Abstract
We previously conducted a randomized phase II trial of OCV-501, a WT1 peptide presented by helper T cells, in elderly AML (acute myeloid leukemia) patients in first remission, indicating no difference in 2-year disease-free survival (DSF) between the OCV-501 and placebo groups. Here, we analyzed 5-year outcome and biomarkers. Five-year DFS was 36.0% in the OCV-501 group (N = 52) and 33.7% in the placebo group (N = 53), with no significant difference (p = 0.74). The peripheral WT1 mRNA levels were marginally suppressed in the OCV-501 group compared with the placebo group. Enhanced anti-OCV-501 IgG response by the 25th week was an independent favorable prognostic factor. Anti-OCV-501 IFNγ responses were less frequent than the IgG reactions. These findings suggest that host immunoreactivity has a significant impact on the prognosis of AML and that further improvement of the WT1 peptide vaccine is needed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The prognosis of elderly patients with acute myeloid leukemia (AML) is poor because of leukemia characteristics, patients’ comorbidities, and treatment toxicities [1, 2]. Even if remission is achieved by chemotherapy, post-remission therapy has not been standardized [3, 4]. Molecular target therapies for AML have been developed, but a problem of resistance emerges [5]. Thus, there is a need for immunotherapy that causes less physical stress and no-cross resistance to the above therapies.
The WT1 gene is highly expressed in hematopoietic and various solid tumors, and cancer immunotherapies targeting WT1 protein have been developed [6,7,8]. Regarding WT1 peptide vaccines, however, there are few reports of studies that have verified its clinical usefulness based on randomized trials. Furthermore, biomarkers related to WT1 vaccine therapy remain unclear.
OCV-501, a tumor vaccine, is an HLA class II-binding polypeptide consisting of 16 amino acid residues derived from WT1 protein [9, 10]. Previous studies revealed that OCV-501 induces not only peptide-specific Th1 cells but also WT1-specific cytotoxic T-lymphocytes, suggesting its potential as a cancer vaccine [9]. From 2013 to 2017, a "multicenter, randomized, placebo-controlled, double-blind, comparative study (Phase II) to evaluate the efficacy and safety of OCV-501 in elderly patients with AML" (referred to as “OCV-501 Phase II trial”) was conducted [11]. Patients with AML aged 60 years or older who had achieved their first complete remission (CR) were randomized to receive OCV-501 (N = 69) or placebo (N = 65), administered the vaccine, and observed for 2 years. Median DFS was 12.1 and 8.4 months in the OCV-501 and placebo groups, respectively, without a significant difference. However, elevated antibody titers or specific T-cell immune responses to OCV-501 were associated with a favorable prognosis. Furthermore, the 2-year DFS rate was approximately 40% in both groups, being higher than expected on planning the OCV-501 Phase II trial. Here we followed the efficacy additionally for 4.2 years (median) and analyzed peripheral WT1 mRNA levels and WT-1-specific immunoreactivity from the perspective of whether they are predictive biomarkers for vaccine efficacy and prognosis (UMIN-CTR ID: UMIN000045499).
Materials and methods
Study design and patients
Among 134 patients who were randomized in the multicenter, randomized, double-blind, placebo-controlled phase II study (ClinicalTrials.gov: NCT01961882), one patient allocated to the OCV-501 group did not receive the study drug, and 28 patients enrolled from overseas institutions were excluded from this study. Of the 105 eligible patients, 52 were the OCV-501 group and 53 were the placebo group. At the end of the OCV-501 phase II trial, 58 of the 105 patients were alive and 47 had died. Among the 58 surviving patients, updated information was obtained from 52 patients and censored data at the end of the trial were used in the remaining 6 patients. The study procedure and assessment were described previously [11].
Briefly, AML patients who were ≥ 60 years, achieved initial CR with one or two cycles of induction chemotherapy, finished consolidation, and were not eligible for transplantation were enrolled. Since binding of OCV-501 to HLA class II molecules can be expected in 83.8–98.8% of Japanese [10], HLA genotyping was not performed for patient recruitment. Patients were randomly assigned to receive either OCV-501 emulsified with Montanide ISA 51 adjuvant (Seppic Inc., Pris, France) or placebo (adjuvant only) for 2 years. Blood was collected to evaluate the WT1 mRNA expression level and anti-OCV-501 antibody at least once every four weeks until 2 years or relapse. Peripheral blood was collected in the 1st, 5th, 9th, and 13th weeks, and every 12 weeks after the 13th week to assess OCV-501-specific interferon γ (IFNγ) production. The primary endpoint was 5-year disease-free survival (DFS), and secondary endpoints were 5-year overall survival (OS) and interactions between immunoreactivities to OCV-501 and the prognosis and between peripheral WT1 mRNA levels and the prognosis.
