Abstract
Introduction
There is paucity of data on tuberculosis in Indian patients with systemic lupus erythematosus (SLE). We retrospectively studied clinical features and outcome of tuberculosis in SLE.
Methods
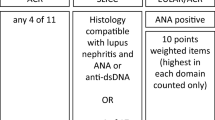
Medical records of patients who developed tuberculosis simultaneous or after the diagnosis of SLE were retrospectively reviewed. All patients fulfilled 1997 ACR and/or SLICC 2012 classification criteria for SLE. A diagnosis of tuberculosis required bacteriological, histopathological or CT/MRI suggestive of tuberculosis and initiation of four drug antituberculous therapy. Baseline parameters were compared with the rest of cohort to identify predictors of tuberculosis.
Results
In our cohort of 1335 SLE patients, 48 (3.6%) developed tuberculosis. Incidence of tuberculosis was calculated to be 733 per 100,000 patient years and occurred after a mean disease duration of 3.0 ± 4.1 years. Extrapulmonary tuberculosis (n = 37) was commoner than pulmonary tuberculosis (n =11). Most common radiological pattern in pulmonary tuberculosis was miliary and musculoskeletal TB was most common extrapulmonary TB. A microbiological diagnosis was obtained in 52.1% patients. Male gender was associated with higher risk of tuberculosis [OR 3.30 (1.55-7.05)]. Mortality was 14.5% and all patients who died had either disseminated (n = 5) or central nervous system (CNS) tuberculosis (n = 2).
Conclusion
Incidence of tuberculosis in SLE is higher than general population and is associated with different phenotype and higher mortality. Male gender was associated with increased risk of tuberculosis in SLE.

Similar content being viewed by others
References
Urowitz MB, Bookman AA, Koehler BE, Gordon DA, Smythe HA, Ogryzlo MA (1976) The bimodal mortality pattern of systemic lupus erythematosus—the American journal of medicine. Am J Med 60:221–225
Mok CC, Kwok CL, Ho LY, Chan PT, Yip SF (2011) Life expectancy, standardized mortality ratios, and causes of death in six rheumatic diseases in Hong Kong. China Arthritis Rheum 63:1182–1189
Yurkovich M, Vostretsova K, Chen W, Aviña-Zubieta JA (2014) Overall and cause-specific mortality in patients with systemic lupus erythematosus: a meta-analysis of observational studies. Arthritis Care Res 66:608–616
Yang Y, Thumboo J, Tan BH, Tan TT, Fong CHJ, Ng HS et al (2017) The risk of tuberculosis in SLE patients from an Asian tertiary hospital. Rheumatol Int 37:1027–1033
Ramagopalan SV, Goldacre R, Skingsley A, Conlon C, Goldacre MJ (2013) Associations between selected immune-mediated diseases and tuberculosis: record-linkage studies. BMC Med 11:97
Doaty S, Agrawal H, Bauer E, Furst DE (2016) Infection and lupus: which causes which? Curr Rheumatol Rep 18:13
Sathiyamoorthy R, Kalaivani M, Aggarwal P, Gupta SK (2020) Prevalence of pulmonary tuberculosis in India: a systematic review and meta-analysis. Lung India 37:45–52
Ribeiro FM, Szyper-Kravitz M, Klumb EM et al (2010) Can lupus flares be associated with tuberculosis infection? Clin Rev Allergy Immunol 38:163–168
Cheng CF, Huang YM, Lu CH, Hsieh SC, Li KJ (2019) Prednisolone dose during treatment of tuberculosis might be a risk factor for mortality in patients with systemic lupus erythematosus: a hospital-based cohort study. Lupus 28:1699–1704
Victorio-Navarra ST, Dy EE, Arroyo CG, Torralba TP (1996) Tuberculosis among Filipino patients with systemic lupus erythematosus. Semin Arthritis Rheum 26:628–634
Prabu V, Agrawal S (2010) Systemic lupus erythematosus and tuberculosis: a review of complex interactions of complicated diseases. J Postgrad Med 56:244–250
tbfacts.org [Internet]. available from https://tbfacts.org/tb-statistics-india/. Accessed 21 May 2021
González-Naranjo LA, Coral-Enríquez JA, Restrepo-Escobar M et al (2020) Factors associated with active tuberculosis in Colombian patients with systemic lupus erythematosus: a case-control study. Clin Rheumatol 40:181–191
Rajadhyaksha AG, Jobanputra K (2020) Infections in systemic lupus erythematosus. J Assoc Physicians India 68:18–21
Cheng CF, Huang YM, Lu CH, Hsieh SC, Li KJ (2019) Prednisolone dose during treatment of tuberculosis might be a risk factor for mortality in patients with systemic lupus erythematosus: a hospital-based cohort study. Lupus 28:1699–1704
Greenstein L, Makan K, Tikly M (2019) Burden of comorbidities in South Africans with systemic lupus erythematosus. Clin Rheumatol 38:2077–2082
Lao M, Chen D, Wu X, Chen H, Qiu Q, Yang X, Zhan Z (2019) Active tuberculosis in patients with systemic lupus erythematosus from Southern China: a retrospective study. Clin Rheumatol 38:535–543
