Abstract
Background
Recent literature highlights anomalous cranial nerves in the sinonasal region, notably in the sphenoid and maxillary sinuses, linked to anatomical factors. However, data on the suspended infraorbital canal (IOC) variant is scarce in cross-sectional imaging. Anatomical variations in the sphenoid sinuses, including optic, maxillary, and vidian nerves, raise interest among specialists involved in advanced sinonasal procedures. The infraorbital nerve’s (ION) course along the orbital floor and its abnormal positioning within the orbital and maxillary sinus region pose risks of iatrogenic complications. A comprehensive radiological assessment is crucial before sinonasal surgeries. Cone-beam computed tomography (CBCT) is preferred for its spatial resolution and reduced radiation exposure.
Objective
The aim of this study was to describe the prevalence of anatomical variants of the infraorbital canal (IOC) and report its association with clinical condition or surgical implication.
Methods
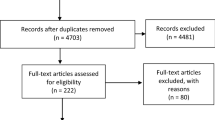
We searched Medline, Scopus, Web of Science, Google Scholar, CINAHL, and LILACS databases from their inception up to June 2023. Two authors independently performed the search, study selection, data extraction, and assessed the methodological quality with assurance tool for anatomical studies (AQUA). Finally, the pooled prevalence was estimated using a random effects model.
Results
Preliminary results show that three types are prevalent, type 1: the IOC does not bulge into the maxillary sinus (MS); therefore, the infraorbital foramen through the anterior wall of MS could be used for identification of the ION. Type 2: the IOC divided the orbital floor into medial and lateral aspects. Type 3: the IOC hangs in the MS and the entire orbital floor lying above the IOC. From which the clinical implications where mainly surgical, in type 1 the infraorbital foramen through the anterior wall of MS could be used for identification of the ION, while in type 2, since the lateral orbital floor could not be directly accessed an inferiorly transposition of ION is helpful to expose the lateral orbital wall directly with a 0 scope; or using angled endoscopes and instruments, however, the authors opinion is that direct exposure potentially facilitates the visualization and management in complex situations such as residual or recurrent mass, foreign body, and fracture located at the lateral aspect of the canal. Lastly, in type 3, the ION it’s easily exposed with a 0° scope.
Conclusions
This systematic review identified four IOC variants: Type 1, within or below the MS roof; Type 2, partially protruding into the sinus; Type 3, fully protruding into the sinus or suspended from the roof; and Type 4, in the orbital floor. Clinical recommendations aim to prevent nerve injuries and enhance preoperative assessments. However, the lack of consistent statistical methods limits robust associations between IOC variants and clinical outcomes. Data heterogeneity and the absence of standardized reporting impede meta-analysis. Future research should prioritize detailed reporting, objective measurements, and statistical approaches for a comprehensive understanding of IOC variants and their clinical implications.
Open Science Framework (OSF): https://doi.org/10.17605/OSF.IO/UGYFZ.





Similar content being viewed by others
Data availability
Not applicable.
References
Açar G, Özen KE, Güler İ, Büyükmumcu M (2018) Computed tomography evaluation of the morphometry and variations of the infraorbital canal relating to endoscopic surgery. Braz J Otorhinolaryngol 84(6):713–721. https://doi.org/10.1016/j.bjorl.2017.08.009
Akın V, Kumbul YÇ, Yasan H, Ayyıldız VA, Okur E (2023) Bilateral barotraumatic involvement of the infraorbital nerve with dehiscence and ectopic course: a case report. Turk Arch Otorhinolaryngol 61(3):134–137. https://doi.org/10.4274/tao.2023.2023-3-4