Statistical analysis
DFS was defined as the length of time from the date of vaccination to any recurrent disease or death, whichever occurred first. OS was defined as the length of time from the date of vaccination to death from any cause. Survival curves were estimated using the Kaplan–Meier method and compared using log-rank tests. Univariate and multivariate analyses were performed using the Cox proportional hazards regression model. The Wilcoxon rank-sum test, Fisher’s exact test, and chi-square test were used to investigate the relationships among various clinical and biological parameters. p-values less than 0.05 were considered significant. Statistical analyses were performed using the statistical software R: A language and environment for statistical computing (ver 4.1.2, R Core Team (2021), R Foundation for Statistical Computing, Vienna, Austria).
Results
The patients’ characteristics are presented in Supplementary Table 1. The 5-year DFS rate (95% confidence interval, 95%CI) was 36.0 (22.8–49.3)% in the OCV-501 group and 33.7 (20.2–47.8)% in the placebo group, indicating no significant difference (p = 0.74, by the log-rank test, Fig. 1). Relapse was reported in 32 of 52 (61.5%) patients in the OCV-501 group and 32 of 53 (60.4%) patients in the placebo group. The 5-year OS rates (95% CI) in the OCV-501 and placebo groups were 36.3 (23.0–49.6)% and 44.4 (30.1–57.7)%, respectively (p = 0.85 by the log-rank test).
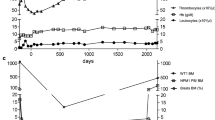
We analyzed the effect of vaccination on peripheral WT1 mRNA levels that were measured every 4 weeks for 2 years in peripheral blood (Supplementary Fig. 1). The median WT1 mRNA level before vaccination was 50.0 copies/cg (49.0–12,000). The individual peak level of WT1 mRNA during the vaccination was lower in the OCV-501 group than in the placebo group, although the difference was marginal (295.0 vs. 910.0/µg RNA, respectively, p = 0.078 by Wilcoxon rank sum test, Table 1).
Next, we analyzed the association between DFS and WT1-specific immunoreactivity. Enhanced WT1-specific IgG responses were observed in the OCV-501 group by the 25th week (Suppl. Figure 2) and this event was not related to age, sex, ECOG score, or myelodysplastic syndromes (MDS)-related changes (data not shown). Peak anti-OCV-501 IgG levels by the 25th week were correlated with the prognosis (p = 0.004, by log-rank test, Fig. 2) The IgG response was an independent prognostic factor (Supplementary Table 2).
Although post-vaccination anti-OCV-501 IFNγ peak levels were also associated with DFS and OS (Fig. 3), the IFNγ response to OCV-501 was less frequent and less persistent than the IgG response (Supplementary Fig. 3).
Discussion
This study revealed that 1) there was no prognostic difference between the OCV-501 and placebo groups even on long-term follow-up, 2) WT1 mRNA levels were marginally suppressed in the OCV-501 group compared with placebo group, 3) the anti-OCV-501 IgG response until the 25th week was independently associated with favorable survival, 4) the anti-OCV-501 IFNγ response was unstable but associated with the prognosis.
Although the first finding is disappointing, the modest suppression of peripheral WT1 mRNA expression levels was encouraging for the WT1 vaccine development. When WT1 mRNA expression was at a low level, its suppressive effect was obvious (Supplementary Fig. 1, Table 1b), and a correlation was observed between the IgG increase and the suppression of WT1 mRNA expression (data not shown). It is expected that this phenomenon reflects the efficacy of vaccines targeting minimal residual disease [12]. Improvement of the vaccination, including dosing methods, intervals, and combination [13], will be necessary, as will the development of non-peptide immunization, as discussed below.
The third finding regarding IgG reactivity is a characteristic observed with this helper peptide. The most likely reason why OCV-501 did not contribute to improved prognosis overall despite IgG reactivity being correlated with prognosis is that vaccine responsiveness reflects general immune functions in AML patients, and that those who retain the functions may have a better prognosis irrespective the vaccine effect.
Recently, there have been reports that there is a difference in immune functions in the bone marrow between a group of patients showing long-term remission with chemotherapy alone and a group of patients showing relapse [14]. Immune-related gene expressions are also related to survival in AML patients [15, 16].
