandaglia G, Briganti A (2017) Obesity and prostate cancer. Curr Opin Urol 27(5):415–421
Gallagher EJ, LeRoith D (2010) The proliferating role of insulin and insulin-like growth factors in cancer. Trends Endocrinol Metab 21(10):610–618
Lane BR, Stephenson AJ, Magi-Galluzzi C, Lakin MM, Klein EA (2008) Low testosterone and risk of biochemical recurrence and poorly differentiated prostate cancer at radical prostatectomy. Urology 72(6):1240–1245
Tang KD, Liu J, Jovanovic L, An J, Hill MM, Vela I et al (2016) Adipocytes promote prostate cancer stem cell self-renewal through amplification of the cholecystokinin autocrine loop. Oncotarget 7(4):4939–4948
Banez LL, Hamilton RJ, Partin AW, Vollmer RT, Sun L, Rodriguez C et al (2007) Obesity-related plasma hemodilution and PSA concentration among men with prostate cancer. JAMA 298(19):2275–2280
Boehm K, Sun M, Larcher A, Blanc-Lapierre A, Schiffmann J, Graefen M et al (2015) Waist circumference, waist-hip ratio, body mass index, and prostate cancer risk: results from the North-American case-control study prostate cancer and environment study. Urol Oncol 33(11):494 e1-497
Onur R, Littrup PJ, Pontes JE, Bianco FJ Jr (2004) Contemporary impact of transrectal ultrasound lesions for prostate cancer detection. J Urol 172(2):512–514
Tominaga Y, Sadahira T, Mitsui Y, Maruyama Y, Tanimoto R, Wada K et al (2019) Favorable long-term oncological and urinary outcomes of incidental prostate cancer following holmium laser enucleation of the prostate. Mol Clin Oncol 10(6):605–609
Rose K, Faraj K, Navaratnam A, Girardo M, Pima AN, Arora K et al (2020) PD56–01: prostate specific antigen kinetics predict incidental prostate cancer progression following holmium laser enucleation of the prostate. J Urol 203(Supplement 4):e1188-e
Author information
Authors and Affiliations
Corresponding authors
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cheng, B.KC., Castellani, D., Chan, I.SH. et al. Incidence, predictive factors and oncological outcomes of incidental prostate cancer after endoscopic enucleation of the prostate: a systematic review and meta-analysis. World J Urol 40, 87–101 (2022). https://doi.org/10.1007/s00345-021-03756-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-021-03756-9