Alfieri A, Jho HD, Schettino R, Tschabitscher M (2003) Endoscopic endonasal approach to the pterygopalatine fossa: anatomic study. Neurosurgery 52(2):374–380. https://doi.org/10.1227/01.neu.0000044562.73763.00
Ali MJ, Murphy J, James CL, Wormald PJ (2015) Perineural squamous cell carcinoma infiltration of infraorbital nerve treated with endoscopic nerve resection up to foramen rotundum. Clin Exp Ophthalmol 43(3):288–290. https://doi.org/10.1111/ceo.12430
Bahşi I, Orhan M, Kervancıoğlu P, Yalçın ED (2019) Morphometric evaluation and surgical implications of the infraorbital groove, canal and foramen on cone-beam computed tomography and a review of literature. Folia Morphol 78(2):331–343. https://doi.org/10.5603/FM.a2018.0084
Cârstocea L, Rusu MC, Pascale C, Săndulescu M (2020) Three-dimensional anatomy of the transantral intraseptal infraorbital canal with the use of cone-beam computed tomography. Folia Morphol 79(3):649–653. https://doi.org/10.5603/FM.a2019.0109
Chi MJ, Ku M, Shin KH, Baek S (2010) An analysis of 733 surgically treated blowout fractures. Ophthalmologica. Journal International D‘ophtalmologie. Int J Ophthalmol. Zeitschrift fur Augenheilkunde 224(3):167–175. https://doi.org/10.1159/000238932
Cho RI, Kahana A (2021) Embryology of the orbit. J Neurol Surg B Skull Base 82(1):2–6. https://doi.org/10.1055/s-0040-1722630
Eiid SB, Mohamed AA (2022) Protrusion of the infraorbital canal into the maxillary sinus: a cross-sectional study in Cairo. Egypt Imaging Sci Dent 52(4):359–364. https://doi.org/10.5624/isd.20220077
Elhadi AM, Zaidi HA, Yagmurlu K, Ahmed S, Rhoton AL Jr, Nakaji P, Preul MC, Little AS (2016) Infraorbital nerve: a surgically relevant landmark for the pterygopalatine fossa, cavernous sinus, and anterolateral skull base in endoscopic transmaxillary approaches. J Neurosurg 125(6):1460–1468. https://doi.org/10.3171/2015.9.JNS151099
Farina D, Lombardi D, Bertuletti M, Palumbo G, Zorza I, Ravanelli M (2019) An additional challenge for head and neck radiologists: anatomic variants posing a surgical risk—a pictorial review. Insights Imaging 10(1):112. https://doi.org/10.1186/s13244-019-0794-7
Ference EH, Smith SS, Conley D, Chandra RK (2015) Surgical anatomy and variations of the infraorbital nerve. Laryngoscope 125(6):1296–1300. https://doi.org/10.1002/lary.25089
Fontolliet M, Bornstein MM, von Arx T (2019) Characteristics and dimensions of the infraorbital canal: a radiographic analysis using cone beam computed tomography (CBCT). Surg Radiol Anat SRA 41(2):169–179. https://doi.org/10.1007/s00276-018-2108-z
Haghnegahdar A, Khojastepour L, Naderi A (2018) Evaluation of infraorbital canal in cone beam computed tomography of maxillary sinus. J Dent 19(1):41–47
Har-El G (2005) Combined endoscopic transmaxillary-transnasal approach to the pterygoid region, lateral sphenoid sinus, and retrobulbar orbit. Ann Otol Rhinol Laryngol 114(6):439–442. https://doi.org/10.1177/000348940511400605
He S, Bakst RL, Guo T, Sun J (2015) A combination of modified transnasal endoscopic maxillectomy via transnasal prelacrimal recess approach with or without radiotherapy for selected sinonasal malignancies. Eur Arch Otorhinolaryngol 272(10):2933–2938. https://doi.org/10.1007/s00405-014-3248-3
Henry BM, Tomaszewski KA, Walocha JA (2016) Methods of evidence-based anatomy: a guide to conducting systematic reviews and meta-analysis of anatomical studies. Ann Anat 205:16–21. https://doi.org/10.1016/j.aanat.2015.12.002
Herman P, Lot G, Silhouette B, Marianowski R, Portier F, Wassef M, Huy PT (1999) Transnasal endoscopic removal of an orbital cavernoma. Ann Otol Rhinol Laryngol 108(2):147–150. https://doi.org/10.1177/000348949910800208
Hwang K, You SH, Sohn IA (2009) Analysis of orbital bone fractures: a 12-year study of 391 patients. J Craniofac Surg 20(4):1218–1223. https://doi.org/10.1097/SCS.0b013e3181acde01
