Abstract
Purpose
To develop and validate a prediction model based on imaging data for the prognosis of mild chronic subdural hematoma undergoing atorvastatin treatment.
Methods
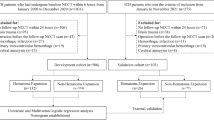
We developed the prediction model utilizing data from patients diagnosed with CSDH between February 2019 and November 2021. Demographic characteristics, medical history, and hematoma characteristics in non-contrast computed tomography (NCCT) were extracted upon admission to the hospital. To reduce data dimensionality, a backward stepwise regression model was implemented to build a prognostic prediction model. We calculated the area under the receiver operating characteristic curve (AUC) of the prognostic prediction model by a tenfold cross-validation procedure.
Results
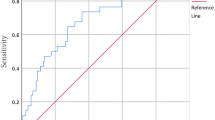
Maximum thickness, volume, mean density, morphology, and kurtosis of the hematoma were identified as the most significant predictors of good hematoma dissolution in mild CSDH patients undergoing atorvastatin treatment. The prediction model exhibited good discrimination, with an area under the curve (AUC) of 0.82 (95% confidence interval [CI], 0.74–0.90) and good calibration (p = 0.613). The validation analysis showed the AUC of the final prognostic prediction model is 0.80 (95% CI 0.71–0.86) and it has good prediction performance.
Conclusion
The imaging data-based prediction model has demonstrated great prediction accuracy for good hematoma dissolution in mild CSDH patients undergoing atorvastatin treatment. The study results emphasize the importance of imaging data evaluation in the management of CSDH patients.





Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Liu W, Bakker NA, Groen RJ (2014) Chronic subdural hematoma: a systematic review and meta-analysis of surgical procedures. J Neurosurg 121(3):665–673
Karibe H, Kameyama M, Kawase M, Hirano T, Kawaguchi T, Tominaga T (2011) Epidemiology of chronic subdural hematomas. No shinkei geka Neurol Surg 39(12):1149–1153
Santarius T, Hutchinson PJ (2004) Chronic subdural haematoma: time to rationalize treatment? Br J Neurosurg 18(4):328–332
Shimamura N, Ogasawara Y, Naraoka M, Ohnkuma H (2009) Irrigation with thrombin solution reduces recurrence of chronic subdural hematoma in high-risk patients: preliminary report. J Neurotrauma 26(11):1929–1933
Lee L, Ker J, Ng HY, Munusamy T, King NK, Kumar D et al (2016) Outcomes of chronic subdural hematoma drainage in nonagenarians and centenarians: a multicenter study. J Neurosurg 124(2):546–551
Jiang R (2018) Safety and efficacy of atorvastatin for chronic subdural hematoma in chinese patients: a randomized clinicaltrial. JAMA Neurol 75(11):1338–1346
Zhang X, Wang D, Tian Y, Wei H, Liu X, Xiang T et al (2021) Risk factors for atorvastatin as a monotherapy for chronic subdural hematoma: a retrospective multifactor analysis. Front Aging Neurosci 13(564):726592
Ahmed OEF, Nagaty A, Helmy M, El Molla ST (2023) The use of dexamethasone therapy for conservative management of chronic subdural hematomas: a question about efficacy and safety. Egypt J Neurol Psychiatry Neurosurg 59(1):48
Zhang J, Fei Z, Feng H, Gao G, Hao J, Hou L et al (2021) Expert consensus on drug treatment of chronic subdural hematoma. Chin Neurosurg J 7(1):47
Nakaguchi H, Tanishima T, Yoshimasu N (2001) Factors in the natural history of chronic subdural hematomas that influence their postoperative recurrence. J Neurosurg 95(2):256–262
Khorasanizadeh M, Chang YM, Enriquez-Marulanda A, Mizuhashi S, Salem MM, Gomez-Paz S et al (2021) Morphological changes in chronic subdural hematomas following upfront middle meningeal artery embolization: sequence, timing, and association with outcomes. J Neurosurg 1–14. https://doi.org/10.3171/2021.8.JNS211691
Kramer AA, Zimmerman JE (2007) Assessing the calibration of mortality benchmarks in critical care: the Hosmer-Lemeshow test revisited. Crit Care Med 35(9):2052–2056
Colombani C, Legarra A, Fritz S, Guillaume F, Croiseau P, Ducrocq V et al (2013) Application of Bayesian least absolute shrinkage and selection operator (LASSO) and BayesCπ methods for genomic selection in French Holstein and Montbéliarde breeds. J Dairy Sci 96(1):575–591
Vickers AJ, Cronin AM, Elkin EB, Gonen M (2008) Extensions to decision curve analysis, a novel method for evaluating diagnostic tests, prediction models and molecular markers. BMC Med Inform Decis Mak 8:53
Sauerbrei W, Royston P, Binder H (2007) Selection of important variables and determination of functional form for continuous predictors in multivariable model building. Stat Med 26(30):5512–5528
Holl DC, Volovici V, Dirven CMF, Peul WC, van Kooten F, Jellema K et al (2018) Pathophysiology and nonsurgical treatment of chronic subdural hematoma: from past to present to future. World Neurosurg 116:402–11.e2
