Abstract
Background
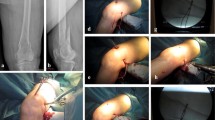
Cementless hemiarthroplasty is a widely used treatment for femoral neck fractures. Intra-operative femoral fracture occasionally occurs during the procedure, and the use of cerclage wire has been proposed to stabilize both the prosthesis and the bone. This study aimed to investigate the outcomes of cerclage wiring to manage intra-operative fractures occurring during cementless hemiarthroplasty in older patients with a femoral neck fracture.
Methods
Medical records and radiographs of older patients with femoral neck fractures who underwent hemiarthroplasty during 2009 to 2015 were retrospectively reviewed. Patients who received cerclage wiring were matched with a demographically matched control group that did not. Patients were followed for at least 12 months. Functional outcomes and health-related quality of life were evaluated by determining the distance of distal stem migration, Barthel Index, EuroQol-visual analog scale (VAS), and pain-VAS.
Results
Eighty-one patients were included, comprising 27 study group and 54 control group patients. A tapered wedge-shaped femoral prosthesis was implanted in all cases. No significant differences in distance of distal stem migration or rate of stem subsidence > 2 mm were observed between the case and control groups (subsidence rate 11.1 vs. 14.8%, respectively). There was also no significant difference in functional outcomes between groups.
Conclusion
Our results revealed a low mean distance of distal stem migration and a low subsidence rate. Functional outcomes and quality of life were similar between the two groups. Cerclage wiring technique is safe, and it should be routinely performed when intra-operative femoral fracture occurs during cementless hemiarthroplasty.



Similar content being viewed by others
References
Kanis JA, Melton LJ 3rd, Christiansen C, Johnston CC, Khaltaev N (1994) The diagnosis of osteoporosis. J Bone Miner Res 9(8):1137–1141. https://doi.org/10.1002/jbmr.5650090802
Millar WJ, Hill GB (1994) Hip fractures: mortality, morbidity and surgical treatment. Health Rep 6(3):323–337
Civinini R, Paoli T, Cianferotti L, Cartei A, Boccaccini A, Peris A et al (2018) Functional outcomes and mortality in geriatric and fragility hip fractures-results of an integrated, multidisciplinary model experienced by the “Florence hip fracture unit”. Int Orthop. https://doi.org/10.1007/s00264-018-4132-3
Cooper C, Campion G, Melton LJ 3rd (1992) Hip fractures in the elderly: a world-wide projection. Osteoporos Int 2(6):285–289. https://doi.org/10.1007/BF01623184
Gullberg B, Johnell O, Kanis JA (1997) World-wide projections for hip fracture. Osteoporos Int 7(5):407–413. https://doi.org/10.1007/PL00004148
Stone AV, Jinnah A, Wells BJ, Atkinson H, Miller AN, Futrell WM et al (2018) Nutritional markers may identify patients with greater risk of re-admission after geriatric hip fractures. Int Orthop 42(2):231–238. https://doi.org/10.1007/s00264-017-3663-3
Wang Z, Bhattacharyya T (2017) Outcomes of hemiarthroplasty and total hip arthroplasty for femoral neck fracture: a Medicare cohort study. J Orthop Trauma 31(5):260–263. https://doi.org/10.1097/BOT.0000000000000814
Sonaje JC, Meena PK, Bansiwal RC, Bobade SS (2018) Comparison of functional outcome of bipolar hip arthroplasty and total hip replacement in displaced femoral neck fractures in elderly in a developing country: a 2-year prospective study. Eur J Orthop Surg Traumatol 28(3):493–498. https://doi.org/10.1007/s00590-017-2057-y
He JH, Zhou CP, Zhou ZK, Shen B, Yang J, Kang PD et al (2012) Meta-analysis comparing total hip arthroplasty with hemiarthroplasty in the treatment of displaced femoral neck fractures in patients over 70 years old. Chin J Traumatol 15(4):195–200. https://doi.org/10.3760/cma.j.issn.1008-1275.2012.04.001