Hwang K, Kim JH, Kang YH (2014) Orbital hematoma caused by bleeding from orbital branch of the infraorbital artery after reconstruction of an orbital fracture. J Craniofac Surg 25(2):375–376. https://doi.org/10.1097/SCS.0000000000000637
Ikeda K, Oshima T, Suzuki H, Kikuchi T, Suzuki M, Kobayashi T (2003) Surgical treatment of subperiosteal abscess of the orbit: Sendai’s ten-year experience. Auris Nasus Larynx 30(3):259–262. https://doi.org/10.1016/s0385-8146(03)00060-9
Kalabalık F, Aktaş T, Akan E, Aytuğar E (2020) Radiographic evaluation of infraorbital canal protrusion into maxillary sinus using cone-beam computed tomography. J Oral Maxillofac Res 11(4):e5. https://doi.org/10.5037/jomr.2020.11405
Kasemsiri P, Solares CA, Carrau RL, Prosser JD, Prevedello DM, Otto BA, Old M, Kassam AB (2013) Endoscopic endonasal transpterygoid approaches: anatomical landmarks for planning the surgical corridor. Laryngoscope 123(4):811–815. https://doi.org/10.1002/lary.23697
Kazkayasi M, Ergin A, Ersoy M, Bengi O, Tekdemir I, Elhan A (2001) Certain anatomical relations and the precise morphometry of the infraorbital foramen–canal and groove: an anatomical and cephalometric study. Laryngoscope 111(4 Pt 1):609–614. https://doi.org/10.1097/00005537-200104000-00010
Kennedy DW, Goodstein ML, Miller NR, Zinreich SJ (1990) Endoscopic transnasal orbital decompression. Arch Otolaryngol Head Neck Surg 116(3):275–282. https://doi.org/10.1001/archotol.1990.01870030039006
Kim JK, Yang SK, Shin DB, Nam JG (2015) Dehiscence of the infraorbital canal with the maxillary antral empyema: a new cause of facial pain. J Craniofac Surg 26(3):e227–e229. https://doi.org/10.1097/SCS.0000000000001479
Kirby EJ, Turner JB, Davenport DL, Vasconez HC (2011) Orbital floor fractures: outcomes of reconstruction. Ann Plast Surg 66(5):508–512. https://doi.org/10.1097/SAP.0b013e31820b3c7a
Lantos JE, Pearlman AN, Gupta A, Chazen JL, Zimmerman RD, Shatzkes DR, Phillips CD (2016) Protrusion of the infraorbital nerve into the maxillary sinus on CT: prevalence, proposed grading method, and suggested clinical implications. AJNR Am J Neuroradiol 37(2):349–353. https://doi.org/10.3174/ajnr.A4588
Lawrence JE, Poole MD (1992) Mid-facial sensation following craniofacial surgery. Br J Plast Surg 45(7):519–522. https://doi.org/10.1016/0007-1226(92)90146-o
Lee UY, Nam SH, Han SH, Choi KN, Kim TJ (2006) Morphological characteristics of the infraorbital foramen and infraorbital canal using three-dimensional models. Surg Radiol Anat SRA 28(2):115–120. https://doi.org/10.1007/s00276-005-0071-y
Li L, London NR Jr, Prevedello DM, Carrau RL (2020) Anatomical variants of the infraorbital canal: implications for the prelacrimal approach to the orbital floor. Am J Rhinol Allergy 34(2):176–182. https://doi.org/10.1177/1945892419882127
Lyson T, Sieskiewicz A, Rogowski M, Mariak Z (2015) The transmaxillary endoscopic approach to the inferior part of the orbit: how I do it. Acta Neurochir 157(4):625–628. https://doi.org/10.1007/s00701-015-2359-y
Michel O (2000). Transnasale Chirurgie der Orbita.Ubersicht aktueller Indikationen und Techniken [Transnasal surgery of the orbita. Rev Curr Indic Tech]. HNO 48(1):4–17. https://doi.org/10.1007/s001060050002
Nam Y, Bahk S, Eo S (2017) Anatomical study of the infraorbital nerve and surrounding structures for the surgery of orbital floor fractures. J Craniofac Surg 28(4):1099–1104. https://doi.org/10.1097/SCS.0000000000003416
Olenczak JB, Hui-Chou HG, Aguila DJ 3rd, Shaeffer CA, Dellon AL, Manson PN (2015) Posttraumatic midface pain: clinical significance of the anterior superior alveolar nerve and canalis sinuosus. Ann Plast Surg 75(5):543–547. https://doi.org/10.1097/SAP.0000000000000335
