Abstract
Purpose
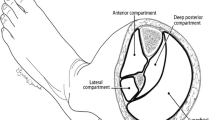
Skin closure disorders in ankle surgery are a recurrent problem not only in traumatology but also in elective surgery. The aim of the study was to describe the anatomical basis of the fasciocutaneous vascularization of the lateral malleolus region to develop a posterior cover flap for the region.
Methods
We dissected ten fresh frozen specimens after arterial injection of an Indian ink preparation and individualized the perforating arteries. Their positions and diameters were collated. Then, the surgical technique was clinically applied for two different cases by transferring the fasciocutaneous flap posterior to the lateral malleolus to cover a loss of skin substance.
Results
There were in average 5 fibular perforators over the last 100 mm of the fibula. The average diameter of the first two perforating arteries was 0.6 ± 0.12 mm and 0.9 ± 0.25 mm, respectively, and the consistency of the latter makes it possible to produce a skin flap with anterior translation. This is an axial flap. Two patients were operated on using this technique. There was no necrosis of the posterior fibular flap and healing was achieved by the third post-operative week.
Conclusion
This study showed the presence of fibular perforating arteries with a high reproducibility of their dissection. This anatomical description served as the basis for the description of a new distal fibular perforating flap.






Similar content being viewed by others
References
Angelis S, Apostolopoulos A, Kosmas L, Balfousias T, Papanikolaou A (2020) The use of vacuum closure-assisted device in the management of compound lower limb fractures with massive soft tissue damage. Cureus 11:e5104. https://doi.org/10.7759/cureus.5104
Bekara F, Herlin C, Somda S, De Runz A, Grolleau J, Chaput B (2018) Free versus perforator-pedicled propeller flaps in lower extremity reconstruction: what is the safest coverage? A meta-analysis. Microsurgery 38:109–119. https://doi.org/10.1002/micr.30047
Bhattacharyya T, Mehta P, Smith M, Pomahac B (2008) Routine use of wound vacuum-assisted closure does not allow coverage delay for open tibia fractures. Plast Reconstr Surg 12:1263–1266. https://doi.org/10.1097/01.prs.0000305536.09242.a6
Costa M, Achten J, Bruce J, Davis S, Hennings S, Willett K et al (2018) Negative-pressure wound therapy versus standard dressings for adults with an open lower limb fracture: the WOLLF RCT. Health Technol Assess Winch Engl 22:1–162. https://doi.org/10.3310/hta22730
Demiri E, Tsimponis A, Pavlidis L, Spyropoulou G, Foroglou P, Dionyssiou D (2020) Reverse neurocutaneous vs propeller perforator flaps in diabetic foot reconstruction. Injury 51:S16–S21. https://doi.org/10.1016/j.injury.2020.03.014
Fisher N, Atanda A, Swensen S, Egol K (2017) Repair of bimalleolar ankle fracture. J Orthop Trauma 31:S14–S15. https://doi.org/10.1097/BOT.0000000000000893
Gaillard J, Bourcheix L, Masquelet A (2018) Perforators of the fibular artery and suprafascial network. Surg Radiol Anat 40:927–933. https://doi.org/10.1007/s00276-017-1927-7
Hamdi M, Khlifi A (2012) Lateral supramalleolar flap for coverage of ankle and foot defects in children. J Foot Ankle Surg 51:106–109. https://doi.org/10.1053/j.jfas.2011.10.014
Henry B, Vikse J, Pekala P, Loukas M, Tubbs S, Walocha J et al (2018) Consensus guidelines for the uniform reporting of study ethics in anatomical research within the framework of the anatomical quality assurance (AQUA) checklist. Clin Anat 31:521–524. https://doi.org/10.1002/ca.23069
Herlin C, Sinna R, Hamoui M, Canovas F, Captier G, Chaput B (2017) Distal lower extremity coverage by distally based sural flaps: methods to increase their vascular reliability. Ann Chir Plast Esthet 62:45–54
Hifny M, Tohamy A, Rabie O, Ali A (2020) Propeller perforator flaps for coverage of soft tissue defects in the middle and distal lower extremities. Ann Chir Plast Esthet 65:54–60
Iheozor-Ejiofor Z, Newton K, Dumville J, Costa M, Norman G, Bruce J (2018) Negative pressure wound therapy for open traumatic wounds. Cochrane Database Syst Rev 7:012522. https://doi.org/10.1002/14651858.CD012522.pub2
Jakubietz R, Jakubietz M, Gruenert J, Kloss D (2007) The 180-degree perforator-based propeller flap for soft tissue coverage of the distal, lower extremity: a new method to achieve reliable coverage of the distal lower extremity with a local, fasciocutaneous perforator flap. Ann Plast Surg 59:667–671
