Abstract
Purpose
To determine the incidence of symptomatic venous thromboembolism (VTE) following anterior cruciate ligament (ACL) reconstruction using a large national database and to identify corresponding independent risk factors.
Methods
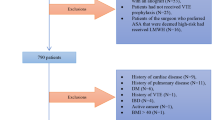
The Humana administrative claims database was reviewed for patients undergoing ACL reconstruction from 2007 to 2017. Patient demographics, medical comorbidities, as well as concurrent procedures were recorded. Postoperative incidence of VTE was measured by identifying symptomatic deep vein thrombosis (DVT) and pulmonary embolism (PE) at 30 days, 90 days, and 1 year postoperatively. Univariate analysis and binary logistic regression were performed to determine independent risk factors for VTE following surgery.
Results
A total of 11,977 patients were included in the study. The incidence of VTE was 1.01% (n = 120) and 1.22% (n = 146) at 30 and 90 days, respectively. Analysis of VTE events within the first postoperative year revealed that 69.6% and 84.3% of VTEs occurred within 30 and 90 days of surgery, respectively. Logistic regression identified age ≥ 45 (odds ratio [OR] = 1.88; 95% confidence interval [CI] 1.32–2.68; p < 0.001), inpatient surgery (OR = 2.07; 95% CI 1.01–4.24; p = 0.045), COPD (OR = 1.51; 95% CI 1.02–2.24; p = 0.041), and tobacco use (OR = 1.75; 95% CI 1.17–2.62; p = 0.007), as well as concurrent PCL reconstruction (OR = 3.85; 95% CI 1.71–8.67; p = 0.001), meniscal transplant (OR = 17.68; 95% CI 3.63–85.97; p < 0.001) or osteochondral allograft (OR = 15.73; 95% CI 1.79–138.43; p = 0.013) as independent risk factors for VTE after ACL reconstruction.
Conclusions
The incidence of symptomatic postoperative VTE is low following ACL reconstruction, with the majority of cases occurring within 90 days of surgery. Risk factors include age ≥ 45, inpatient surgery, COPD, tobacco use and concurrent PCL reconstruction, meniscal transplant or osteochondral allograft.
Level of evidence
III.


Similar content being viewed by others
References
Abram SGF, Judge A, Beard DJ, Price AJ (2019) Rates of adverse outcomes and revision surgery after anterior cruciate ligament reconstruction: a study of 104,255 procedures using the national hospital episode statistics database for England, UK. Am J Sports Med 47:2533–2542
Adala R, Anand A, Kodikal G (2011) Deep vein thrombosis and thromboprophylaxis in arthroscopic anterior cruciate ligament reconstruction. Indian J Orthop 45:450–453
Alaia MJ, Patel D, Levy A, Youm T, Bharam S, Meislin R et al (2013) (2014) The incidence of venous thromboembolism (VTE)–after hip arthroscopy. Bull HospJt Dis 72:154–158
Alaia MJ, Zuskov A, Davidovitch RI (2011) Contralateral deep venous thrombosis after hip arthroscopy. Orthopedics 34:e674-677
Anderson FA Jr, Spencer FA (2003) Risk factors for venous thromboembolism. Circulation 107:I9-16
Beasley LS, Weiland DE, Vidal AF, Chhabra A, Herzka AS, Feng MT et al (2005) Anterior cruciate ligament reconstruction: a literature review of the anatomy, biomechanics, surgical considerations, and clinical outcomes. Oper Tech Orthop 15:5–19
Bokshan SL, DeFroda SF, Panarello NM, Owens BD (2018) Risk factors for deep vein thrombosis or pulmonary embolus following anterior cruciate ligament reconstruction. Orthop J Sports Med 6:2325967118781328
Cancienne JM, Gwathmey FW, Miller MD, Werner BC (2016) Tobacco use is associated with increased complications after anterior cruciate ligament reconstruction. Am J Sports Med 44:99–104
Chen D, Li Q, Rong Z, Yao Y, Xu Z, Shi D et al (2017) Incidence and risk factors of deep venous thrombosis following arthroscopic posterior cruciate ligament reconstruction. Medicine (Baltimore) 96:e7074
Cullison TR, Muldoon MP, Gorman JD, Goff WB (1996) The incidence of deep venous thrombosis in anterior cruciate ligament reconstruction. Arthroscopy 12:657–659
