Abstract
Purpose
Previous investigations suggested that femoral side-to-side differences were located in the upper femur anatomy. However, little is known about the asymmetry between distal femur and patella. The degree of bony asymmetry in the patellofemoral joint was evaluated using pairs of CT-scans with emphasis on morphometric measurements and risk factors relevant to patellofemoral disorders.
Methods
Patellofemoral morphometric parameters and anatomical risk factors were analyzed from 345 pairs of CT scans to evaluate side-to-side differences for each patient. All measurements were automatized using previously published algorithm-calculated bone landmarks. We analyzed asymmetry based on absolute differences (AD) and percentage asymmetry (AS%). Significant asymmetry was defined as AS% > 10%.
Results
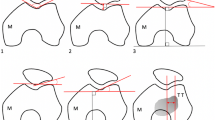
Patellar height was found to be highly symmetric (mean AD 0.1 for both Insall-Salvatti and Caton-Deschamps methods, AS% 8% and 9%, respectively). Patellar and femoral morphometric parameters were found highly symmetric, except for the trochlear groove depth. Substantial asymmetry was reported in two patellofemoral risk factors: the lateral trochlear inclination (mean AD 2°, AS% 16%) and the tibial tuberosity-trochlear groove distance (1 mm, 116%). Patellar and femoral morphometric asymmetries were independent of demographics, including age, gender, height, weight and ethnicity.
Conclusion
Patellar height was found to be highly symmetric and is, therefore, a reasonable index for contralateral templating. While very few patellofemoral morphometric parameters and anatomical risk factors were asymmetric, the mean differences were clinically negligible and independent of demographics.
Level of evidence
III.

Similar content being viewed by others
References
Benítez-Martínez JC, Valera-Garrido F, Martínez-Ramírez P, Ríos-Díaz J, Del Baño-Aledo ME, Medina-Mirapeix F (2019) Lower limb dominance, morphology, and sonographic abnormalities of the patellar tendon in elite basketball players: a cross-sectional study. J Athl Train 54:1280–1286
Biyani R, Elias JJ, Saranathan A, Feng H, Guseila LM, Morscher MA, Jones KC (2014) Anatomical factors influencing patellar tracking in the unstable patellofemoral joint. Knee Surg Sports Traumatol Arthrosc 22:2334–2341
Boling M, Padua D, Marshall S, Guskiewicz K, Pyne S, Beutler A (2010) Gender differences in the incidence and prevalence of patellofemoral pain syndrome. Scand J Med Sci Sports 20:725–730
Bull AMJ, Katchburian MV, Shih Y-F, Amis AA (2002) Standardisation of the description of patellofemoral motion and comparison between different techniques. Knee Surg Sports Traumatol Arthrosc 10:184–193
Caton J, Deschamps G, Chambat P, Lerat JL, Dejour H (1982) Patella infera. Apropos of 128 cases. Rev Chir Orthop Reparatrice Appar Mot 68:317–325
Crema MD, Cortinas LG, Lima GBP, Abdalla RJ, Ingham SJM, Skaf AY (2018) Magnetic resonance imaging-based morphological and alignment assessment of the patellofemoral joint and its relationship to proximal patellar tendinopathy. Skelet Radiol 47:341–349
Dargel J, Feiser J, Gotter M, Pennig D, Koebke J (2009) Side differences in the anatomy of human knee joints. Knee Surg Sports Traumatol Arthrosc 17:1368–1376
Davies-Tuck M, Teichtahl AJ, Wluka AE, Wang Y, Urquhart DM, Cui J, Cicuttini FM (2008) Femoral sulcus angle and increased patella facet cartilage volume in an osteoarthritic population. Osteoarthr Cartil 16:131–135
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Demehri S, Thawait GK, Williams AA, Kompel A, Elias JJ, Carrino JA, Cosgarea AJ (2014) Imaging characteristics of contralateral asymptomatic patellofemoral joints in patients with unilateral instability. Radiology 273:821–830
Faul F, Erdfelder E, Buchner A, Lang A-G (2009) Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav Res Methods 41:1149–1160
Fucentese SF, Schöttle PB, Pfirrmann CWA, Romero J (2007) CT changes after trochleoplasty for symptomatic trochlear dysplasia. Knee Surg Sports Traumatol Arthrosc 15:168–174
Grassi L, Hraiech N, Schileo E, Ansaloni M, Rochette M, Viceconti M (2011) Evaluation of the generality and accuracy of a new mesh morphing procedure for the human femur. Med Eng Phys 33:112–120
Grelsamer RP, Dejour D, Gould J (2008) The pathophysiology of patellofemoral arthritis. Orthop Clin North Am 39:269–274
Grelsamer RP, Meadows S (1992) The modified Insall-Salvati ratio for assessment of patellar height. Clin Orthop Relat Res 282:170–176
Huntington LS, Webster KE, Devitt BM, Scanlon JP, Feller JA (2020) Factors associated with an increased risk of recurrence after a first-time patellar dislocation: a systematic review and meta-analysis. Am J Sports Med 48:2552–2562
Iranpour F, Merican AM, Teo SH, Cobb JP, Amis AA (2017) Femoral articular geometry and patellofemoral stability. Knee 24:555–563
Iriuchishima T, Ryu K, Murakami T, Yorifuji H (2017) The correlation between femoral sulcus morphology and osteoarthritic changes in the patello-femoral joint. Knee Surg Sports Traumatol Arthrosc 25:2715–2720