Orhan K, Misirli M, Aksoy S, Seki U, Hincal E, Ormeci T, Arslan A (2016) Morphometric analysis of the infraorbital foramen, canal and groove using cone beam CT: considerations for creating artificial organs. Int J Artif Organs 39(1):28–36. https://doi.org/10.5301/ijao.5000469
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA et al (2021). The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ (Clinical research ed.) 372:n71. https://doi.org/10.1136/bmj.n71
Papadopoulou AM, Chrysikos D, Samolis A, Tsakotos G, Troupis T (2021) Anatomical variations of the nasal cavities and paranasal sinuses: a systematic review. Cureus 13(1):e12727. https://doi.org/10.7759/cureus.12727
Przygocka A, Szymański J, Jakubczyk E, Jędrzejewski K, Topol M, Polguj M (2013) Variations in the topography of the infraorbital canal/groove complex: a proposal for classification and its potential usefulness in orbital floor surgery. Folia Morphol 72(4):311–317. https://doi.org/10.5603/fm.2013.0052
Rusu MC, Săndulescu M, Ilie OC (2015) Infraorbital canal bilaterally replaced by a lateroantral canal. Surg Radiol Anat 37(9):1149–1153. https://doi.org/10.1007/s00276-015-1468-x
Sadler TW, Langman J (2019). Langman embriología médica, 14th edn. Wolters Kluwer
Salzano G, Turri-Zanoni M, Karligkiotis A, Zocchi J, Dell’Aversana Orabona G, Califano L, Battaglia P, Castelnuovo P (2017) Infraorbital nerve transposition to expand the endoscopic transnasal maxillectomy. Int Forum Allergy Rhinol 7(2):149–153. https://doi.org/10.1002/alr.21858
Schultheiß S, Petridis AK, El Habony R, Maurer P, Scholz M (2013) The transmaxillary endoscopic approach to the orbit. Acta Neurochir 155(1):87–97. https://doi.org/10.1007/s00701-012-1525-8
Shin KJ, Lee SH, Park MG, Shin HJ, Lee AG (2020) Location of the accessory infraorbital foramen with reference to external landmarks and its clinical implications. Sci Rep 10(1):8566. https://doi.org/10.1038/s41598-020-65330-4
Sieśkiewicz A, Piszczatowski B, Olszewska E, Lukasiewicz A, Tarasow E, Rogowski M (2014) Minimally invasive transnasal medial maxillectomy for treatment of maxillary sinus and orbital pathologies. Acta Otolaryngol 134(3):290–295. https://doi.org/10.3109/00016489.2013.857786
Singh A, Manjunath K, Singh H (2022) Relationship of sphenoid sinus to adjacent structures in South India: a retrospective cross sectional study. Egypt J Otolaryngol 38(1). https://doi.org/10.1186/s43163-021-00191-w
Tawfik HA, Dutton JJ (2018) Embryologic and fetal development of the human orbit. Ophthalmic Plast Reconstr Surg 34(5):405–421. https://doi.org/10.1097/iop.0000000000001172
Yenigun A, Gun C, Uysal II, Nayman A (2016) Radiological classification of the infraorbital canal and correlation with variants of neighboring structures. Eur Arch Otorhinolaryngol 273(1):139–144. https://doi.org/10.1007/s00405-015-3550-8
Yesilova E, Bayrakdar IS (2018) The appearance of the infraorbital canal and infraorbital ethmoid (Haller’s) cells on panoramic radiography of edentulous patients. Biomed Res Int 2018:1293124. https://doi.org/10.1155/2018/1293124
Zhou B, Han DM, Cui SJ, Huang Q, Wang CS (2013) Intranasal endoscopic prelacrimal recess approach to maxillary sinus. Chin Med J 126(7):1276–1280
Funding
No funding has been received to make up this review.
Author information
Authors and Affiliations
Contributions
MO: Protocol/project development MO, AF, DR, PA: Data collection or management MO, AF, DR, PA, JV: Data analysis MO, AF, DR, JV, JS, PN: Manuscript writing/editing JS, MK: Other (Translation)
Corresponding author
Ethics declarations
Conflit of interests
The authors declare no competing interests.
Ethical approval
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Orellana-Donoso, M., Romero-Zucchino, D., Fuentes-Abarca, A. et al. Infraorbital canal variants and its clinical and surgical implications. A systematic review. Surg Radiol Anat (2024). https://doi.org/10.1007/s00276-024-03348-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00276-024-03348-3