Regarding the fourth finding, the IFNγ-response was observed not only in the OCV-501 group but also in a small number of the placebo group, and both the IFNγ-response subgroups showed a trend towards a better prognosis than the IFNγ-nonresponse subgroup (data not shown). Cell-mediated immunity may have been enhanced by the adjuvants, which might be associated with that 5-year DFS rates exceeded 30% in both groups. WT1-specific cytotoxic T-cells were reportedly detected in AML patients with longer survival [17].
This study shows that responsiveness to the WT1 vaccine in AML patients in CR is variable. For immune-response groups, it will be necessary to improve vaccines to induce earlier responses. For immunocompromised groups, passive immunotherapy, targeting immune suppression or a new kind of WT1 vaccine should be developed [18]. Since immunoreactivity does not correlate with AML classification or age, predicting such reactivity presents a new challenge. Analysis of lymphocyte parameters with or without WT1 peptide specificity is extremely important from the point of view of clinical utility.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Klepin HD, Rao AV, Pardee TS (2014) Acute myeloid leukemia and myelodysplastic syndromes in older adults. J Clin Oncol 32(24):2541–2552. https://doi.org/10.1200/JCO.2014.55.1564
Yanada M, Naoe T (2012) Acute myeloid leukemia in older adults. Int J Hematol 96(2):186–193. https://doi.org/10.1007/s12185-012-1137-3
Gardin C, Turlure P, Fagot T et al (2007) Postremission treatment of elderly patients with acute myeloid leukemia in first complete remission after intensive induction chemotherapy: results of the multicenter randomized acute leukemia French association (ALFA) 9803 trial. Blood 109(12):5129–5135. https://doi.org/10.1182/blood-2007-02-069666
Farag SS, Maharry K, Zhang MJ et al (2011) Comparison of reduced-intensity hematopoietic cell transplantation with chemotherapy in patients age 60–70 years with acute myelogenous leukemia in first remission. Biol Blood Marrow Transplant 17(12):1796–1803. https://doi.org/10.1016/j.bbmt.2011.06.005
Bazinet A, Kantarjian HM (2023) Moving toward individualized target-based therapies in acute myeloid leukemia. Ann Oncol 34(2):141–151. https://doi.org/10.1016/j.annonc.2022.11.004
Sugiyama H (2010) WT1 (Wilms’ tumor gene 1): biology and cancer immunotherapy. Jpn J Clin Oncol 40(5):377–387. https://doi.org/10.1093/jjco/hyp194
Przespolewski A, Szeles A, Wang ES (2018) Advances in immunotherapy for acute myeloid leukemia. Future Oncol 14(10):963–978. https://doi.org/10.2217/fon-2017-0459
Barbullushi K, Rampi N, Serpenti F et al (2022) Vaccination therapy for acute myeloid leukemia: where do we stand? Cancers (Basel) 14(12):2994. https://doi.org/10.3390/cancers14122994
Fujiki F, Oka Y, Tsuboi A et al (2007) Identification and characterization of a WT1 (Wilms Tumor Gene) protein-derived HLA-DRB1*0405-restricted 16-mer helper peptide that promotes the induction and activation of WT1-specific cytotoxic T lymphocytes. J Immunother 30(3):282–293. https://doi.org/10.1097/01.cji.0000211337.91513.94
Kobayashi Y, Sakura T, Miyawaki S et al (2017) A new peptide vaccine OCV-501: in vitro pharmacology and phase 1 study in patients with acute myeloid leukemia. Cancer Immunol Immunother 66(7):851–863. https://doi.org/10.1007/s00262-017-1981-3
Kiguchi T, Yamaguchi M, Takezako N et al (2022) Efficacy and safety of Wilms’ tumor 1 helper peptide OCV-501 in elderly patients with acute myeloid leukemia: a multicenter, randomized, double-blind, placebo-controlled phase 2 trial. Cancer Immunol Immunother 71(6):1419–1430. https://doi.org/10.1007/s00262-021-03074-4
Ogawa H, Tamaki H, Ikegame K et al (2003) The usefulness of monitoring WT1 gene transcripts for the prediction and management of relapse following allogeneic stem cell transplantation in acute type leukemia. Blood 101(5):1698–1704. https://doi.org/10.1182/blood-2002-06-1831
Tsuboi A, Hashimoto N, Fujiki F et al (2019) A phase I clinical study of a cocktail vaccine of Wilms’ tumor 1 (WT1) HLA class I and II peptides for recurrent malignant glioma. Cancer Immunol Immunother 68(2):331–340. https://doi.org/10.1007/s00262-018-2274-1