Yang Y, Thumboo J, Tan BH et al (2017) The risk of tuberculosis in SLE patients from an Asian tertiary hospital. Rheumatol Int 37:1027–1033
Wang J, Pan HF, Su H, Li XP, Xu JH, Ye DQ (2009) Tuberculosis in systemic lupus erythematosus in Chinese patients. Trop Doct 39:165–167
Chu AD, Polesky AH, Bhatia G, Bush TM (2009) Active and latent tuberculosis in patients with systemic lupus erythematosus living in the United States. J Clin Rheumatol 15:226–229
Hou CL, Tsai YC, Chen LC, Huang JL (2008) Tuberculosis infection in patients with systemic lupus erythematosus: pulmonary and extra-pulmonary infection compared. Clin Rheumatol 27:557–563
Erdozain JG, Ruiz-Irastorza G, Egurbide MV, Martinez-Berriotxoa A, Aguirre C (2006) High risk of tuberculosis in systemic lupus erythematosus? Lupus 15:232–235
Sayarlioglu M, Inanc M, Kamali S, Cefle A, Karaman O, Gul A, Ocal L, Aral O, Konice M (2004) Tuberculosis in Turkish patients with systemic lupus erythematosus: increased frequency of extrapulmonary localization. Lupus 13:274–278
Tam LS, Li EK, Wong SM, Szeto CC (2002) Risk factors and clinical features for tuberculosis among patients with systemic lupus erythematosus in Hong Kong. Scand J Rheumatol 31:296–300
Shyam C, Malaviya AN (1996) Infection-related morbidity in systemic lupus erythematosus: a clinico-epidemiological study from northern India. Rheumatol Int 16:1–3
Feng PH, Tan TH (1982) Tuberculosis in patients with systemic lupus erythematosus. Ann Rheum Dis 41:11–14
Sharma SK, Mohan A (2004) Extrapulmonary tuberculosis. Indian J Med Res 120:316–353
Torres-González P, Romero-Díaz J, Cervera-Hernández ME et al (2018) Tuberculosis and systemic lupus erythematosus: a case-control study in Mexico City. Clin Rheumatol 37:2095–2102
Hussain SF, Irfan M, Abbasi M et al (2004) Clinical characteristics of 110 miliary tuberculosis patients from a low HIV prevalence country. Int J Tuberc Lung Dis 8:493–499
Natsis K, Grammatikopoulou D, Kokkinos P, Fouka E, Totlis T (2017) Isolated tuberculous arthritis of the ankle: a case report and review of the literature. Hippokratia 21:97–100
Ryu YJ (2015) Diagnosis of pulmonary tuberculosis: recent advances and diagnostic algorithms. Tuberc Respir Dis (Seoul) 78:64–71
Atashi S, Izadi B, Jalilian S, Madani SH, Farahani A, Mohajeri P (2017) Evaluation of GeneXpert MTB/RIF for determination of rifampicin resistance among new tuberculosis cases in west and northwest Iran. New Microbes New Infect 19:117–120
Masenga SK, Mubila H, Hamooya BM (2017) Rifampicin resistance in mycobacterium tuberculosis patients using GeneXpert at Livingstone Central Hospital for the year 2015: a cross sectional explorative study. BMC Infect Dis 17:640
Goyal V, Kadam V, Narang P, Singh V (2017) Prevalence of drug-resistant pulmonary tuberculosis in India: systematic review and meta-analysis. BMC Public Health 17:817
Saha A, Shanthi FXM, Winston AB, Das S et al (2016) Prevalence of hepatotoxicity from antituberculosis therapy: a five year experience from South India. J Prim Care Community Health 7:171–174
Huddart S, Svadzian A, Nafade V et al (2020) Tuberculosis case fatality in India: a systematic review and meta-analysis. BMJ Glob Health 5:e002080. https://doi.org/10.1136/bmjgh-2019-002080
Cheng VC, Ho PL, Lee RA et al (2002) Clinical spectrum of paradoxical deterioration during antituberculosis therapy in non-HIV-infected patients. Eur J Clin Microbiol Infect Dis 21:803–809
Author information
Authors and Affiliations
Contributions
All authors contributed to the data. HM, AJ, RC, SSP, NR, HK extracted the data from records. HM and AJ wrote the first draft. SSP, RC, NR, HK modified the draft further. All authors approved the final version of the manuscript, take responsibility for the content of the entire manuscript, and affirm that any queries related to any aspect of the same are appropriately managed.
Corresponding author
Ethics declarations
Conflicts of interest
The author declares that they have no conflicts of interest.
Ethical approval
The study was cleared by institute ethics committee. As this was a retrospective review of data, the requirement of patient consent was waived off by the committee (IEC Number-2020–148-IP-EXP-21).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Muhammed, H., Jain, A., Pattanaik, S.S. et al. Clinical spectrum of active tuberculosis in patients with systemic lupus erythematosus. Rheumatol Int 41, 2185–2193 (2021). https://doi.org/10.1007/s00296-021-04933-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-021-04933-0