Kaya B, Feigl G, Kose S, Apaydin N (2022) Cutaneous perforators of the arm and anatomical landmarks for defining the flap donor sites. Surg Radiol Anat 44:1079–1089. https://doi.org/10.1007/s00276-022-02976-x
Kehrer A, Sachanadani N, Da Silva N, Lonic D, Heidekrueger P, Taeger C et al (2019) Step-by-step guide to ultrasound-based design of alt flaps by the microsurgeon—basic and advanced applications and device settings. J Plast Reconstr Aesthet Surg 73:1081–1090. https://doi.org/10.1016/j.bjps.2019.11.035
Kunze K, Hamid K, Lee S, Halvorson J, Earhart J, Bohl D (2020) Negative-pressure wound therapy in foot and ankle surgery. Foot Ankle Int 41:364–372
Liu D, Sofiadellis F, Ashton M, MacGill K, Webb A (2012) Early soft tissue coverage and negative pressure wound therapy optimises patient outcomes in lower limb trauma. Injury 43:772–778. https://doi.org/10.1016/j.injury.2011.09.003
Masquelet A, Beveridge J, Romana C, Gerber C (1988) The lateral supramalleolar flap. Plast Reconstr Surg 81:74–84. https://doi.org/10.1097/00006534-198801000-00014
Masquelet A, Romana M, Wolf G (1992) Skin island flaps supplied by the vascular axis of the sensitive superficial nerves: anatomic study and clinical experience in the leg. Plast Reconstr Surg 89:1115–1121
Mb O, Aksan T, Ertekin C, Tezcan M (2020) Coverage of exposed bone and hardware of the medial malleolus with tibialis posterior artery perforator flap after ankle fracture surgery complications. Int Wound J 17:429–435. https://doi.org/10.1111/iwj.13289
Poulet V, Prevost A, Cavallier Z, Alshehri S, Lauwers F, Lopez R (2022) Fibula free flap perforasomes: vascular anatomical study and clinical applications. Surg Radiol Anat 44:637–644. https://doi.org/10.1007/s00276-022-02953-4
Rong K, Chen C, Hao L, Xu X, Wang Z (2016) Redefining the vascular classifications of the lateral supramalleolar. Ann Plast Surg 77:341–344. https://doi.org/10.1097/SAP.0000000000000576
Scherer S, Pietramaggiori G, Mathews J, Prsa M, Huang S, Orgill D (2008) The mechanism of action of the vacuum-assisted closure device. Plast Reconstr Surg 122:786–797. https://doi.org/10.1097/PRS.0b013e31818237ac
Shibuya N, Davis M, Jupiter D (2014) Epidemiology of foot and ankle fractures in the United States: an analysis of the National Trauma Data Bank (2007 to 2011). J Foot Ankle Surg 53:606–608. https://doi.org/10.1053/j.jfas.2014.03.011
Taylor G, Palmer J (1987) The vascular territories (angiosomes) of the body: experimental study and clinical applications. Br J Plast Surg 40:113–141
Valenti P, Masquelet A, Romana C, Nordin J (1991) Technical refinement of the lateral supramalleolar flap. Br J Plast Surg 44:459–462. https://doi.org/10.1016/0007-1226(91)90207-z
Xiao W, Li K, Kiu-Huen N, Feng S, Zhou H, Nicoli F et al (2020) A prospective comparative study of color Doppler ultrasound and infrared thermography in the detection of perforators for anterolateral thigh flaps. Ann Plast Surg 84:S190–S195. https://doi.org/10.1097/SAP.0000000000002369
Zhang F, Lin S, Song Y, Zhang G, Zheng H (2009) Distally based sural neuro-lesser saphenous veno-fasciocutaneous compound flap with a low rotation point: microdissection and clinical application. Ann Plast Surg 62:395–404
Funding
The authors declare no funding for this study.
Author information
Authors and Affiliations
Contributions
PC: project development, data analysis, manuscript writing. BP: data collection, analysis, and manuscript writing. DE: manuscript editing, data analysis and translation. IO: data collection. FB: manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no direct conflicts of interest with this study. P. Clavert is a member of SRA Board.
Ethics approval
Not Applicable for the anatomical study. For the clinical part of the study, included patients gave informed consent to participate, and the study obtained ethical committee approval to participate, and for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Clavert, P., Puliero, B., Eichler, D. et al. The distal fibular perforating axial flap for lateral malleolus coverage: an anatomical description and surgical technique. Surg Radiol Anat 45, 1191–1196 (2023). https://doi.org/10.1007/s00276-023-03204-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-023-03204-w