Abstract
Introduction and hypothesis
Running is known to cause urinary leakage in women with stress urinary incontinence (SUI). Task-specific fiber-type recruitment while running can be estimated using wavelets. The aim of this study was to compare the effect of a new physiotherapy program including involuntary, reflexive training with a standard physiotherapy program on pelvic floor muscle (PFM) activation patterns and fiber-type recruitment behavior while running.
Methods
In this triple-blinded randomized controlled trial, women with SUI were randomly allocated to the control group (CON), which performed a standard physiotherapy program, or the experimental group (EXP), which received additional involuntary, reflexive training. PFM electromyography (EMG) was recorded during 10 s at three running speeds and analyzed using Morse wavelets. The relative distribution of power (%) over the frequencies from 20 to 200 Hz was extracted and analyzed within six-time intervals of 30 ms. Statistical nonparametric mapping was performed to identify power spectra differences.
Results
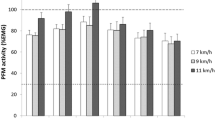
Thirty-nine (CON) and 38 (EXP) women were included. The power spectra showed no statistically significant group differences. The time intervals from 30 ms before to 30 ms after initial contact showed significantly lower intensities than the intervals from 30 to 150 ms after initial contact in the lowest and higher intensities in the highest frequencies for all running speeds and both groups.
Conclusions
Power spectra shifts toward higher frequency bands in the pre-initial contact phase could indicate a feed-forward anticipation and a muscle tuning for the expected impact of initial contact event in order to maintain continence.





Similar content being viewed by others
References
Dumoulin C, Hay-Smith EJ, MacHabee-Seguin G (2014) Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database Syst Rev (5):Cd005654.
Bo K. Pelvic floor muscle training in treatment of female stress urinary incontinence, pelvic organ prolapse and sexual dysfunction. World J Urol. 2012;30(4):437–43.
Cacciari LP, Dumoulin C, Hay-Smith EJ. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women: a Cochrane systematic review abridged republication. Braz J Phys Ther. 2019;23(2):93–107.
Baessler K, Miska K, Draths R, Schuessler B. Effects of voluntary pelvic floor contraction and relaxation on the urethral closure pressure. Int Urogynecol J Pelvic Floor Dysfunct. 2005;16(3):187–90; discussion 190–191.
Shishido K, Peng Q, Jones R, Omata S, Constantinou CE. Influence of pelvic floor muscle contraction on the profile of vaginal closure pressure in continent and stress urinary incontinent women. J Urol. 2008;179(5):1917–22.
Hay JG. Citius, altius, longius (faster, higher, longer): the biomechanics of jumping for distance. J Biomech. 1993;26(Suppl 1):7–21.
Luginbuehl H, Naeff R, Zahnd A, Baeyens JP, Kuhn A, Radlinger L. Pelvic floor muscle electromyography during different running speeds: an exploratory and reliability study. Arch Gynecol Obstet. 2016;293(1):117–24.
Leitner M, Moser H, Eichelberger P, Kuhn A, Radlinger L. Evaluation of pelvic floor muscle activity during running in continent and incontinent women: an exploratory study. Neurourol Urodyn. 2017;36(6):1570–6.
Leitner M, Moser H, Eichelberger P, Kuhn A, Radlinger L. Pelvic floor muscle activity during fast voluntary contractions in continent and incontinent women. Neurourol Urodyn. 2019;38(2):625–31.
Wakeling JM, Pascual SA, Nigg BM, von Tscharner V. Surface EMG shows distinct populations of muscle activity when measured during sustained sub-maximal exercise. Eur J Appl Physiol. 2001;86(1):40–7.
Von Tscharner V. Intensity analysis in time-frequency space of surface myoelectric signals by wavelets of specified resolution. J Electromyogr Kinesiol. 2000;10(6):433–45.
Lindstrom L, Kadefors R, Petersen I. An electromyographic index for localized muscle fatigue. J Appl Physiol Respir Environ Exerc Physiol. 1977;43(4):750–4.
Von Tscharner V, Goepfert B. Estimation of the interplay between groups of fast and slow muscle fibers of the tibialis anterior and gastrocnemius muscle while running. J Electromyogr Kinesiol. 2006;16(2):188–97.
Luginbuehl H, Lehmann C, Baeyens J-P, Kuhn A, Radlinger L. Involuntary reflexive pelvic floor muscle training in addition to standard training versus standard training alone for women with stress urinary incontinence: study protocol for a randomized controlled trial. Trials. 2015;16:524.
Winstein CJ. Knowledge of results and motor learning—implications for physical therapy. Phys Ther. 1991;71(2):140–9.
