Abstract
Objectives
We wished to determine whether tumor morphology descriptors obtained from pretreatment magnetic resonance images and clinical variables could predict survival for glioblastoma patients.
Methods
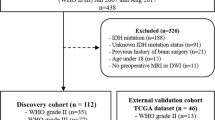
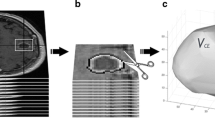
A cohort of 404 glioblastoma patients (311 discoveries and 93 validations) was used in the study. Pretreatment volumetric postcontrast T1-weighted magnetic resonance images were segmented to obtain the relevant morphological measures. Kaplan-Meier, Cox proportional hazards, correlations, and Harrell’s concordance indexes (c-indexes) were used for the statistical analysis.
Results
A linear prognostic model based on the outstanding variables (age, contrast-enhanced (CE) rim width, and surface regularity) identified a group of patients with significantly better survival (p < 0.001, HR = 2.57) with high accuracy (discovery c-index = 0.74; validation c-index = 0.77). A similar model applied to totally resected patients was also able to predict survival (p < 0.001, HR = 3.43) with high predictive value (discovery c-index = 0.81; validation c-index = 0.92). Biopsied patients with better survival were well identified (p < 0.001, HR = 7.25) by a model including age and CE volume (c-index = 0.87).
Conclusions
Simple linear models based on small sets of meaningful MRI-based pretreatment morphological features and age predicted survival of glioblastoma patients to a high degree of accuracy. The partition of the population using the extent of resection improved the prognostic value of those measures.
Key Points
• A combination of two MRI-based morphological features (CE rim width and surface regularity) and patients’ age outperformed previous prognosis scores for glioblastoma.
• Prognosis models for homogeneous surgical procedure groups led to even more accurate survival prediction based on Kaplan-Meier analysis and concordance indexes.



Similar content being viewed by others
Change history
13 December 2018
The original version of this article, published on 15 October 2018, unfortunately contained a mistake. The following correction has therefore been made in the original: The name of Mariano Amo-Salas and the affiliation of Ismael Herruzo were presented incorrectly.
Abbreviations
- 3D:
-
Three-dimensional
- c-index:
-
Concordance index
- CE:
-
Contrast-enhanced
- CoI:
-
Confidence interval
- DICOM:
-
Digital imaging and communication in medicine
- GBM:
-
Glioblastoma
- HR:
-
Hazard ratio
- MA:
-
Morphology- and age-based
- MAB:
-
Morphology- and age-based prognosis score for biopsied patients
- MASR:
-
Morphology- and age-based prognosis score for subtotally resected patients
- MATR:
-
Morphology- and age-based prognosis score for totally resected patients
- MRI:
-
Magnetic resonance images
- OS:
-
Overall survival
- P :
-
p value
- TCIA:
-
The Cancer Image Archive
- WHO:
-
World Health Organization
References
Verma V, Simone CB 2nd, Krishnan S, Lin SH, Yang J, Hahn SM (2017) The Rise of Radiomics and Implications for Oncologic Management. J Natl Cancer Inst 109(7). https://doi.org/10.1093/jnci/djx055
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: Images Are More than Pictures, They Are Data. Radiology 278(2):563–577
Narang S, Lehrer M, Yang D, Lee J, Rao A (2016) Radiomics in glioblastoma: current status, challenges and opportunities. Transl Cancer Res 5(4):383–397
Ellingson BM, Bendszus M, Sorensen AG, Pope WB (2014) Emerging techniques and technologies in brain tumor imaging. Neuro Oncol 16(7):12–23
Ellingson BM (2015) Radiogenomics and imaging phenotypes in glioblastoma: novel observations and correlation with molecular characteristics. Curr Neurol Neurosci Rep 15(1):506
Pérez-Beteta J, Martínez-González A, Molina D et al (2017) Glioblastoma: Does the pretreatment geometry matter? A postcontrast T1 MRI-based study. Eur Radiol 27:1096–1104
Abrol S, Kotrotsou A, Salem A, Zinn PO, Colen RR (2017) Radiomic phenotyping in brain cancer to unravel hidden information in medical images. Top Magn Reson Imaging 26(1):43–53
Cui Y, Tha KK, Teresaka S et al (2016) Prognostic imaging biomarkers in glioblastoma: Development and independent validation on the basis of multiregion and quantitative analysis of MR images. Radiology 278(2):546–553
Pérez-Beteta J, Molina-García D, Ortiz-Alhambra JA et al (2018) Tumor surface regularity at MR imaging predicts survival and response to surgery in patients with glioblastoma. Radiology 288(1):218–225
Cui Y, Ren S, Tha KK, Wu J, Shirato H, Li R (2017) Volume of high-risk intratumoral subregions at multi-parametric MR imaging predicts overall survival and complements molecular analysis of glioblastoma. Eur Radiol 27(9):3583–3592
Kickingereder P, Burth S, Wick A et al (2016) Radiomic Profiling of Glioblastoma: Identifying an Imaging Predictor of Patient Survival with Improved Performance over Established Clinical and Radiologic Risk Models. Radiology 280(3):880–889
Lao J, Chen Y, Li ZC et al (2017) A Deep Learning-Based Radiomics Model for Prediction of Survival in Glioblastoma Multiforme. Sci Rep 7(1):10353
Wangaryattawanich P, Hatami M, Wang J et al (2015) Multicenter imaging outcomes study of The Cancer Genome Atlas glioblastoma patient cohort: imaging predictors of overall and progression-free survival. Neuro Oncol 17(11):1525–1537
Ingrisch M, Schneider MJ, Nörenberg D et al (2017) Radiomic Analysis Reveals Prognostic Information in T1-Weighted Baseline Magnetic Resonance Imaging in Patients With Glioblastoma. Invest Radiol 52(6):360–366
Ellingson BM, Harris RJ, Woodworth DC et al (2017) Baseline pretreatment contrast enhancing tumor volume including central necrosis is a prognostic factor in recurrent glioblastoma: evidence from single and multicenter trials. Neuro Oncol 19(1):89–98
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352(10):987–996
Grabowsky MM, Recinos PF, Nowacki AS et al (2014) Residual tumor volume versus extent of resection: predictors of survival after surgery for glioblastoma. J Neurosurg 121:1115–1123
Kuhnt D, Becker A, Ganslandt O, Bauer M, Buchfelder M, Nimsky C (2011) Correlation of the extent of tumor volume resection and patient survival in surgery of glioblastoma multiforme with high-field intraoperative MRI guidance. Neuro Oncol 13(12):1339–1348
Chaichana KL, Jusue-Torres I, Lemos AM et al (2014) The butterfly effect on glioblastoma: is volumetric extent of resection more effective than biopsy for these tumors? J Neurooncol 120(3):625–634
Li YM, Suki D, Hess K, Sawaya R (2016) The influence of maximum safe resection of glioblastoma on survival in 1229 patients: Can we do better than gross-total resection? J Neurosurg 124(4):977–988
Lacroix M, Abi-Said D, Fourney DR et al (2001) A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg 95:109–198
Prior FW, Clark K, Commean P et al (2013) TCIA: an information resource to enable open science. Conf Proc IEEE Eng Med Biol Soc 1282–1285. https://doi.org/10.1109/EMBC.2013.6609742.
