Abstract
Introduction
In a population-based case–control study (PROtEuS), we examined the association between prostate cancer (PCa) and (1) benign prostatic hypertrophy (BPH) history at any time prior to PCa diagnosis, (2) BPH-history reported at least 1 year prior to interview/diagnosis (index date) and (3) exposure to BPH-medications.
Methods
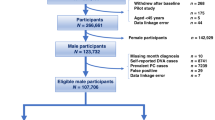
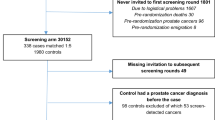
Cases were 1933 men with incident prostate cancer diagnosed across Montreal French hospitals between 2005 and 2009. Population controls were 1994 men from the same age distribution and residential area. In-person interviews collected socio-demographic characteristics and medical history, e.g., BPH diagnosis, duration and treatment, as well as on PCa screening. Logistic regression analyses tested overall and grade-specific associations, including subgroup analyses with frequent PSA testing.
Results
A BPH-history was associated with an increased risk of PCa (OR 1.37 [95 % CI 1.16–2.61]), more pronounced for low-grade PCa (Gleason ≤6: OR 1.54 [1.26–1.87]; Gleason ≥7: OR 1.05 [0.86–1.27]). The association was not significant when BPH-history diagnosis was more than 1 year prior to index date, except for low-grade PCa (OR 1.29 [1.05–1.60]). Exposure to 5α reductase inhibitors (5α-RI) resulted in a decreased risk of overall PCa (OR 0.62 [0.42–0.92]), particularly for intermediate- to high-grade PCa (Gleason ≤6: OR 0.70 [0.43–1.14]; Gleason ≥7: OR 0.43 [0.26–0.72]). Adjusting for PSA testing frequency or restricting analyses to frequently screened subjects did not affect these results.
Conclusion
BPH-history was associated with an increased PCa risk, which disappeared, when BPH-history did not include BPH diagnosis within the previous year. Our results also suggest that 5α-RI exposure exerts a protective effect on intermediate and high-grade PCa.
Similar content being viewed by others
References
Orsted DD, Bojesen SE, Nielsen SF, Nordestgaard BG (2011) Association of clinical benign prostate hyperplasia with prostate cancer incidence and mortality revisited: a nationwide cohort study of 3,009,258 men. Eur Urol 60(4):691–698
Chokkalingam AP, Nyren O, Johansson JE, Gridley G, McLaughlin JK, Adami HO et al (2003) Prostate carcinoma risk subsequent to diagnosis of benign prostatic hyperplasia: a population-based cohort study in Sweden. Cancer 98(8):1727–1734
Freedland SJ, Isaacs WB, Platz EA, Terris MK, Aronson WJ, Amling CL et al (2005) Prostate size and risk of high-grade, advanced prostate cancer and biochemical progression after radical prostatectomy: a search database study. J Clin Oncol 23(30):7546–7554
Alcaraz A, Hammerer P, Tubaro A, Schroder FH, Castro R (2009) Is there evidence of a relationship between benign prostatic hyperplasia and prostate cancer? Findings of a literature review. Eur Urol 55(4):864–873
Schenk JM, Kristal AR, Arnold KB, Tangen CM, Neuhouser ML, Lin DW et al (2011) Association of symptomatic benign prostatic hyperplasia and prostate cancer: results from the prostate cancer prevention trial. Am J Epidemiol 173(12):1419–1428
Simons BD, Morrison AS, Young RH, Verhoek-Oftedahl W (1993) The relation of surgery for prostatic hypertrophy to carcinoma of the prostate. Am J Epidemiol 138(5):294–300
Orsted DD, Bojesen SE (2013) The link between benign prostatic hyperplasia and prostate cancer. Nat Rev Urol 10(1):49–54
Parsons JK (2007) Modifiable risk factors for benign prostatic hyperplasia and lower urinary tract symptoms: new approaches to old problems. J Urol 178(2):395–401
Andriole GL, Bostwick DG, Brawley OW, Gomella LG, Marberger M, Montorsi F et al (2010) Effect of dutasteride on the risk of prostate cancer. N Engl J Med 362(13):1192–1202
Thompson IM, Goodman PJ, Tangen CM, Lucia MS, Miller GJ, Ford LG et al (2003) The influence of finasteride on the development of prostate cancer. N Engl J Med 349(3):215–224
Preston MA, Wilson KM, Markt SC, Ge R, Morash C, Stampfer MJ et al (2014) 5alpha-Reductase inhibitors and risk of high-grade or lethal prostate cancer. JAMA Intern Med 174(8):1301–1307
Parent ME, Goldberg MS, Crouse DL, Ross NA, Chen H, Valois MF et al (2013) Traffic-related air pollution and prostate cancer risk: a case-control study in Montreal, Canada. Occup Environ Med 70(7):511–518
Spence AR, Rousseau MC, Karakiewicz PI, Parent ME (2014) Circumcision and prostate cancer: a population-based case-control study in Montreal, Canada. BJU Int 114(6b):E90–E98
Blanc-Lapierre A, Weiss D, Parent ME (2014) Use of oral anticoagulants and risk of prostate cancer: a population-based case-control study in Montreal, Canada. Cancer Causes Control 25(9):1159–1166
Weight CJ, Kim SP, Jacobson DJ, McGree ME, Boorjian SA, Thompson RH et al (2013) The effect of benign lower urinary tract symptoms on subsequent prostate cancer testing and diagnosis. Eur Urol 63(6):1021–1027
Norman RW, Nickel JC, Fish D, Pickett SN (1994) ‘Prostate-related symptoms’ in Canadian men 50 years of age or older: prevalence and relationships among symptoms. Br J Urol 74(5):542–550
Acknowledgments
This study was supported financially through grants from the Canadian Cancer Society, the Cancer Research Society, the Fonds de la recherche du Québec—Santé (FRQS), FRQS-RRSE, and the Ministère du Développement économique, de l’Innovation et de l’Exportation du Québec. Marie-Élise Parent holds career awards from the FRQS. Fred Saad holds the University of Montreal Endowed Chair in Prostate Cancer Research.
Conflict of interest
None.
Ethical standard
The study was approved by the ethics boards of all participating institutions, and all subjects provided written informed consent.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Boehm, K., Valdivieso, R., Meskawi, M. et al. BPH: a tell-tale sign of prostate cancer? Results from the Prostate Cancer and Environment Study (PROtEuS). World J Urol 33, 2063–2069 (2015). https://doi.org/10.1007/s00345-015-1546-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-015-1546-z