Abstract
Background
In recent years, the demand for facial rejuvenation is increasing year by year. This study aims to use bibliometric analysis to construct a visualization map of the facial rejuvenation research and provide the research hotspots and trend frontiers in the field.
Methods
Publications on facial rejuvenation research were extracted from the Web of Science Core Collection database. VOSviewer 1.6.18 was used to analyze the co-authorship, the citations of countries, institutions, and authors, the co-occurrence of keywords, and the journals in which the studies were published.
Results
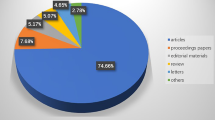
In total, 6,196 records of facial rejuvenation research published between 2000 and 2021 were collected. The USA had published the most publications in this field (2,647), and its main partners were Canada, Germany, and China. University of California, Los Angeles, was the institution with the greatest contribution (127 publications). Plastic and Reconstructive Surgery (623 publications) published the most research in this field and was also the most frequently co-cited journal (17,349 citations, total link strength: 586,955). Rohrich RJ (70 publications) was the most prolific and most frequently co-cited author (1,230 citations, TLS: 26,603). Among the 100 most cited articles, 57 articles are amenable to grading level of evidence, and most papers presented their findings utilizing level IV evidence.
Conclusions
At present, the research hotspots in this field included the following six aspects: facial photoelectric therapy, aging manifestation and treatment in the middle of the face, the application of autologous fat transfer in facial rejuvenation, facial plastic surgery, facial injection cosmetology, and rhytidectomy and related anatomy. According to the analysis of the timing diagram, the research trends were esthetic medicine, mesenchymal stem cells, laser therapy, the application of platelet-rich plasma, and platelet-rich fibrin.
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.









Similar content being viewed by others
References
Ko AC, Korn BS, Kikkawa DO (2017) The aging face. Surv Ophthalmol 62:190–202. https://doi.org/10.1016/j.survophthal.2016.09.002
Mendelson BC, Wong CH (2020) Changes in the facial skeleton with aging: implications and clinical applications in facial rejuvenation. Aesthet Plast Surg 44:1159–1161. https://doi.org/10.1007/s00266-020-01785-0
Swift A, Liew S, Weinkle S et al (2021) The facial aging process from the “inside out.” Aesthet Surg J 41:1107–1119. https://doi.org/10.1093/asj/sjaa339
Yao W, Chen X, Li X et al (2021) Current trends in the anti-photoaging activities and mechanisms of dietary non-starch polysaccharides from natural resources. Crit Rev Food Sci Nutr. https://doi.org/10.1080/10408398.2021.1939263
Coleman SR, Grover R (2006) The anatomy of the aging face: volume loss and changes in 3-dimensional topography. Aesthet Surg J 26:S4-9. https://doi.org/10.1016/j.asj.2005.09.012
Reilly MJ, Tomsic JA, Fernandez SJ et al (2015) Effect of facial rejuvenation surgery on perceived attractiveness, femininity, and personality. JAMA Fac Plast Surg 17:202–207. https://doi.org/10.1001/jamafacial.2015.0158
Kreutz-Rodrigues L, Shapiro D, Mardini S et al (2020) Landmarks in facial rejuvenation surgery: the top 50 most cited articles. Aesthet Surg J 40:NP1–NP7. https://doi.org/10.1093/asj/sjz207
van Eck NJ, Waltman L (2010) Software survey: VOSviewer, a computer program for bibliometric mapping. Scientometrics 84:523–538. https://doi.org/10.1007/s11192-009-0146-3
Joyce CW, Joyce KM, Sugrue CM et al (2014) Plastic surgery and the breast: a citation analysis of the literature. Plast Reconstr Surg Glob Open 2:e251. https://doi.org/10.1097/GOX.0000000000000202
Anderson RR, Parrish JA (1983) Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science 220:524–527. https://doi.org/10.1126/science.6836297
Britt CJ, Marcus B (2017) Energy-based facial rejuvenation: advances in diagnosis and treatment. JAMA Fac Plast Surg 19:64–71. https://doi.org/10.1001/jamafacial.2016.1435
Goldberg DJ (2003) Lasers for facial rejuvenation. Am J Clin Dermatol 4:225–234. https://doi.org/10.2165/00128071-200304040-00002
Papadavid E, Katsambas A (2003) Lasers for facial rejuvenation: a review. Int J Dermatol 42:480–487. https://doi.org/10.1046/j.1365-4362.2003.01784.x
Langton AK, Sherratt MJ, Griffiths CE et al (2010) A new wrinkle on old skin: the role of elastic fibres in skin ageing. Int J Cosmet Sci 32:330–339. https://doi.org/10.1111/j.1468-2494.2010.00574.x