von Roth P, Abdel MP, Harmsen WS, Berry DJ (2015) Cemented bipolar hemiarthroplasty provides definitive treatment for femoral neck fractures at 20 years and beyond. Clin Orthop Relat Res 473(11):3595–3599. https://doi.org/10.1007/s11999-015-4462-z
Donaldson AJ, Thomson HE, Harper NJ, Kenny NW (2009) Bone cement implantation syndrome. Br J Anaesth 102(1):12–22. https://doi.org/10.1093/bja/aen328
Yli-Kyyny T, Ojanpera J, Venesmaa P, Kettunen J, Miettinen H, Salo J et al (2013) Perioperative complications after cemented or uncemented hemiarthroplasty in hip fracture patients. Scand J Surg 102(2):124–128. https://doi.org/10.1177/1457496913482249
Olsen F, Kotyra M, Houltz E, Ricksten SE (2014) Bone cement implantation syndrome in cemented hemiarthroplasty for femoral neck fracture: incidence, risk factors, and effect on outcome. Br J Anaesth 113(5):800–806. https://doi.org/10.1093/bja/aeu226
Bell KR, Clement ND, Jenkins PJ, Keating JF (2014) A comparison of the use of uncemented hydroxyapatite-coated bipolar and cemented femoral stems in the treatment of femoral neck fractures: a case-control study. Bone Joint J 96-B(3):299–305. https://doi.org/10.1302/0301-620x.96b3.32271
McGraw IW, Spence SC, Baird EJ, Eckhardt SM, Ayana GE (2013) Incidence of periprosthetic fractures after hip hemiarthroplasty: are uncemented prostheses unsafe? Injury 44(12):1945–1948. https://doi.org/10.1016/j.injury.2013.07.023
Ng ZD, Krishna L (2014) Cemented versus cementless hemiarthroplasty for femoral neck fractures in the elderly. J Orthop Surg (Hong Kong) 22(2):186–189. https://doi.org/10.1177/230949901402200214
Morris K, Davies H, Wronka K (2015) Implant-related complications following hip hemiarthroplasty: a comparison of modern cemented and uncemented prostheses. Eur J Orthop Surg Traumatol 25(7):1161–1164. https://doi.org/10.1007/s00590-015-1671-9
Davidson D, Pike J, Garbuz D, Duncan CP, Masri BA (2008) Intraoperative periprosthetic fractures during total hip arthroplasty. Evaluation and management. J Bone Joint Surg Am 90(9):2000–2012. https://doi.org/10.2106/jbjs.h.00331
Berend KR, Lombardi AV Jr, Mallory TH, Chonko DJ, Dodds KL, Adams JB (2004) Cerclage wires or cables for the management of intraoperative fracture associated with a cementless, tapered femoral prosthesis: results at 2 to 16 years. J Arthroplast 19(7 Suppl 2):17–21. https://doi.org/10.1016/j.arth.2004.06.008
Capello WN, D'Antonio JA, Naughton M (2014) Periprosthetic fractures around a cementless hydroxyapatite-coated implant: a new fracture pattern is described. Clin Orthop Relat Res 472(2):604–610. https://doi.org/10.1007/s11999-013-3137-x
Unnanuntana A, Unkanawarapan H (2017) Short-term radiographic result of cementless hemiarthroplasty using taperer wedge-shaped femoral component in older patients with femoral neck fracture. J Med Assoc Thail 100(8):894–900
Dorr LD, Faugere MC, Mackel AM, Gruen TA, Bognar B, Malluche HH (1993) Structural and cellular assessment of bone quality of proximal femur. Bone 14(3):231–242. https://doi.org/10.3290/j.qi.a39746
Bieger R, Cakir B, Reichel H, Kappe T (2014) Accuracy of hip stem migration measurement on plain radiographs: reliability of bony and prosthetic landmarks Orthopade 43(10): p. 934–939. https://doi.org/10.1007/s00132-014-3014-7
Gruen TA, McNeice GM, Amstutz HC (1979) “Modes of failure” of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res (141):17–27
Mahoney FI, Barthel DW (1965) Functional evaluation: the Barthel Index. Md State Med J 14:61–65
Laohaprasitiporn P, Jarusriwanna A, Unnanuntana A (2017) Validity and reliability of the Thai version of the Barthel Index for elderly patients with femoral neck fracture. J Med Assoc Thail 100(5):539–548