Jacquet C, Laumonerie P, LiArno S, Faizan A, Sharma A, Dagneaux L, Ollivier M (2020) Contralateral preoperative templating of lower limbs’ mechanical angles is a reasonable option. Knee Surg Sports Traumatol Arthrosc 28:1445–1451
Katchburian MV, Bull AMJ, Shih Y-F, Heatley FW, Amis AA (2003) Measurement of patellar tracking: assessment and analysis of the literature. Clin Orthop Relat Res 412:241–259
Lacey RJ, Thomas E, Duncan RC, Peat G (2008) Gender difference in symptomatic radiographic knee osteoarthritis in the Knee Clinical Assessment—CAS(K): a prospective study in the general population. BMC Musculoskelet Disord 9:82
Laumonerie P, Ollivier M, LiArno S, Faizan A, Cavaignac E, Argenson J-N (2018) Which factors influence proximal femoral asymmetry?: A 3D CT analysis of 345 femoral pairs. Bone Jt J 100B:839–844
Lewallen L, McIntosh A, Dahm D (2015) First-time patellofemoral dislocation: risk factors for recurrent instability. J Knee Surg 28:303–309
Mahfouz M, Badawi A, Merkl B, Fatah EEA, Pritchard E, Kesler K, Moore M, Jantz R, Jantz L (2007) Patella sex determination by 3D statistical shape models and nonlinear classifiers. Forensic Sci Int 173:161–170
Mehl J, Feucht MJ, Bode G, Dovi-Akue D, Südkamp NP, Niemeyer P (2016) Association between patellar cartilage defects and patellofemoral geometry: a matched-pair MRI comparison of patients with and without isolated patellar cartilage defects. Knee Surg Sports Traumatol Arthrosc 24:838–846
Ollivier M, Parratte S, Lecorroller T, Reggiori A, Champsaur P, Argenson J-N (2015) Anatomy of the proximal femur at the time of total hip arthroplasty is a matter of morphotype and etiology but not gender. Surg Radiol Anat 37:377–384
Pangaud C, Laumonerie P, Dagneaux L, LiArno S, Wellings P, Faizan A, Sharma A, Ollivier M (2020) Measurement of the posterior tibial slope depends on ethnicity, sex, and lower limb alignment: a computed tomography analysis of 378 healthy participants. Orthop J Sports Med 8:232596711989525
Pfirrmann CW, Zanetti M, Romero J, Hodler J (2000) Femoral trochlear dysplasia: MR findings. Radiology 216:858–864
Pierre MA, Zurakowski D, Nazarian A, Hauser-Kara DA, Snyder BD (2010) Assessment of the bilateral asymmetry of human femurs based on physical, densitometric, and structural rigidity characteristics. J Biomech 43:2228–2236
Prakash J, Seon J-K, Woo S-H, Jin C, Song E-K (2016) Comparison of radiological parameters between normal and patellar dislocation groups in Korean population: a rotational profile CT-based study. Knee Surg Relat Res 28:302–311
Teng H-L, Chen Y-J, Powers CM (2014) Predictors of patellar alignment during weight bearing: an examination of patellar height and trochlear geometry. Knee 21:142–146
Wright SJ, Boymans TAEJ, Grimm B, Miles AW, Kessler O (2014) Strong correlation between the morphology of the proximal femur and the geometry of the distal femoral trochlea. Knee Surg Sports Traumatol Arthrosc 22:2900–2910
Young EY, Gebhart J, Cooperman D, Ahn NU (2013) Are the left and right proximal femurs symmetric? Clin Orthop Relat Res 471:1593–1601
Zaffagnini S, Dejour D, Grassi A, Bonanzinga T, Marcheggiani Muccioli GM, Colle F, Raggi F, Benzi A, Marcacci M (2013) Patellofemoral anatomy and biomechanics: current concepts. Joints 1:15–20
Funding
None.
Author information
Authors and Affiliations
Contributions
LD, AF, SL, PW, MO the conception and design of the study, or acquisition of data, or analysis and interpretation of data. LD, HR, P-L, CJ drafting the article or revising it critically for important intellectual content. LD, HR, P-L, AF, SL, PW, MO, CJ final approval of the version to be submitted. AF, SL, PW, MO statistics. CJ experimentation or surgery performance.
Corresponding author
Ethics declarations
Conflict of interest
One or more of the authors declared the following potential conflict of interest or source of funding: S.L., P.W., and A.F. are employees of Stryker. M.O. has received consulting fees from Arthrex, Newclip Technics, and Stryker. LD received a research scholarship grant from the French Society of Orthopaedic Surgery (SOFCOT) and from the University of Montpellier in 2019, that is not related to this work. PL and CJ: no conflicts of interest.
Ethical approval
Each author certifies that his institution has approved the reporting of these cases, that all investigations were conducted in conformity with ethical principles of research. This manuscript contains a study with human participants, which has been approved by our institutional ethics committee (2019-A00912533).
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dagneaux, L., Bin Abd Razak, H.R., Laumonerie, P. et al. Bony asymmetry in patellofemoral morphology and risk factors of instability are mostly clinically negligible. Knee Surg Sports Traumatol Arthrosc 29, 3793–3799 (2021). https://doi.org/10.1007/s00167-020-06413-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06413-7