Ferraro F, Miller CA, Christensen KA et al (2021) Immunosuppression and outcomes in adult patients with de novo acute myeloid leukemia with normal karyotypes. Proc Natl Acad Sci USA 118(49):e2116427118. https://doi.org/10.1073/pnas.2116427118
Ragaini S, Wagner S, Marconi G et al (2022) An IDO1-related immune gene signature predicts overall survival in acute myeloid leukemia. Blood Adv 6(1):87–99. https://doi.org/10.1182/bloodadvances.2021004878
Ding H, Feng Y, Xu J et al (2022) A novel immune prognostic model of non-M3 acute myeloid leukemia. Am J Transl Res 14(8):5308–5325
Casalegno-Garduño R, Schmitt A, Spitschak A, Schmitt M et al (2016) Immune responses to WT1 in patients with AML or MDS after chemotherapy and allogeneic stem cell transplantation. Int J Cancer 138(7):1792–1801. https://doi.org/10.1002/ijc.29909
Fujii S, Kawamata T, Shimizu K et al (2022) Reinvigoration of innate and adaptive immunity via therapeutic cellular vaccine for patients with AML. Mol Ther Oncolytics 27:315–332. https://doi.org/10.1016/j.omto.2022.09.001
Acknowledgements
We would like to express our gratitude to Prof. Haruo Sugiyama for his suggestion of this study and data analysis. We thank Mr. Nobuhito Sanada, Ms. Akiko Kageyama, and Mr. Junji Ikeda (Otsuka Pharmaceutical Co., Ltd., Tokyo, Japan) for their helpful advice on the data of "multicenter, randomized, placebo-controlled, double-blind, comparative study (Phase II) to evaluate the efficacy and safety of OCV-501 in elderly patients with acute myeloid leukemia”, which was provided by Cancer Immunology Laboratory Co., Ltd., Osaka, Japan.
Funding
This study was funded by Cancer Immunology Laboratory Co., Ltd. (Osaka, Japan).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collections were performed by all authors except TN and AS. Data management and analysis were done by TN and AS. The first draft of the manuscript was written by AS and TN, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.”
Corresponding author
Ethics declarations
Conflict of interest
Financial interests: Tomoki Naoe has received speaker honoraria from Astellas, Otsuka, Nippon-Shinyaku, Pfizer, Bristol-Myers Saquibb and Sysmex. Nahoko Hosono has received honorarium from Abbvie GK. Mizuki Ogura has received honorarium from Nippon Shinyaku, Chugai, and AstraZeneca. Kensuke Usuki has received research funding from Astellas、AbbVie、Ono, Chugai, Bristol-Myers Saquibb, Otsuka, Yakult, Agios, MSD, Aperis, Amgen, Alxion, Incyte, Eisai, Kyowa-Kirin, Sanfi, SymBio, Celgene, Daichi Sankyo, Sumitomo-Dainippon, Nippon Shinyaku, Novartis, Mundi, Janssen, and Takeda, has served on speaker honoraria for Novartis, Astellas, Alexion, Eisai, MSD, Otsuka, Ono, Kyowa-Kirin, Celgene, Daiichi Sankyo, Takeda, Nippon-Shinyaku, PharmaEssentia, Bristol-Myers Squibb, Yakult, Sanofi, Pfizer, Abbvie, and Chugai, and has served on consulting bureaus for Alexion, SymBio, Nippon Shinyaku, Otsuka, Chugai, Sanofi, Takeda, Kyowa-Kirin, Astellas, SOBI, and Alnylam Japan. Hirokazu Nagai has received speaker honoraria from Abbvie GK and Nihon Shinyaku Co. Ltd., and research funding from Nihon Shinyaku Co. Ltd.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki and Ethical Guidelines for Medical and Health Research Involving Human Subjects established by the Ministry of Health, Labor and Welfare. The protocol was approved by the Ethics Committee of NHO Nagoya Medical Center (Dec. 03. 2021/No. 2021–032). Permission was obtained from all medical institutions participating in this clinical study.
Consent to participate
Since this study was an academic study using only existing clinical information without acquiring new materials or information, written or verbal consent was not required from the research subjects. Information about the research was posted on the hospital website, and research subjects were guaranteed an opportunity to refuse to participate in the research.
Consent for publication
Not applicable to this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Naoe, T., Saito, A., Hosono, N. et al. Immunoreactivity to WT1 peptide vaccine is associated with prognosis in elderly patients with acute myeloid leukemia: follow-up study of randomized phase II trial of OCV-501, an HLA class II-binding WT1 polypeptide. Cancer Immunol Immunother 72, 2865–2871 (2023). https://doi.org/10.1007/s00262-023-03432-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-023-03432-4