Abstract
Purpose
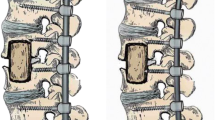
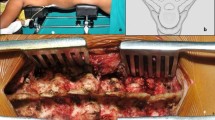
The purpose of this study was to assess the clinical efficacy of intervertebral focal surgery by complete debridement, deformity correction, graft fusion, and internal fixation for patients with non-contiguous multifocal spinal tuberculosis.
Methods
A total of 29 cases with non-contiguous multifocal spinal tuberculosis admitted to the hospital from January 2000 to January 2007 were treated by intervertebral focal surgery. There were 63 foci in 29 cases, averaging 2.2 foci per case, and 146 affected vertebral bodies, averaging 2.3 vertebral bodies per focus. Three cases had one normal intervertebral disc between two foci, and the other 26 cases had two or more normal intervertebral discs between two foci.
Results
All cases were followed-up for an average of five years. The kyphosis showed a mean correction rate of 67.7% after surgery. A mean loss rate of correction of 8.2% was observed at the final follow-up. The levels of erythrocyte sedimentation rate and C-reactive protein returned to normal in 27 cases on average at 5.8 months and bone union could be observed at five months after surgery. Eleven cases with nerve damage recovered to E grade at the final follow-up.
Conclusions
Intervertebral focal surgery by complete debridement, deformity correction, graft fusion, and internal fixation for patients with non-contiguous multifocal spinal tuberculosis was feasible and effective.

Similar content being viewed by others
References
Polley P, Dunn R (2009) Noncontiguous spinal tuberculosis: incidence and management. Eur Spine J 18:1096–1101
Ibn Yacoub Y, Amine B, Hajjaj-Hassouni N (2009) Multilevel vertebral body tuberculosis: a case report. Clin Rheumatol 28:23–26
Lee SH, Sung JK, Park YM (2006) Single-stage transpedicular decompression and posterior instrumentation in treatment of thoracic and thoracolumbar spinal tuberculosis: a retrospective case series. J Spinal Disord Tech 19:595–602
Cengiz Y, Hakan YS, Ilksen G et al (1999) Anterior instrumentation for the treatment of spine tuberculosis. J Bone Joint Surg Am 18:1261–1267
Erturer E, Tezer M, Aydogan M et al (2010) The results of simultaneous posterior-anterior-posterior surgery in multilevel tuberculosis spondylitis associated with severe kyphosis. Eur Spine J 19:2209–2215
Qijun Wu, Wang Z, Ge Z et al (2010) Biomechanical test of varied segment pedicle screw instrumentation following a single of anterior and mid column spine corpectomy. Chinese J Spine Spinal Cord 20:267–271
Wang Z, Qijun Wu, Jin W et al (2010) Debridement and single segment fusion and instrumentation for spinal tuberculosis. Chinese J Spine Spinal Cord 20:811–815
Defino HL, Scarparo P (2005) Fractures of thoracolumbar spine: mon-segmental fixation. Injury 36:90–97
Moon MS, Woo YK, Lee KS et al (1995) Posterior instrumentation and anterior interbody fusion for tuberculous kyphosis of dorsaland lumbar spines. Spine 20:1910–1916
Kaila R, Malhi AM, Mahmood B et al (2007) The incidence of multiple level noncontiguous vertebral tuberculosis detected using whole spine MRI. J Spinal Disord Tech 20:78–81
Shou-Hsin Sua, Wen-Cheng Tsaib, Chun-Yu Linc et al (2010) Clinical features and outcomes of spinal tuberculosis in Southern Taiwan. Microbiol Immunol Infect 43:291–300
Emel E, Guzey FK, Guzey D et al (2006) Non-contiguous multifocal spinal tuberculosis involving cervical, thoracic, lumbar and sacral segments: a case report. Eur Spine J 15:1019–1024
Dunn R, Zondagh I, Candy S (2011) Spinal tuberculosis: magnetic resonance imaging and neurological impairment. Spine 36:469–473
Christodoulou AG, Givissis P, Karataglis D (2006) Treatment of tuberculous spondylitis with anterior stabilization and titanium cage. Clin Orthop Relat Res 5:60–65
Hirakawa A, Miyamoto K, Masuda T et al (2010) Surgical outcome of 2-stage (posterior and anterior) surgical treatment using spinal instrumentation for tuberculous spondylitis. J Spinal Disord Tech 23:133–138
Hou S (2005) Spinal surgery. Beijing: People’s Military Medical Press (1/e): 29–30
Sudo H, Oda I, Abumi K et al (2006) Biomechanical study on the effect of five different lumbar reconstruction techniques on adjacent-level intradiscal pressure and lamina strain. J Neurosurg Spine 5:150–155
Gillet P (2003) The fate of the adjacent motion segments after lumbar fusion. J Spinal Disord 16:338–345
Wang Z, Wang Q (2009) Surgical strategy for spinal tuberculosis. Chinese J Orthopaedics 30(7):717–723
Jin G, Yao L, Cui Y et al (2007) The risk factors analysis of recurrence for spinal tuberculosis. Chinese J Spine Spinal Cord 17:516–519
Sundararaj GD, Amritanand R, Venkatesh K et al (2011) The use of titanium mesh cages in the reconstruction of anterior column defects in active spinal infections: can we rest the crest? Asian Spine J 5:155–161
Liu SY, Li HM, Liang CX et al (2009) Monosegmental transpedicular fixation for selected patients with thoracolumbar burst fractures. J Spinal Disord Tech 22:38–44
Cavusoglu H, Kaya RA, Turkmenoglu ON et al (2008) A long-term follow-up study of anterior tibial allografting and instrumentation in the management of thoracolumbar tuberculous spondylitis. J Neurosurg Spine 8:30–38
Mukhtar AM, Farghaly MM, Ahmed SH (2003) Surgical treatment of thoracic and lumbar tuberculosis by anterior interbody fusion and posterior instrumentation. Med Princ Pract 12:92–96
Moon MS, Kim SS, Lee BJ et al (2011) Surgical management of severe rigid tuberculous kyphosis of dorsolumbar spine. Int Orthop 35:75–81
Author information
Authors and Affiliations
Corresponding author
Additional information
Financial disclosure
Drs Shi, Wang, Geng, and Niu have no relevant financial relationships to disclose. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Both Jian-Dang Shi and Zi-Li Wang contributed equally to this paper.
Rights and permissions
About this article
Cite this article
Shi, JD., Wang, ZL., Geng, GQ. et al. Intervertebral focal surgery for the treatment of non-contiguous multifocal spinal tuberculosis. International Orthopaedics (SICOT) 36, 1423–1427 (2012). https://doi.org/10.1007/s00264-011-1478-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-011-1478-1