Cvetanovich GL, Chalmers PN, Verma NN, Cole BJ, Bach BR Jr (2016) Risk factors for short-term complications of anterior cruciate ligament reconstruction in the United States. Am J Sports Med 44:618–624
Dong JT, Wang X, Men XQ, Wang XF, Zheng XZ, Gao SJ (2015) Incidence of deep venous thrombosis in Chinese patients undergoing arthroscopic knee surgery for cruciate ligament reconstruction. Knee Surg Sports TraumatolArthrosc 23:3540–3544
Ekdahl V, Stalman A, Forssblad M, Samuelsson K, Edman G, Kraus Schmitz J (2020) There is no general use of thromboprophylaxis and prolonged antibiotic prophylaxis in anterior cruciate ligament reconstruction: a nation-wide survey of ACL surgeons in Sweden. Knee Surg Sports TraumatolArthrosc. https://doi.org/10.1007/s00167-020-05851-7
Erickson BJ, Saltzman BM, Campbell KA, Fillingham YA, Harris JD, Gupta AK et al (2015) Rates of deep venous thrombosis and pulmonary embolus after anterior cruciate ligament reconstruction: a systematic review. Sports Health 7:261–266
Gaskill T, Pullen M, Bryant B, Sicignano N, Evans AM, DeMaio M (2015) The prevalence of symptomatic deep venous thrombosis and pulmonary embolism after anterior cruciate ligament reconstruction. Am J Sports Med 43:2714–2719
Gowd AK, Cvetanovich GL, Liu JN, Christian DR, Cabarcas BC, Redondo ML et al (2019) Management of chondral lesions of the knee: analysis of trends and short-term complications using the national surgical quality improvement program database. Arthroscopy 35:138–146
Ilahi OA, Reddy J, Ahmad I (2005) Deep venous thrombosis after knee arthroscopy: a meta-analysis. Arthroscopy 21:727–730
Janssen RP, Reijman M, Janssen DM, van Mourik JB (2016) Arterial complications, venous thromboembolism and deep venous thrombosis prophylaxis after anterior cruciate ligament reconstruction: a systematic review. World J Orthop 7:604–617
Janssen RP, Sala HA (2007) Fatal pulmonary embolism after anterior cruciate ligament reconstruction. Am J Sports Med 35:1000–1002
Jenny JY, Francophone Arthroscopy S (2020) Thromboprophylaxis in arthroscopy: survey of current practices in France and comparison with recommendations. OrthopTraumatolSurg Res 106:S183–S187
Jenny JY, Pabinger I, Samama CM, Force EVGT (2018) European guidelines on perioperative venous thromboembolism prophylaxis: Aspirin. Eur J Anaesthesiol 35:123–129
Keller RA, Moutzouros V, Dines JS, Bush-Joseph CA, Limpisvasti O (2018) Deep venous thrombosis prophylaxis in anterior cruciate ligament reconstructive surgery: what is the current state of practice? Sports Health 10:156–159
Khazi ZM, An Q, Duchman KR, Westermann RW (2019) Incidence and risk factors for venous thromboembolism following hip arthroscopy: a population-based study. Arthroscopy 35(2380–2384):e2381
Kraus Schmitz J, Lindgren V, Janarv PM, Forssblad M, Stalman A (2019) Deep venous thrombosis and pulmonary embolism after anterior cruciate ligament reconstruction: incidence, outcome, and risk factors. Bone Jt J 101:34–40
Maletis GB, Inacio MC, Funahashi TT (2013) Analysis of 16,192 anterior cruciate ligament reconstructions from a community-based registry. Am J Sports Med 41:2090–2098
Maletis GB, Inacio MC, Reynolds S, Funahashi TT (2012) Incidence of symptomatic venous thromboembolism after elective knee arthroscopy. J Bone JtSurg Am 94:714–720
Manzoli L, De Vito C, Marzuillo C, Boccia A, Villari P (2012) Oral contraceptives and venous thromboembolism: a systematic review and meta-analysis. Drug Saf 35:191–205
Marlovits S, Striessnig G, Schuster R, Stocker R, Luxl M, Trattnig S et al (2007) Extended-duration thromboprophylaxis with enoxaparin after arthroscopic surgery of the anterior cruciate ligament: a prospective, randomized, placebo-controlled study. Arthroscopy 23:696–702
Mohtadi NG, Johnston K, Gaudelli C, Chan DS, Barber RS, Walker R et al (2016) The incidence of proximal deep vein thrombosis after elective hip arthroscopy: a prospective cohort study in low risk patients. J Hip PreservSurg 3:295–303