Unnanuntana A, Jarusriwanna A, Nepal S (2018) Validity and responsiveness of Barthel index for measuring functional recovery after hemiarthroplasty for femoral neck fracture. Arch Orthop Trauma Surg:1–7. https://doi.org/10.1007/s00402-018-3020-z
Brooks R (1996) EuroQol: the current state of play. Health Policy 37(1):53–72. https://doi.org/10.1016/0168-8510(96)00822-6
Tidermark J, Bergstrom G, Svensson O, Tornkvist H, Ponzer S (2003) Responsiveness of the EuroQol (EQ 5-D) and the SF-36 in elderly patients with displaced femoral neck fractures. Qual Life Res 12(8):1069–1079. https://doi.org/10.1023/A:1026193812514
DeLoach LJ, Higgins MS, Caplan AB, Stiff JL (1998) The visual analog scale in the immediate postoperative period: intrasubject variability and correlation with a numeric scale. Anesth Analg 86(1):102–106. https://doi.org/10.1213/00000539-199801000-00020
Roberts KC, Brox WT, Jevsevar DS, Sevarino K (2015) Management of hip fractures in the elderly. J Am Acad Orthop Surg 23(2):131–137. https://doi.org/10.5435/jaaos-d-14-00432
Figved W, Opland V, Frihagen F, Jervidalo T, Madsen JE, Nordsletten L (2009) Cemented versus uncemented hemiarthroplasty for displaced femoral neck fractures. Clin Orthop Relat Res 467(9):2426–2435. https://doi.org/10.1007/s11999-008-0672-y
Dammerer D, Putzer D, Glodny B, Petersen J, Arrich F, Krismer M et al (2018) Occult intra-operative periprosthetic fractures of the acetabulum may affect implant survival. Int Orthop. https://doi.org/10.1007/s00264-018-4084-7
Kim SM, Han SB, Rhyu KH, Yoo JJ, Oh KJ, Yoo JH et al (2018) Periprosthetic femoral fracture as cause of early revision after short stem hip arthroplasty—a multicentric analysis. Int Orthop 42(9):2069–2076. https://doi.org/10.1007/s00264-018-3930-y
Barlas KJ, Ajmi QS, Bagga TK, Howell FR, Roberts JA, Eltayeb M (2008) Association of intra-operative metaphyseal fractures with prosthesis size during hemiarthroplasty of the hip. J Orthop Surg (Hong Kong) 16(1):30–34. https://doi.org/10.1177/230949900801600108
Kuo CL, Tan SH, Lee HC (2015) Intra-operative fractures in cementless bipolar hemiarthroplasty. J Orthop Surg (Hong Kong) 23(2):218–222. https://doi.org/10.1177/230949901502300222
Husmann O, Rubin PJ, Leyvraz PF, de Roguin B, Argenson JN (1997) Three-dimensional morphology of the proximal femur. J Arthroplast 12(4):444–450. https://doi.org/10.1016/S0883-5403(97)90201-1
Mahaisavariya B, Sitthiseripratip K, Tongdee T, Bohez EL, Vander Sloten J, Oris P (2002) Morphological study of the proximal femur: a new method of geometrical assessment using 3-dimensional reverse engineering. Med Eng Phys 24(9):617–622. https://doi.org/10.1016/S1350-4533(02)00113-3
Baharuddin MY, Kadir MRA, Zulkifly AH, Saat A, Aziz AA, Lee MH (2011) Morphology study of the proximal femur in malay population. Int J Morphol 29(4):1321–1325
ACt W, Owen JR, Wayne JS, Hess SR, Golladay GJ, Jiranek WA (2017) The effect of prophylactic cerclage wires in primary total hip arthroplasty: a biomechanical study. J Arthroplast 32(6):2023–2027. https://doi.org/10.1016/j.arth.2017.01.019
Lenz M, Perren SM, Richards RG, Muckley T, Hofmann GO, Gueorguiev B et al (2013) Biomechanical performance of different cable and wire cerclage configurations. Int Orthop 37(1):125–130. https://doi.org/10.1007/s00264-012-1702-7
Frisch NB, Charters MA, Sikora-Klak J, Banglmaier RF, Oravec DJ, Silverton CD (2015) Intraoperative periprosthetic femur fracture: a biomechanical analysis of cerclage fixation. J Arthroplast 30(8):1449–1457. https://doi.org/10.1016/j.arth.2015.02.026
Gordon K, Winkler M, Hofstadter T, Dorn U, Augat P (2016) Managing Vancouver B1 fractures by cerclage system compared to locking plate fixation—a biomechanical study. Injury 47(Suppl 2):S51–S57. https://doi.org/10.1016/s0020-1383(16)47009-9