Moser H, Leitner M, Eichelberger P, Kuhn A, Baeyens JP, Radlinger L. Pelvic floor muscle activity during jumps in continent and incontinent women: an exploratory study. Arch Gynecol Obstet. 2018;297(6):1455–63.
Hermens HJ, Freriks B, Disselhorst-Klug C, Rau G. Development of recommendations for SEMG sensors and sensor placement procedures. J Electromyogr Kinesiol. 2000;10(5):361–74. https://doi.org/10.1016/s1050-6411(00)00027-4.
Von Tscharner V, Goepfert B, Nigg BM. Changes in EMG signals for the muscle tibialis anterior while running barefoot or with shoes resolved by non-linearly scaled wavelets. J Biomech. 2003;36(8):1169–76.
Fleischmann J, Gehring D, Mornieux G, Gollhofer A. Task-specific initial impact phase adjustments in lateral jumps and lateral landings. Eur J Appl Physiol. 2011;111(9):2327–37.
Nystrom E, Sjöström M, Stenlund H, Samuelsson E. ICIQ symptom and quality of life instruments measure clinically relevant improvements in women with stress urinary incontinence. Neurourol Urodyn. 2015;34(8):747–51.
Riemsma R, Hagen S, Kirschner-Hermanns R, et al. Can incontinence be cured? A systematic review of cure rates. BMC Med. 2017;15(1):63.
Ross A, Leveritt M, Riek S. Neural influences on sprint running: training adaptations and acute responses. Sports Med. 2001;31(6):409–25. https://doi.org/10.2165/00007256-200131060-00002.
Sleivert GG, Backus RD, Wenger HA. The influence of a strength-sprint training sequence on multi-joint power output. Med Sci Sports Exerc. 1995;27(12):1655–65.
Hartmann H, Wirth K, Keiner M, Mickel C, Sander A, Szilvas E. Short-term periodization models: effects on strength and speed-strength performance. Sports Med. 2015;45(10):1373–86. https://doi.org/10.1007/s40279-015-0355-2.
Nygaard I, Barber MD, Burgio KL, et al. Prevalence of symptomatic pelvic floor disorders in US women. JAMA. 2008;300(11):1311–6. https://doi.org/10.1001/jama.300.11.1311.
Constantinou CE, Govan DE. Spatial distribution and timing of transmitted and reflexly generated urethral pressures in healthy women. J Urol. 1982;127(5):964–9.
Koenig I, Eichelberger P, Leitner M, et al. Pelvic floor muscle activity patterns in women with and without stress urinary incontinence while running. Ann Phys Rehabil Med. 2019;13(19):30160–5.
Koenig I, Eichelberger P, Blasimann A, Hauswirth A, Baeyens JP, Radlinger L. Wavelet analyses of electromyographic signals derived from lower extremity muscles while walking or running: a systematic review. PLoS One. 2018;13(11):e0206549.
Flury N, Koenig I, Radlinger L. Crosstalk considerations in studies evaluating pelvic floor muscles using surface electromyography in women: a scoping review. Arch Gynecol Obstet. 2017;295(4):799–809.
Keshwani N, McLean L. State of the art review: intravaginal probes for recording electromyography from the pelvic floor muscles. Neurourol Urodyn. 2013;34(2):104–12.
Authors’ contribution to the manuscript
All listed authors have made the required substantive intellectual contributions and meet the criteria for authorship. I. Koenig: project development, conception, and design, data extraction and analyses, manuscript writing, article revision, final approval; P. Eichelberger: data analyses, article revision, final approval; H. Luginbuehl: project development, data collection, article revision, final approval; A. Kuhn: project development, data collection, article revision, and final approval; C. Lehmann: project development, article revision, and final approval; J. Taeymans: manuscript writing, article revision, and final approval; L. Radlinger: project development, conception, and design, data analyses, manuscript writing, article revision, and final approval.
Funding
The RCT was funded by the Swiss National Science Foundation, Division III (Medicine & Biology; 320030_153424/1). The granting organization was not involved in the development and conduction of the present study.
The protocol was registered at Clinical Trials.gov (NCT02318251).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Declaration of interest
None.
Ethics
Ethics committee approval (Ethics Committee of the Canton of Bern, reference number 249/14), in accordance with the Declaration of Helsinki and the Swiss Human Research Act, and written informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Koenig, I., Eichelberger, P., Luginbuehl, H. et al. Activation patterns of pelvic floor muscles in women with incontinence while running: a randomized controlled trial. Int Urogynecol J 32, 335–343 (2021). https://doi.org/10.1007/s00192-020-04334-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04334-0