Hirmand H (2010) Anatomy and nonsurgical correction of the tear trough deformity. Plast Reconstr Surg 125:699–708. https://doi.org/10.1097/PRS.0b013e3181c82f90
Coleman SR (1995) Long-term survival of fat transplants: controlled demonstrations. Aesthetic Plast Surg 19:421–425. https://doi.org/10.1007/BF00453875
Venkataram J (2008) Tumescent liposuction: a review. J Cutan Aesthet Surg 1:49–57. https://doi.org/10.4103/0974-2077.44159
Suh A, Pham A, Cress MJ et al (2019) Adipose-derived cellular and cell-derived regenerative therapies in dermatology and aesthetic rejuvenation. Ageing Res Rev 54:100933. https://doi.org/10.1016/j.arr.2019.100933
Isse NG (1994) Endoscopic facial rejuvenation: endoforehead, the functional lift. Case reports. Aesthetic Plast Surg 18:21–29. https://doi.org/10.1007/BF00444243
Drolet BC, Phillips BZ, Hoy EA et al (2014) Finesse in forehead and brow rejuvenation: modern concepts, including endoscopic methods. Plast Reconstr Surg 134:1141–1150. https://doi.org/10.1097/PRS.0000000000000756
Patrocinio LG, Patrocinio TG, Patrocinio JA (2013) Subperiosteal midface-lift. Facial Plast Surg 29:206–213. https://doi.org/10.1055/s-0033-1347000
Bukhari SNA, Roswandi NL, Waqas M et al (2018) Hyaluronic acid, a promising skin rejuvenating biomedicine: a review of recent updates and pre-clinical and clinical investigations on cosmetic and nutricosmetic effects. Int J Biol Macromol 120:1682–1695. https://doi.org/10.1016/j.ijbiomac.2018.09.188
de Maio M, DeBoulle K, Braz A et al (2017) Facial assessment and injection guide for botulinum toxin and injectable hyaluronic acid fillers: focus on the midface. Plast Reconstr Surg 140:540e–550e. https://doi.org/10.1097/PRS.0000000000003716
Sundaram H, Signorini M, Liew S et al (2016) Global aesthetics consensus: botulinum toxin type A-evidence-based review, emerging concepts, and consensus recommendations for aesthetic use, including updates on complications. Plast Reconstr Surg 137:518e–529e. https://doi.org/10.1097/01.prs.0000475758.63709.23
Pedroza F, Iniguez-Cuadra R, Chavez-Franco L et al (2016) Rhytidoplasty: SMAS imbrication vector comparison. Facial Plast Surg 32:599–606. https://doi.org/10.1055/s-0036-1597145
Hamra ST (1990) The deep-plane rhytidectomy. Plast Reconstr Surg 86:53–61; discussion 62–63
Hoefflin SM (1992) Decreasing prolonged swelling and pain associated with deep plane face lifts. Plast Reconstr Surg 90:1125. https://doi.org/10.1097/00006534-199212000-00047
Torsello F, Mirigliani L, D’Alessio R et al (2010) Do the neoclassical canons still describe the beauty of faces? An anthropometric study on 50 Caucasian models. Prog Orthod 11:13–19. https://doi.org/10.1016/j.pio.2010.04.003
Kanavakis G, Halazonetis D, Katsaros C et al (2021) Facial shape affects self-perceived facial attractiveness. PLoS ONE 16:e0245557. https://doi.org/10.1371/journal.pone.0245557
Daar AS, Greenwood HL (2007) A proposed definition of regenerative medicine. J Tissue Eng Regen Med 1:179–184. https://doi.org/10.1002/term.20
Bacakova L, Zarubova J, Travnickova M et al (2018) Stem cells: their source, potency and use in regenerative therapies with focus on adipose-derived stem cells—a review. Biotechnol Adv 36:1111–1126. https://doi.org/10.1016/j.biotechadv.2018.03.011
Ozpur MA, Guneren E, Canter HI et al (2016) Generation of skin tissue using adipose tissue-derived stem cells. Plast Reconstr Surg 137:134–143. https://doi.org/10.1097/PRS.0000000000001927
Krawczenko A, Klimczak A (2022) Adipose tissue-derived mesenchymal stem/stromal cells and their contribution to angiogenic processes in tissue regeneration. Int J Mol Sci. https://doi.org/10.3390/ijms23052425
Kolle SF, Fischer-Nielsen A, Mathiasen AB et al (2013) Enrichment of autologous fat grafts with ex-vivo expanded adipose tissue-derived stem cells for graft survival: a randomised placebo-controlled trial. Lancet 382:1113–1120. https://doi.org/10.1016/S0140-6736(13)61410-5
Xu Y, Guo S, Wei C et al (2016) The comparison of adipose stem cell and placental stem cell in secretion characteristics and in facial antiaging. Stem Cells Int. https://doi.org/10.1155/2016/7315830
Fleming D (1999) Controversies in skin resurfacing: the role of erbium. J Cutan Laser Ther 1:15–21. https://doi.org/10.1080/14628839950517048
Manstein D, Herron GS, Sink RK et al (2004) Fractional photothermolysis: a new concept for cutaneous remodeling using microscopic patterns of thermal injury. Lasers Surg Med 34:426–438. https://doi.org/10.1002/lsm.20048
