Abstract
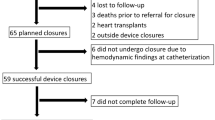
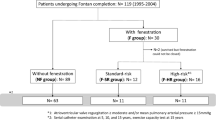
Fontan fenestration decreases central venous pressure and preserves cardiac output while decreasing systemic oxygen saturation. Transcatheter fenestration closure increases oxygen saturation, though the persistence of this increase and the long-term incidence of adverse outcomes such as death and heart transplant remain unknown. We describe immediate and long-term clinical and adverse outcomes following fenestration closure. Catheterization, echocardiogram, and clinic reports were reviewed following transcatheter Fontan fenestration closure. Data were reported as n (%) and median (IQR). Continuous variables were compared using Wilcoxon ranked sum test. 51 patients had fenestration closure 0.9 (0.7–1.5) years following extracardiac Fontan operation. Most (84%) were closed with Amplatzer Septal Occluders. Systemic O2 saturation immediately increased from 87 (83–89) to 95 (94–97)%, P < 0.05. Cardiac index decreased from 4 (3–5) to 2.9 (2.6–3.5) L/min/m2. Fontan pressure and pulmonary vascular resistance were not significantly changed. Clinical follow-up duration for all patients was 7.3 (range 1.3–16) years. Oxygen saturation at last follow-up was 94.5 (92–97)% and did not decrease over time (P < 0.05). One patient (2%) developed protein losing enteropathy, 1 (2%) had heart transplant, and 1 (2%) patient died 9.4 years following fenestration closure. No patient required fenestration re-creation following closure. Transcatheter Fontan fenestration closure leads to sustained increases in systemic oxygen saturation and a low incidence of adverse outcomes such as death and transplant. Further study comparing fenestration closure to non-closure and longer follow-up duration are required to determine if there is a survival benefit to fenestration closure.
Similar content being viewed by others
References
Rychik J et al (2019) Evaluation and management of the child and adult with Fontan circulation: a scientific statement from the American Heart Association. Circulation 140(6):e234–e284
Fontan F, Baudet E (1971) Surgical repair of tricuspid atresia. Thorax 26(3):240–248
Marcelletti C et al (1990) Inferior vena cava-pulmonary artery extracardiac conduit. J Thorac Cardiovasc Surg 100(2):228–232
Lemler MS et al (2002) Fenestration improves clinical outcome of the Fontan procedure: a prospective, randomized study. Circulation 105(2):207–212
Bridges ND, Lock JE, Castaneda AR (1990) Baffle fenestration with subsequent transcatheter closure. Modification of the Fontan operation for patients at increased risk. Circulation 82(5):1681–1689
Zahn E et al (1998) Transcatheter closure of an extracardiac fontan fenestration. Ann Thorac Surg 66:260–262
Jacobs ML, Norwood Jr WI (1994) Fontan operation: influence of modifications on morbidity and mortality. Ann Thorac Surg 58(4):945–951. (discussion 951–952)
Atz AM et al (2011) Late status of Fontan patients with persistent surgical fenestration. J Am Coll Cardiol 57(24):2437–2443
Hijazi ZM et al (1992) Hemodynamic evaluation before and after closure of fenestrated Fontan. An acute study of changes in oxygen delivery. Circulation 86(1):196–202
Goff DA et al (2000) Clinical outcome of fenestrated Fontan patients after closure: the first 10 years. Circulation 102(17):2094–2099
Webb MK et al (2020) Extracardiac Fontan fenestration device closure with amplatzer vascular plug II and septal occluder: procedure results and medium-term follow-up. Pediatr Cardiol 41(4):703–708
Itkin M et al (2017) Protein-losing enteropathy in patients with congenital heart disease. J Am Coll Cardiol 69(24):2929–2937
Healy F, Hanna BD, Zinman R (2012) Pulmonary complications of congenital heart disease. Paediatr Respir Rev 13(1):10–15
Avitabile CM et al (2014) A multifaceted approach to the management of plastic bronchitis after cavopulmonary palliation. Ann Thorac Surg 98(2):634–640
Daniels CJ et al (2017) Fontan-associated liver disease: proceedings from the American College of Cardiology stakeholders meeting, October 1 to 2, 2015, Washington DC. J Am Coll Cardiol 70(25):3173–3194
Bae EJ et al (2003) De novo creation of fenestration and stent implantation for failed extracardiac conduit Fontan operation. Int J Cardiol 88(2–3):321–322
Chaudhari M, Stumper O (2004) Plastic bronchitis after Fontan operation: treatment with stent fenestration of the Fontan circuit. Heart 90(7):801
Vyas H et al (2007) Results of transcatheter Fontan fenestration to treat protein losing enteropathy. Catheter Cardiovasc Interv 69(4):584–589
Funding
The authors did not receive funding from any organization for the submitted work.
Ethics declarations
Competing Interests
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Devanagondi, R., Leonard, G. Transcatheter Fontan Fenestration Closure: Sustained Improvements in Oxygen Saturation with Minimal Morbidity and Mortality. Pediatr Cardiol 44, 922–926 (2023). https://doi.org/10.1007/s00246-022-03077-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-022-03077-7