Nagashima M, Otani T, Takeshima K, Seki H, Nakayama M, Origuchi N et al (2020) Unexpectedly high incidence of venous thromboembolism after arthroscopic anterior cruciate ligament reconstruction: prospective, observational study. J ISAKOSJtDisordOrthopaed Sports Med 5:80–82
Oshiba H, Nawata M, Morioka S, Momose T, Maeda T, Nakatsuchi Y (2019) The incidence and risk factor of deep venous thrombosis after arthroscopically assisted anterior cruciate ligament reconstruction. J Orthop Sci. https://doi.org/10.1016/j.jos.2019.05.014
PeragalloUrrutia R, Coeytaux RR, McBroom AJ, Gierisch JM, Havrilesky LJ, Moorman PG et al (2013) Risk of acute thromboembolic events with oral contraceptive use: a systematic review and meta-analysis. Obstet Gynecol 122:380–389
Planes A, Vochelle N, Darmon JY, Fagola M, Bellaud M, Huet Y (1996) Risk of deep-venous thrombosis after hospital discharge in patients having undergone total hip replacement: double-blind randomised comparison of enoxaparin versus placebo. Lancet 348:224–228
Pugely AJ, Martin CT, Harwood J, Ong KL, Bozic KJ, Callaghan JJ (2015) Database and registry research in orthopaedic surgery: part I: claims-based data. J Bone JtSurg Am 97:1278–1287
Salvo JP, Troxell CR, Duggan DP (2010) Incidence of venous thromboembolic disease following hip arthroscopy. Orthopedics 33:664
Scurr JH (1990) How long after surgery does the risk of thromboembolism persist? Acta ChirScandSuppl 556:22–24
Struijk-Mulder MC, Ettema HB, Verheyen CC, Buller HR (2013) Deep vein thrombosis after arthroscopic anterior cruciate ligament reconstruction: a prospective cohort study of 100 patients. Arthroscopy 29:1211–1216
Sun Y, Chen D, Xu Z, Shi D, Dai J, Qin J et al (2014) Incidence of symptomatic and asymptomatic venous thromboembolism after elective knee arthroscopic surgery: a retrospective study with routinely applied venography. Arthroscopy 30:818–822
Trenor CC 3rd, Chung RJ, Michelson AD, Neufeld EJ, Gordon CM, Laufer MR et al (2011) Hormonal contraception and thrombotic risk: a multidisciplinary approach. Pediatrics 127:347–357
Ye S, Dongyang C, Zhihong X, Dongquan S, Jin D, Jianghui Q et al (2013) The incidence of deep venous thrombosis after arthroscopically assisted anterior cruciate ligament reconstruction. Arthroscopy 29:742–747
Funding
There was no funding obtained for this study.
Author information
Authors and Affiliations
Contributions
Author participation using the ICMJE criteria for authorship: EMF, KCP, MRC, OLG, ZMK, YL, WC: Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; Drafting the work or revising it critically for important intellectual content; Final approval of the version to be published; Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. BF: Drafting the work or revising it critically for important intellectual content; Final approval of the version to be published; Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Ethical approval
This study was granted exemption from the Institutional Review Board as PearlDiver uses deidentified patient information.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1: International classification of disease (ICD) codes
Appendix 1: International classification of disease (ICD) codes
ICD-9 | ICD-10 | |
|---|---|---|
Deep vein thrombosis | 45340, 45341, 45342, 45382, 45383, 45384 | I8240, I82401, I82402, I82403, I82409, I82410, I82411, I82412, I82413, I82419, I82420, I82421, I82422, I82423, I82429, I82430 to I82499, I824Y1, I824Y2, I824Y3, I824Y9, I824Z1, I824Z2, I824Z3, I824Z9, I82621 to I82629 |
Pulmonary embolism | 41510, 41511, 41519 | I2600, I2602, I2609, I2699 |
Rights and permissions
About this article
Cite this article
Forlenza, E.M., Parvaresh, K.C., Cohn, M.R. et al. Incidence and risk factors for symptomatic venous thromboembolism following anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 30, 1552–1559 (2022). https://doi.org/10.1007/s00167-021-06583-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06583-y