Falez F, Santori N, Panegrossi G (1998) Intraoperative type 1 proximal femoral fractures: influence on the stability of hydroxyapatite-coated femoral components. J Arthroplast 13(6):653–659. https://doi.org/10.1016/S0883-5403(98)80009-0
Schewelov T, Ahlborg H, Sanzen L, Besjakov J, Carlsson A (2012) Fixation of the fully hydroxyapatite-coated Corail stem implanted due to femoral neck fracture: 38 patients followed for 2 years with RSA and DEXA. Acta Orthop 83(2):153–158. https://doi.org/10.3109/17453674.2011.641107
Lee YK, Joung HY, Kim SH, Ha YC, Koo KH (2014) Cementless bipolar hemiarthroplasty using a micro-arc oxidation coated stem in patients with displaced femoral neck fractures. J Arthroplast 29(12):2388–2392. https://doi.org/10.1016/j.arth.2014.04.020
Al-Najjim M, Khattak U, Sim J, Chambers I (2016) Differences in subsidence rate between alternative designs of a commonly used uncemented femoral stem. J Orthop 13(4):322–326. https://doi.org/10.1016/j.jor.2016.06.026
Kabelitz M, Fritz Y, Grueninger P, Meier C, Fries P, Dietrich M (2018) Cementless stem for femoral neck fractures in a patient’s 10th decade of life: high rate of periprosthetic fractures. Geriatr Orthop Surg Rehabil 9:2151459318765381. https://doi.org/10.1177/2151459318765381
Ries C, Boese CK, Dietrich F, Miehlke W, Heisel C (2018) Femoral stem subsidence in cementless total hip arthroplasty: a retrospective single-centre study. Int Orthop. https://doi.org/10.1007/s00264-018-4020-x
Masri BA, Meek RM, Duncan CP (2004) Periprosthetic fractures evaluation and treatment. Clin Orthop Relat Res 420:80–95. https://doi.org/10.1097/00003086-200403000-00012
Pioli G, Barone A, Giusti A, Oliveri M, Pizzonia M, Razzano M et al (2006) Predictors of mortality after hip fracture: results from 1-year follow-up. Aging Clin Exp Res 18(5):381–387
Franzo A, Francescutti C, Simon G (2005) Risk factors correlated with post-operative mortality for hip fracture surgery in the elderly: a population-based approach. Eur J Epidemiol 20(12):985–991. https://doi.org/10.1007/s10654-005-4280-9
Jiang HX, Majumdar SR, Dick DA, Moreau M, Raso J, Otto DD et al (2005) Development and initial validation of a risk score for predicting in-hospital and 1-year mortality in patients with hip fractures. J Bone Miner Res 20(3):494–500. https://doi.org/10.1359/jbmr.041133
Carow J, Carow JB, Coburn M, Kim BS, Bucking B, Bliemel C et al (2017) Mortality and cardiorespiratory complications in trochanteric femoral fractures: a ten year retrospective analysis. Int Orthop 41(11):2371–2380. https://doi.org/10.1007/s00264-017-3639-3
Forni C, Gazineo D, D'Alessandro F, Fiorani A, Morri M, Sabattini T et al (2018) Predictive factors for thirty day mortality in geriatric patients with hip fractures: a prospective study. Int Orthop. https://doi.org/10.1007/s00264-018-4057-x
Bliemel C, Buecking B, Oberkircher L, Knobe M, Ruchholtz S, Eschbach D (2017) The impact of pre-existing conditions on functional outcome and mortality in geriatric hip fracture patients. Int Orthop 41(10):1995–2000. https://doi.org/10.1007/s00264-017-3591-2
Acknowledgements
The authors gratefully acknowledge Ms. Wachirapan Narktang of the Department of Orthopaedic Surgery for assistance with data collection, and Mr. Sutthipol Udompunthurak of the Division of Clinical Epidemiology, Department of Research and Development, Faculty of Medicine Siriraj Hospital, Mahidol University for assistance with statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Unnanuntana, A., Saiyudthong, N. Outcomes of cerclage wiring to manage intra-operative femoral fracture occurring during cementless hemiarthroplasty in older patients with femoral neck fractures. International Orthopaedics (SICOT) 43, 2637–2647 (2019). https://doi.org/10.1007/s00264-019-04327-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-019-04327-9