Harrell FE Jr, Califf RM, Pryor DB, Lee KL, Rosati RA (1982) Evaluating the yield of medical tests. JAMA 247(1):2543–2546
Cordova JS, Gurbani SS, Holder CA et al (2016) Semi-automated volumetric and morphological assessment of glioblastoma resection with fluorescence-guided surgery. Mol Imaging Biol 18:454–462
Molina D, Pérez-Beteta J, Martínez-González A et al (2017) Lack of robustness of textural measures obtained from 3D brain tumor MRIs impose a need for standardization. PLoS One 12(6):e0178843
Pérez-García VM, Calvo GF, Belmonte-Beitia J, Diego D, Pérez-Romasanta L (2011) Bright solitary waves in malignant gliomas. Phys Rev E Stat Nonlin Soft Matter Phys 84:021921
Anderson AR, Weaver A, Cummings PT, Quaranta V (2006) Tumor morphology and phenotypic evolution driven by selective pressure from the microenvironment. Cell 127:905–915
Martin M (2008) Comparing invasive species to metastatic cancers inspires new insights for modelers. J Natl Cancer Inst 100:88
Henker C, Kriesen T, Glass Ä, Schneider B, Piek J (2017) Volumetric quantification of glioblastoma: experiences with different measurement techniques and impact on survival. J Neurooncol 135:391–402
Gittleman H, Lim D, Kattan MW et al (2017) An independently validated nomogram for individualized estimation of survival among patients with newly diagnosed glioblastoma: NRG Oncology RTOG 0525 and 0825. Neuro Oncol 19(5):669–677
Chung C (2015) Imaging biomarkers in preclinical studies on brain tumors. In: Preedy V, Patel V (eds) Biomarkers in cancer. Biomarkers in disease: methods, discoveries and applications. Springer, Dordrecht
Yip SS, Aerts HJ (2016) Applications and limitations of radiomics. Phys Med Biol 61(13):R150–R166
Grossmann P, Gutman DA, Dunn WD Jr, Holder CA, Aerts HJ (2016) Imaging-genomics reveals driving pathways of MRI derived volumetric tumor phenotype features in Glioblastoma. BMC Cancer 16:611
Acknowledgements
We would like to thank C. López (Radiology Department, Hospital General de Ciudad Real), M. Claramonte (Neurosurgery Department, Hospital General de Ciudad Real), L. Iglesias (Neurosurgery Department, Hospital Clínico San Carlos), J. Avecillas (Radiology Department, Hospital Clínico San Carlos), J. M. Villanueva (Medical Oncology Department, Hospital Universitario de Salamanca), and J. C. Paniagua (Medical Oncology Department, Hospital Universitario de Salamanca) for their help in the data collection. We would also like to thank J. A. Ortiz Alhambra (Mathematical Oncology Laboratory) and A. Fernández-Romero (Mathematical Oncology Laboratory) for their help in the tumor segmentation tasks.
Funding
This research has been supported by the Ministerio de Economía y Competitividad/FEDER, Spain (grant number MTM2015-71200-R), and James S. Mc. Donnell Foundation Twenty-First Century Science Initiative in Mathematical and Complex Systems Approaches for Brain Cancer (Collaborative award 220020450).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Victor Manuel Pérez-García, full professor and head of Department of Mathematics at Universidad de Castilla-La Mancha (Spain).
Conflict of interest
The authors declare that they have no conflict of interest.
Statistics and biometry
Complex statistical methods were necessary for this paper. However, Victor M. Pérez-García, Alicia Martínez-González, and David Molina (mathematicians) have significant statistical expertise.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• Retrospective
• Observational
• Multicenter study
Additional information
The original version of this article was revised: The name of Mariano Amo-Salas and the affiliation of Ismael Herruzo were presented incorrectly.
Electronic supplementary material
ESM 1
(DOCX 142 kb)
Rights and permissions
About this article
Cite this article
Pérez-Beteta, J., Molina-García, D., Martínez-González, A. et al. Morphological MRI-based features provide pretreatment survival prediction in glioblastoma. Eur Radiol 29, 1968–1977 (2019). https://doi.org/10.1007/s00330-018-5758-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-018-5758-7