Edlmann E, Giorgi-Coll S, Whitfield PC, Carpenter KLH, Hutchinson PJ (2017) Pathophysiology of chronic subdural haematoma: inflammation, angiogenesis and implications for pharmacotherapy. J Neuroinflammation 14(1):108
Wang D, Li T, Wei H, Wang Y, Yang G, Tian Y et al (2016) Atorvastatin enhances angiogenesis to reduce subdural hematoma in a rat model. J Neurol Sci 362:91–99
Verschuren L, Kleemann R, Offerman EH, Szalai AJ, Emeis SJ, Princen HM et al (2005) Effect of low dose atorvastatin versus diet-induced cholesterol lowering on atherosclerotic lesion progression and inflammation in apolipoprotein E*3-Leiden transgenic mice. Arterioscler Thromb Vasc Biol 25(1):161–167
Friede RL, Schachenmayr W (1978) The origin ofsubdural neomembranes. II. Fine structural of neomembranes. Am J Pathol 92(1):69–84
Apfelbaum RI, Guthkelch AN, Shulman K (1974) Experimental production of subdural hematomas. J Neurosurg 40(3):336–346
Killeffer JA, Killeffer FA, Schochet SS (2000) The outer neomembrane of chronic subdural hematoma. Neurosurg Clin N Am 11(3):407–412
Manickam A, Marshman LAG, Johnston R (2017) Membrane surface area to volume ratio in chronic subdural hematomas: critical size and potential postoperative target. World Neurosurg 100:256–260
Li Y, Zhang G, Shan Y, Wu X, Liu J, Xue Y et al (2022) Noninvasive assessment of intracranial hypertension in patients with traumatic brain injury using CT radiomic features: a pilot study. J Neurotrauma 40(3-4):250–259
Shan Y, Li Y, Xu X, Feng J, Wu X, Gao G (2021) Evaluation of intracranial hypertension in traumatic brain injury patient: a noninvasive approach based on cranial computed tomography features. J Clin Med 10(11):2524
Kanazawa T, Takahashi S, Minami Y, Jinzaki M, Toda M, Yoshida K (2020) Early prediction of clinical outcomes in patients with aneurysmal subarachnoid hemorrhage using computed tomography texture analysis. J Clin Neurosci : Off J Neurosurg Soc Australas 71:144–149
Shen Q, Shan Y, Hu Z, Chen W, Yang B, Han J et al (2018) Quantitative parameters of CT texture analysis as potential markersfor early prediction of spontaneous intracranial hemorrhage enlargement. Eur Radiol 28(10):4389–4396
Thomas R, Qin L, Alessandrino F, Sahu SP, Guerra PJ, Krajewski KM et al (2019) A review of the principles of texture analysis and its role in imaging of genitourinary neoplasms. Abdom Radiol (New York) 44(7):2501–2510
Lubner MG, Smith AD, Sandrasegaran K, Sahani DV, Pickhardt PJ (2017) CT texture analysis: definitions, applications, biologic correlates, and challenges. Radiographics : Rev Publ Radiol Soc N Am Inc 37(5):1483–503
Ng F, Ganeshan B, Kozarski R, Miles KA, Goh V (2013) Assessment of primary colorectal cancer heterogeneity by using whole-tumor texture analysis: contrast-enhanced CT texture as a biomarker of 5-year survival. Radiology 266(1):177–184
Kanazawa T, Takahashi S, Minami Y, Jinzaki M, Toda M, Yoshida K (2020) Prediction of postoperative recurrence of chronic subdural hematoma using quantitative volumetric analysis in conjunction with computed tomography texture analysis. J Clin Neurosci : Off J Neurosurg Soc Australas 72:270–276
Jensen TSR, Andersen-Ranberg N, Poulsen FR, Bergholt B, Hundsholt T, Fugleholm K (2020) The Danish Chronic Subdural Hematoma Study-comparison of hematoma age to the radiological appearance at time of diagnosis. Acta Neurochir 162(9):2007–2013
Funding
This research was supported by the National Natural Science Foundation of China (Nos. 81671221, 81271359, and 81671380); Beijing Tianjin Hebei Basic Research Cooperation Project: Grant Number 19JCZDJC64600 (Z); the Tianjin Research Program of Application Foundation and Advanced Technology (No.19YFZCSY00650) and The Clinical Study of Tianjin Medical University (2017kylc007).
Author information
Authors and Affiliations
Contributions
(I) Conception and design: X. Zhang, R. Jiang, J. Wang; (II) administrative support: Z. Sha, D. Wu; (III) provision of study materials or patients: Y. Tian, D. Wang, M. Nie; (IV) collection and assembly of data: X. Zhang, J. Yuan, M. Liu, C. Gao; (V) data analysis and interpretation: X. Zhang, Z. Sha, D. Wu; (VI) manuscript writing: all authors; (VII) final approval of manuscript: all authors.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was approved by Ethics Committee of Tianjin Medical University General Hospital (Ethical.NO.IRB2022-WZ-157) and individual consent for this retrospective analysis was waived. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013).
Informed consent
Individual consent for this retrospective analysis was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, X., Sha, Z., Feng, D. et al. Establishment and validation of a CT-based prediction model for the good dissolution of mild chronic subdural hematoma with atorvastatin treatment. Neuroradiology (2024). https://doi.org/10.1007/s00234-024-03340-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00234-024-03340-z