Alexiades-Armenakas MR, Dover JS, Arndt KA (2008) The spectrum of laser skin resurfacing: nonablative, fractional, and ablative laser resurfacing. J Am Acad Dermatol 58:719–737. https://doi.org/10.1016/j.jaad.2008.01.003
Firooz A, Rajabi-Estarabadi A, Nassiri-Kashani MH (2016) Treatment of atrophic facial acne scars with fractional Er:YAG laser in skin phototype III-IV: A pilot study. J Cosmet Laser Ther 18:204–207. https://doi.org/10.3109/14764172.2016.1157354
Khatri KA, Mahoney D, Hakam L (2012) High-fluence fractional treatment of photodamaged facial skin using a 2940 nm erbium:yttrium-aluminum-garnet laser. J Cosmet Laser Ther 14:260–266. https://doi.org/10.3109/14764172.2012.738911
Lee HM, Haw S, Kim JE et al (2012) A fractional 2940 nm short-pulsed, erbium-doped yttrium aluminium garnet laser is effective and minimally invasive for the treatment of photodamaged skin in Asians. J Cosmet Laser Ther 14:253–259. https://doi.org/10.3109/14764172.2012.738909
Moon HR, Yun WJ, Lee YJ et al (2015) A prospective, randomized, double-blind comparison of an ablative fractional 2940-nm erbium-doped yttrium aluminum garnet laser with a nonablative fractional 1550-nm erbium-doped glass laser for the treatment of photoaged Asian skin. J Dermatolog Treat 26:551–557. https://doi.org/10.3109/09546634.2014.999020
Ozkoca D, Askin O, Engin B (2021) Treatment of periorbital and perioral wrinkles with fractional Er:YAG laser: what are the effects of age, smoking, and Glogau stage? J Cosmet Dermatol 20:2800–2804. https://doi.org/10.1111/jocd.13984
Dadkhahfar S, Fadakar K, Robati RM (2019) Efficacy and safety of long pulse Nd:YAG laser versus fractional erbium:YAG laser in the treatment of facial skin wrinkles. Lasers Med Sci 34:457–464. https://doi.org/10.1007/s10103-018-2614-6
Milanic M, Muc BT, Jezersek M et al (2018) Experimental and numerical assessment of hyperthermic laser lipolysis with 1,064 nm Nd:YAG laser on a porcine fatty tissue model. Lasers Surg Med 50:125–136. https://doi.org/10.1002/lsm.22743
Yim S, Lee YH, Choi YJ et al (2020) Split-face comparison of the picosecond 1064-nm Nd:YAG laser using a microlens array and the quasi-long-pulsed 1064-nm Nd:YAG laser for treatment of photoaging facial wrinkles and pores in Asians. Lasers Med Sci 35:949–956. https://doi.org/10.1007/s10103-019-02906-1
Hong JK, Shin SH, Park SJ et al (2022) A prospective, split-face study comparing 1,064-nm picosecond Nd:YAG laser toning with 1,064-nm Q-switched Nd:YAG laser toning in the treatment of melasma. J Dermatol Treat. https://doi.org/10.1080/09546634.2022.2033674
Ungaksornpairote C, Manuskiatti W, Junsuwan N et al (2020) A prospective, split-face, randomized study comparing picosecond to Q-switched Nd: YAG laser for treatment of epidermal and dermal pigmented lesions in Asians. Dermatol Surg 46:1671–1675. https://doi.org/10.1097/DSS.0000000000002486
Yang H, Guo L, Jia G et al (2021) Treatment of nevus of Ota with 1064 nm picosecond Nd:YAG laser: a retrospective study. Dermatol Ther 34:e15152. https://doi.org/10.1111/dth.15152
Cameli N, Mariano M, Cordone I et al (2017) autologous pure platelet-rich plasma dermal injections for facial skin rejuvenation: clinical, instrumental, and flow cytometry assessment. Dermatol Surg 43:826–835. https://doi.org/10.1097/DSS.0000000000001083
Dohan Ehrenfest DM, Del Corso M, Diss A et al (2010) Three-dimensional architecture and cell composition of a Choukroun’s platelet-rich fibrin clot and membrane. J Periodontol 81:546–555. https://doi.org/10.1902/jop.2009.090531
Funding
This research received no funding from any public or private organizations/institutions.
Author information
Authors and Affiliations
Contributions
Conceptualization was done by JM and CR; investigation was carried out by JM; data curation was done by XZ and BL; the original draft preparation was written by JM; writing, reviewing, and editing were done by CR; and supervision and project administration were done by MZ. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose
Ethics Approval
The Ethics Committee of the Second Affiliation Hospital of Dalian Medical University approved this study.
Human and Animal Rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mao, J., Ri, C., Li, B. et al. Research Hotspots and Emerging Trends of Facial Rejuvenation: A Bibliometric Analysis. Aesth Plast Surg 47, 1039–1058 (2023). https://doi.org/10.1007/s00266-022-03099-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-022-03099-9